Documentos de Académico
Documentos de Profesional
Documentos de Cultura
Fracturas de La Clavícula en Bebés y Niños - DynaMed
Cargado por
DAENA KAROLINA SALCEDO CORNEJOTítulo original
Derechos de autor
Formatos disponibles
Compartir este documento
Compartir o incrustar documentos
¿Le pareció útil este documento?
¿Este contenido es inapropiado?
Denunciar este documentoCopyright:
Formatos disponibles
Fracturas de La Clavícula en Bebés y Niños - DynaMed
Cargado por
DAENA KAROLINA SALCEDO CORNEJOCopyright:
Formatos disponibles
CONDICIÓN • Actualizado el 29 de octubre de 2023
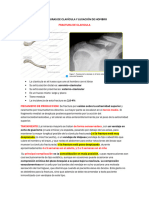
Fracturas de clavícula en bebés y niños
Descripción general y recomendaciones
Fondo
● La clavícula es un hueso de doble curva en forma de S que actúa como un puntal
para la escápula con el !n de suspender la extremidad superior lejos del tórax y
permitir un amplio rango de movimiento.
● La clavícula es el hueso más comúnmente fracturado en el cuerpo, con > 90 % en la
ubicación del eje medio en los adolescentes.
● Las fracturas de la clavícula se pueden clasi!car en función de la ubicación anatómi-
ca.
⚬ Grupo I: fractura del tercio medio de la clavícula
⚬ Grupo II: fractura del tercio lateral (distal) de la clavícula
⚬ Grupo III: fractura del tercio medial (proximal) de la clavícula
● Las fracturas ocurren con mayor frecuencia después de caer sobre el hombro.
Otras causas incluyen un trauma directo en la clavícula, una caída sobre una mano
extendida y un trauma de nacimiento.
● La curación de las fracturas de la clavícula comienza inmediatamente después de
una lesión por 2 vías potenciales: curación ósea indirecta (más común) o curación
ósea directa.
● Las complicaciones raras de las fracturas de la clavícula incluyen neumotórax o le-
siones neurovasculares.
● La mayoría de los niños tienen buenos resultados funcionales después de una frac-
tura de la clavícula, y las no uniones son extremadamente raras.
Evaluación
● Las fracturas de la clavícula en los recién nacidos pueden ser asintomáticas o estar
https://www.dynamed.com/condition/clavicle-fractures-in-infants-and-children 15/02/24, 8 36 p.m.
Página 1 de 46
:
presentes con
⚬ Falta de movimiento espontáneo de la extremidad superior afectada (la llamada
pseudoparálisis); el re"ejo moro puede ser asimétrico
⚬ Edema y crepitus localizados alrededor del lugar de la fractura
⚬ Masa de callos normalmente observada sobre la clavícula afectada 7-10 días des-
pués de la fractura
● Las fracturas de clavícula en bebés, niños y adolescentes pueden presentarse con
⚬ Dolor agudo con moretones, edema y crepitus alrededor del lugar de la fractura
⚬ Mano del brazo no lesionado que sostiene el codo del brazo afectado
● Realice un examen físico exhaustivo, buscando signos/síntomas de un neumotórax
(raro) y signos de un examen neurovascular comprometido (roca, papel, tijera, OK y
signos de autoestopista). Si no hay antecedentes de trauma, considere causas sub-
yacentes alternativas, como la malignidad o el ractismo.
● Las fracturas distales (laterales) de la clavícula pueden parecer benignas en una ra-
diografía, pero pueden estar asociadas con un desplazamiento signi!cativo. Evalúe
el dolor y busque moretones o arrugas en la piel en el aspecto posterior del hom-
bro.
● Obtenga rayos X como método de imagen inicial, con las vistas estándar de antero-
posterior vertical (AP) y AP vertical con una inclinación cefálica de 30 grados.
● Considere la tomografía computarizada para
⚬ Identi!car o descartar la fractura de la clavícula medial (las radiografías no pue-
den ser concluyentes)
⚬ Determinar la dirección del desplazamiento en las fracturas de la clavícula me-
dial
⚬ Determinar la dirección y la gravedad del desplazamiento en las fracturas físicas
laterales de la "manga clavicular"
⚬ Diferenciar entre fracturas de clavícula y dislocaciones de las articulaciones es-
ternoclaviculares
⚬ Descartar el neumotórax, si hay una alta sospecha clínica de lesión y una radio-
grafía de tórax y una evaluación enfocada extendida con ecografía para el trau-
ma no son de diagnóstico
https://www.dynamed.com/condition/clavicle-fractures-in-infants-and-children 15/02/24, 8 36 p.m.
Página 2 de 46
:
● Considere la resonancia magnética para
⚬ Fracturas de la clavícula distal para evaluar si hay lesiones ligamentosas o de la-
brum
⚬ Fracturas de clavícula con sospechas de lesiones neurovasculares
● Para la fractura de la clavícula neonatal:
⚬ Obtener radiografías para diagnosticar una fractura desplazada
⚬ Si la fractura no se desplaza, el diagnóstico se puede hacer mediante el descubri-
miento de un callo palpable semanas después
Gestión
● La mayoría de las fracturas de clavícula en niños y adolescentes se manejan de for-
ma no operativa.
● El manejo no operativo puede consistir en
⚬ Analgesia para ayudar a controlar el dolor
⚬ Inmovilización del hombro con un simple cabestrillo durante 3-4 semanas
⚬ Aumento gradual del rango de movimiento
⚬ Volver al fortalecimiento a las 6 semanas
● Se deben considerar los siguientes tipos de fracturas para el manejo quirúrgico:
⚬ Fracturas abiertas
⚬ Fracturas con perforación cercana a la piel
⚬ Implicación neurovascular
⚬ Lesión "otante en el hombro
● Para la fractura de la clavícula neonatal:
⚬ No se necesita un tratamiento especí!co
⚬ Considere el acetaminofén oral o rectal para el control del dolor
● La reducción abierta y la !jación interna con una placa y un tornillo contorneados
es el procedimiento quirúrgico más utilizado para las fracturas de la clavícula, pero
la !jación con un pasador intramedular también se utiliza para fracturas menos
complejas.
● El cable de Kirschner debe evitarse en la !jación de las fracturas de la clavícula debi-
https://www.dynamed.com/condition/clavicle-fractures-in-infants-and-children 15/02/24, 8 36 p.m.
Página 3 de 46
:
do al riesgo de complicación grave de la migración del alambre hacia la vasculatura,
así como al aumento de la tasa de infección.
● El manejo postoperatorio de las fracturas de la clavícula varía según el tipo de frac-
tura.
Related Topics
● Clavicle Fracture in Adults
● Clavicle Fracture - Emergency Management
● Acromioclavicular (AC) Joint Injuries
● Acromioclavicular Separation - Emergency Management
General Information
Description
● fracture of the clavicle (collarbone) of the shoulder, typically resulting in acute
shoulder pain, bruising, tenderness, and limited range of motion (J Am Acad Orthop
Surg 2011 Jul;19(7):392)
Also Called
● broken collarbone
● collarbone fracture
● midshaft clavicle fracture
● distal clavicle fracture
● lateral clavicle fracture
● medial clavicle fracture
Normal Clavicle Anatomy and Function
● osseous anatomy and function
https://www.dynamed.com/condition/clavicle-fractures-in-infants-and-children 15/02/24, 8 36 p.m.
Página 4 de 46
:
⚬ clavicle bone characteristics
– S-shaped, double-curved bone 4
– forms by endochondral and intramembranous ossi!cation 2
– central portion of bone more tubular in nature and subjected to greatest ben-
ding and torsional forces (making this area more vulnerable to fractures) (Bull
NYU Hosp Jt Dis 2009;67(1):52)
– medial and lateral epiphyses close at about ages 19 years and 25 years, res-
pectively 2
⚬ clavicle acts as a strut for scapula in order to suspend upper extremity away
from thorax and permit extensive range of motion 4
● ligament anatomy and function
⚬ acromioclavicular (AC) ligaments (anterior, posterior, superior, and inferior) at-
tach distal end of clavicle with acromion of scapula, forming the AC joint; AC liga-
ments
– strengthen AC joint capsule
– resist anterior and posterior translation of AC joint
⚬ coracoclavicular ligaments (lateral trapezoid and medial conoid) attach superior
surface of scapula coracoid with undersurface of clavicle and act to prevent su-
perior migration of clavicle
⚬ articulation of clavicle and sternum reinforced with sternoclavicular and costocla-
vicular ligaments; only joint that links upper extremity with axial skeleton
⚬ Reference - Phys Sportsmed 2011 Sep;39(3):142
⚬ in children and adolescents, these ligaments attach to a thick periosteal sleeve 2
● muscular anatomy 2
⚬ sternocleidomastoid, sternohyoid, and pectoralis major attach medially
⚬ subclavius attaches in midportion
⚬ deltoid and trapezius attach laterally
● neurovascular structures located near the clavicle include 3
⚬ brachial plexus
⚬ subclavian artery and vein
⚬ internal jugular vein
https://www.dynamed.com/condition/clavicle-fractures-in-infants-and-children 15/02/24, 8 36 p.m.
Página 5 de 46
:
⚬ axillary artery
⚬ supraclavicular nerves
Types
● Allman classi!cation of clavicle fractures (most widely used)
⚬ group I: fracture of middle third of clavicle
⚬ group II: fracture of lateral (distal) third of clavicle
⚬ group III: fracture of medial (proximal) third of clavicle
⚬ References - J Bone Joint Surg Am 1967 Jun;49(4):774,
Epidemiology
Incidence/Prevalence
● clavicle is the most commonly fractured bone in the body 3
● clavicle fractures account for reported 10%-15% of all fractures in children (J Pediatr
Orthop 2012 Jun;32 Suppl 1:S1)
● reported > 90% of clavicle fractures in adolescents are midshaft fractures 1
● clavicle is most commonly injured bone during labor and delivery, accounting for
reported 90% of all obstetrical fractures and reported in 1%-7% of all births (Orthop
Nurs 2009 Sep-Oct;28(5):210-4; quiz 215-6)
Risk Factors
● participation in all types of sports, including
⚬ cycling (may involve falling over the handlebars) (BMJ Open Sport Exerc Med
2016;2(1):e000042)
⚬ hockey (Am J Orthop (Belle Mead NJ) 2017 May/Jun;46(3):123)
⚬ football (Int J Sports Med 2014 Jan;35(1):83)
⚬ wrestling (Orthop J Sports Med 2019 May;7(5):2325967119847470)
⚬ judo (Orthop J Sports Med 2019 May;7(5):2325967119847470)
⚬ weightlifting (powerlifting) (Scand J Med Sci Sports 2016 Oct;26(10):1233)
https://www.dynamed.com/condition/clavicle-fractures-in-infants-and-children 15/02/24, 8 36 p.m.
Página 6 de 46
:
⚬ skiing and snowboarding (Curr Sports Med Rep 2019 Nov;18(11):394)
● most common activities reported during clavicle fracture in cohort of 185 children
(median age 14.4 years)
⚬ bicycling
⚬ soccer
⚬ skiing
⚬ falling, either during running or from a height
⚬ horseback riding
⚬ playing on playground
⚬ riding motorcycle or scooter
⚬ ice hockey
⚬ Reference - J Pediatr Orthop 2014 Jun;34(4):393
● nonaccidental trauma (Clin Pediatr (Phila) 2019 Jun;58(6):618)
● congenital disorders that include 3
⚬ osteogenesis imperfecta (in which defective collagen formation compromises in-
tegrity of bone)
⚬ oxalosis (rare inborn error of metabolism)
● risk factors for neonatal clavicle fracture include
⚬ fetal macrosomia
⚬ shoulder dystocia
⚬ delivery requiring specialized obstetrical maneuvers
⚬ use of instruments, such as vacuum and forceps, during delivery
⚬ older age of birthing parent
⚬ References - Pediatr Rev 2016 Nov;37(11):451, Orthop Nurs 2009 Sep-
Oct;28(5):210-4; quiz 215-6,
Associated Conditions
● neonatal clavicle fracture associated with brachial plexus birth palsy (Orthop Clin
North Am 2014 Apr;45(2):225 )
Etiology and Pathogenesis
https://www.dynamed.com/condition/clavicle-fractures-in-infants-and-children 15/02/24, 8 36 p.m.
Página 7 de 46
:
Causes
● most commonly caused by axial load transmitted by fall on shoulder 2
● less commonly caused by 2
⚬ direct trauma to clavicle
⚬ fall on outstretched hand
● in the obstetric setting 3
⚬ clavicle is most commonly injured bone during labor and delivery (Orthop Nurs
2009 Sep-Oct;28(5):210)
⚬ clavicle fracture may occur as a complication of breech delivery (may occur with
shoulder dystocia)
⚬ intentional fracture (cleidotomy) is sometimes used as third-line management
for shoulder dystocia during delivery
Pathogenesis
● clavicle forms by both endochondral and intramembranous ossi!cation 2
⚬ primary ossi!cation center of the clavicle appears in utero at about 5.5 weeks
gestation and continues to facilitate postnatal clavicular growth, which occurs via
intramembranous ossi!cation
⚬ lateral and medial growth centers appear in adolescence and contribute growth
at the ends of the clavicle via endochondral ossi!cation
– lateral epiphyseal growth center fuses at age 19 years
– medial epiphyseal growth center fuses at age 25 years
⚬ adolescent patients may have increased potential for remodeling of the clavicle
compared to adult patients 1
● bone healing begins immediately following injury
⚬ 2 potential healing pathways
– indirect bone healing (most common pathway)
● bone's natural healing process, which begins immediately following injury
● consists of both intramembranous and endochondral bone formation
https://www.dynamed.com/condition/clavicle-fractures-in-infants-and-children 15/02/24, 8 36 p.m.
Página 8 de 46
:
● does not require surgery or rigid stable conditions; best if some micromo-
tion and weight-bearing takes place
● generally, this pathway occurs in nonoperative fracture management and in
certain operative treatments in which some motion occurs at the fracture
site, such as with
⚬ intramedullary nailing
⚬ external !xation (rarely used)
⚬ internal !xation of complicated comminuted fractures
– direct bone healing
● permits bone structure to immediately regenerate anatomic lamellar bone
and the Haversian systems without requiring any remodeling steps
● requires all of the following
⚬ correct anatomic reduction of fracture ends
⚬ no gap formation
⚬ stable !xation (primary goal of open reduction and internal !xation sur-
gery with plate and screws)
⚬ biological process of indirect bone healing
– acute in"ammatory response
● immediately after injury, a hematoma is formed and consists of cells from
peripheral and intramedullary blood and bone marrow cells
● an in"ammatory response is then triggered that leads to coagulation of the
hematoma near and within the fracture area, which begins the process of
forming a callus to bridge the fracture; response peaks in 24 hours and is
completed after 7 days
● additionally, a proin"ammatory response occurs and involves secretion of
factors that recruit in"ammatory cells and foster angiogenesis as well as
formation of primary soft cartilaginous callus
– generation of callus tissues
● after formation of primary hematoma, !brin-rich granulation tissue forms
● within granulation tissue, endochondral formation occurs in between frac-
ture ends and external to periosteal sites
● cartilaginous tissue forms a soft callus, providing the fracture a stable struc-
https://www.dynamed.com/condition/clavicle-fractures-in-infants-and-children 15/02/24, 8 36 p.m.
Página 9 de 46
:
ture
● simultaneously, an intramembranous ossi!cation response occurs subpe-
riosteally directly adjacent to distal and proximal ends of fracture, creating
a hard callus
● generation of callus tissues dependent on recruitment of mesenchymal
stem cells, as they proliferate and di#erentiate into osteogenic cells
– bone remodeling
● the hard callus provides biomechanical stability but does not fully restore
normal bone biomechanical properties
● a second resorptive phase initiated to remodel the hard callus into a lame-
llar bone structure with a central medullary cavity
⚬ remodelling process accomplished by a balance of hard callus resorption
by osteoclasts and lamellar bone deposition by osteoblasts
⚬ process initiated as early as 3-4 weeks after fracture but may take years
to develop fully regenerated bone structure (may occur faster in younger
patients)
⚬ for bone remodelling to be successful, an adequate blood supply and a
gradual increase in mechanical stability is critical
– blood supply and revascularization
● essential for successful bone repair
● in endochondral fracture healing, this consists of both of the following
⚬ angiogenic pathways
⚬ chondrocyte apoptosis and cartilaginous degradation (removal of cells
and extracellular matrices required to allow blood vessel in-growth at
repair site)
⚬ Reference - Injury 2011 Jun;42(6):551
History and Physical
Clinical Presentation
● clavicle fracture in infants and children
https://www.dynamed.com/condition/clavicle-fractures-in-infants-and-children 15/02/24, 8 36 p.m.
Página 10 de 46
:
⚬ typically presents with acute pain with bruising, edema, and crepitus around
fracture site
⚬ child often presents with opposite hand supporting the elbow of the a#ected
arm
⚬ Reference - Orthop Nurs 2009 Sep-Oct;28(5):210
● most often presents with history of trauma; if no history of trauma, important to
consider other uncommon underlying causes
⚬ physical abuse
⚬ malignancy
⚬ rickets
⚬ congenital pseudoarthrosis of the clavicle (only if right side a#ected) (Glob Pe-
diatr Health 2014;1:2333794X14563384)
⚬ Reference - Am Fam Physician 2008 Jan 1;77(1):65, commentary can be found in
Am Fam Physician 2008 Sep 15;78(6):697
● pneumothorax due to displaced clavicle fracture possible although rare (Emerg
Med Clin North Am 2020 Feb;38(1):103)
● symptoms of pneumothorax include
⚬ chest pain
⚬ dyspnea
⚬ tachypnea
⚬ tachycardia
⚬ Reference - J Emerg Trauma Shock 2008 Jan;1(1):34
● neonatal clavicle fracture
⚬ often asymptomatic
⚬ parents may report lack of spontaneous movement of a#ected upper extremity
(pseudoparalysis); Moro re"ex may be asymmetric
⚬ edema, petechiae, and/or crepitus may be localized around fracture site
⚬ callus mass typically noted over a#ected clavicle 7-10 days after fracture
⚬ References - Pediatr Rev 2016 Nov;37(11):451, Orthop Nurs 2009 Sep-
Oct;28(5):210
History
https://www.dynamed.com/condition/clavicle-fractures-in-infants-and-children 15/02/24, 8 36 p.m.
Página 11 de 46
:
History of Present Illness (HPI)
● for infants and older children, ask about 3
⚬ time of injury
⚬ mechanism of injury
⚬ location of pain
⚬ presence of paresthesias or subjective numbness
⚬ hand dominance
● if no history of trauma, ask about history of seizures, pain in lower limbs or back, or
muscle weakness, all suggestive of rickets
● in neonates, ask about
⚬ birth history, including breech presentation, shoulder dystocia, and delivery re-
quiring specialized obstetrical maneuvers or use of instruments
⚬ onset of callus mass if present (usually presents 7-10 days following fracture)
⚬ Reference - 3 , Orthop Nurs 2009 Sep-Oct;28(5):210
Past Medical History (PMH)
● ask about history of congenital disorders associated with increased risk of fracture,
including 3
⚬ oxalosis
⚬ osteogenesis imperfecta
Social History (SH)
● ask about 3
⚬ participation in sports
⚬ smoking history
● ask about any concerns about nonaccidental trauma (Clin Pediatr (Phila) 2019
Jun;58(6):618)
Physical
https://www.dynamed.com/condition/clavicle-fractures-in-infants-and-children 15/02/24, 8 36 p.m.
Página 12 de 46
:
General Physical
● if no history of trauma, look for signs of physical abuse (Am Fam Physician 2008 Jan
1;77(1):65, commentary can be found in Am Fam Physician 2008 Sep 15;78(6):697)
Clavicle
● inspect the area around the clavicle for 3
⚬ asymmetry
⚬ swelling
⚬ ecchymosis
⚬ skin integrity
⚬ deformity
⚬ skin tenting (may indicate impending open fracture)
CLINICIANS' PRACTICE POINT
Assess the posterior aspect of the shoulder, and look for bruising or dimpling of the
skin in displaced fractures of the lateral end of the clavicle.
● palpate the length of the clavicle, and assess for 3
⚬ crepitus
⚬ instability
⚬ location of tenderness
Lungs
● if pneumothorax suspected, assess for diminished breath sounds (J Emerg Trauma
Shock 2008 Jan;1(1):34)
● !ndings of pneumothorax may also include
⚬ decreased vocal resonance and tactile fremitus
⚬ increased tympany with percussion on a#ected side
⚬ unequal chest wall excursion
⚬ see Pneumothorax - Emergency Management for additional information
https://www.dynamed.com/condition/clavicle-fractures-in-infants-and-children 15/02/24, 8 36 p.m.
Página 13 de 46
:
Musculoskeletal
● evaluate for associated injuries, including 3
⚬ scapular fractures
⚬ rib fractures
⚬ acromioclavicular or sternoclavicular dislocation
⚬ "ail limb
● enlarged wrists, knees, or ankles or bowing of weight-bearing extremities are signs
suggestive of rickets
Neurovascular
● palpate distal radial and ulnar pulses 3
● perform motor and sensory exam of a#ected extremity to assess radial, median,
ulnar, and axillary nerve distributions 3
● simpli!ed exam to exclude nerve injury due to clavicle fracture consists of
⚬ rock, paper, scissor, OK, and hitchhiker's sign
– rock - making !st will assess median nerve
– paper - extending !ngers will assess radial nerve
– scissor - "exion of fourth and !fth digit will assess ulnar nerve
– OK - will assess anterior interosseous nerve (branch of median nerve)
– hitchhiker's sign- will assess posterior interosseous nerve (branch of radial
nerve)
⚬ checking deltoid region for axillary nerve sensation
⚬ checking bicep strength to assess musculocutaneous nerve
https://www.dynamed.com/condition/clavicle-fractures-in-infants-and-children 15/02/24, 8 36 p.m.
Página 14 de 46
:
⚬ Reference - Clin Pediatr (Phila) 2017 May;56(5):467
Diagnosis
Making the Diagnosis
● in neonates
⚬ suspect clavicle fracture in neonates with the following signs and symptoms, es-
pecially if history of high birth weight, shoulder dystocia, or use of vacuum for-
ceps
– lack of spontaneous movement of a#ected upper extremity (pseudoparalysis)
– edema, petechiae, and/or crepitus around a#ected clavicle
– callus mass on a#ected clavicle
⚬ x-ray con!rms diagnosis of displaced fracture
⚬ if fracture is not displaced, diagnosis can be made by discovery of palpable callus
weeks later
⚬ Reference - Pediatr Rev 2016 Nov;37(11):451
● in children
⚬ suspect clavicle fracture in children with the following signs and symptoms, espe-
cially if recent history of trauma 3
– acute shoulder pain
– swelling
– shoulder deformity
– impaired function of ipsilateral arm
⚬ imaging typically used to con!rm diagnosis
Di!erential Diagnosis
● in patients with history of trauma, other possible causes of shoulder pain include
⚬ acromioclavicular separation
⚬ sternoclavicular joint dislocation (rare)
⚬ proximal humerus fracture
https://www.dynamed.com/condition/clavicle-fractures-in-infants-and-children 15/02/24, 8 36 p.m.
Página 15 de 46
:
⚬ rotator cu# tear
⚬ shoulder dislocation
⚬ shoulder contusion
⚬ biceps or pectoralis rupture
⚬ cervical injury
⚬ Reference - Emerg Med Clin North Am 2020 Feb;38(1):103
● if no history of trauma, important to consider
⚬ physical abuse
⚬ malignancy
⚬ rickets
⚬ Reference - Am Fam Physician 2008 Jan 1;77(1):65, commentary can be found in
Am Fam Physician 2008 Sep 15;78(6):697
● conditions to consider in neonates
⚬ brachial plexus palsy
⚬ congenital muscular torticollis
⚬ pseudoartrosis congénita
⚬ Reference - Orthop Nurs 2009 Sep-Oct;28(5):210-4; quiz 215-6
Testing Overview
● x-rays are typically initial imaging method; standard views include 2
⚬ upright anteroposterior (AP) of site of injury (clavicle and ipsilateral shoulder)
⚬ upright AP with 30-degree cephalic tilt
● additional imaging may be needed
⚬ for assessing distal clavicle fractures (axillary lateral view of shoulder or magnetic
resonance imaging)
⚬ for assessing extent of other injuries, including possible pneumothorax (compu-
ted tomography)
⚬ if medial clavicle fracture suspected but initial x-rays not conclusive (computed
tomography)
● if signi!cant trauma, review imaging for other musculoskeletal injuries and lung
!elds for pneumothorax (J Am Acad Orthop Surg 2018 Nov 15;26(22):e468)
https://www.dynamed.com/condition/clavicle-fractures-in-infants-and-children 15/02/24, 8 36 p.m.
Página 16 de 46
:
Imaging Studies
X-ray
● x-rays are typically initial imaging method; standard views include 2
⚬ upright anteroposterior (AP) of site of injury (clavicle and ipsilateral shoulder)
⚬ upright AP with 30-degree cephalic tilt
● additional x-ray views may include
⚬ an apical oblique view of the clavicle (completed with patient standing 45 de-
grees toward beam and beam angled 20-30 degrees cephalad) to evaluate extent
of displacement (Open Orthop J 2013;7:329full text )
⚬ Zanca view of acromioclavicular (AC) joint with 10-15 degrees of cephalic tilt to
evaluate intra-articular involvement (J Am Acad Orthop Surg 2011 Jul;19(7):392)
⚬ contralateral shoulder or chest if suspected asymmetric AC joint widening or in-
jury 3
⚬ axillary lateral view of shoulder, which should be obtained in patients with distal
clavicle fracture (J Am Acad Orthop Surg 2011 Jul;19(7):392)
● distal (lateral) and shaft clavicle fractures typically detected on plain x-rays; howe-
ver, medial clavicle fractures frequently challenging to diagnose with conventional
x-rays alone (Eur J Trauma Emerg Surg 2020 Jun;46(3):519)
CLINICIANS' PRACTICE POINT
Distal (lateral) clavicle fractures may appear benign on an x-ray but can be associated with
signi!cant displacement. Look for signs of pain, bruising, or puckering of the skin in the
posterior aspect of the shoulder.
https://www.dynamed.com/condition/clavicle-fractures-in-infants-and-children 15/02/24, 8 36 p.m.
Página 17 de 46
:
STUDY
● SUMMARY
use of 4-view x-ray series (standard 2 views plus orthogonal views) may increase
likelihood of surgeons recommending operative management
COHORT STUDY: J Shoulder Elbow Surg 2012 Oct;21(10):1263
Details
⚬ based on retrospective cohort study
⚬ 50 patients with con!rmed acute midshaft clavicular fractures had 2-view and 4-
view x-ray series evaluated by 4 (blinded) orthopedists to determine optimal care
– for each patient, standard 2-view x-ray series evaluated by orthopedists !rst,
followed by 4-view series ≥ 1 week later; procedure then repeated ≥ 2 months
later
● 2-view x-ray series consisted of anterior-posterior and 20-degree cephalic
tilt
● 4-view x-ray series consisted of anterior-posterior, 20-degree cephalic tilt,
45-degree cephalic tilt, and 45-degree caudal tilt
– treatment decisions made according to individual surgeon’s criteria for surgi-
cal intervention
⚬ during !rst assessment period, cases classi!ed as surgical in 61 of 200 reviews
(31%) with 2-view series vs. 81 of 200 reviews (40.5%) with 4-view series (p < 0.05)
⚬ for 17 patients (34%), at least 1 surgeon changed treatment decision between 2-
and 4-view review; for 13 of these patients, treatment was changed from nono-
https://www.dynamed.com/condition/clavicle-fractures-in-infants-and-children 15/02/24, 8 36 p.m.
Página 18 de 46
:
perative to operative
⚬ intraobserver reliability signi!cantly greater for 4-view vs. 2-view series, with no
signi!cant di#erence in interobserver reliability
⚬ Reference - J Shoulder Elbow Surg 2012 Oct;21(10):1263
Computed Tomography (CT)
● CT not routinely used in patients with nondisplaced clavicle fractures (Skeletal Ra-
diol 2011 Jul;40(7):831)
● CT scans should be carefully considered given exposure to moderate levels of radia-
tion (Prim Care 2013 Dec;40(4):849)
● if medial clavicle fracture suspected and x-rays inconclusive, CT scan may be obtai-
ned (Eur J Trauma Emerg Surg 2020 Jun;46(3):519)
● CT scan may also be used to
⚬ determine direction of displacement in medial clavicle fractures (Phys Sportsmed
2011 Sep;39(3):142)
⚬ determine direction and severity of displacement in lateral "clavicular sleeve"
physeal fracture (Radiographics 2016 Oct;36(6):1672)
⚬ di#erentiate between clavicle fractures and sternoclavicular joint dislocations
(Prim Care 2013 Dec;40(4):911)
⚬ help rule out pneumothorax if high clinical suspicion for injury and chest x-ray
and extended focused assessment with sonography for trauma are nondiagnos-
tic; see Pneumothorax - Emergency Management for additional information
Magnetic Resonance Imaging (MRI)
● for distal clavicle fractures, MRI may be used to
⚬ characterize concomitant ligamentous injury and assist in more granular injury
classi!cation (Skeletal Radiol 2011 Jul;40(7):831)
⚬ identify labrum tears and superior labrum anterior posterior tears (BMC Muscu-
loskelet Disord 2018 Jan 19;19(1):24)
⚬ identify partial- or full-thickness rotator cu# tears or lesions of biceps pulley sys-
tem (BMC Musculoskelet Disord 2018 Jan 19;19(1):24)
https://www.dynamed.com/condition/clavicle-fractures-in-infants-and-children 15/02/24, 8 36 p.m.
Página 19 de 46
:
● MRI may also be used with clavicle fracture and suspected
⚬ neurovascular complications
⚬ pseudoaneurysm formation
⚬ impingement of fracture fragments on brachial plexus and adjacent vessels
⚬ hematoma formation
⚬ Reference - Skeletal Radiol 2011 Jul;40(7):831
Management
Management Overview
● focus of treatment on prevention of malunion and functional de!cits 2
● 3 factors di#erentiating clavicle fractures in children or adolescents from those in
adults 1
⚬ growth remaining; clavicle achieves 80% of its length by age
– 9 years in girls
– 12 years in boys
⚬ increased remodeling potential in children and adolescents
⚬ greater physical activity during childhood/adolescence
● most clavicle fractures in children are managed nonoperatively
⚬ no speci!c treatment necessary for neonatal clavicle fracture
⚬ sling typically preferred over !gure-of-8 bracing
⚬ nonoperative management of simple closed fractures may not require regular
orthopedic and radiographic follow-up
⚬ for displaced clavicle fractures in adolescents, good functional outcomes have
been reported for nonoperative management, but there are also reports of ma-
lunion after nonoperative management
● following types of fractures should be considered for surgery
⚬ indications for surgical treatment of clavicle fractures in children include
– open fractures
– fractures with near skin perforation
https://www.dynamed.com/condition/clavicle-fractures-in-infants-and-children 15/02/24, 8 36 p.m.
Página 20 de 46
:
– fractures with neurovascular involvement
– displaced clavicle fractures in "oating shoulder injuries
– markedly displaced "clavicular sleeve" lateral physeal fractures that have po-
tential for Y-shaped malunion
⚬ clavicle fractures with 100% displacement or signi!cant shortening of clavicle (> 2
cm) have been increasingly managed operatively in adults based on evidence
showing better outcomes with surgery over nonoperative management; mana-
gement of these kinds of clavicle fractures in adolescents has followed a similar
trend even though evidence for improved outcomes with surgery in adolescents
is lacking
⚬ currently, studies comparing outcomes of nonoperative vs. operative manage-
ment of clavicle fractures in children are limited by di#erences in the 2 groups
evaluated, including injury severity and patient age
⚬ open reduction and internal !xation with contoured plate and screws is the most
commonly used surgical procedure, but !xation with intramedullary pin also
used for less complex fractures
⚬ Kirschner wire should be avoided in !xation of clavicle fractures due to risk of
serious complication of wire migration into vasculature as well as increased rate
of infections
⚬ postoperative management varies by fracture type
Nonoperative Management
● most clavicle fractures in children and adolescents managed nonoperatively 2
● nonoperative management may consist of 2
⚬ analgesia to help manage pain
⚬ immobilization of shoulder with a simple sling for 3-4 weeks
⚬ gradual increase in range of motion
⚬ return to strengthening at 6 weeks
● in neonates with clavicle fracture
⚬ no speci!c treatment is needed
⚬ oral or rectal acetaminophen can be used for pain management
⚬ Reference - Pediatr Rev 2016 Nov;37(11):451
https://www.dynamed.com/condition/clavicle-fractures-in-infants-and-children 15/02/24, 8 36 p.m.
Página 21 de 46
:
● union of bone expected by 12 weeks in adolescents and may be earlier in younger
children 2
● sling typically preferred over !gure-of-8 brace 1,2
⚬ brace reported to be associated with increased pain and discomfort
⚬ although not evaluated in pediatric and adolescent population, bracing not asso-
ciated with improved outcomes compared to use of sling in a trial of 60 patients
≥ 15 years old with midshaft clavicle fracture (Bone Joint J 2015 Nov;97-
B(11):1562)
● reported complications from nonoperative management include 1,2
⚬ symptomatic malunion including pain, fatigability, and decreased endurance of
a#ected extremity
⚬ dissatisfaction with appearance of shoulder
⚬ thoracic outlet syndrome resulting from malunion
STUDY
● SUMMARY
high rates of reunion and return to sports reported in children with mostly sim-
ple clavicle fractures managed nonoperatively; mean 4.2 radiographs/child re-
ported during combined treatment and follow-up DynaMed Level 3
COHORT STUDY: Pediatr Emerg Care 2018 Oct;34(10):706
Details
⚬ based on retrospective cohort study
⚬ 340 children aged 0.1-17.8 years managed for clavicle fractures at a single pedia-
tric hospital were included
⚬ 93% were simple fractures; 4.1% had skin tenting, 0.6% were open fractures, and
none had neurovascular involvement
⚬ fracture involvement
– middle third of clavicle in 82%
– distal (lateral) clavicle in 17.4%
– medial (proximal) clavicle in 0.6%
⚬ 98% managed nonoperatively
⚬ clinical and radiographic reunion occurred in all children, and all children retur-
ned to sports
https://www.dynamed.com/condition/clavicle-fractures-in-infants-and-children 15/02/24, 8 36 p.m.
Página 22 de 46
:
⚬ 2 refractures reported
⚬ mean number of clinic visits, including initial emergency department visit, 2.1
⚬ children had mean 4.2 radiographs during mean 1.8 radiology appointments du-
ring treatment and follow-up
⚬ Reference - Pediatr Emerg Care 2018 Oct;34(10):706
● nonoperative management of simple closed fractures may not require regular ort-
hopedic and radiographic follow-up
STUDY
⚬ SUMMARY
simple clavicle fractures in adolescents < 16 years old managed with sling by
primary care physician reported to result in complete union, full range of mo-
tion, and no pain DynaMed Level 3
CASE SERIES: Clin Pediatr (Phila) 2017 May;56(5):467
Details
– based on case series
– 16 adolescents < 16 years old (88% male) with simple clavicle fractures were
treated conservatively with sling by primary care physician
– simple clavicle fractures included angulated, minimally displaced, or greens-
tick fractures
– no malunions and no nonunions occurred
– at mean follow-up of 83 days
● all adolescents had full range of motion
● no reports of painful bumps, paresthesias, or di$culties with daily activities
– Reference - Clin Pediatr (Phila) 2017 May;56(5):467
⚬ 100% of respondents (18 of 24 treated adolescents) reported return to full acti-
vity with no residual pain at 6-month follow-up after institution of new protocol
in which isolated, uncomplicated medial clavicle fractures are managed nonope-
ratively with sling without orthopedic referral (Br J Hosp Med (Lond) 2014
May;75(5):287)
● for displaced clavicle fractures in adolescents, good functional outcomes have been
reported for nonoperative management, but there are also reports of malunion af-
ter nonoperative management
https://www.dynamed.com/condition/clavicle-fractures-in-infants-and-children 15/02/24, 8 36 p.m.
Página 23 de 46
:
STUDY
⚬ SUMMARY
nonoperative management of displaced midshaft clavicle fractures with sling
reported to result in good functional outcomes in adolescents DynaMed Level 3
CASE SERIES: J Bone Joint Surg Am 2013 Jul 3;95(13):1159
Details
– based on case series
– 16 adolescents (mean age 14.2 years, 75% male) with isolated, completely dis-
placed, shortened midshaft clavicle fracture treated nonoperatively with sling
were included
– mean clavicle shortening at time of injury 11.75 mm (range 5-21 mm)
– at mean follow-up of 2 years, all adolescents had returned to full activity
– all adolescents had no signi!cant di#erence in Constant Scores between inju-
red and noninjured shoulders
– 15 adolescents reported being satis!ed with appearance of injured clavicle
– no signi!cant di#erence between shoulders for most measures of range of
motion or strength except for 8% decrease in maximal shoulder external rota-
tion strength (p = 0.04) and 11% loss of shoulder abduction endurance
strength (p = 0.04)
– Reference - J Bone Joint Surg Am 2013 Jul 3;95(13):1159
STUDY
⚬ SUMMARY
fracture shortening 15 mm at or near time of injury not associated with worse
functional outcomes in adolescents with displaced clavicle fracture managed
nonoperatively
COHORT STUDY: Injury 2015 Jul;46(7):1372
Details
– based on retrospective cohort study
– 22 adolescents (mean age 14 years, 77% male) with displaced clavicle fracture
treated nonoperatively had measurement of fracture shortening from x-ray
obtained at or near time of injury and were evaluated
● management consisted of sling plus non-weight-bearing for 2-4 weeks with
gradual return to activity at 1-3 months
● functional and subjective outcomes evaluated using Constant Score and
https://www.dynamed.com/condition/clavicle-fractures-in-infants-and-children 15/02/24, 8 36 p.m.
Página 24 de 46
:
Nottingham Clavicle Score (NCS)
● custom questionnaire used to assess sports participation and attitudes
about cosmesis after recovery
– at mean follow-up of 2.4 years
● no signi!cant di#erence in Constant Score of injured and noninjured shoul-
ders
● mean radiographic shortening of 11.2 mm (range 0-24 mm)
– no signi!cant di#erences in mean NCS or Constant Score when comparing
● length of fracture shortening, ≥ 15 mm vs. < 15 mm
● sex, girls to boys
● duration of participation in overhead or intense contact sports in year, ≥ 6
months to < 6 months
– 5 adolescents who reported being unhappy about how their shoulder looked
at the beach or pool had nonsigni!cant increased mean fracture shortening
compared to those with no cosmetic concern, 12.1 mm vs. 10.9 mm (not signi-
!cant)
– Reference - Injury 2015 Jul;46(7):1372
STUDY
⚬ SUMMARY
symptomatic malunion reported in 5 of 14 adolescents with displaced midshaft
clavicle fractures after nonoperative management DynaMed Level 3
CASE SERIES: J Pediatr Orthop 2010 Jun;30(4):307
Details
– based on case series
– 42 adolescents (aged 12-17 years) with 43 closed midshaft clavicle fractures
were included
● 25 adolescents treated nonoperatively with sling or !gure-of-8 brace for
mean 4 weeks
● 17 adolescents treated operatively with open reduction internal !xation
(ORIF)
– excluded from study were adolescents with open fracture, objective neurolo-
gic !ndings associated with neurovascular injury, or medical contraindication
https://www.dynamed.com/condition/clavicle-fractures-in-infants-and-children 15/02/24, 8 36 p.m.
Página 25 de 46
:
to surgery
– nonoperative group included 14 adolescents with displaced fractures with
fracture shortening (range 10-32 mm)
– among adolescents treated nonoperatively
● symptomatic malunion 6-24 months after initial injury developed in 5 ado-
lescents with displaced fractures (mean fracture displacement 26 mm)
● 4 adolescents with malunion had corrective osteotomy with internal !xa-
tion that resulted in union at mean 6.8 weeks and return to activities at
mean 12 weeks
– among adolescents treated with ORIF
● no nonunions or malunions
● 3 adolescents had additional surgery to remove hardware
– comparing ORIF to nonoperative management
● mean time to return to activity 12 weeks vs. 16 weeks (no p value reported)
● mean time to union for displaced fractures 7.5 weeks vs. 9.9 weeks (p =
0.003)
– Reference - J Pediatr Orthop 2010 Jun;30(4):307
Operative Management of Midshaft Clavicle Fractures
Indications
● following types of clavicle fractures should be evaluated for surgery 1,2
⚬ open fractures
⚬ fractures with near skin perforation
⚬ fractures with neurovascular involvement
⚬ displaced clavicle fractures in "oating shoulder injuries
⚬ markedly displaced "clavicular sleeve" lateral physeal fractures that have poten-
tial for Y-shaped malunion of the clavicle after nonoperative management Case
Rep Orthop 2016;2016:4015212
https://www.dynamed.com/condition/clavicle-fractures-in-infants-and-children 15/02/24, 8 36 p.m.
Página 26 de 46
:
CLINICIANS' PRACTICE POINT
"Poke hole" open fractures may be irrigated in the emergency department and treated
with oral antibiotics for 5-7 days. The need for surgery in fractures with near skin perfo-
ration may depend on the degree of skin tenting. Associated neurologic or vascular in-
jury should be thoroughly evaluated to determine the appropriateness of surgery. The
need for surgery in "oating shoulder injuries depends on the fracture pattern. Grossly
unstable injuries should be !xed on both sides. Relatively stable injury patterns may
bene!t from stable !xation of either the clavicle or humerus fracture.
● need for surgery in children and adolescents with 100% displaced fractures and/or
fractures with signi!cant shortening of clavicle (> 2 cm) is controversial 2
⚬ evidence in adults showing worse functional outcomes associated with nonope-
rative management compared to open reduction and !xation supports more fre-
quent operative management of clavicle fractures in adults
⚬ switch away from nonoperative management of clavicle fractures in adults has
in"uenced management decisions in adolescents
⚬ evidence too limited to know if outcomes improved with more frequent surgical
intervention in adolescents
● in younger adolescents aged 10-14 years, severe displacement may be an indication
for surgical management severity determined at discretion of treating surgeon 2
● other factors that may prompt consideration of surgical !xation include 1
⚬ marked comminution
⚬ polytrauma
⚬ vertical bone fragment
⚬ fractures of proximal (medial) or distal (lateral) part of the clavicle
⚬ signi!cant cosmetic deformity (Transl Med UniSa 2012 Jan;2:47)
Procedures
● surgical procedures 1,2
⚬ open reduction and internal !xation with contoured plate and screw (most com-
monly used)
https://www.dynamed.com/condition/clavicle-fractures-in-infants-and-children 15/02/24, 8 36 p.m.
Página 27 de 46
:
– o#ers more rigid !xation and direct visual control of fracture fragment
– reported complications include implant irritation and prominence and chest
wall numbness
⚬ intramedullary pin !xation
– preserves soft tissue around fracture site, but not amenable to more complex
fracture patterns
– reported complications include hardware breakage, prominent hardware, skin
breakdown near hardware, and pin migration
● open reduction and internal !xation with contoured plate and screw 3
⚬ considered standard of care option in surgical treatment
⚬ performed by !rst realigning displaced clavicle fragments back to original posi-
tion with use of bone clamps; a plate is then placed on surface of clavicle where
it is aligned with bone and secured with screws
⚬ plating allows rigid !xation and rotational control over fracture; however, dama-
ge to surrounding neurovascular structures is a risk during procedure, and grea-
ter soft tissue stripping may be necessary to better visualize adjacent structures
⚬ plate considerations
– precontoured plates reported to lower risk of injury to surrounding structures,
reduce postoperative hardware complications, and provide better clinical out-
comes (compared to traditional plates)
– common plate positions are superior and anterior-inferior
● superior (traditional method)
⚬ potential advantage - permits !xation on tension side of fracture
⚬ potential disadvantages - prominent hardware with minimal soft tissue
coverage and screw trajectories toward neurovascular structures
● anterior-inferior
⚬ potential advantages - greater screw length and purchase, safer trajec-
tory of screws, reduced prominence of hardware, and decreased like-
lihood of future hardware removal
⚬ potential disadvantage - lack of !xation on tension side of fracture
– dual plating may be used
https://www.dynamed.com/condition/clavicle-fractures-in-infants-and-children 15/02/24, 8 36 p.m.
Página 28 de 46
:
● involves use of 2.7-mm or 3.5-mm reconstruction-style plate located ante-
rior-inferior, paired with 2-mm or 2.4-mm mini-fragment plate superior
● may create sti#er construct and involve less implant irritation
● Reference - J Am Acad Orthop Surg 2018 Nov 15;26(22):e468
● intramedullary !xation 3
⚬ minimally invasive procedure; small incision may cause less soft tissue dissection
⚬ performed in supine or beach-chair position
– involves drilling hole into canal of clavicle and inserting pin to hold fracture
fragments in place
– pin surgically removed 2-6 months after healing con!rmed
● Kirschner wire
⚬ should be avoided in !xation of clavicle fractures due to risk of serious complica-
tion of wire migration into vasculature as well as increased rate of infections 1
⚬ intra-aortic migration of Kirschner wire resulting in death reported in 5-year-old
boy presenting with history of syncope, shortness of breath, and chest pain 7
days after wire placement in case report (Medicine (Baltimore) 2016
May;95(21):e3741)
E"cacy
STUDY
● SUMMARY
elastic stable intramedullary nailing (ESIN) associated with similar improve-
ments in postoperative pain and function but better cosmesis compared to pla-
ting in children aged 10-14 years with displaced midshaft clavicle fractures
DynaMed Level 2
COHORT STUDY: J Orthop Traumatol 2022 Aug 22;23(1):42
Details
⚬ based on retrospective cohort study
⚬ 73 children aged 10-14 years (mean age 12 years, 60% male) who had surgery for
fully displaced midshaft clavicle fracture between 2014 and 2018 were followed
for ≥ 24 months
– 62% had ESIN with nail removal 6-9 months after surgery
https://www.dynamed.com/condition/clavicle-fractures-in-infants-and-children 15/02/24, 8 36 p.m.
Página 29 de 46
:
– 38% had plating with plate removal 9-12 months after surgery
⚬ postoperative outcomes included
– pain assessed on visual analog scale, score range 0-10 points, with higher sco-
res indicating greater pain severity
– cosmetic healing assessed on Scar Cosmesis Assessment and Rating (SCAR)
scale, score range 0-15 points, with higher scores indicating worse scarring
⚬ mean preoperative pain score was 7 points in both groups
⚬ comparing ESIN vs. plating
– mean pain scores 3 days after surgery 2.5 points vs. 2.8 points (not signi!cant)
– mean SCAR scale scores
● 3.5 points vs. 7.7 points (p < 0.001) at 3 months
● 2.9 points vs. 8.3 points (p < 0.001) 3 months after hardware removal
– cosmetic counsel sought by 22.2% vs. 71.4% (p < 0.001)
– mean length of hospital stay 1.5 days vs. 2.5 days (p < 0.001)
– mean operative time 31 minutes vs. 60 minutes (p < 0.001)
– mean incision size 2.4 cm vs. 5.4 cm (p < 0.001)
– refracture in 0% vs. 7.1% (p = 0.08)
– surgical site infection in 4.4% vs. 7.1% (not signi!cant)
⚬ no signi!cant di#erence in postoperative elbow function assessed on American
Shoulder and Elbow Surgeons scale
⚬ Reference - J Orthop Traumatol 2022 Aug 22;23(1):42
STUDY
● SUMMARY
high rate of return to full activity with minimal complications reported after open
reduction and fixation of completely displaced midshaft clavicle fractures in chil-
dren DynaMed Level 3
CASE SERIES: J Pediatr Orthop 2009 Dec;29(8):851
Details
⚬ based on case series
⚬ 24 children (mean age 12.7 years; 88% male) with completely displaced midshaft
clavicle fracture treated with open reduction and !xation were included
⚬ !xation procedures included plate and screw in 22 children, isolated screw in 1
https://www.dynamed.com/condition/clavicle-fractures-in-infants-and-children 15/02/24, 8 36 p.m.
Página 30 de 46
:
child, and Kirschner wire in 1 child
⚬ at mean follow-up of 2.2 years, 21 children had returned to complete activity; re-
maining children restricted from full activity based on parental preference
⚬ no nonunions and infections reported
⚬ complications included persistent scar sensitivity in 2 children and transient ul-
nar nerve neurapraxia secondary to initial injury in 1 child
⚬ Reference - J Pediatr Orthop 2009 Dec;29(8):851, commentary can be found in J
Pediatr Orthop 2010 Oct-Nov;30(7):746
STUDY
● SUMMARY
intramedullary fixation of displaced midshaft clavicle fractures reported to result
in return to sport at mean 18 weeks postinjury in adolescent athletes
DynaMed Level 3
CASE SERIES: J Orthop Trauma 2019 Nov;33(11):e439
Details
⚬ based on case series
⚬ 29 adolescents (aged 11.4-17.9 years) with displaced midshaft clavicle fractures
treated with intramedullary clavicle pins from 2007 to 2013 were included
⚬ 25 adolescents were student athletes
⚬ displacement > 100% occurred in 27 adolescents (93%), with mean preoperative
shortening of 18 mm
⚬ 7 adolescents had multifragmentary fractures
⚬ mean time to return to sport for student athletes 18 weeks postinjury
⚬ all adolescents had union at mean 8 weeks postinjury
⚬ Reference - J Orthop Trauma 2019 Nov;33(11):e439
STUDY
● SUMMARY
second surgery to remove hardware required in reported 28% of children with
displaced clavicle fracture after open reduction and internal fixation with plate
and screw
CASE SERIES: J Pediatr Orthop 2011 Jul-Aug;31(5):507
Details
⚬ based on case series
https://www.dynamed.com/condition/clavicle-fractures-in-infants-and-children 15/02/24, 8 36 p.m.
Página 31 de 46
:
⚬ 14 children (mean age 12.9 years) with displaced clavicle fractures treated with
open reduction and internal !xation with plate and screw were included
⚬ 12 children had been treated nonoperatively initially but ultimately had surgery
because of increased displacement at 3 weeks
⚬ 4 children had additional surgery to remove hardware
⚬ 8 children had numbness at site of injury
⚬ Reference - J Pediatr Orthop 2011 Jul-Aug;31(5):507
Comparative E"cacy of Nonoperative vs. Operative Management
STUDY
● SUMMARY
operative management may not improve function or quality of life and may in-
crease risk of complications at 2 years compared to nonoperative management in
children aged 10-18 years with completely displaced midshaft clavicle fractures
DynaMed Level 2
COHORT STUDY: Am J Sports Med 2022 Sep;50(11):3045
Details
⚬ based on cohort study
⚬ 416 children aged 10-18 years treated for completely displaced midshaft clavicle
fracture between 2013 and 2017 were followed for 2 years
⚬ 30% had operative management and 70% had nonoperative management
⚬ 282 children who had data for patient-reported outcomes at 2 years were inclu-
ded in e$cacy analysis
⚬ all children were included in safety analysis
⚬ no signi!cant di#erences between groups in shoulder function, patient satisfac-
tion, or quality of life
⚬ complication rates comparing operative management vs. nonoperative manage-
ment
– any complication in 43.2% vs. 5.5% (p < 0.001)
– any unexpected additional surgery in 10.4% vs. 1.4% (p = 0.004)
– hardware pain or irritation in 8.8% vs. 0.3% (p < 0.0001)
– sensory symptoms in 22.4% vs. 0.3% (p < 0.0001)
– delayed union in 3.2% vs. 1.4% (not signi!cant)
https://www.dynamed.com/condition/clavicle-fractures-in-infants-and-children 15/02/24, 8 36 p.m.
Página 32 de 46
:
– refracture in 4% vs. 2.1% (not signi!cant)
⚬ no super!cial or deep infection in either group
⚬ Reference - Am J Sports Med 2022 Sep;50(11):3045
● for literature reviews comparing nonoperative vs. operative management of clavicle
fractures in children and adolescents, see J Orthop Trauma 2019 Nov;33(11):e439
ahd JBJS Rev 2019 Mar;7(3):e5
Management of Distal (Lateral) Clavicle Fractures
● distal clavicle fractures in children
⚬ most often, pseudodislocation occurs as coracoclavicular ligaments remain atta-
ched to periosteum and clavicle herniates through torn periosteum
⚬ this type of injury is treated like adult acromioclavicular (AC) joint injuries
⚬ Reference - Am Fam Physician 2008 Jan 1;77(1):65, commentary can be found in
Am Fam Physician 2008 Sep 15;78(6):697
● indications for surgical treatment of distal clavicle fractures may include
⚬ signi!cant posterior displacement
⚬ exposed fractures
⚬ impact on soft tissues
⚬ risk of skin perforation
⚬ displaced fractures with a potential risk of injury to structures of the neuromus-
cular bundle or mediastinum
⚬ Reference - Rev Bras Ortop 2016 Jan-Feb;51(1):24
● duplicated clavicle resulting from distal clavicle fracture occurring at physeal-me-
taphyseal junction
⚬ periosteal sleeve in children and adolescents is osteogenic, has great capacity for
remodeling, and may !ll any gap between periosteum and metaphysis (Surg Ra-
diol Anat 2019 Apr;41(4):373)
⚬ goal of operative management may be to prevent potential formation of duplica-
ted clavicle or to address duplicated clavicle previously treated nonoperatively
(Injury 2011 Apr;42(4):376)
https://www.dynamed.com/condition/clavicle-fractures-in-infants-and-children 15/02/24, 8 36 p.m.
Página 33 de 46
:
CLINICIANS' PRACTICE POINT
Early recognition is important to avoid this complication. A#ected patients will have ten-
derness, bruising, or skin puckering in the posterior aspect of the shoulder, near the
trapezius muscle. Surgical treatment with reduction of the fracture and repair of the
periosteal sleeve results in an anatomic or near-anatomic reconstruction. A computed
tomography scan may be indicated to accurately assess the position of the clavicle sin-
ce plain x-rays often underestimate the degree of displacement.
STUDY
● SUMMARY
good long-term functional outcomes reported after operative and nonoperative
management of distal clavicle fractures in children DynaMed Level 3
CASE SERIES: Injury 2011 Apr;42(4):376
Details
⚬ based on case series
⚬ 75 children aged 3-16 years with distal clavicle fractures treated between 1983
and 2008 were included
– 63 children had nonoperative management with sling for 4 weeks, with return
to full activity at 2 months
– 12 children had open reduction and !xation with Kirschner wire, with 11 chil-
dren also having superior periosteal repair
⚬ children treated surgically had oblique displaced fracture (8), transverse displa-
ced fracture (3), and AC dislocation (1)
⚬ all fractures healed by 4 weeks postinjury
⚬ among 59 patients reexamined 2-18 years postinjury
– no patients complained of limitations in daily activities that included competi-
tive sports activities
– 5 patients treated nonoperatively complained of visible prominence at fractu-
re site
– perfect score in all 52 patients evaluated with Constant Score
– no AC arthritis or subluxation of the joint seen in any patients, including those
with true joint dislocation
– shortening of a#ected clavicle (< 2 cm) observed in 5 patients
https://www.dynamed.com/condition/clavicle-fractures-in-infants-and-children 15/02/24, 8 36 p.m.
Página 34 de 46
:
⚬ Reference - Injury 2011 Apr;42(4):376
● cannulated screw !xation technique reported to result in full range of motion at 12-
month follow-up in 3 children (aged 8-17 years) with distal clavicle fracture associa-
ted with coracoclavicular ligament rupture in case series (J Trauma 2006
Jun;60(6):1358)
Management of Medial Clavicle Fractures
● medial clavicle fractures uncommon in children
STUDY
● SUMMARY
successful closed reduction reported in adolescents with posterior sternoclavicu-
lar joint injuries treated within 24 hours of injury DynaMed Level 3
CASE SERIES: J Pediatr Orthop 2014 Jun;34(4):369
Details
⚬ based on case series
⚬ 48 adolescents aged 13-18 years with posterior sternoclavicular joint injuries
were included; 40 adolescents ultimately treated with open reduction and inter-
nal !xation, and 8 adolescents treated with closed reduction
⚬ closed reduction attempted in 22 adolescents initially but was successful in only
8 adolescents
– all 8 successful closed reductions occurred within 24 hours of injury
– 12 of 14 unsuccessful closed reductions were true dislocations
⚬ among 40 adolescents treated operatively, 50% had true sternoclavicular joint
dislocation and 50% had medial clavicle physeal fracture
⚬ sternoclavicular joint injury missed on initial presentation in 23%
⚬ Reference - J Pediatr Orthop 2014 Jun;34(4):369
STUDY
● SUMMARY
surgical management of posterior sternoclavicular joint injuries reported to re-
sult in high rate of return to full activity in adolescents DynaMed Level 3
CASE SERIES: Orthopedics 2014 Feb;37(2):e174
Details
https://www.dynamed.com/condition/clavicle-fractures-in-infants-and-children 15/02/24, 8 36 p.m.
Página 35 de 46
:
⚬ based on case series
⚬ 12 adolescent boys (mean age 14.8 years) with medial clavicular physeal fracture
or sternoclavicular dislocation followed for mean 10.3 months were asked about
long-term outcomes via mailed questionnaire
⚬ closed reduction attempted in 8 boys, but 6 boys required subsequent open re-
duction
⚬ 4 boys had open reduction
⚬ among 10 boys treated operatively, 6 had medial clavicular physeal fractures and
4 had posterior sternoclavicular dislocations
⚬ complete long-term follow-up data in 6 boys (all had been managed surgically),
with return to full activity in 100% and perfect QuickDash and Simple Shoulder
Test in 100%
⚬ Reference - Orthopedics 2014 Feb;37(2):e174
Postoperative Management
● postoperative management for midshaft clavicle fractures 2
⚬ sling for comfort worn for 2 weeks, and pendulum exercises allowed
⚬ range of motion is progressed from weeks 2 to 6
⚬ shoulder strengthening can commence at 6 weeks
⚬ contact sports can be resumed once full radiographic union and strength achie-
ved
● postoperative management for distal clavicle fractures
⚬ sling immobilization for 6 weeks
⚬ supine passive and active-assisted range-of-motion exercises begun immediately
⚬ active range-of-motion exercises started at 6 weeks
⚬ strengthening exercises beginning 6-12 weeks postoperatively
⚬ restricted from heavy labor or sports for 12 weeks
⚬ Reference - J Am Acad Orthop Surg 2011 Jul;19(7):392
● postoperative management for proximal clavicle fractures
⚬ sling immobilization for 6 weeks until healing evident on radiograph
⚬ active-assisted shoulder stretching exercises beginning at 6 weeks
⚬ strengthening exercises at about 8 weeks, with return to sports at about 10
https://www.dynamed.com/condition/clavicle-fractures-in-infants-and-children 15/02/24, 8 36 p.m.
Página 36 de 46
:
weeks postoperatively
⚬ Reference - Case Rep Orthop 2017;2017:6354284
Complications
● potential, rare complications of clavicle fracture include 3
⚬ pneumothorax (rare)
⚬ neurovascular injuries
● reported complications from nonoperative management include 1,2
⚬ symptomatic malunion including pain, fatigability, and decreased endurance of
a#ected extremity
⚬ dissatisfaction with appearance of shoulder
Prognosis
General Prognosis
● nonunions exceedingly rare in children and adolescents 2
● only reported 10%-20% of malunions after clavicle fracture in adolescents are sym-
ptomatic (J Pediatr Orthop 2016 Jun;36 Suppl 1:S41)
● uncomplicated, closed isolated midshaft clavicle fractures treated with nonoperati-
ve management generally result in good functional outcomes 1
● neonatal clavicle fractures
⚬ generally heals rapidly with pain subsiding after callus formation (usually by 7-10
days)
⚬ patients typically have excellent outcomes without any long-term complications
⚬ References - Pediatr Rev 2016 Nov;37(11):451,
STUDY
● SUMMARY
increasing age and complete displacement associated with increased risk of com-
plications in children with clavicle fracture managed nonoperatively
COHORT STUDY: J Emerg Med 2012 Jul;43(1):29
https://www.dynamed.com/condition/clavicle-fractures-in-infants-and-children 15/02/24, 8 36 p.m.
Página 37 de 46
:
Details
⚬ based on cohort study
⚬ 537 children aged 0-17 years (median age 10 years, 73% male) with clavicle frac-
tures had medical record reviewed, including radiographic review of x-rays taken
at time of injury
⚬ 40% of fractures were displaced, and fracture occurred in
– diaphyseal region in 90.7%
– lateral region in 5.4%
– medial region in 3.9%
⚬ complications occurred in 2.5% of 530 clavicle fractures treated nonoperatively,
including
– 6 refractures
– 3 delayed unions
– 3 bony protrusions causing chronic skin irritation
– 1 nonunion
⚬ factors associated with increased risk of complication
– complete displacement (odds ratio 3.2, 95% CI 1.2-8.3)
– increasing age (odds ratio 1.18, 95% CI 1.03-1.36)
⚬ Reference - J Emerg Med 2012 Jul;43(1):29
STUDY
● SUMMARY
angulated fractures associated with increased risk of refracture compared to
completely displaced fractures in children
COHORT STUDY: J Orthop Trauma 2014 Nov;28(11):648
Details
⚬ based on cohort study
⚬ 161 children < 18 years old with clavicle fractures managed nonoperatively were
included
– 120 children had angulated fractures
– 41 children had completely displaced, nonangulated fractures
⚬ refracture de!ned as new fracture treated nonoperatively ≥ 1 year after initial
https://www.dynamed.com/condition/clavicle-fractures-in-infants-and-children 15/02/24, 8 36 p.m.
Página 38 de 46
:
injury
⚬ higher refracture rate in patients with angulated fractures compared to patients
with completely displaced fractures (18% vs. 0%, p = 0.002)
⚬ patients with angulated fractures further subdivided (angulation of 40 degrees
corresponds to about 6% shortening of 2 ends of clavicle)
– less-angulated fractures (< 40 degrees)
– more-angulated fractures (≥ 40 degrees)
⚬ higher refracture rate in less-angulated fractures compared to more-angulated
fractures (26% vs. 6%, p = 0.004)
⚬ Reference - J Orthop Trauma 2014 Nov;28(11):648
Patient-reported Outcome Measures
● measures relating to shoulder function
⚬ Disabilities of the Arm, Shoulder, and Hand (DASH) score
– 30-item patient-administered questionnaire used to evaluate symptoms and
physical function
– 3 primary domains are
● physical (21 items)
● symptoms (6 items)
● social or role functions (3 items)
– 2 optional sections evaluate participation in
● sports/music (4 items)
● work activities (4 items)
– responses scored on 5-point Likert scale, ranging from
● "no di$culty" to "unable"
● "none" to "extreme"
● "no impact" to "high impact"
– function/symptom scores range from 0 to 100, with 0 being best possible sco-
re (optimal functioning) (United States population normative value for DASH
score has been reported at 10.1)
– minimal clinically important di#erence (MCID) reported to be 10.2 points
https://www.dynamed.com/condition/clavicle-fractures-in-infants-and-children 15/02/24, 8 36 p.m.
Página 39 de 46
:
– Reference - J Am Acad Orthop Surg 2010 Jul;18(7):436
⚬ Constant-Murley Score (also called Constant Score)
– outcome measure used to compare shoulder function before and after sur-
gery
– scores range from 0 to 100, with 100 being best possible score (optimal fun-
ctioning)
● 35 points derived from patient self-assessment, including pain and activities
of daily living
● 65 points derived from physical examination, including active range of mo-
tion and strength
– MCID reported to be 10.4 points
– Reference - J Shoulder Elbow Surg 2013 Dec;22(12):1650
● measures relating to pain
⚬ Numeric Rating Scale
– scores range from 0 to 10, with 0 being best possible score (no pain)
– MCID reported to be 2 points
– Reference - Pain 2001 Nov;94(2):149
⚬ Visual Analog Scale
– measured on a 10-cm line (or alternatively, a 100-mm line) representing conti-
nuum between "no pain" and worst pain"
– scores range from 0 cm to 10 cm (0 mm to 100 mm), with 0 cm (0 mm) being
best possible score (no pain)
– MCID reported to be 1.4 cm (14 mm)
– Reference - J Am Acad Orthop Surg Glob Res Rev 2018 Mar;2(3):e088
Prevention and Screening
● not applicable
Guidelines and Resources
https://www.dynamed.com/condition/clavicle-fractures-in-infants-and-children 15/02/24, 8 36 p.m.
Página 40 de 46
:
Guidelines
United States Guidelines
● American College of Radiology (ACR) Appropriateness Criteria for traumatic shoul-
der pain can be found at ACR 2017 PDF or in J Am Coll Radiol 2018
May;15(5S):S171
European Guidelines
● French National College of Gynecologists and Obstetricians (Collège National des
Gynécologues et Obstétriciens Français [CNGOF]) clinical practice guideline on
shoulder dystocia can be found in Eur J Obstet Gynecol Reprod Biol 2016
Aug;203:156
Australian and New Zealand Guidelines
● Royal Children's Hospital Melbourne (RCH) clinical practice guideline on clavicle
fractures in the emergency department can be found at RCH accessed 2023 Jul
28
Review Articles
● review of clavicle fractures in adolescents can be found in JBJS Rev 2018 Sep;6(9):e4
● review of clavicle fractures in adolescents can be found in Orthop Clin North Am
2017 Jan;48(1):47
● review of clavicle fractures in the emergency department can be found in Am J
Emerg Med 2021 Nov;49:315
● review of birth injuries in neonates can be found in Pediatr Rev 2016 Nov;37(11):451
● review of imaging and classi!cation of clavicle fractures can be found in Curr Probl
Diagn Radiol 2020 May-Jun;49(3):199
● review of management of simple clavicle fractures by primary care physicians can
be found in Clin Pediatr (Phila) 2017 May;56(5):467
https://www.dynamed.com/condition/clavicle-fractures-in-infants-and-children 15/02/24, 8 36 p.m.
Página 41 de 46
:
● review of operative versus nonoperative management of displaced midshaft clavi-
cle fractures in children can be found in Orthop Res Rev 2022;14:373
● review of upper extremity fractures in children can be found in J Pediatr Orthop
2020 Apr;40(4):e283
MEDLINE Search
● to search MEDLINE for ([Clavicle fracture] AND [infant OR child]) with targeted
search (Clinical Queries), click therapy , diagnosis , or prognosis
Patient Information
● handout from EBSCO Health or in Spanish
● handout from Victorian Paediatric Orthopaedic Network PDF
● handout from KidsHealth or in Spanish
References
General References Used
The references listed below are used in this DynaMed topic primarily to support back-
ground information and for guidance where evidence summaries are not felt to be neces-
sary. Most references are incorporated within the text along with the evidence summaries.
1. Gausden EB, Fabricant PD. Management of Clavicle Fractures in Adolescents: A Criti-
cal Analysis Review. JBJS Rev. 2018 Sep;6(9):e4.
2. Yang S, Andras L. Clavicle Shaft Fractures in Adolescents. Orthop Clin North Am.
2017 Jan;48(1):47-58.
3. Burnham JM, Kim DC, Kamineni S. Midshaft Clavicle Fractures: A Critical Review. Ort-
hopedics. 2016 Sep 1;39(5):e814-21.
4. Moverley R, Little N, Gulihar A, Singh B. Current Concepts in the Management of
Clavicle Fractures. J Clin Orthop Trauma. 2020 Feb;11(Suppl 1):S25-30.
https://www.dynamed.com/condition/clavicle-fractures-in-infants-and-children 15/02/24, 8 36 p.m.
Página 42 de 46
:
Synthesized Recommendation Grading System for DynaMed
Content
● The DynaMed Team systematically monitors clinical evidence to continuously provi-
de a synthesis of the most valid relevant evidence to support clinical decision-ma-
king (see 7-Step Evidence-Based Methodology ).
● Guideline recommendations summarized in the body of a DynaMed topic are provi-
ded with the recommendation grading system used in the original guideline(s), and
allow users to quickly see where guidelines agree and where guidelines di#er from
each other and from the current evidence.
● In DynaMed content, we synthesize the current evidence, current guidelines from
leading authorities, and clinical expertise to provide recommendations to support
clinical decision-making in the Overview & Recommendations section.
● We use the Grading of Recommendations Assessment, Development and Evalua-
tion (GRADE) to classify synthesized recommendations as Strong or Weak.
⚬ Strong recommendations are used when, based on the available evidence, cli-
nicians (without con"icts of interest) consistently have a high degree of con!den-
ce that the desirable consequences (health bene!ts, decreased costs and bur-
dens) outweigh the undesirable consequences (harms, costs, burdens).
⚬ Weak recommendations are used when, based on the available evidence, clini-
cians believe that desirable and undesirable consequences are !nely balanced,
or appreciable uncertainty exists about the magnitude of expected consequen-
ces (bene!ts and harms). Weak recommendations are used when clinicians disa-
gree in judgments of relative bene!t and harm, or have limited con!dence in
their judgments. Weak recommendations are also used when the range of pa-
tient values and preferences suggests that informed patients are likely to make
di#erent choices.
● DynaMed synthesized recommendations (in the Overview & Recommendations sec-
tion) are determined with a systematic methodology:
⚬ Recommendations are initially drafted by clinical editors (including ≥ 1 with met-
hodological expertise and ≥ 1 with content domain expertise) aware of the best
current evidence for bene!ts and harms, and the recommendations from guide-
https://www.dynamed.com/condition/clavicle-fractures-in-infants-and-children 15/02/24, 8 36 p.m.
Página 43 de 46
:
lines.
⚬ Recommendations are phrased to match the strength of recommendation.
Strong recommendations use "should do" phrasing, or phrasing implying an
expectation to perform the recommended action for most patients. Weak re-
commendations use "consider" or "suggested" phrasing.
⚬ Recommendations are explicitly labeled as Strong recommendations or Weak
recommendations when a quali!ed group has explicitly deliberated on making
such a recommendation. Group deliberation may occur during guideline deve-
lopment. When group deliberation occurs through DynaMed Team-initiated
groups:
– Clinical questions will be formulated using the PICO (Population, Intervention,
Comparison, Outcome) framework for all outcomes of interest speci!c to the
recommendation to be developed.
– Systematic searches will be conducted for any clinical questions where syste-
matic searches were not already completed through DynaMed content deve-
lopment.
– Evidence will be summarized for recommendation panel review including for
each outcome, the relative importance of the outcome, the estimated e#ects
comparing intervention and comparison, the sample size, and the overall qua-
lity rating for the body of evidence.
– Recommendation panel members will be selected to include at least 3 mem-
bers that together have su$cient clinical expertise for the subject(s) pertinent
to the recommendation, methodological expertise for the evidence being con-
sidered, and experience with guideline development.
– All recommendation panel members must disclose any potential con"icts of
interest (professional, intellectual, and !nancial), and will not be included for
the speci!c panel if a signi!cant con"ict exists for the recommendation in
question.
– Panel members will make Strong recommendations if and only if there is
consistent agreement in a high con!dence in the likelihood that desirable con-
sequences outweigh undesirable consequences across the majority of expec-
ted patient values and preferences. Panel members will make Weak recom-
mendations if there is limited con!dence (or inconsistent assessment or dis-
https://www.dynamed.com/condition/clavicle-fractures-in-infants-and-children 15/02/24, 8 36 p.m.
Página 44 de 46
:
senting opinions) that desirable consequences outweigh undesirable conse-
quences across the majority of expected patient values and preferences. No
recommendation will be made if there is insu$cient con!dence to make a re-
commendation.
– All steps in this process (including evidence summaries which were shared
with the panel, and identi!cation of panel members) will be transparent and
accessible in support of the recommendation.
⚬ Recommendations are veri!ed by ≥ 1 editor with methodological expertise, not
involved in recommendation drafting or development, with explicit con!rmation
that Strong recommendations are adequately supported.
⚬ Recommendations are published only after consensus is established with agree-
ment in phrasing and strength of recommendation by all editors.
⚬ If consensus cannot be reached then the recommendation can be published with
a notation of "dissenting commentary" and the dissenting commentary is inclu-
ded in the topic details.
⚬ If recommendations are questioned during peer review or post publication by a
quali!ed individual, or reevaluation is warranted based on new information de-
tected through systematic literature surveillance, the recommendation is subject
to additional internal review.
DynaMed Editorial Process
● DynaMed topics are created and maintained by the DynaMed Editorial Team
and Process .
● All editorial team members and reviewers have declared that they have no !nancial
or other competing interests related to this topic, unless otherwise indicated.
● DynaMed content includes Practice-Changing Updates, with support from our part-
ners, McMaster University and F1000.
Special Acknowledgements
● DynaMed topics are written and edited through the collaborative e#orts of the abo-
ve individuals. Deputy Editors, Section Editors, and Topic Editors are active in clinical
https://www.dynamed.com/condition/clavicle-fractures-in-infants-and-children 15/02/24, 8 36 p.m.
Página 45 de 46
:
or academic medical practice. Recommendations Editors are actively involved in de-
velopment and/or evaluation of guidelines.
● Editorial Team role de!nitions
Topic Editors de!ne the scope and focus of each topic by formulating a set of
clinical questions and suggesting important guidelines, clinical trials, and other
data to be addressed within each topic. Topic Editors also serve as consultants
for the internal DynaMed Editorial Team during the writing and editing process,
and review the !nal topic drafts prior to publication.
Section Editors have similar responsibilities to Topic Editors but have a broader
role that includes the review of multiple topics, oversight of Topic Editors, and
systematic surveillance of the medical literature.
Recommendations Editors provide explicit review of Overview and
Recommendations sections to ensure that all recommendations are sound,
supported, and evidence-based. This process is described in "Synthesized
Recommendation Grading."
Deputy Editors oversee DynaMed internal publishing groups. Each is
responsible for all content published within that group, including supervising
topic development at all stages of the writing and editing process, !nal review
of all topics prior to publication, and direction of an internal team.
Published by EBSCO Information Services. Copyright © 2024, EBSCO Information Services. All rights reserved. No
part of this may be reproduced or utilized in any form or by any means, electronic or mechanical, including
photocopying, recording, or by any information storage and retrieval system, without permission.
EBSCO Information Services accepts no liability for advice or information given herein or errors/omissions in the
text. It is merely intended as a general informational overview of the subject for the healthcare professional.
https://www.dynamed.com/condition/clavicle-fractures-in-infants-and-children 15/02/24, 8 36 p.m.
Página 46 de 46
:
También podría gustarte
- La anatomía de las lesiones deportivas (Color)De EverandLa anatomía de las lesiones deportivas (Color)Calificación: 4.5 de 5 estrellas4.5/5 (12)
- Memorias de México, Henrick EggersDocumento247 páginasMemorias de México, Henrick EggersRaúl Morán BetanzosAún no hay calificaciones
- Principios de tratamiento en fracturas de extremidadesDe EverandPrincipios de tratamiento en fracturas de extremidadesCalificación: 5 de 5 estrellas5/5 (3)
- Fractura de FemurDocumento4 páginasFractura de FemurJaviier EspiinozaAún no hay calificaciones
- Manual de prácticas de Neuroanatomía 2da edición: Laboratorio de morfologíaDe EverandManual de prácticas de Neuroanatomía 2da edición: Laboratorio de morfologíaAún no hay calificaciones
- Fracturas Del Miembro SuperiorDocumento118 páginasFracturas Del Miembro SuperiorGabriel Silva BarraAún no hay calificaciones
- Esguinces y LuxacionesDocumento6 páginasEsguinces y LuxacionesSergio ChangAún no hay calificaciones
- Los Vestigios de La Guerra de Corea en El Cuento El Regreso, de Emilio Díaz Valcárcel, Por Jhon Alexánder Monsalve FlórezDocumento8 páginasLos Vestigios de La Guerra de Corea en El Cuento El Regreso, de Emilio Díaz Valcárcel, Por Jhon Alexánder Monsalve FlórezJhon Monsalve100% (1)
- 8 Observo LiquidacionDocumento11 páginas8 Observo LiquidacionMilagros Velasquez valdesAún no hay calificaciones
- Miembro InferiorDocumento14 páginasMiembro Inferiormgonzalez_29100% (1)
- Contrato Compraventa DroneDocumento4 páginasContrato Compraventa DroneDaniel Castro100% (1)
- Los 8 Tipos de Líderes EjemplosDocumento5 páginasLos 8 Tipos de Líderes EjemplosFernanda Martinez0% (1)
- Hombro FlotanteDocumento11 páginasHombro FlotanteJuan IsidroAún no hay calificaciones
- Conflicto Entre Voluntad Real y Voluntad DeclaradaDocumento3 páginasConflicto Entre Voluntad Real y Voluntad Declaradacamilo100% (1)
- Codo y AntebrazoDocumento124 páginasCodo y Antebrazonaomy uribeAún no hay calificaciones
- PRACTICA 3 LESIONESTRAUMATICAS DEL HUMERO Y LA CINTURA ESCAPULAR Wendy SanchezDocumento12 páginasPRACTICA 3 LESIONESTRAUMATICAS DEL HUMERO Y LA CINTURA ESCAPULAR Wendy SanchezWendy SanchezAún no hay calificaciones
- Fractura Humero Distal en Niños y AdultosDocumento65 páginasFractura Humero Distal en Niños y Adultossteven arellanoAún no hay calificaciones
- Resumen Clases TraumatologiaDocumento54 páginasResumen Clases TraumatologiaKate CastañoAún no hay calificaciones
- Ivette de Paula, Practica #7. Lesiones Traumáticas de Pelvis, Fémur y CaderaDocumento9 páginasIvette de Paula, Practica #7. Lesiones Traumáticas de Pelvis, Fémur y CaderaIvette De PaulaAún no hay calificaciones
- CervicobraquialgiasDocumento18 páginasCervicobraquialgiasnataliaAún no hay calificaciones
- Revision BibliograficaDocumento10 páginasRevision BibliograficaC. Antonio PernasAún no hay calificaciones
- Fracturas de Escápula y ClavículaDocumento169 páginasFracturas de Escápula y ClavículaKatherine SorianoAún no hay calificaciones
- Resumen Fractura de CaderaDocumento6 páginasResumen Fractura de CaderaJaneth GomezAún no hay calificaciones
- Traumatismos Verte Part 2Documento16 páginasTraumatismos Verte Part 2Dalwan VermilusAún no hay calificaciones
- Fracturas Kine - Apuntes-1Documento46 páginasFracturas Kine - Apuntes-1jaaviandreaaAún no hay calificaciones
- Tema 16. Fractura Diáfisis Femoral y Superficies Articulares de La RodillaDocumento14 páginasTema 16. Fractura Diáfisis Femoral y Superficies Articulares de La RodillaCarlos SerranoAún no hay calificaciones
- Fracturas Del Cuello Femoral...... Musculo BlogDocumento8 páginasFracturas Del Cuello Femoral...... Musculo BlogKatherine FlorezAún no hay calificaciones
- 2dos 4 TEMAS INTENSIVO ORTOPEDIADocumento15 páginas2dos 4 TEMAS INTENSIVO ORTOPEDIAdaniela britoAún no hay calificaciones
- BenjaminBritoC - LESIONESTRAUMATICAS DEL HUMERO Y LA CINTURA ESCAPULARDocumento13 páginasBenjaminBritoC - LESIONESTRAUMATICAS DEL HUMERO Y LA CINTURA ESCAPULARBenjamin Brito CorreaAún no hay calificaciones
- Ivette de Paula-PRACTICA 6 LESIONES TRAUMÁTICAS DE LA MANODocumento6 páginasIvette de Paula-PRACTICA 6 LESIONES TRAUMÁTICAS DE LA MANOIvette De PaulaAún no hay calificaciones
- Fracturas de Cadera.Documento53 páginasFracturas de Cadera.Emmanuel Oropeza AguilarAún no hay calificaciones
- JavierRosell Practica 3 LESIONESTRAUMATICAS DEL HUMERO Y LA CINTURA ESCAPULARDocumento13 páginasJavierRosell Practica 3 LESIONESTRAUMATICAS DEL HUMERO Y LA CINTURA ESCAPULARJavier RosellAún no hay calificaciones
- FX de Clavicula y Omoplato-2.Documento39 páginasFX de Clavicula y Omoplato-2.Roberto NavarroAún no hay calificaciones
- Fracturas de Clavícula ExposicionDocumento37 páginasFracturas de Clavícula ExposicionAnonymous Kj8ABF7AAún no hay calificaciones
- 4 - Tibia y PeronéDocumento61 páginas4 - Tibia y Peronéochoa.paulaAún no hay calificaciones
- Lesiones de AntebrazoDocumento36 páginasLesiones de AntebrazoMichelle SolorioAún no hay calificaciones
- Luxacion Cadera y RodillaDocumento28 páginasLuxacion Cadera y Rodillakay guzmanAún no hay calificaciones
- 2.2 Fractura de ClaviculaDocumento3 páginas2.2 Fractura de Claviculajairocamacho2010Aún no hay calificaciones
- Traumatología de La Región EscapularDocumento20 páginasTraumatología de La Región EscapularPedro Angel del VasAún no hay calificaciones
- Fractura de Columna CervicalDocumento9 páginasFractura de Columna CervicalViqui BlancoAún no hay calificaciones
- Caso Clinico-Fractura de ClaviculaDocumento45 páginasCaso Clinico-Fractura de ClaviculaHector Moises Vilavila NoriegaAún no hay calificaciones
- Clavicula Ac 2022Documento143 páginasClavicula Ac 2022kawaki otsutsikiAún no hay calificaciones
- Cap 41 Humero DistalDocumento18 páginasCap 41 Humero DistalvictoriafkAún no hay calificaciones
- Tema 74traumatismos Vertebrales CompletoDocumento32 páginasTema 74traumatismos Vertebrales CompletoOmar AntonioAún no hay calificaciones
- Fractura y Luxofractura de Columna CervicalDocumento16 páginasFractura y Luxofractura de Columna CervicalSebastian CarusoAún no hay calificaciones
- 2 Fracturas de La Escápula y La ClavículaDocumento13 páginas2 Fracturas de La Escápula y La ClavículaBrenda Lizbeth Garay YabrAún no hay calificaciones
- Fracturas y Luxaciones de Miembro SuperiorDocumento44 páginasFracturas y Luxaciones de Miembro SuperiorVanessa VargasAún no hay calificaciones
- Clase 4 Fractura de Miembro Superior 1Documento35 páginasClase 4 Fractura de Miembro Superior 1Bélice Yupanqui BustamanteAún no hay calificaciones
- FX Patillo TibialDocumento11 páginasFX Patillo TibialAnibal MongeAún no hay calificaciones
- Tema 10 Fracturas y Luxaciones de La Cintura EscapularDocumento17 páginasTema 10 Fracturas y Luxaciones de La Cintura EscapularCarlos SerranoAún no hay calificaciones
- Traumatologia PDFDocumento11 páginasTraumatologia PDFKenneddy D. YaugerAún no hay calificaciones
- Clase N°13 TraumatologíaDocumento16 páginasClase N°13 TraumatologíaPaola Massai MontanerAún no hay calificaciones
- Fracturas de Miembro Superior Final.Documento15 páginasFracturas de Miembro Superior Final.janaAún no hay calificaciones
- RAFI, Fractura de Humero Con Placa y Tornillo, Fractura de Humero Con Clavo Centro MedularDocumento31 páginasRAFI, Fractura de Humero Con Placa y Tornillo, Fractura de Humero Con Clavo Centro MedularDaniel Angeles MartinezAún no hay calificaciones
- Fracturas de Clavícula y Lesiones Alrededor Del HombroDocumento74 páginasFracturas de Clavícula y Lesiones Alrededor Del Hombrokaterine vargasAún no hay calificaciones
- Clase 10Documento20 páginasClase 10Marco Antonio Sanchez BetetaAún no hay calificaciones
- Pabellón 2Documento56 páginasPabellón 2Allison ContrerasAún no hay calificaciones
- Fracturas de Miembros Superior e InferioresDocumento30 páginasFracturas de Miembros Superior e InferioresAndrade Laura100% (3)
- Fracturas de Clavícula-Traumatología PDFDocumento3 páginasFracturas de Clavícula-Traumatología PDFJosé Miguel Villavicencio SainzAún no hay calificaciones
- Fractura de La PelvisDocumento5 páginasFractura de La PelvisLorenita Martínez PinchiAún no hay calificaciones
- Fracturas de ClavículaDocumento14 páginasFracturas de Clavículafrailyn garciaAún no hay calificaciones
- FX ClaviculaDocumento29 páginasFX ClaviculaBruno HamstercitoAún no hay calificaciones
- Fractura Del Cuello Del Fémur y de La Región TrocantereaDocumento5 páginasFractura Del Cuello Del Fémur y de La Región TrocantereaNaty Galarce Ortiz0% (1)
- 420-2014-03!28!16 Traumatismos Codo y AntebrazoDocumento12 páginas420-2014-03!28!16 Traumatismos Codo y AntebrazojordyAún no hay calificaciones
- Miembro SuperiorDocumento124 páginasMiembro SuperiorAlicia MoraAún no hay calificaciones
- FOL Ud05Documento20 páginasFOL Ud05jcc1981Aún no hay calificaciones
- Expel 06282201700764 20572410 16122023Documento50 páginasExpel 06282201700764 20572410 16122023sata6_5Aún no hay calificaciones
- ONU Técnicas de EntrevistaDocumento23 páginasONU Técnicas de EntrevistaJorge NavarroAún no hay calificaciones
- Informe Sipiav 2020Documento13 páginasInforme Sipiav 2020ElPaisUyAún no hay calificaciones
- De-964 Derecho Privativo Militar Policial B GDocumento4 páginasDe-964 Derecho Privativo Militar Policial B GHelbert CamposAún no hay calificaciones
- Cruz Roja Internacional y Convenios de GinebraDocumento7 páginasCruz Roja Internacional y Convenios de GinebraJUEGOBARAún no hay calificaciones
- Nueva España PinturaDocumento9 páginasNueva España PinturaDavid RomeroAún no hay calificaciones
- GreciaDocumento2 páginasGreciaevelin rocca ayquiAún no hay calificaciones
- Cómo Tratar Con Personas DifícilesDocumento76 páginasCómo Tratar Con Personas DifícilesJose Leguim AllesemacAún no hay calificaciones
- Medidas Sustitutivas de Prision Preventiva 2021Documento7 páginasMedidas Sustitutivas de Prision Preventiva 2021Alex MelendezAún no hay calificaciones
- Tercera Entrega - Hab. NegDocumento11 páginasTercera Entrega - Hab. NegCindy FonsecaAún no hay calificaciones
- Sesic3b3n 15 Compartiendo Mis Ideas Sobre El Deseo Sexual3Documento5 páginasSesic3b3n 15 Compartiendo Mis Ideas Sobre El Deseo Sexual3J Diego SaldañaAún no hay calificaciones
- Boletín Del Ejército #02 OCRDocumento106 páginasBoletín Del Ejército #02 OCRPablo Thomasset TrakaloAún no hay calificaciones
- Justicia ComunitariaDocumento4 páginasJusticia ComunitariaEspinoza Villafuerte Luis AlbertoAún no hay calificaciones
- Ejercicios de Conteo de Figuras Pagina EducativaDocumento10 páginasEjercicios de Conteo de Figuras Pagina EducativaJasseli Carranza Abad100% (1)
- Acta de EsponsalesDocumento1 páginaActa de Esponsalesemma carrizoAún no hay calificaciones
- Un Corazon CargadoDocumento2 páginasUn Corazon CargadohaideeAún no hay calificaciones
- Hseq - For.021 Fmedevac - Base OasisDocumento12 páginasHseq - For.021 Fmedevac - Base OasisPaola Andrea Quintero RamirezAún no hay calificaciones
- Las Aventuras de Sherlock Holmes (Sin Terminar)Documento4 páginasLas Aventuras de Sherlock Holmes (Sin Terminar)Cristobal Rivera YungeAún no hay calificaciones
- Garcia - 1130901 - 21032021 - UVA 4Documento3 páginasGarcia - 1130901 - 21032021 - UVA 4Eze GarcíaAún no hay calificaciones
- Inventario de Bienes Muebles Escolares 2009Documento220 páginasInventario de Bienes Muebles Escolares 2009José Luis Fernández100% (1)
- Formato Informe MensualDocumento1 páginaFormato Informe MensualPaola RuilobaAún no hay calificaciones
- Informe El Error en El Acto JuridicoDocumento14 páginasInforme El Error en El Acto JuridicoAnnder Velásquez VásquezAún no hay calificaciones
- Modelo de Poder (Representación)Documento13 páginasModelo de Poder (Representación)Jennifer Rubi Lopez AlvaAún no hay calificaciones