Documentos de Académico
Documentos de Profesional
Documentos de Cultura
1109 Case 1
Cargado por
willygopeDescripción original:
Derechos de autor
Formatos disponibles
Compartir este documento
Compartir o incrustar documentos
¿Le pareció útil este documento?
¿Este contenido es inapropiado?
Denunciar este documentoCopyright:
Formatos disponibles
1109 Case 1
Cargado por
willygopeCopyright:
Formatos disponibles
doi:10.1111/j.1750-3639.2009.00362.
x
COM NOVEMBER 2009 CASE 1 bpa_362 507..510
A 76-YEAR-OLD WOMAN WITH PARAPLEGIA
Jan Rémi, Thomas Pfefferkorn, Fatima B. König, Hans Lassmann, Wolfgang Brück,
Markus Holtmannspötter, Andreas Straube, Hans A. Kretzschmar and Ulrich Schüller
From the Departments of Neurology (J.R., T.P., A.S.), Neuroradiology (M.H.), Neuropathology (H.A.K., U.S.) of the University of Munich, Germany,
the Department of Neuropathology of the University Medical Center of Göttingen, Germany (F.B.K., W.B.), and the Center for Brain Research of the
University of Vienna, Austria (H.L.).
Over the three and a half years prior to admission, the patient had
CLINICAL HISTORY AND unintentionally lost 10–15 kg of body weight, and there had been
NEUROIMAGING an extensive work-up for a neoplasm which yielded no specific
A 76 year old woman was admitted to a spinal trauma hospital after a pathological results. A bone-marrow biopsy three years ago had not
collapse at home with paraplegia and total loss of deep tendon retrieved enough bone marrow cells at that time to be conclusive,
reflexes of unknown duration. Upon admission she was responsive the blood leukocyte levels in the previous three years were around,
but not well orientated. A spinal MRI showed T2 signal enhance- the high normal limit (but never above). Her other past medical
ment from Th4 to L2, without revealing evidence of the etiology. history was non-contributory.
Over the course of the next 3 days her mental status decreased to
where she could only be woken up with strong pain stimuli. Leuko-
cytosis (30.3 G/l) and fever (39°C) were noted. In a cerebral com-
puted tomography, several hypodense white matter lesions were
PATHOLOGY
visible. The cerebrospinal fluid (CSF) contained 61 cells/ml with The post mortem analysis secured the diagnosis of an acute
3.33 g/l protein and 1.8 mmol/l glucose (serum: 6.0 mmol/l) and myeloid leukemia (AML, sub-type M2) in bone marrow, spleen
treatment with broad spectrum antibiotics and glucocorticosteroids (weight: 380 g) and liver. No other neoplasm was found. The analy-
was started. sis of brain tissue revealed large, partly confluent lesions in the
On hospital day 5 she was transferred to our neurological inten- white matter of both cerebral hemispheres as well as the spinal
sive care unit because of deteriorating mental status and the need cord. A representative gross image is shown in Figure 2 demon-
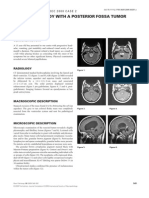
for mechanical ventilation. On day 12, an axial FLAIR-weighted strating a well-demarcated lesion in the right occipital lobe. Dis-
MRI showed large confluent white matter lesions in the brain tinct lesional areas within the cerebral white matter are visible in a
(Figure 1). Similar abnormalities were found in the spinal cord. Luxol-Fast-Blue stain (Figure 3). Axonal destruction varied, but
The lesions showed no signal enhancement on diffusion weighted was severe in some areas. GFAP+ reactive astrocytes and macroph-
imaging, but had patchy gadolinium contrast enhancement. CSF ages with LFB-positive material (Figure 3, insert) were detectable
cell, protein and glucose levels remained stable over several lumbar throughout the lesions. C9neo+ complement deposits were also
punctures, and CSF specific antibody production was shown with present at some sites (Figure 4, brown signal). Blood vessels as
CSF specific oligoclonal bands. Microbiological CSF analyses well as perivascular spaces within the lesions were packed with
were negative for bacterial or viral pathogens, including JC-virus myeloblasts (Figure 5). The spread of myeloblasts was most severe
and enteroviruses. Anti-aquaporin 4 antibodies were not detectable. within the lesions, but they could also be found throughout the
The peripheral leukocytosis of her blast crisis peaked at 102 G/l. whole brain parenchyma outside the lesions.
No BCR-ABL rearrangement was detectable. The patient’s condi- What is the diagnosis?
tion continued to deteriorate despite anti-microbial and steroid
treatment. The patient died on hospital day 16.
Figure 1. Figure 2.
Brain Pathology 20 (2010) 507–510 507
© 2010 The Authors; Journal Compilation © 2010 International Society of Neuropathology
Correspondence
Figure 3.
Figure 4.
508 Brain Pathology 20 (2010) 507–510
© 2010 The Authors; Journal Compilation © 2010 International Society of Neuropathology
Correspondence
Figure 5.
Brain Pathology 20 (2010) 507–510 509
© 2010 The Authors; Journal Compilation © 2010 International Society of Neuropathology
Correspondence
after and be related to the CNS spread of myeloblastic leukemic
DIAGNOSIS cells. Whether immunosuppression itself may trigger acute demy-
CNS spread of untreated acute myeloid leukemia associated with elination or exacerbation of a chronic multiple sclerosis or whether
acute demyelination further mechanisms of immune system modulation related to AML
are involved in the reported scenario need to be investigated in
further studies and experimental settings. By all means, we believe
DISCUSSION that our case strengthens the need to strictly monitor CNS functions
C9neo+ complement deposits were also present at sites of active of AML patients.
demyelination (Figure 4, brown signal). This is a pattern of pathol-
ogy that is typically seen in the antibody- and complement-
mediated pattern II of multiple sclerosis lesions according to the REFERENCES
classification scheme of Lucchinetti et al (4). 1. Jaster JH, Dohan FC Jr, O’Brien TF (2003) Demyelination in the brain
Patients suffering from leukemias may develop CNS complica- as a paraneoplastic disorder: candidates include some cases of
tions of their disease. Spread of the disease into the central nervous leukemia and non-Hodgkin’s lymphoma. Ann Hematol 82:714–5.
system (CNS) is a rare example, which is generally less frequent in 2. Johnston DL, Alonzo TA, Gerbing RB, Lange BJ, Woods WG (2005)
adults than in children (2, 8), and particularly uncommon in Risk factors and therapy for isolated central nervous system relapse of
untreated patients, where only single cases are reported (5). pediatric acute myeloid leukemia. J Clin Oncol 23:9172–8.
Leukoencephalopathy is more common and potentially life- 3. Kesari S, Akar S, Saad A, Drappatz J, Koralnik IJ, DeAngelo DJ
(2008) Progressive multifocal leukoencephalopathy in a patient with
threatening. It may have several different etiologies, for example
relapsed acute myelogenous leukemia. J Clin Oncol 26:3804–7.
demyelination as a paraneoplastic disorder (1), progressive multi- 4. Lucchinetti C, Brück W, Parisi J, Scheithauer B, Rodriguez M,
focal leukoencephalopathy after a JC-virus infection (3) or multi- Lassmann H (2000) Heterogeneity of multiple sclerosis lesions:
focal necrotizing leukoencephalopathy after chemotherapy (6). implications for the pathogenesis of demyelination. Ann Neurol
However, as these examples illustrate, reports on leukoencephal- 47:707–17.
opathy in relation to leukemia may be ambiguous because the 5. Maynor ML (1989) Neurological manifestations as the initial
patients typically receive treatment with potential neurotoxicity. presentation of acute myelogenous leukemia. Am J Emerg Med
Recently, a CNS relapse of an AML associated with leukoen- 7:481–4.
cephalopathy was suggested in an adult patient that had only been 6. Robb J, Chalmers L, Rojiani A, Chamberlain M (2006) Multifocal
treated with cytarabine, which is not thought to penetrate the CNS, necrotizing leukoencephalopathy: An unusual complication of acute
leukemia. Arch Neurol 63:1028–9.
making a neurotoxic effect unlikely (7). MRI in that patient showed
7. Schumann, M., Kiewe P, Hartlieb S, Neumann M, Schilling A, Koch
widespread leukoencephalopathy, but there was only indirect HC et al. Diffuse Leukoencephalopathy and Brain Edema: Unusual
evidence for a role of a parenchymal CNS spread of the AML. Presentations of CNS Relapse of Acute Myeloid Leukemia. J
Myeloblasts were found in the CSF and the leukoencephalopathy Neuroimaging, (e-pub ahead of print) DOI:
improved after chemotherapy, but no brain tissue was examined. 10.1111/j.1552-6569.2008.00300.x.
That patient could be discharged without any neurological 8. Stewart DJ, Keating MJ, McCredie KB, Smith TL, Youness E, Murphy
symptoms. SG et al (1981) Natural history of central nervous system acute
Our patient had very similar pathological features on MRI, but leukemia in adults. Cancer 47:184–96.
she had not been treated with any chemotherapeutic agents at all. In
her case, though, the CNS-spread of the AML and the histopatho-
logic pattern of the severe and extensive leukoencephalopathy
ABSTRACT
could be shown in post mortem analysis. Our patient was seriously A-76-year old woman was admitted to the hospital with paraplegia
affected by a CNS-spread of the AML which may have been after a collapse at home. Magnetic resonance imaging showed
present for years, as suggested from her past medical history, and white matter lesions from Th4 to L2 as well as large confluent white
finally resulted in the patient’s death from a blast crisis. Autopsy matter lesions in the cerebrum. Within 3 days, the patient’s mental
revealed active demyelination with complement deposits that status decreased dramatically and she finally died on day 16 after
extended over the cerebrum and myelon (spinal cord). While pro- her fall. Autopsy examination revealed an acute myeloid leukemia,
nounced axonal destruction and complement-mediated demyelina- which had not previously been diagnosed and which had never
tion can be typical for neuromyelitis optica (NMO), the patient had been treated. In the CNS, we found spread of myeloblasts in com-
no clinical signs of NMO and we failed to detect any aquaporin-4 bination with acute demyelinating lesions which corresponded to
antibodies, arguing against this possibility. the antibody- and complement-mediated pattern II of multiple scle-
In summary, we present a patient with CNS spread of an rosis lesions. This case implies that association of acute myeloid
untreated acute myeloid leukemia, which is a very uncommon leukemia and acute CNS demyelination needs to be discussed and
finding. Moreover, it was associated with acute demyelination and suggests that AML patients need to be strictly monitored for CNS
axonal destruction. We suggest that such demyelination may occur functions.
510 Brain Pathology 20 (2010) 507–510
© 2010 The Authors; Journal Compilation © 2010 International Society of Neuropathology
También podría gustarte
- The Yellow House: A Memoir (2019 National Book Award Winner)De EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Calificación: 4 de 5 estrellas4/5 (98)
- A Tiling of The Plane With TrianglesDocumento6 páginasA Tiling of The Plane With TriangleswillygopeAún no hay calificaciones
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceDe EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceCalificación: 4 de 5 estrellas4/5 (895)
- Trig SubstitutionDocumento13 páginasTrig SubstitutionwillygopeAún no hay calificaciones
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeDe EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeCalificación: 4 de 5 estrellas4/5 (5794)
- A 45-Year Old Male With Left-Sided Hemihypesthesia: Clinical HistoryDocumento4 páginasA 45-Year Old Male With Left-Sided Hemihypesthesia: Clinical HistorywillygopeAún no hay calificaciones
- The Little Book of Hygge: Danish Secrets to Happy LivingDe EverandThe Little Book of Hygge: Danish Secrets to Happy LivingCalificación: 3.5 de 5 estrellas3.5/5 (399)
- Putnam InequalitiesDocumento15 páginasPutnam InequalitieswillygopeAún no hay calificaciones
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaDe EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaCalificación: 4.5 de 5 estrellas4.5/5 (266)
- Chords RegionsDocumento3 páginasChords RegionswillygopeAún no hay calificaciones
- Shoe Dog: A Memoir by the Creator of NikeDe EverandShoe Dog: A Memoir by the Creator of NikeCalificación: 4.5 de 5 estrellas4.5/5 (537)
- Geometry BasicsDocumento2 páginasGeometry BasicswillygopeAún no hay calificaciones
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureDe EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureCalificación: 4.5 de 5 estrellas4.5/5 (474)
- A 10-Year Old Girl With Neck Pain: Clinical HistoryDocumento4 páginasA 10-Year Old Girl With Neck Pain: Clinical HistorywillygopeAún no hay calificaciones
- Never Split the Difference: Negotiating As If Your Life Depended On ItDe EverandNever Split the Difference: Negotiating As If Your Life Depended On ItCalificación: 4.5 de 5 estrellas4.5/5 (838)
- 1208 Case 2Documento4 páginas1208 Case 2willygopeAún no hay calificaciones
- Grit: The Power of Passion and PerseveranceDe EverandGrit: The Power of Passion and PerseveranceCalificación: 4 de 5 estrellas4/5 (588)
- 1108 Case 2Documento4 páginas1108 Case 2willygopeAún no hay calificaciones
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryDe EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryCalificación: 3.5 de 5 estrellas3.5/5 (231)
- 1009 Case 2Documento4 páginas1009 Case 2willygopeAún no hay calificaciones
- 1208 Case 1Documento2 páginas1208 Case 1willygopeAún no hay calificaciones
- The Emperor of All Maladies: A Biography of CancerDe EverandThe Emperor of All Maladies: A Biography of CancerCalificación: 4.5 de 5 estrellas4.5/5 (271)
- 1108 Case 1Documento2 páginas1108 Case 1willygopeAún no hay calificaciones
- 1109 Case 2Documento4 páginas1109 Case 2willygopeAún no hay calificaciones
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyDe EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyCalificación: 3.5 de 5 estrellas3.5/5 (2259)
- 1008 Case 2Documento4 páginas1008 Case 2willygopeAún no hay calificaciones
- On Fire: The (Burning) Case for a Green New DealDe EverandOn Fire: The (Burning) Case for a Green New DealCalificación: 4 de 5 estrellas4/5 (73)
- 0709 Case 2Documento4 páginas0709 Case 2willygopeAún no hay calificaciones
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersDe EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersCalificación: 4.5 de 5 estrellas4.5/5 (344)
- 1009 Case 1Documento4 páginas1009 Case 1willygopeAún no hay calificaciones
- Rise of ISIS: A Threat We Can't IgnoreDe EverandRise of ISIS: A Threat We Can't IgnoreCalificación: 3.5 de 5 estrellas3.5/5 (137)
- 0909 Case 2Documento2 páginas0909 Case 2willygopeAún no hay calificaciones
- Team of Rivals: The Political Genius of Abraham LincolnDe EverandTeam of Rivals: The Political Genius of Abraham LincolnCalificación: 4.5 de 5 estrellas4.5/5 (234)
- 0909 Case 1Documento4 páginas0909 Case 1willygopeAún no hay calificaciones
- 0609 Case 1Documento4 páginas0609 Case 1willygopeAún no hay calificaciones
- 1008 Case 1Documento4 páginas1008 Case 1willygopeAún no hay calificaciones
- The Unwinding: An Inner History of the New AmericaDe EverandThe Unwinding: An Inner History of the New AmericaCalificación: 4 de 5 estrellas4/5 (45)
- 0809 Case 2Documento4 páginas0809 Case 2willygopeAún no hay calificaciones
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreDe EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreCalificación: 4 de 5 estrellas4/5 (1090)
- 0610case1 Metastatic MelanomaDocumento4 páginas0610case1 Metastatic MelanomawillygopeAún no hay calificaciones
- A 7-Year-Old Boy Dying of Acute Encephalopathy: Case History Autopsy FindingsDocumento4 páginasA 7-Year-Old Boy Dying of Acute Encephalopathy: Case History Autopsy FindingswillygopeAún no hay calificaciones
- 0609 Case 2Documento2 páginas0609 Case 2willygopeAún no hay calificaciones
- 0410case1 GBM With PNETDocumento4 páginas0410case1 GBM With PNETwillygopeAún no hay calificaciones
- 0409 Case 2Documento4 páginas0409 Case 2willygopeAún no hay calificaciones
- 0509 Case 1Documento4 páginas0509 Case 1willygopeAún no hay calificaciones
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)De EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Calificación: 4.5 de 5 estrellas4.5/5 (121)
- 0510 Case 1Documento2 páginas0510 Case 1willygopeAún no hay calificaciones
- A 24-Year-Old Male With Headaches: Clinical HistoryDocumento4 páginasA 24-Year-Old Male With Headaches: Clinical HistorywillygopeAún no hay calificaciones
- Genes For All DisordersDocumento86 páginasGenes For All Disordersvenkyreddy97Aún no hay calificaciones
- PS31 - CML Booklet - 2019Documento64 páginasPS31 - CML Booklet - 2019ameliaAún no hay calificaciones
- The Philadelphia Chromosome InfographicDocumento1 páginaThe Philadelphia Chromosome InfographicThe Experiment100% (1)
- Alkeran®: (Melphalan) TabletsDocumento8 páginasAlkeran®: (Melphalan) Tabletskaren rodriguezAún no hay calificaciones
- Serum Plasma Minus Fibrinogen Albumin Provides Osmotic PressureDocumento13 páginasSerum Plasma Minus Fibrinogen Albumin Provides Osmotic PressureFreeNursingNotesAún no hay calificaciones
- The Perks of Being a WallflowerDe EverandThe Perks of Being a WallflowerCalificación: 4.5 de 5 estrellas4.5/5 (2102)
- Association of Leukemia Cutis With Survival in Acute Myeloid LeukemiaDocumento7 páginasAssociation of Leukemia Cutis With Survival in Acute Myeloid LeukemiafikriafisAún no hay calificaciones
- Pediatrics Final2021Documento165 páginasPediatrics Final2021TayaAún no hay calificaciones
- Unit 4 Study Guide PathoDocumento10 páginasUnit 4 Study Guide Pathoangieswenson100% (1)
- G. Mauger - Cours de Langue Et de Civilisation FrançaisesDocumento619 páginasG. Mauger - Cours de Langue Et de Civilisation FrançaisesAdrian Mucileanu0% (1)
- Her Body and Other Parties: StoriesDe EverandHer Body and Other Parties: StoriesCalificación: 4 de 5 estrellas4/5 (821)
- STEM CELL TherapyDocumento23 páginasSTEM CELL Therapycamila hartmann100% (1)
- MUST To KNOW in Immunohematology Blood BankingDocumento42 páginasMUST To KNOW in Immunohematology Blood BankingMerhella Amor Suerte MendozaAún no hay calificaciones
- Laporan IKM KSM PK FEBRUARI 2022Documento28 páginasLaporan IKM KSM PK FEBRUARI 2022Nur iffahAún no hay calificaciones
- Hematology 2015-2016 CM 299Documento36 páginasHematology 2015-2016 CM 299Nadejda DoroseviciAún no hay calificaciones
- Hematologic DisordersDocumento40 páginasHematologic DisordersMary Grace LeronAún no hay calificaciones
- MEDICAL TERMINOLOGY PRAKTIKUM.2020docxDocumento17 páginasMEDICAL TERMINOLOGY PRAKTIKUM.2020docxEvangeline EngieAún no hay calificaciones
- 2004 - Practice Test EcpeDocumento24 páginas2004 - Practice Test EcpeZoi Plessa100% (4)
- Data Sheet Daunorubicin Injection: Name of The MedicineDocumento15 páginasData Sheet Daunorubicin Injection: Name of The MedicineAbulHasan Idrus IstarAún no hay calificaciones
- LeukemiaDocumento8 páginasLeukemiapriscillaAún no hay calificaciones
- Large Granular Lymphocytic Leukemia. Current Diagnostic and Therapeutic Approaches and Novel Treatment OptionsDocumento29 páginasLarge Granular Lymphocytic Leukemia. Current Diagnostic and Therapeutic Approaches and Novel Treatment OptionsOrxan HumbetovAún no hay calificaciones
- Tumors of The Body + All Normal ValuesDocumento16 páginasTumors of The Body + All Normal ValuesSifat DewanAún no hay calificaciones
- Student Worksheet - General ImmunologyDocumento7 páginasStudent Worksheet - General ImmunologyzaraongkoAún no hay calificaciones
- 2012.01.12!02!07-48CV Mammen Chandy WebsiteDocumento16 páginas2012.01.12!02!07-48CV Mammen Chandy WebsitePradeep BabuAún no hay calificaciones
- G7 HEALTH Prevention and Control of Diseases and Disorders (Non-Communicable)Documento30 páginasG7 HEALTH Prevention and Control of Diseases and Disorders (Non-Communicable)JOHN FRITS GERARD MOMBAYAún no hay calificaciones
- Bruising OSCE History Taking PaediatricsDocumento6 páginasBruising OSCE History Taking PaediatricsJJ LimAún no hay calificaciones
- Leukemia StudyDocumento18 páginasLeukemia StudyaneeshdAún no hay calificaciones
- Everyday Science Book For CSSDocumento50 páginasEveryday Science Book For CSSshahzad jalbani100% (1)
- Covid LeukemiaDocumento9 páginasCovid LeukemiamahadianismailnstAún no hay calificaciones
- Flow Cytometry: By: Dr. Megha Gupta & Dr. Tashi AgarwalDocumento116 páginasFlow Cytometry: By: Dr. Megha Gupta & Dr. Tashi Agarwalanggaririn100% (1)
- Punjab An Environmental Health Hotspot Heading Towards DeathDocumento12 páginasPunjab An Environmental Health Hotspot Heading Towards DeathDr. Amar Singh AzadAún no hay calificaciones
- Summary: The Psychology of Money: Timeless Lessons on Wealth, Greed, and Happiness by Morgan Housel: Key Takeaways, Summary & Analysis IncludedDe EverandSummary: The Psychology of Money: Timeless Lessons on Wealth, Greed, and Happiness by Morgan Housel: Key Takeaways, Summary & Analysis IncludedCalificación: 5 de 5 estrellas5/5 (80)
- The Obesity Code: Unlocking the Secrets of Weight LossDe EverandThe Obesity Code: Unlocking the Secrets of Weight LossCalificación: 4 de 5 estrellas4/5 (6)
- ADHD is Awesome: A Guide to (Mostly) Thriving with ADHDDe EverandADHD is Awesome: A Guide to (Mostly) Thriving with ADHDCalificación: 5 de 5 estrellas5/5 (1)
- Think This, Not That: 12 Mindshifts to Breakthrough Limiting Beliefs and Become Who You Were Born to BeDe EverandThink This, Not That: 12 Mindshifts to Breakthrough Limiting Beliefs and Become Who You Were Born to BeCalificación: 2 de 5 estrellas2/5 (1)
- The Age of Magical Overthinking: Notes on Modern IrrationalityDe EverandThe Age of Magical Overthinking: Notes on Modern IrrationalityCalificación: 4 de 5 estrellas4/5 (24)
- LIT: Life Ignition Tools: Use Nature's Playbook to Energize Your Brain, Spark Ideas, and Ignite ActionDe EverandLIT: Life Ignition Tools: Use Nature's Playbook to Energize Your Brain, Spark Ideas, and Ignite ActionCalificación: 4 de 5 estrellas4/5 (404)