Documentos de Académico
Documentos de Profesional
Documentos de Cultura
Joint Mobilization
Cargado por
marcelo_haranoDescripción original:
Derechos de autor
Formatos disponibles
Compartir este documento
Compartir o incrustar documentos
¿Le pareció útil este documento?
¿Este contenido es inapropiado?
Denunciar este documentoCopyright:
Formatos disponibles
Joint Mobilization
Cargado por
marcelo_haranoCopyright:
Formatos disponibles
University of Oklahoma Health Sciences Center Division of Rehabilitation Sciences
Evaluations & Interventions I PHTH/OCTH 7233 Spring
PRINCIPLES OF JOINT MOBILIZATION by Vince Lepak, PT, MPH, CWS Lectures 1 & 2 HISTORICAL DEVELOPMENTS -Hippocrates 460 - 380 BC -Galan 131 - 202 AD - Bonesetters vs. Physicians - 17th and 18th centuries - During the 19th century 2 categories of healers: - Osteopathy - Andrew Still -1892 Law of the Artery - Chiropractic - Daniel Palmer, a grocery worker and former patient of Dr. Still - 1895 Law of the Nerve - Allopathic medicines knowledge of using manual therapy was furthered by two physicians James Mennell and Cyriax. Physical therapists have a published record of practicing manipulation dating from the 1920s to the present. Physical therapy journals and medical journals from the 1920s to the present contain more than a thousand articles on manipulation and mobilization by physical therapists. The U.S. Clinical Practice Guideline Acute Low Back Problems in Adults based its recommendations for spinal manipulation on clinical trials. The professions who provided spinal manipulation for those studies were physical therapists (6 studies), medical doctors (4), osteopaths (2), and chiropractors (2). (AHCPR, 1994) Physical therapists, Doctors or Osteopathy, Doctors of Allopathy, are trained to use mobilization and manipulation to treat disorders of the back, neck, arm, or leg. The public is safe in the hands of physical therapists who provide mobilization and manipulation services. Two of the nation's largest physical therapist liability insurers (Maginnis and Associates and Kirke-Van Orsdel) found no evidence of higher claims loss due to physical therapists utilizing manipulative or mobilization procedures. MOBILIZATION Definition: - passive by the therapist - slow - patient can stop the movement - oscillatory or sustained - aimed at decreasing pain and/or increasing mobility
MANIPULATION - Definition: - high velocity, low amplitude thrust (non-oscillatory) performed by the therapist
ACCESSORY AND PHYSIOLOGICAL MOVEMENTS - Physiologic movements - can be done actively by patient or passively by therapist.
Page 1 of 5
- Accessory movements - movements within the joint and surrounding tissues that are necessary for full ROM but cannot be performed actively in isolation: - Joint play - movements not under voluntary control but necessary to full painless joint function - cannot be achieved actively, no active movement or contraction of a muscle can reproduce it - Component movements - accompany active movements and are necessary for active full painless joint motion. *These concepts help us compartmentalize. Nevertheless, they are not necessarily mutually exclusive when they describe the accessory movements at each joint. - Importance of treating accessory movements vs. simply using physiological movements to maintain/improve ROM ACCESSORY MOVEMENTS include: (Tomberlin & Saunders, 1995; Hertling & Kessler, 1996) 1. Spin - rotation around a stationary axis 2. Roll - New points on one articular surface meet new points on opposing articular surface. 3. Glide - Same point on one articular surface encounters new points on opposing articular surface - pure glide never occurs because no joint surfaces are completely congruent - RULE OF CONVEXITY/CONCAVITY: - if moving surface is concave - glide occurs in same direction as bone movement - if moving surface is convex - glide occurs in opposite direction of bone movement 4. Compression - decreased space between articular surfaces 5. Traction - Separation of bony surfaces
PRINCIPLE OF JOINT MOBILIZATIONS (Tomberlin & Saunders, 1995; Hertling & Kessler, 1996) 1. Place joint in resting position Closed pack position - maximal congruency & compression of the articular surfaces - the ligaments and capsule are taut Loose pack position - Any position that is not close packed. 2. Determine treatment plane: Draw a line over the articular surface of the concave joint partner. When the concave surface is moving the treatment plane moves but when the convex surface is moving the treatment plane remains the same. - Gliding - Move the joint surface parallel to the treatment plane. - Traction and compression - Move the joint surface perpendicular to the treatment plane.
3. 4. 5. 6. 7. 8. 9.
Determine direction of mobilization using concave/convex rule. Patient and body part well supported Patient and therapist relaxed Mobilizing force should be close to therapists center of gravity Compare involved extremity to uninvolved. Check one joint at a time, one movement at a time Stabilize one bone and mobilize the other. Usually stabilize proximal bone. Contact should not be painful.
10. Therapists hands should be as close to joint surfaces as possible. 11. When possible work with force of gravity rather than against it. 12. Stop the mobilization test or treatment if too painful. 13. Initial mobs are in the loose pack position. 14. Treat deficiencies in joint play before attempting to treat component motions. 15. Assess before and after treatment. ASSESSING PHYSIOLOGICAL & ACCESSORY MOVEMENTS 1. 2. Quantity Quality of motion Note where in the range pain was felt and where in the range resistance was felt. End Feel
INDICATIONS FOR JOINT MOBILIZATIONS (not an inclusive list) 1. Pain 2. Subluxation or Dislocation 3. Joint Hypomobility - majority of the time treating a capsular pattern Definition of a Capsular Pattern: Irritation of the joint capsule or the synovium producing characteristic, proportional limitation of movement.
ABSOLUTE CONTRAINDICATIONS TO JOINT MOBILIZATIONS (not an inclusive list) Malignancy Rheumatoid collagen necrosis Fracture - recent or unhealed Joint ankylosis Vertebrobasilar insufficiency
Page 3 of 5
Active inflammatory or infective arthritis
RELATIVE CONTRAINDICATIONS TO JOINT MOBILIZATIONS (not an inclusive list) Osteoporosis Pregnancy History of malignancy Hypermobility Dizziness Neurological signs Spondylolisthesis
TREATMENT VARIABLES 1. 2. 3. 4. 5. Position of joint Direction of mobilization Type - sustained or oscillatory Grade of mobilization Length of mobilization
SUSTAINED VS. OSCILLATORY MOBILIZATION Oscillatory - passive oscillatory movements, two or three per second, of small or large amplitude, and applied anywhere in a range of movement. Sustained - sustained stretching often with tiny amplitude oscillations at the limit of the range.
MAITLANDS GRADES OF OSCILLATORY MOBILIZATIONS Grade I Grade II Small amplitude movement performed at the beginning of the range. Large-amplitude movement performed within the range but not reaching the limit of the range. It can occupy any part of the range that is free of any stiffness or muscle spasm. Large amplitude movement performed up to the limit of the range.
Grade III
Grade IV
Small amplitude movement performed at the limit of the range
MANIPULATION (non-oscillatory motion) Grade V High velocity thrust performed at the limit of the range
When pathology or a mechanical disorder limits the range of movement, the grades are decreased in range. Generally, grades I and II treat pain, while grade III maintains ROM, and grade IV increases ROM. SUSTAINED (TRACTION) MOBILIZATIONS Grade I Small amplitude movement with no appreciable movement. Nullifies the normal compression forces.
Page 4 of 5
Grade II
Sustained movement performed within the ROM to the restriction. The ligaments and joints capsule are taut. The slack is taken up. Sustained movement performed at the end of the ROM through the restriction.
Grade III
DURATION OF MOBILIZATION Sustained - continue mobilization for 20 - 30 seconds Oscillatory - continue mobilization for 60 - 90 seconds
PROPOSED EFFECTS OF JOINT MOBILIZATIONS Pain relief - Stimulation of mechanoreceptors causing increased proprioceptive input to the spinal cord, thereby inhibiting transmission of pain impulses to the anterior horn cells and higher centers. Increase extensibility of joint capsule. Breaking adhesions Stretching the capsule Disrupt abnormal cross-linking Elastic vs. Plastic deformation Can morphological changes occur in the short time that joint mobilizations are applied?
REFERENCES: Hertling, D., & Kessler, R. M. (1996). Management of common musculoskeletal disorders (3rd ed.). Philadelphia: Lippincott. Kaltenborn, F. M. (1989). Manual mobilization of extremity joints: Basic examination. Minneapolis, MN: OTPT. Kisner, C. & Colby L. A. (1996). Therapeutic exercise: Foundations and techniques (3rd ed.). Philadelphia: F. A. Davis. Maitland, G.D. (1977). Peripheral Manipulation. (2nd ed.). London: Butterworths. Maitland, G.D. (1986). Vertebral Manipulation. (5th ed.). London: Butterworths. Nordin, M. & Frankel, V. H. (1989). Basic biomechanics of the musculoskeletal system (2nd ed.). Philadelphia: Lea & Febiger. Randall, T., Portney, L., & Harris, B. A. (1992, July). Effects of joint mobilization on joint stiffness and active motion of the metacarpal-phalangeal joint. Journal of Orthopedic and Sports Medicine, 16 (1), 30-36. Tomberlin, J. P. & Saunders, D. H. (1995). Evaluation, treatment and prevention of musculoskeletal disorders: Extremities (3rd ed., Vol. 2). Chaska, MN: Educational Opportunities.
Page 5 of 5
También podría gustarte
- Kaltenborn MobilizationDocumento40 páginasKaltenborn MobilizationjayadevanAún no hay calificaciones
- Length Tension Testing Book 2, Upper Quadrant: A Workbook of Manual Therapy TechniquesDe EverandLength Tension Testing Book 2, Upper Quadrant: A Workbook of Manual Therapy TechniquesCalificación: 1 de 5 estrellas1/5 (1)
- Length Tension Testing Book 1, Lower Quadrant: A Workbook of Manual Therapy TechniquesDe EverandLength Tension Testing Book 1, Lower Quadrant: A Workbook of Manual Therapy TechniquesCalificación: 3.5 de 5 estrellas3.5/5 (3)
- Releasing the Rotator Cuff: A complete guide to freedom of the shoulderDe EverandReleasing the Rotator Cuff: A complete guide to freedom of the shoulderAún no hay calificaciones
- Kinesiology Taping for Rehab and Injury Prevention: An Easy, At-Home Guide for Overcoming Common Strains, Pains and ConditionsDe EverandKinesiology Taping for Rehab and Injury Prevention: An Easy, At-Home Guide for Overcoming Common Strains, Pains and ConditionsCalificación: 4.5 de 5 estrellas4.5/5 (3)
- The Kinetic Chain Approach To PainDocumento4 páginasThe Kinetic Chain Approach To PaincharbelhannaAún no hay calificaciones
- Interferential Therapy Sept 08Documento8 páginasInterferential Therapy Sept 08api-19753815100% (1)
- Dry Needling Course Level 1 16-17 March 2020Documento4 páginasDry Needling Course Level 1 16-17 March 2020mantopt6Aún no hay calificaciones
- Effects of Maitland Mobilization and Mul PDFDocumento6 páginasEffects of Maitland Mobilization and Mul PDFKuroha Hagane KunAún no hay calificaciones
- Multifidus ExercicesDocumento2 páginasMultifidus Exercicesjo21cu100% (1)
- Myofascial ReleaseDocumento8 páginasMyofascial Releaseprokin_martinezAún no hay calificaciones
- Proprioceptive Neuromuscular FacilitationDocumento69 páginasProprioceptive Neuromuscular Facilitationvenkata ramakrishnaiah100% (1)
- MWM's On Painful ShouldersDocumento6 páginasMWM's On Painful Shouldersrudhras22Aún no hay calificaciones
- PNF Techniques 3rd SessionDocumento59 páginasPNF Techniques 3rd SessionBasma T. Zewar100% (1)
- Maitland Joint MobilizationDocumento1 páginaMaitland Joint Mobilizationapi-289275035Aún no hay calificaciones
- What Is PhysiotherapyDocumento61 páginasWhat Is PhysiotherapySharikh NorazrinAún no hay calificaciones
- C!"CCC C C C CC CC CCCDocumento13 páginasC!"CCC C C C CC CC CCCRaji JesurajAún no hay calificaciones
- What Is Shock Wave Therap 2Documento7 páginasWhat Is Shock Wave Therap 2api-457017927Aún no hay calificaciones
- ISMST GuidelinesDocumento112 páginasISMST GuidelinesDhrubo TaraAún no hay calificaciones
- Manual Therapy Techniques Guide - McKenzie, Mulligan, Kaltenborn Methods ExplainedDocumento78 páginasManual Therapy Techniques Guide - McKenzie, Mulligan, Kaltenborn Methods ExplainedHitesh RohitAún no hay calificaciones
- PAE 5 Techniques of The Treatment With Faradic Type Current-1Documento35 páginasPAE 5 Techniques of The Treatment With Faradic Type Current-1Huzaifa HabibAún no hay calificaciones
- PAE 1 Introduction To ElectrotherapyDocumento37 páginasPAE 1 Introduction To ElectrotherapyHasnat AhmedAún no hay calificaciones
- Active and Passive InsufficiencyDocumento25 páginasActive and Passive Insufficiencydina sharafAún no hay calificaciones
- A Patients Guide To Plantar Fasciitis Heel PainDocumento4 páginasA Patients Guide To Plantar Fasciitis Heel PainJacobfranAún no hay calificaciones
- Kinetic Control Cap1Documento17 páginasKinetic Control Cap1Yennifer Serna MoncadaAún no hay calificaciones
- Pain and Pain Gate Control MechanismDocumento17 páginasPain and Pain Gate Control MechanismKapil LakhwaraAún no hay calificaciones
- Turocy StainCounterstrain LabPATS06ADocumento53 páginasTurocy StainCounterstrain LabPATS06Awillone08Aún no hay calificaciones
- ESWTDocumento16 páginasESWTPrahoveanu IoanaAún no hay calificaciones
- Physiotherapy Rehabilitation Guidelines - Lumbar DisectomyDocumento6 páginasPhysiotherapy Rehabilitation Guidelines - Lumbar Disectomyalina4891Aún no hay calificaciones
- Shoulder Special TestsDocumento36 páginasShoulder Special TestsNidal HusseinAún no hay calificaciones
- MC Kenzie: Diagnostic, Prognostic, Therapeutic, and ProphylacticDocumento19 páginasMC Kenzie: Diagnostic, Prognostic, Therapeutic, and ProphylacticEvaAún no hay calificaciones
- The Spencer TechniqueDocumento11 páginasThe Spencer TechniqueDavidAgelliAún no hay calificaciones
- Pathomechanics of the Shoulder: Factors, Causes, EffectsDocumento27 páginasPathomechanics of the Shoulder: Factors, Causes, EffectsVenkat RamanaAún no hay calificaciones
- Therapybook Interferencial TherapyDocumento34 páginasTherapybook Interferencial TherapyBrian RaymondAún no hay calificaciones
- The Cyriax Method of MSK Examination ROMDocumento78 páginasThe Cyriax Method of MSK Examination ROMMittulAún no hay calificaciones
- Rene Cailliet - Shoulder Pain PDFDocumento170 páginasRene Cailliet - Shoulder Pain PDFm alfin alfauziAún no hay calificaciones
- Application of Fascial Manipulation Technique in Chronic Shoulder Pain Ok PDFDocumento8 páginasApplication of Fascial Manipulation Technique in Chronic Shoulder Pain Ok PDFBruno DiasAún no hay calificaciones
- Introduction PhysiotherapistDocumento12 páginasIntroduction Physiotherapistapi-371068989Aún no hay calificaciones
- Clinical Neurodynamics and Sports Medicine: Origins and DevelopmentDocumento8 páginasClinical Neurodynamics and Sports Medicine: Origins and DevelopmentWahid NasrudinAún no hay calificaciones
- Effectiveness of Mulligan's Mobilization Technique Versus Eccentric Exercises On Pain, Hand Grip Strength and Function in Subjects With Lateral EpicondylitisDocumento8 páginasEffectiveness of Mulligan's Mobilization Technique Versus Eccentric Exercises On Pain, Hand Grip Strength and Function in Subjects With Lateral EpicondylitisInternational Journal of Innovative Science and Research TechnologyAún no hay calificaciones
- Physio Shacklock 95Documento8 páginasPhysio Shacklock 95Raihan HabibAún no hay calificaciones
- ElectrotherapyDocumento11 páginasElectrotherapyabdul azizAún no hay calificaciones
- Mulligan Spinal Concept PDFDocumento7 páginasMulligan Spinal Concept PDFRabbeya AltafAún no hay calificaciones
- Lec 6 AcompareDocumento2 páginasLec 6 AcomparematshAún no hay calificaciones
- Dry Needling in The Management of Musculoskeletal Pain: Leonid Kalichman, PT, PHD, and Simon Vulfsons, MDDocumento7 páginasDry Needling in The Management of Musculoskeletal Pain: Leonid Kalichman, PT, PHD, and Simon Vulfsons, MDLuis Gustavo PetroskiAún no hay calificaciones
- Cervical Spine EvaluationDocumento9 páginasCervical Spine EvaluationS.Muhaymen HussainAún no hay calificaciones
- Musculoskeletal ExaminationDocumento42 páginasMusculoskeletal ExaminationMaghfirahEkasariLaitjinaraAún no hay calificaciones
- Measurement and Scales Used in PhysiotherapyDocumento38 páginasMeasurement and Scales Used in PhysiotherapyAnurag BhuyanAún no hay calificaciones
- Manual Therapy Techniques For The ShoulderDocumento12 páginasManual Therapy Techniques For The ShoulderadhikarisamirAún no hay calificaciones
- PathomechanicsDocumento8 páginasPathomechanicsMike B AndersonAún no hay calificaciones
- Ijspt-Biomechanics and Pathomechanics of The Patellofemoral JointDocumento11 páginasIjspt-Biomechanics and Pathomechanics of The Patellofemoral JointDevi MigiekaAún no hay calificaciones
- Sample Chapter 7 Therapeutic Mod Ali TiesDocumento28 páginasSample Chapter 7 Therapeutic Mod Ali Tiesmdarif4ptAún no hay calificaciones
- Basic of Geriatrics and Internal Medicine For PhysiotherapistDocumento128 páginasBasic of Geriatrics and Internal Medicine For PhysiotherapistDoha EbedAún no hay calificaciones
- 9 Pregnancy Stretches For The Whole Body 4 Pager Apr17 v3Documento4 páginas9 Pregnancy Stretches For The Whole Body 4 Pager Apr17 v3LeiltonAún no hay calificaciones
- Physical Therapy (PT), Also Known As PhysiotherapyDocumento7 páginasPhysical Therapy (PT), Also Known As PhysiotherapyKarolina DudaAún no hay calificaciones
- Drugs Used in Current Physical Therapy PracticeDocumento22 páginasDrugs Used in Current Physical Therapy PracticeAngelic khanAún no hay calificaciones
- Effects of Petrissage Massage On Fatigue and ExercDocumento8 páginasEffects of Petrissage Massage On Fatigue and ExercJGRBBKDVRAún no hay calificaciones
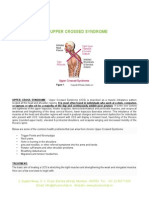
- Upper Crossed SyndromeDocumento3 páginasUpper Crossed SyndromeFleur Vella100% (1)