Documentos de Académico
Documentos de Profesional
Documentos de Cultura
Vestibuloplasty
Cargado por
Zullia TaftyantiTítulo original
Derechos de autor
Formatos disponibles
Compartir este documento
Compartir o incrustar documentos
¿Le pareció útil este documento?
¿Este contenido es inapropiado?
Denunciar este documentoCopyright:
Formatos disponibles
Vestibuloplasty
Cargado por
Zullia TaftyantiCopyright:
Formatos disponibles
[Downloaded free from http://www.amsjournal.com on Thursday, August 17, 2017, IP: 140.0.245.
82]
Original Clinical Studies
Comparison of vestibular sulcus depth in vestibuloplasty
using standard Clark’s technique with and without
amnion as graft material
Access this article online
Website:
Basavaraj C. Sikkerimath, Satyajit Dandagi, Santosh. S. Gudi, Deeptha Jayapalan
www.amsjournal.com Department of Oral and Maxillofacial Surgery, P.M.N.M. Dental College and Hospital,
DOI: Bagalkot, Karnataka, India
10.4103/2231-0746.95313
Quick Response Code:
Address for correspondence:
Dr. Deeptha J., Department of Oral and Maxillofacial Surgery,
P.M.N.M. Dental College and Hospital, Bagalkot, Karnataka, India.
E-mail: deepthamagnet@gmail.com
ABSTRACT
Introduction: A number of materials are used as grafts in vestibuloplasty like mucosal and skin grafts with several advantages
and disadvantages. To circumvent the disadvantages of these grafts, biological membranes such as amnion membranes are
often recommended. Materials and Methods: The objective of this study was to clinically assess the vestibular sulcus depth
in vestibuloplasty using Clark’s technique with and without amnion as graft material. Twenty edentulous patients underwent
mandibular labial vestibuloplasty using Clark’s technique. Amnion was used as graft material in 10 patients (group I) and no
grafts used in remaining 10 patients (group II). The vestibular depth was evaluated at time intervals of 1 week, 2 weeks, 1
month and 3 months, postoperatively. Results: Mean postoperative vestibular depth after 3 months in group I and II were 10.0
± 3.13 mm and 7.8±0.63 mm, respectively. Mean of 2.2 ± 2.50 mm increase in depth was achieved after 3 months in Group I.
Conclusion: Amnion graft is a viable and reliable option that promotes early healing and maintains postoperative vestibular
depth.
Keywords: Amnion graft, clark’s technique, vestibular depth, vestibuloplasty
INTRODUCTION the exposed periosteum because a nearly complete relapse
could be proven during secondary healing with contraction
The oral rehabilitation of patients after loss of teeth has made much and epithelialization of the vestibular periosteum.[3] To date
progress in recent times. Vestibuloplasty, ridge augmentation various autogenous soft tissue grafts from autogenous mucosal
and different types of implants were used to overcome the to allogeneic collagen membrane[4] have been used for vestibular
problems of flat alveolar ridge.[1] Many different methods have
extension. All grafts have the disadvantages of increased
been described for regenerating or replacing bone for secondary
morbidity, postoperative pain and risk of surgical complications
implant placement but until now no substantial progress has been
in the donor site.[5] This led to search for an alternate graft material.
made in soft tissue management.[2] The most common procedure
in vestibuloplasty are submucosal vestibuloplasty, secondary
epithelial vestibuloplasty, soft tissue graft vestibuloplasty and Biological membrane obtained from placenta opens new
Edlanplasty. [3] The aim of all these techniques is to create perspectives. The human amnion membrane is a biological
adequate vestibular depth and limit the traction of fiber and graft which has unique properties like antiadhesive effects,
muscle attachments.[2] bacteriostatic properties, wound protection, pain reduction and
epithelisation effects. Its easy availability, low cost makes it the
In secondary epithelial vestibuloplasty, there is a need to cover best material.
30 Annals of Maxillofacial Surgery | January - June 2012 | Volume 2 | Issue 1
[Downloaded free from http://www.amsjournal.com on Thursday, August 17, 2017, IP: 140.0.245.82]
Sikkerimath, et al.: Vestibuloplasty-amnion graft
The use of amnion in vestibuloplasty has been first reported MATERIALS AND METHOD
by Guler et al.,[6] who concentrated on the blood flow to the
graft. Lawson studied the use of amniotic membrane along with Twenty patients who presented with insufficient vestibular depth
but adequate mandibular bone heights were referred for the
pectoralis major muscle for oral reconstruction.[7]
correction of vestibular depth. Bone height and mucosal quality
and quantity were assessed using radiographic and clinical
methods. The procedure to be performed was explained, followed
by informed written consent. Ethical committee clearance was
obtained and endorsed duly by the head of the institution.
Preoperative impression, cast and measurements were made
[Figures 1 and 2]. The cast was arbitrarily scraped till the desired
depth as per the clinical requirements. A splint was fabricated
with clear acrylic, finished and polished [Figure 3]. Fresh amniotic
membrane was obtained from healthy seronegative mothers who
underwent Cesarean section. The amnion was separated from the
chorion [Figure 4] and was cleansed of blood by flushing with
copious amounts of tap water.
The membranes were placed in a large glass bottle containing
85% glycerol, made by taking 85 ml of glycerol and making up
to 100 ml with normal saline and stored at room temperature for
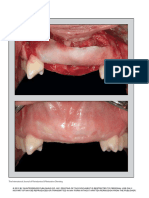
Figure 1: Preoperative cast 24 hours. They were then transferred to another bottle of 85%
glycerol and stored at 40C for the time period till used.
Figure 2: Preoperative depth
Figure 3: Acrylic splint
Figure 4: Separation of amnion from chorion Figure 5: Harvested amnion graft
Annals of Maxillofacial Surgery | January - June 2012 | Volume 2 | Issue 1 31
[Downloaded free from http://www.amsjournal.com on Thursday, August 17, 2017, IP: 140.0.245.82]
Sikkerimath, et al.: Vestibuloplasty-amnion graft
Immediately prior to their use, small clean sections (6 x 10 cm2) flap [Figure 6] and suturing to desired depth [Figure 7] and the
of membrane were cut and kept in 400 ml of saline containing amniotic graft material so prepared is transferred over the surgical
10,00,000 IU penicillin at 480C up to 24 hours. The obtained graft site with mesenchymal side against the wound and sutured in
material was then properly cleaned in saline solution [Figure 5]. place with 5-0 absorbable sutures [Figure 8]. The surgical splint
was placed after lining with soft liner[7] to prevent formation of
Clark’s technique of vestibuloplasty was done after reflection of dead space, and secured either with circum-mandibular suturing
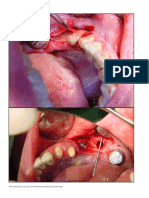
Figure 6: Reflection of flap Figure 7: Flap sutured to desired depth
Figure 8: Suturing of amnion graft to denuded periosteum Figure 9: Splints secured by bone screw
Figure 10: Postoperative cast Figure 11: Postoperative vestibular depth
32 Annals of Maxillofacial Surgery | January - June 2012 | Volume 2 | Issue 1
[Downloaded free from http://www.amsjournal.com on Thursday, August 17, 2017, IP: 140.0.245.82]
Sikkerimath, et al.: Vestibuloplasty-amnion graft
or with bone screws of 1.5 x 6 mm [Figure 9]. Postoperative was of bearable state which can effectively be controlled by using
impression, cast and measurements were made [Figures 10 and 11]. analgesics. No complications such as immunological rejection
and infection occurred in study population, and the prosthetic
Out of 20 patients, randomly 10 patients (Group I) had the raw treatment could be started as early as a month after the surgery.
surface covered with amnion graft followed by splint placement Although in one of our patient there was relapse of the vestibular
and remaining 10 patients(Group II) underwent secondary depth to almost near to its preoperative value, mainly due to
epithelisation without any graft under local anaesthesia. Splints inability to maintain the oral hygiene. In Group II, one patient
were secured to bone through the tranmucosal bone screws. The had postoperative edema and swelling which subsided on further
splint was removed after 7th day postoperatively and grafted site course of antibiotics. Pain of higher scale chiefly on 1st and 2nd day
was thoroughly cleaned. Patients were followed up and their were present in group II. The graft area could not be differentiated
vestibular depths were measured at intervals of 1 week, 2 weeks, from nongrafted tissue after 3 months. Group I showed better
1month and 3 months, postoperatively [Tables 1 and 2]. results when compared to group II [Graph 1].
Descriptive statistics were presented. Paired t test was performed DISCUSSION
to find the difference between the percentages of reduction
in depth of the buccal vestibule. P value ≤0.05 was taken as Lack of an adequate residual alveolar ridge and basal seat severely
significant. compromises the success of prosthodontic treatment. It has been
suggested that expansion of the denture-bearing area by means
RESULTS of a vestibuloplasty would reduce denture load per square
unit of supporting bone and thus reduce the bone resorption
The reduction in the depth of the buccal vestibule in Group I caused by transfer of occlusal forces.[8] Numerous graft materials
was found to be 24.81% after 3 months follow-up and 42.22% are available but all suffer from certain limitations. In order to
reduction in the depth of the buccal vestibule was seen in group overcome the same there is a search for more appropriate graft
II [Table 3]. The difference in between the groups at various post- material. Skin graft,[8] mucosal grafts,[8] palatal graft,[9] buccal
operative measurements was statistically significant. graft,[10] cultured mucosal grafts, allogenic collagen membrane,[4]
dural graft,[5] placental graft[6,7] were suggested.
Postoperatively there were no mental nerve paresthesias in both
the groups. Vestibular depth was assessed in all patients. Group Split skin graft is well-tolerated, but can be subjected to
I patients had no postoperative edema, swelling and even pain postoperative shrinkage, [2] and when compared with the
Table 1: Vestibular depth in vestibuloplasty cases with amnion graft
Case No. Preoperative Intraoperative Postoperative Postoperative Postoperative Postoperative
Vestibular depth Vestibular depth Vestibular depth Vestibular depth Vestibular depth Vestibular depth
(in mm) (in mm) (1 week) (2 week) (1 month) (3 months)
1 4 15 14 14 14 14
2 3 15 14 14 14 14
3 4 13 12 10 8 8
4 3 15 14 12 12 12
5 3 12 9 9 9 9
6 3 10 9 8 7 5
7 4 14 13 12 11 11
8 4 15 14 13 13 12
9 2 12 10 10 9 9
10 3 12 10 9 8 6
Mean 3.3 13.3 11.9 11.1 10.5 10.0
Table 2: Vestibular depth in vestibuloplasty cases without amnion graft
Case No. Preoperative Intraoperative Postoperative Postoperative Postoperative Postoperative
Vestibular depth Vestibular depth Vestibular depth Vestibular depth Vestibular depth Vestibular depth
(in mm) (in mm) (1 week) (2 week) (1 month) (3 months)
1 3 14 10 10 8 7
2 4 15 11 10 9 8
3 4 13 10 9 9 8
4 2 12 9 8 8 7
5 3 13 10 10 9 8
6 4 13 10 10 9 8
7 3 14 11 10 9 9
8 3 15 11 10 9 8
9 3 14 11 9 8 8
10 4 12 10 9 8 7
Mean 3.3 13.5 10.3 9.5 8.6 7.8
Annals of Maxillofacial Surgery | January - June 2012 | Volume 2 | Issue 1 33
[Downloaded free from http://www.amsjournal.com on Thursday, August 17, 2017, IP: 140.0.245.82]
Sikkerimath, et al.: Vestibuloplasty-amnion graft
Table 3: Reduction rate in group 1 and group 2 from
intraoperative to 3 months by t-test
Time % of % of P-value
Reduction Reduction
in group 1 in group 2
Intraoperative to 1 week 10.53 23.7 0.0000*
Intraoperative to 2 weeks 16.54 29.63 0.0001*
Intraoperative to 1 month 21.05 36.3 0.0005*
Intraoperative to 3 months 24.81 42.22 0.0008*
*P<0.05
surrounding mucosa, the grafted area displays a marked clinical
difference in consistency and color. Common complications of
the donor site include susceptibility to Candida infection, pain,
discomfort, delayed healing, hypertrophic or discolored scars and
dysethesia. The problem with mucosal (buccal and palatal grafts) Graph 1: Comparison of group 1 and group 2 with respect to vestibular
is the limited amount of mucosa available for grafting. Possibility depth (in mm) at different time intervals
of nerve damages and an increased rate of ulceration altogether
prevent its use for prosthetic purposes.[4] Palatal mucosal wounds
the upper denture, as the alveolar ridge resorption is four times
leave an open wound with a healing course of 4-6 and half weeks
greater in the mandible than in the maxilla. So we included
and possible complications of soreness, ulcers, and difficulty in
mandibular anterior region as the site for our study.
wearing an upper denture.[10]
The main potential issue that one could expect to raise with use
To circumvent these disadvantages biological membranes have
of processed amnion is of cross infections, especially with prion
been suggested as options including fetal membranes. The
diseases. Adequate care need to be exercised while collecting the
amniotic membrane is formed from the ectoderm of the fetus.
same from voluntary donors. Proper screening and sterilization
It has a stromal matrix, a thick collagen layer, and an overlying
modalities need to be instituted. The next issue would be of
basement membrane with a single layer of epithelium. It
voluntary, informed consent of the patients owing to the ethical
closely resembles the epidermis of the skin and has been used
issues involved in such treatment.
as a physiological wound dressing with great success.[6] The
amnion has the following advantages: it promotes secondary
epithelialization, vascularize healthy granulation tissue and The result of the present study indicates that reduction in
stimulate the neovascularisation in neighbouring tissues and it postoperative vestibular depth is less when human amniotic
is antibacterial. Another characteristic of amniotic membrane membrane is used as a graft material to cover the denuded
is the lack of immunogenicity as it did not express antigens of periosteum when compared to standard Clark’s technique
histocompatibility, the allograft was never rejected.[7] without amnion graft. The results of this study indicates that
the amnion is an appropriate graft material for vestibuloplasty.
The concept of using biodegradable amniotic membrane could
They are inexpensive, readily available, used fresh or lyophilised,
lead to better results, shorter treatment time and less donor site
and stored at room temperature after sterilisation by -irradiation.
morbidity. Also, the study proves the versatility of angiogenic
biodegradable amniotic membrane as a favourable graft material
Human amnion has been known to be an effective dressing since
for vestibuloplasty which promotes healing and prevent relapse.
John Staige Davis used it way back in 1910.[7] Since then extensive
studies on amnion have been performed all over the world and
it has been proved to be an excellent biological dressing with REFERENCES
almost all the qualities of an ideal dressing. Chao et al., were the
1. Mehanna MB. Evaluation of the fenestrated mucosal flap vestibuloplasty
first who used it for the coverage of huge dural defects. Lawson and a modification of the Kazanjian’s vestibuloplasty technique for
placed amnion over the deep aspect of the pectoralis major mandibular anterior ridge extension. J Egypt Dent Assoc 2000;46:19-21.
muscle for oral cavity reconstruction.[7] A single layer of fresh 2. Raguse JD, Gath HJ. A metabolically active dermal replacement
amnion for surgical treatment of oral submucous fibrosis. Guler (Dermagraft) for vestibuloplasty. J Oral Rehabil 2005;32:337-40.
et al., used the grafts of amnion in mandibular vestibuloplasty.[6] 3. Froschl T, Kerscher A. The optimal vestibuloplasty in preprosthetic
surgery of the mandible. J Craniomaxillofac Surg 1997;25:85-90.
4. Raghoebar GM, Tomson AM, Scholma J, Blaauw EH, Witjes MJ,
To evaluate the efficacy of human amniotic membrane as a graft Vissink A. Use of cultured mucosal grafts to cover defects caused by
material in vestibuloplasty, we conducted the present clinical vestibuloplasty: An in vivo study. J Oral Maxillofac Surg 1995;53:872-8;
study comparing vestibular depths between group I where the discussion 878-9.
denuded surface of periosteum in mandibular labial surface 5. Martis C, Lazaridis N, Karabouta I, Trigonidis G. Free transplantation
was covered with glycerol-preserved amnion graft using Clark’s of lyophilized dura for vestibuloplasty: A clinical and histological study.
technique and group II where standard Clark’s technique was J Oral Surg 1979;37:646-9.
6. Güler R, Ercan MT, Ulutunçel N, Devrim H, Uran N. Measurement of
performed without graft. blood flow by the 133Xe clearance technique to grafts of amnion used
in vestibuloplasty. Br J Oral Maxillofac Surg 1997;35:280-3.
In most patients problem with lower denture are more than with 7. Samandari MH, Yaghmaei M, Ejlali M, Moshref M, Saffar AS. Use of
34 Annals of Maxillofacial Surgery | January - June 2012 | Volume 2 | Issue 1
[Downloaded free from http://www.amsjournal.com on Thursday, August 17, 2017, IP: 140.0.245.82]
Sikkerimath, et al.: Vestibuloplasty-amnion graft
amnion as a graft material in vestibuloplasty: A preliminary report. Oral mucosal graft. A 2-year follow up study. Int J Oral Surg 1982;11:81-8.
Surg Oral Med Oral Pathol Oral Radiol Endod 2004;97:574-8
8. Hillerup S, Eriksen E, Solow B. Reduction of mandibular residual ridge
after vestibuloplasty. A two-year follow-up study comparing the Edlan Cite this article as: Sikkerimath BC, Dandagi S, Gudi SS, Jayapalan D.
flap, mucosal and skin graft operations. Int J Oral Maxillofac Surg Comparison of vestibular sulcus depth in vestibuloplasty using standard
1989;18:271-6. Clark's technique with and without amnion as graft material. Ann Maxillofac
9. Amphlett J, Colwell WC. Edentulous vestibuloplasty using the palatal Surg 2012;2:30-5.
graft technique. J Prosthet Dent 1982;48:8-14. Source of Support: Nil, Conflict of Interest: None declared.
10. Hillerup S. Pre-prosthetic mandibular vestibuloplasty with Buccal
Author Help: Online Submission of the Manuscripts
Articles can be submitted online from http://www.journalonweb.com. For online submission articles should be prepared in two files (first page
file and article file). Images should be submitted separately.
1) First Page File:
Prepare the title page, covering letter, acknowledgement, etc., using a word processor program. All information which can reveal your
identity should be here. Use text/rtf/doc/pdf files. Do not zip the files.
2) Article file:
The main text of the article, beginning from Abstract till References (including tables) should be in this file. Do not include any information
(such as acknowledgement, your names in page headers, etc.) in this file. Use text/rtf/doc/pdf files. Do not zip the files. Limit the file size to
1 MB. Do not incorporate images in the file. If file size is large, graphs can be submitted as images separately without incorporating them
in the article file to reduce the size of the file.
3) Images:
Submit good quality color images. Each image should be less than 4096 kb (4 MB) in size. Size of the image can be reduced by decreasing
the actual height and width of the images (keep up to about 6 inches and up to about 1200 pixels) or by reducing the quality of image. JPEG
is the most suitable file format. The image quality should be good enough to judge the scientific value of the image. Always retain a good
quality, high resolution image for print purpose. This high resolution image should be sent to the editorial office at the time of sending a
revised article.
4) Legends:
Legends for the figures/images should be included at the end of the article file.
Annals of Maxillofacial Surgery | January - June 2012 | Volume 2 | Issue 1 35
También podría gustarte
- Effectiveness of Human Amnion As A Graft MaterialDocumento6 páginasEffectiveness of Human Amnion As A Graft MaterialJuan Sierra ZambranoAún no hay calificaciones
- Clinical and Histological Evaluation of Two Dressi PDFDocumento4 páginasClinical and Histological Evaluation of Two Dressi PDFJoha AriasAún no hay calificaciones
- Anterior Ridge Extension Using Modified Kazanjian Technique in Mandible-A Clinical StudyDocumento5 páginasAnterior Ridge Extension Using Modified Kazanjian Technique in Mandible-A Clinical StudyHélder MouraAún no hay calificaciones
- Kazanjian ModificadoDocumento4 páginasKazanjian ModificadoMaximiliano Jara ContrerasAún no hay calificaciones
- Guided Tissue RegenerationDocumento7 páginasGuided Tissue RegenerationElenaLazarAún no hay calificaciones
- Tabanella Bucall Pedicle Con Collagen Matrix2021Documento8 páginasTabanella Bucall Pedicle Con Collagen Matrix2021SergioAún no hay calificaciones
- Evolution of Mandibular Defects Reconstruction Procedures: From Older Principles To Newer Techniques and TechnologyDocumento11 páginasEvolution of Mandibular Defects Reconstruction Procedures: From Older Principles To Newer Techniques and Technologykarthik kumarAún no hay calificaciones
- Piezosurgery Versus Conventional Method AlveoloplaDocumento7 páginasPiezosurgery Versus Conventional Method Alveoloplamirah indrianiAún no hay calificaciones
- Ibm 5Documento7 páginasIbm 5rintanfsAún no hay calificaciones
- Subperiostial Minimally Invasive Aesthetic Ridge Augmentation Technique (SMART)Documento10 páginasSubperiostial Minimally Invasive Aesthetic Ridge Augmentation Technique (SMART)Pat TellezAún no hay calificaciones
- 371-Article Text-1509-3-10-20210710Documento6 páginas371-Article Text-1509-3-10-20210710Fransiski HoAún no hay calificaciones
- Guided Tissue Regeneration: A Review: Journal of Dental Health Oral Disorders & TherapyDocumento7 páginasGuided Tissue Regeneration: A Review: Journal of Dental Health Oral Disorders & TherapyLouis HutahaeanAún no hay calificaciones
- Ab 2019Documento7 páginasAb 2019Dome CárdenasAún no hay calificaciones
- Articulo en Inglés 2Documento8 páginasArticulo en Inglés 2Luis Ramirez BenaventeAún no hay calificaciones
- 3 (1) 11 14Documento4 páginas3 (1) 11 14marcelodentAún no hay calificaciones
- Three-Dimensional Vertical Alveolar Ridge Augmentation in The Posterior Maxilla: A 10-Year Clinical StudyDocumento10 páginasThree-Dimensional Vertical Alveolar Ridge Augmentation in The Posterior Maxilla: A 10-Year Clinical StudyFabian Sanabria100% (1)
- Guided Bone RegenerationDocumento4 páginasGuided Bone Regenerationahmad955mlsAún no hay calificaciones
- Aesthetic Crown LengtheningDocumento4 páginasAesthetic Crown LengtheningGopuAún no hay calificaciones
- The New "Cubism" Graft Technique in Tympanoplasty - A Randomized Controlled TrialDocumento9 páginasThe New "Cubism" Graft Technique in Tympanoplasty - A Randomized Controlled Trialian danarkoAún no hay calificaciones
- Techniques On Vertical Ridge Augmentation IndicatiDocumento30 páginasTechniques On Vertical Ridge Augmentation IndicatiFelix SchweppeAún no hay calificaciones
- Effect of Retraction Materials On Gingival HealthDocumento5 páginasEffect of Retraction Materials On Gingival HealthAastha DuaAún no hay calificaciones
- The Injection Resin Technique A Novel ConceptDocumento15 páginasThe Injection Resin Technique A Novel ConceptJuan Francisco CamposAún no hay calificaciones
- Artículo 1 - OstectomíaDocumento10 páginasArtículo 1 - OstectomíaEmilio RodríguezAún no hay calificaciones
- Restoration in Gingival Recession PDFDocumento4 páginasRestoration in Gingival Recession PDFannysaAún no hay calificaciones
- CR2 CocktailManagement KhusbooMishraDocumento6 páginasCR2 CocktailManagement KhusbooMishradella sainAún no hay calificaciones
- CCD 4 509Documento3 páginasCCD 4 509gbaez.88Aún no hay calificaciones
- Simion 2012)Documento13 páginasSimion 2012)SergioAún no hay calificaciones
- Windisch 등 - 2021 - Vertical-guided bone regeneration with a titaniumDocumento12 páginasWindisch 등 - 2021 - Vertical-guided bone regeneration with a titaniumsupercool0120Aún no hay calificaciones
- Esthetic and Functional Reconstruction of Large Mandibular Defects Using Free Fibula Flap and Implant-Retained Prosthetics - A Case Series With Long-Term Follow-UpDocumento7 páginasEsthetic and Functional Reconstruction of Large Mandibular Defects Using Free Fibula Flap and Implant-Retained Prosthetics - A Case Series With Long-Term Follow-UppankajAún no hay calificaciones
- JofIMAB - 2015 21 4p964 968 PDFDocumento5 páginasJofIMAB - 2015 21 4p964 968 PDFKarta SudibyoAún no hay calificaciones
- Crid2014 658790Documento6 páginasCrid2014 658790paula catanaAún no hay calificaciones
- Preprosthetic Surgery: An Adjunct To Complete Denture TherapyDocumento3 páginasPreprosthetic Surgery: An Adjunct To Complete Denture TherapyrintanfsAún no hay calificaciones
- Epiphora Drainage by DCR - Long-Term Results: Original ResearchDocumento5 páginasEpiphora Drainage by DCR - Long-Term Results: Original ResearchSaatvik AtriAún no hay calificaciones
- Periodontology 2000 - 2023 - Stefanini - Complications and Treatment Errors in Peri Implant Soft Tissue ManagementDocumento15 páginasPeriodontology 2000 - 2023 - Stefanini - Complications and Treatment Errors in Peri Implant Soft Tissue Managementmạnh nguyễn xuânAún no hay calificaciones
- Jurnal Periapikal 2Documento6 páginasJurnal Periapikal 2Rahmania AlikhlasAún no hay calificaciones
- Periodontology 2000 - 2023 - Roccuzzo - The Importance of Soft Tissue Condition in Bone Regenerative Procedures To EnsureDocumento10 páginasPeriodontology 2000 - 2023 - Roccuzzo - The Importance of Soft Tissue Condition in Bone Regenerative Procedures To Ensuremạnh nguyễn xuânAún no hay calificaciones
- Apiko 3Documento4 páginasApiko 3Asri DamayantiAún no hay calificaciones
- Case SeriesDocumento3 páginasCase SeriesDr. DeeptiAún no hay calificaciones
- CTG Histologic EvaluationDocumento7 páginasCTG Histologic EvaluationDr. DeeptiAún no hay calificaciones
- Periosteal Pocket Flap For Horizontal Bone RegenerDocumento10 páginasPeriosteal Pocket Flap For Horizontal Bone RegenerViorel Ion100% (1)
- Aaid Joi D 12 00028Documento9 páginasAaid Joi D 12 00028NancyLiaoAún no hay calificaciones
- SM Jurnal 2Documento3 páginasSM Jurnal 2Kurnia SelaAún no hay calificaciones
- 2011 Article 99Documento4 páginas2011 Article 99ali baridiAún no hay calificaciones
- Clin Adv Periodontics - 2022 - Velasquez Plata - Osseous Topography in Biologically Driven Flap Design in MinimallyDocumento5 páginasClin Adv Periodontics - 2022 - Velasquez Plata - Osseous Topography in Biologically Driven Flap Design in Minimally安西 泰規Aún no hay calificaciones
- 3rd Publication IJOI PDFDocumento14 páginas3rd Publication IJOI PDFSafu SalehAún no hay calificaciones
- Jpis 42 105Documento5 páginasJpis 42 105Jean Pierre Alcántara VigoAún no hay calificaciones
- (11) Nghiên cứu mẫu đo niêm mạc khẩu cái bằng CBCT Gupta2015Documento5 páginas(11) Nghiên cứu mẫu đo niêm mạc khẩu cái bằng CBCT Gupta2015Kiet Tran TuanAún no hay calificaciones
- Complications of Using Retraction CordDocumento4 páginasComplications of Using Retraction CordAya Ibrahim YassinAún no hay calificaciones
- Cricchio 2009Documento7 páginasCricchio 2009elver galargaAún no hay calificaciones
- Jurnal 6Documento7 páginasJurnal 6Dha Dina SevofrationAún no hay calificaciones
- The Use of Biocompatible Membranes in Oral SurgeryDocumento14 páginasThe Use of Biocompatible Membranes in Oral SurgeryHarvey BarriosAún no hay calificaciones
- البحث الثالثDocumento12 páginasالبحث الثالثMostafa Shaker El AasserAún no hay calificaciones
- Unusual Encroachers in OKCDocumento3 páginasUnusual Encroachers in OKCDIVYABOSEAún no hay calificaciones
- Implante Articulo 2Documento5 páginasImplante Articulo 2alessandrachumbimuneAún no hay calificaciones
- Prosthodontic Rehabilitation of An Edentulous Patient Affected With Oral Submucous FibrosisDocumento3 páginasProsthodontic Rehabilitation of An Edentulous Patient Affected With Oral Submucous FibrosisMaqbul AlamAún no hay calificaciones
- A New Porcine-Derived Collagen Matrix To Thicken Peri-Implant Soft Tissues in High Aestethic Value AreasDocumento1 páginaA New Porcine-Derived Collagen Matrix To Thicken Peri-Implant Soft Tissues in High Aestethic Value AreasEdoardo BiancoAún no hay calificaciones
- Case SeriesDocumento5 páginasCase SeriesPavithra balasubramaniAún no hay calificaciones
- Prosthodontic Rehabilitation of Patient With FlabbDocumento4 páginasProsthodontic Rehabilitation of Patient With FlabbLaras Dwi AyuningrumAún no hay calificaciones
- Emergency Endodontics 6Documento3 páginasEmergency Endodontics 6098 - SILVYARA AYU PRATIWIAún no hay calificaciones
- Frenectomy As Previous Treatment of Maxillary Central DiastemDocumento1 páginaFrenectomy As Previous Treatment of Maxillary Central DiastemZullia TaftyantiAún no hay calificaciones
- 01156Documento13 páginas01156riskysetAún no hay calificaciones
- Forensic Odontology: The Investigative Branch of Dentistry - A ReviewDocumento6 páginasForensic Odontology: The Investigative Branch of Dentistry - A ReviewZullia TaftyantiAún no hay calificaciones
- Serialextraction 2Documento6 páginasSerialextraction 2Zullia TaftyantiAún no hay calificaciones
- Serial Extractions - A Review PDFDocumento8 páginasSerial Extractions - A Review PDFJose CollazosAún no hay calificaciones
- Care Plan ChartDocumento5 páginasCare Plan Chartapi-385503945Aún no hay calificaciones
- LINAC HistoryDocumento19 páginasLINAC Historycrusader8880% (1)
- How Do You Handle StressDocumento15 páginasHow Do You Handle StressLing HockAún no hay calificaciones
- Psychological Projection Effect On Family ViolenceDocumento3 páginasPsychological Projection Effect On Family ViolenceMody NasserAún no hay calificaciones
- Lange Q&A: Radiography ExaminationDocumento18 páginasLange Q&A: Radiography ExaminationSamuel JeebanAún no hay calificaciones
- Cervical Cancer (ECC)Documento14 páginasCervical Cancer (ECC)Legi VamelaAún no hay calificaciones
- Diadynamic CurrentDocumento30 páginasDiadynamic CurrentvladAún no hay calificaciones
- Clinical Observation On Greeva StambhaDocumento10 páginasClinical Observation On Greeva StambhaSanjay SoniAún no hay calificaciones
- DobutamineDocumento1 páginaDobutamineAnnie SethiAún no hay calificaciones
- Section 3: Functional DiagramsDocumento10 páginasSection 3: Functional DiagramsHatman ManhatAún no hay calificaciones
- Degenhardt Melissa - Sowk Community PaperDocumento8 páginasDegenhardt Melissa - Sowk Community Paperapi-358773906Aún no hay calificaciones
- 11 01 06 Bambach BrochureDocumento6 páginas11 01 06 Bambach BrochureFred StoreyAún no hay calificaciones
- Is Your Home Harming You?Documento4 páginasIs Your Home Harming You?Iris Brooks100% (2)
- Fluoroscopy-Guided Periradicular Injections in SpineDocumento8 páginasFluoroscopy-Guided Periradicular Injections in SpineAlvaro Perez HenriquezAún no hay calificaciones
- Xerostomia BrochureDocumento2 páginasXerostomia Brochureapi-312451539Aún no hay calificaciones
- Checklist of Nonverbal Pain IndicatorsDocumento41 páginasChecklist of Nonverbal Pain IndicatorsantipaticoAún no hay calificaciones
- Rudolfo S. Agustin JR.: Ragus003@odu - EduDocumento2 páginasRudolfo S. Agustin JR.: Ragus003@odu - EduRudolfo AgustinAún no hay calificaciones
- Canadian GPC AnsiedadDocumento83 páginasCanadian GPC AnsiedadFabiana FloresAún no hay calificaciones
- Testicular Self ExaminationDocumento3 páginasTesticular Self ExaminationEmman Ramos100% (1)
- Sample Nurse Aide ResumeDocumento2 páginasSample Nurse Aide ResumeMayta Bacud RamosAún no hay calificaciones
- How Would We Know If Psychotherapy Were Harmful?: What Do We Mean by Harm?Documento13 páginasHow Would We Know If Psychotherapy Were Harmful?: What Do We Mean by Harm?CoordinacionPsicologiaVizcayaGuaymasAún no hay calificaciones
- Hasler 2004 Prochaska Eating DisordersDocumento7 páginasHasler 2004 Prochaska Eating Disordersandra_coralia9112Aún no hay calificaciones
- What Did Freud Get RightDocumento3 páginasWhat Did Freud Get RightGustavo AvendañoAún no hay calificaciones
- Periodic Safety Update ReportDocumento28 páginasPeriodic Safety Update ReportnidhisaxenaAún no hay calificaciones
- Non Hodgkin's Lymphoma: Rakesh BiswasDocumento16 páginasNon Hodgkin's Lymphoma: Rakesh BiswasDayledaniel SorvetoAún no hay calificaciones
- Introduction - NephrolithiasisDocumento5 páginasIntroduction - NephrolithiasismissmakaiAún no hay calificaciones
- Factors Affecting Bone Development, Growth, and RepairDocumento6 páginasFactors Affecting Bone Development, Growth, and RepairJoseph Arnold AlmonteAún no hay calificaciones
- Nursing Care Plan (CVA)Documento2 páginasNursing Care Plan (CVA)Mel Rodolfo50% (2)
- Self Worth and PerfectionismDocumento1 páginaSelf Worth and Perfectionismapi-490252017Aún no hay calificaciones
- Neonatal SepsisDocumento44 páginasNeonatal SepsisIsabel Barredo Del MundoAún no hay calificaciones