Documentos de Académico
Documentos de Profesional
Documentos de Cultura
Pericardial Diseases - Dr. Bartolome
Cargado por
Medisina101Descripción original:
Derechos de autor
Formatos disponibles
Compartir este documento
Compartir o incrustar documentos
¿Le pareció útil este documento?
¿Este contenido es inapropiado?
Denunciar este documentoCopyright:
Formatos disponibles
Pericardial Diseases - Dr. Bartolome
Cargado por
Medisina101Copyright:
Formatos disponibles
adiuvante Dei gratia doctorum factionis 2014-2015
CARDIO:PERICARDIAL DISEASES Dr. Bartolome
Pericardial Diseases Essentials of Diagnosis
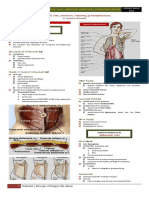
Pericardium
Visceral and Parietal Pericardium Central chest pain aggravated by coughing, inspiration, or
recumbency
Visceral pericardium is a serous membrane separated from the Pericardial friction rub on auscultation
parietal pericardium by a small quantity (15-50ml) of fluid.
Characteristic ECG changes
Inside the pericardial cavity (space between visceral and parietal
pericardium) is pericardial fluid of about 50-70cc (ibasa notes)
Prevalence
Functions of Pericardium
Admitting diagnosis in 0.1% of hospital admissions
1. Prevents sudden dilation of the cardiac chambers during exercise More common in men than in women
and with hypervolemia In pericarditis class, there is chest pain but you must remember that
2. Restricts the anatomic position of the heart when you see a patient having a chest pain you should know the
3. Minimizes friction between the heart and surrounding structures risk probability of the patient having that condition.
4. Prevents displacement of the heart and kinking of the great vessels Eto, katuladnitongbatangetopag nag-chest pain (simiki? )
5. Retards the spread of infections from the lungs and pleural cavities anongiisipinnyo? Iisipinnyobana may ischemic heart disease sya?
Unlikelydiba? Thats why you always have to remember the risk
factors for the development of heart disease.
Hindi nyodapatkinakalimutanang modifiable and non-modifiable
risk factors diba?
So what are the modifiable risk factors?
Hypertension
DM
Hyperlipidemia
Smoking
obesity
Sedentary lifestyle
And the non-modifiable risk factors are as follows:
45 yo male or 55 yo female
Early history of CAD
Eto, katuladnito (miki again?) pwede bang ischemic heart disease
yan? Rheumatic heart disease pwede pa.
At the ER you should be able to diagnose ischemic heart disease
within 10min., and then do the PE you have to rule out allthe
things that can cause death.
Anobayung chest pain napwedengmamatayyung patient mo?
Myocardial ischemia or infarction
Pneumothorax
Aortic dissection
Acute pulmonary embolism
All of these can cause acute chest pain and dyspnea and all are life
threatening condition.
Then, history, risk factors, diba?
Prolonged chest pain, more than 20 minutes will you consider it to
be MI? How do you diagnose a patient with MI? 1, 2, 3 anoyun?
Prolonged chest pain of more than 20 min
Acute Pericarditis You have to request for ECG and lastly
Definition Cardiac enzymes
So how about pulmonary embolism? Another term for acute PE is
acute corpulmonale. So you know that there is a risk for developing
inflammatory process involving the pericardium DVTanobayungmga risk factors for developing DVT? Patients who
results in a clinical syndrome with triad of chest pain, pericardial are immobile, have prosthesis, those who underwent orthopedic
friction rub, and changes in the ECG surgery, cancer patientsand then all of a sudden may dyspnea
so for pericardial diseases actually were talking about so, where will that be lodge? SaPulmonary artery, thats why it is
inflammation and we call that pericarditis. And this pericardial called pulmonary embolism. So, when you obstruct the pulmonary
inflammation can be acute or chronic. And that inflammation may artery what will happen next? Youll end up having pulmonary
have complications later and these are as follows: arterial hypertension, R ventricular hypertension, and venous
pericardial effusion or hypertension.So what is the physical examination? So you end up
constrictive pericarditis having R sided PE findings like neck vein engorgement in a patient
Pericardial effusion may be small in amount or large in amount, if it who is hypotensive???
is in large amount it may become what you call cardiac tamponade Another thing that you have to rule out is the possibility of having
disorders. pneumothorax, what do you expect to see? There is lagging of the
So basically the problem in pericardium is inflammation and that affected side; by percussion will you be able to appreciate
inflammation can later produce effusion and then constriction. pneumothorax? There will be what? Hyper-resonance on the
affected side; now in auscultation? There will be absence of breath Viral Pericarditis
sound on the affected side. Thats why in the ER you request for ECG
and Xray. Peronakitamonahindinagumagalaw, anonguunahinmo, Most common causes: coxsackievirus B, echovirus usual cause of
ECG or Xray? sipon and uboubonyo.
Sa aortic dissection? What is the presentation? Prolonged chest 4-fold increase in antiviral titer required for diagnosis
pain masyadongmatagal like 2 hours or 3 to 4 hours. What is the withprodrome of URTI mga 1-2 weeks that later complaints of
PE finding of aortic dissection that differentiates it with other severe pleuritic chest pain.
diseases mentioned? You have to palpate the pulses. Patients with Prognosis good usually self-limited
aortic dissection haveassymetrical pulse, but with normal ECG. You
can also request for chest Xray. Anongmakikitanyo? Theres Purulent Pericarditis
widening of the mediastinum.
So yanyungsinasabikosainyonaapatnapwedemagcausengdeath, but This is the one that causes problem compared to viral in origin.
not acute pericarditis. Predisposing Factors:
1. Thoracic Surgery
Common Causes of Pericarditis and Pericardial Effusion 2. Chemotherapy
3. Immunosuppression
Idiopathic the most common cause is idiopathic in origin. The 4. Hemodialysis
problem is that probably most of these are secondary to viral Acute onset: high fever, chills, night sweats, dyspnea; chest pain or
infection. Its very hard to document a viral infection. Sino friction rub rare
nanakakitasainyong viral titer result?Nakikitakolangsalibro. Thats Cardiac tamponade common (42%-77%) dont forget that
why probably this idiopathic cause is due to viral infection. Puro purulent pericarditis is associated with cardiac tamponade. You
clinical tayosapinas. really need to document if it is really purulent.
Infectious bacterial, viral, fungal, HIV Paanomosususpentyahinna may purulent pericarditis yan? So,
Myocardial Infarction yanyungmga people prone to have infection later developing
Radiation cardiac tamponade. Once you have cardiac tamponade it is a
Postoperatively after open heart surgery medical emergency. Additional medical emergency,
Chest trauma blunt, sharp kaninaapatdiba? Oh, plus one!
Malignancy High mortality rate kasiyungmga patient immunosuppressed.
1o Mesothelioma, angiosarcoma Hospital admission with immediate pericardiocentesis + IV broad
Metastatic lung, breast, bone, lymphoma, melanoma spectrum antibiotics mandatory followed by early surgical
Collagen vascular disease RA, SLE drainage.
Metabolic uremia, hypothyroidism Kailangantanggalinyung fluid agad and then give anitbiotics.
Pharmacologic penicillin, phenytoin, procainamide, hydralazine,
minoxidil, cromolyn Na, methysergide, doxorubicin Tuberculous Pericarditis
Para saanang hydralazine? Hydralazine is for
hypertension specifically for pregnant patient. 1%- 2% of cases of PTB
Cromolyn Na for allergy. You must be careful. Increased risk in patients who are immunocompromised or HIV (+)
if patient have Tuberculous pericarditis, you always have to rule
Signs and Symptoms out the possibility of having HIV. Actually for patient suffering from
TB not in Philippines, the probability that that patient is suffering
Most common symptom: chest pain from HIV is very high! More than 30-40%. Sa US now, pag positive
- Described as pleuritic in nature. TB ka, kahit PTB lang, automatic nagpapoHIV test na din sila. Satin,
- severe, sharp, retrosternal hindikapinoypagwalang TB. LOL
- often radiating to the neck, shoulder, or back Slow development of non-specific symptoms; chest pain and
- worsens in the supine position and with inspiration friction rub often absent
- Improved with sitting upright and leaning forward but not always Chest radiography useful when findings of PTB present
present. Hospital admission indicated + anti-TB therapy (e.g. Rifampicin,
- Now, dont forget your PPQRRST, for any kind of pain you use this INH, streptomycin, ethambutol) started promptly
as a guide. You can do this in 1 minute. Pericardial fluid analysis: very high specific gravity, very high
- How will you differentiate MI from unstable angina pectoris? Thats protein (>6 g/dL), & predominantly lymphocytic cells
why it is important to use that guide. Pericardial biopsy with acidfast bacilli PCR recommended
Friction Rub
- Scratchy, grating, high-pitched friction rubs (squeak of leather of Uremic Pericarditis
a new saddle)walangkabayosi doc so hindinyaalamyan
- Due to fibrous deposits in the pericardial space Incidence: 6%-10% of patients with advanced renal failure before
- With three components: initiation of dialysis
1. atrial systole BUN usually >60 mg/dL
2. ventricular systole Large hemorrhagic effusion due to impaired platelet function
3. early ventricular diastole common
- best heard during inspiration at left lower sternal border, with Dialysis indicated
patient leaning forward
- Thats why pagnagPE kayo you always have to do this. Actually this Dialysis - Associated Pericarditis
is the best position for you to appreciate aortic and pulmonic
sounds and also at the same time the friction rub.so you have 3. An irony, since patient with uremic pericarditis needs dialysis.
- Ano daw Brazilian? LOL Si Santillan girl or boy? waaaah! The main problem here is inadequate dialysis treatment.
Ditokasisapinas 2x a week lang, and ideally dapat minimum of 3x a
Specific Types week yan.
Idiopathic Pericarditis Cause by fluid overload fluid usually serous
Intensification of hemodialysis indicated
Cause difficult to establish Improvement in 1-2 weeks
Most common diagnosis
Shiela and Young
Work hard in silence
let success make the noise Page 2 of 8
Treatment is give NSAID peropwedeng acute pericarditis yun
Post MI Pericarditis because of the trauma, but one thing about costochondritis is you
can localize the pain now.
Common complication in patients with MI (25%-40%)
1. within 3-10 days after MI Diagnosis
2. development correlates with extent of necrosis
more frequent with anterior than inferior infarcts Remains a clinical diagnosis based on:
Happens esp. in large anterior infarction, so pag may post MI 1. History
pericarditis ka, ibigsabihin nun malakiang infarction. The size 2. PE
depends on what artery is affected. 3. ECG there is typical ECG changes in acute pericarditis.There is
associated with a higher 1-year mortality rate and incidence of CHF diffuse ST segment elevation in acute pericarditis. Dibarinurule out
Diagnosis requires: natinsyasa MI? anobayungsa MI, diffuse or localized? Localized. It
1. Symptoms or a new pericardial friction rub only involves the arterial supply affected. Remember anatomy.
2. ECG changes Aside from that, there is also PR segment depression in acute
typical ST elevation seen with acute pericarditis pericarditis. In MI, it doesnt happen except if you have auricular
persistently positive T waves more than 2 days post-MIor infarction.
normalization of previously inverted T waves Other imaging studies: CT scan, MRI, Echocardiography not really useful
so, pericarditis has chest pain, what differentiates it from MI? except if with pericardial effusion.
one is pleuritic the other is not
MI has ECG changes while pericarditis none
Another is Cardiac enzyme but you have to know its
release pattern.
CKMB 6-8hours present in blood; peak- 24-
48 hours and would last for 72 hours
Troponin T/I - 6-8hours present in blood;
peak- same but would last for 10-14 days
Can I use trop T if may chest pain on 5th day? No. kasi
positive pa sya. You will use CKMB, kasiwalanasya after
3 days. (diko gets, pabasana lang.)
Actually class if you have to request for cardiac
enzymes, dapat serial yun, 0, 6, 12, and 14. Kaya
langpagsiguradonayung doctor hindinasiniserial.
Pagnatitipid pa yun, kungnakitanana may ST elevation
yunhindinamagrerequestyun.
Post Cardiac Injury Pericarditis
Dresslers syndrome
occurs 2-3 weeks after MI or open heart surgery
Autoimmune component and possibly a latent viral infection
implicated
consists of pleuritic chest pain, fever, leukocytosis, and a
pericardial friction rub
Malignancy - Associated Pericarditis
caused mostly by metastatic disease mostly with tumor
metastatic to the heart. Nagkakaroonnang cardiac tamponade
physiology.
Bronchogenic or breast carcinoma, Hodgkins disease and
lymphoma are common you have to rule this out immediately.
Diagnosis is based on analysis of pericardial fluid cytology
sensitivity ranging from 70% to 90%
specificity of up to 95% to 100%
Radiation Pericarditis
Recent or remote mediastinal radiation
Any time from weeks to months after the exposure
Paminsannakaligtaan to. Pag may history ng malignancy yung
patient mo, dont forget to ask if nagkaroonbang radiation
treatment before. Can be used as ddx. - In AP, concave. In MI convex, payong.
Trauma Pericarditis
May accompany sharp or blunt trauma and even a minimally
invasive procedure such as cardiac diagnostic or interventional
catheterizations
Iba pa yungcostochondral fracture/ inflammation
Shiela and Young
Work hard in silence
let success make the noise Page 3 of 8
Stage I Acute Pericarditis Colchicine for persistent or refractory cases of
Dresslers syndrome and idiopathic pericarditis
Anticoagulants avoided during acute phase reduce
bleeding and tamponade
Pericardiectomy
Indications:
1. development of pericardial constriction
2. recurrent pericarditis rare
most definitive procedure
30-day perioperative mortality rateis about 5%
Outcome
Patients with uncomplicated acute pericarditis should have regular
follow-up after the initial visit to ensure resolution of symptoms
and rule out the development of constrictive symptoms.
PERICARDIAL EFFUSION
Myocardial Infarction Definition
increased amount of pericardial fluid
Essentials of Diagnosis
echocardiographic demonstration of pericardial fluid
Echocardiogram- to confirm the diagnosis
Acute Pericarditis: Chest Radiography
May be entirely normal unless there is a pericardial effusion
causing cardiomegaly or changes caused by underlying disease
Acute Pericarditis: Echocardiography
Indications:
1. symptoms persisting for longer than 1-2 week
2. presence of hemodynamic abnormalities
3. clinical suspicion of a large or increasing pericardial effusion, or
4. recent cardiac surgery
Treatment
most cases uncomplicated and self-limited kahitwalanggagawin,
but dont forget that acute pericarditis is with pain and
inflammation. So, what can you give to reduce pain and
inflammation? So you give drug with analgesic and anti-
inflammatory property. And that is NSAIDs. Most common causes of large effusions are:
Indications for an imaging modality, hospital admission, or both: 1. Malignancy (25% of cases)
1. clinical suspicion of a large effusion
2. Infection (27%) most common cause is secondary tuberculosis
2. hemodynamic instability
3. Collagen vascular disease (12%)
3. severe pain or other symptoms
4. suspicion of a serious underlying condition, or 4. Chest radiation (14%)
5. any other signs or symptoms of clinical instability or Most common Cardiovascular manifestation of acquired immunodeficiency
impending deterioration syndrome worse outcome ( BOARD EXAM QUESTION)
HIV + pericardial effusionassociated with poor prognosis,
Medical Management WHY? Actually it is not secondary to AIDS that produces Pericardial
Treatment of underlying disease- mainstay inflammation,
NSAIDs for pain relief it its secondary to secondary problem of HIV infection
1. Ibuprofen 400 mg q8h , it is secondary to pneumocystis or Kaposi sarcoma or tb going to
2. Ketorolac tromethamine parenteral pericardium,
3. Contraindicated in the early period (<7-10 days) after MI (may so ibig sabihin niyan talagang highly immunosupress yung patient,
predispose to cardiac rupture) use aspirin instead why? konting sipon lang ng rhinovirus, deads na!
You give it as an anti-inflammatory drug and as an
antithrombotic, not as analgesic.
Prednisone high dose taper over 3 weeks
1. if pericarditis recurs (20%-30% of patients OR
2. response to NASAIDs is poor
Shiela and Young
Work hard in silence
let success make the noise Page 4 of 8
Pathophysiology
Pericardial sac normally contains 15-30 ml of fluid can hold 80-200ml
of fluid acutely and even up to 2L if the fluid accumulates slowly
development of tamponade depends on the rate of accumulation rather
than on the volume of the effusion typically, signs of right ventricular
diastolic failure develop first, followed by left-sided symptoms
Symptoms
Arise from the compression of surrounding structures (lung, stomach, phrenic
nerve) or diastolic heart failure
Include:
1. Chest pressure or pain
2. Dyspnea
3. Nausea, abdominal fullness, and dysphagia
4. Phrenic nerve irrirtation may cause hiccup Echocardiography
Hiccup- merong patient dati hiccup ng hiccup, wala daw nagtatanong Echo-free space between visceral and parietal pericardium the
sa PE, eh yung patient nag underwent nuclear ablation of thyroid extent of the space defines the size of the effusion
gland,
Large effusions may produce the picture of a swinging heart
so pinaxray, ang laki ng heart! Yun pala yung patient is suffering
severe hypothyroidism tapos walang nagbother to look up the neck Imaging modality of choice for diagnosing a pericardial effusion
, eh 1 week na yung patient, nalusutan na daw lahat, yung but may miss small loculated effusions
clerk,intern, 3 residents, and even the consultant and the another
consultant., eh nagtamponade yung patient, Sizing of Small Medium Large
Kaya daw ipractice yung P.E.. may medical officer pang di nag PE, Pericardial
tapos after 1 hr, deads yung patient. Effusion by
NO ONE CAN ARGUE ON YOUR PE,! In short mag P.E. or change your Echocardiogra
course.( halerrrr!!! Third year na kaya! ) phy Size
Vol (ml) <100 100-500 >500
Physical Examination Localization Localized Circum- Circum-
ferential ferenial
Small effusion PE unremarkable ,asymptomatic Width <1 1-2 >2
Large effusion:
1. Muffled heart sounds Analysis of Pericardial Fluid
2. Ewarts sign (dullness to percussion, bronchial breath sounds, and egophony 1. CBC
below the angle of the left scapula) rare 2. Chemistry panel
3. With increasing volume of the effusion, signs and symptoms of cardiac 3. ESR
tamponade may occur
Diagnostic pericardiocentesis done if the cause is unclear or any of the
Diagnosis following is suspected
1. Malignancy
Electrocardiography 2. TB
Low voltage & electrical alterans 3. Fungal or bacterial infection
Therapeutic pericardiocentesis done for large effusions that are
increasing in size or causing tamponade
Diagnostic pericardiocentesis done if the cause is unclear or any of the
following is suspected
1. Malignancy
2. TB
3. Fungal or bacterial infection
Therapeutic pericardiocentesis done for large effusions that are increasing in
size or causing tamponade
Chest Radiography
Cardiomegaly occurs if there is more than 250 ml of fluid in the
pericardial sac
Shiela and Young
Work hard in silence
let success make the noise Page 5 of 8
Exudate vs. Exudate Transudate Pericardial tamponade end up in having Venous Hypetension
Transudate
Parameter Essentials of Diagnosis
Cause Malignancy Radiation
Infectious, Uremia Increase jugular venous pressure with an obliterated y descent
parainfectious Hypothyroidism Pulsus paradoxus
Postpericardiotomy Trauma Echocardiographic evidence of right atrial and ventricular collapse
syndrome
Equal diastolic pressures in all four cardiac chambers
Collagen vascular
disease
Spg (g/ml) >1.015 <1.015 Pathophysiology
Elevated intrapericardial pressure progressive limitation of mostly early
Total protein >3.0 <3.0
diastolic ventricular filling low cardiac output
Fluid-to-serum >0.5 <0.5
protein ratio
Symptoms
Fluid-to-serum LDH >0.6 <0.6
Symptoms resulting from decreased cardiac output and congestion:
Fluid-to-serum <1.0 >1.0 dyspnea,
glucose ratio
chest discomfort
weakness restlessness
Treatment
Agitation
Medical Management
Diuretics help decrease the intensity of fluid overload symptoms if present Drowsiness
Effusions causing pretamponade or tamponade immediate drainage Oliguria
Volume expansion and inotropic for hemodynamic stabilization pending anorexia
drainage If the tamponade develops acutely as a complication of an acute MI (free
wall rupture) or trauma catastrophic, with sudden death or shock and
Pericardiocentesis high mortality
Echocardiographically guided pericardiocentesis is safe and
effective Physical Examination
Indications: Classic findings Becks triad (10% to 40% of patients):
1. A large effusion with hemodynamic compromise or tamponade 1. Hypotension
2. For diagnostic purposes 2. JVD
3. Muffled heart sounds
Surgical Treatment Manifestations are right sided(neckvein engorgement,ascites, and
1. Percutaneous Balloon Pericardiotomy bipedal edema)
Least invasive Other things that produced your massive pleural effusion
Used mostly for neoplastic effusion with a poor prognosis as a can also produce these clinical manifestations such as muffling of
palliative treatment
the heart sound bec of that fluid
Success rate for relieving re-accumulation of pericardial fluid is 85%
Since there is fluid in between the precordium, dati kasi walang
to 92% at 30 days
2. Subxiphoid Pericardiostomy fluid, now there is a large fluid , it will muffles the heart sound s the
Known as a pericardial window transmission on the stethoscope Muffling of the heart sound-
May be done under local anesthesia humihina yung heart sounds to the point na hindi mo marinig
High success rate, with few complications talaga.
Recurrence of fluid accumulation is rare
Ewart sign- dullness to percussion ,brochial breath sound
Cardiac Tamponade ,egophony in the angle of scapula-
Definition where will you look for this sign?BACK,LEFT, kasi andun yung
heart... lumaki yung cardiac silhouette , so nacompress yung
Occurs when fluid accumulation in the finite pericardial space lungs cardiac t
causes an increase in pressure, with subsequent cardiac
compression and hemodynamic compromise Ewart's sign is a set of findings on physical examination in people
Pag nagka effusion,lalaki yan,magkakaroon ng pericardial space with large collections of fluid around their heart (pericardial
with fluid inside, effusions).
and thats fluid inside will have increase intracardial pressure Dullness to percussion (described historically as "woody" in
quality), egophony, and bronchial breath sounds may be
and it will compress the heart.
appreciated at the inferior angle of the left scapula when the
In the left heart, which is much thicker than your right heart,
effusion is large enough to compress the left lower lobe of the lung,
and thats why when you have compreesion, the one that will be causing consolidation or atelectasis.
easily compress is your right side of the heart( the right ventricle
and the right autirum) Tachycardia, tachypnea, hepatomegaly common
It will not allow blood flow coming from the veins going to the Pulsus paradoxus inspiratory decline in systolic BP of more than 10
right atrium and right ventricle mmHg due to compression and poor filling of the LV caused by
And it will Decrease preload, decrease CO, Decrease BP and as increased venous return to the right side of the heart
-during inspiration tapos medyo nawala-wala pait is pulsus
compensatory mechanism it will dec your heart rate Pericardial
paradoxus or alterans
tamponade with Tachycardia
Since your not allowing blood flow from great arc veins going to
right atrium venous hypertension
Shiela and Young
Work hard in silence
let success make the noise Page 6 of 8
Hyoptension, neck veing engorgement, muflled heart
sound + narrow pulse pressure+ pulsus paradoxus
Pericardial tamponade(MEDICAL EMERGENCY)
Diagnosis
Electrocardiography
Abnormal findings may include:
1. Electrical alternans - height of QRS varies like 3 mvolt, 5,8 millivolts.
Check the height of ECG.
It is commonly seen on pt with neck vein engorgement,
cardiomegalySUSPECT CARDIAC TAMPONADE
Massive pericardial effusion
you need at least 250 cc of pericardial fluid for you to
produce Cardiomegaly secondary to Pleural effusion,
Cardiothoracic ratio of >0.5 or something like 0.7
Typical water bottle configuration
2. Low voltage
3. Changes associated with acute pericarditis
Since there is a fluid in between the transmission of electrical potential
going to the ECG DOUBLE lean lead ecg? ??? ano d daw? Sorry ..
QRS is small
Lean? Leads- at least 5 millivolts( para hind maconsiderdouble...)
Chest lead- V1-V6- 5 millivolt;
Lead II and V -7 millivolts
Lead 3 and 4 9millivolts
IF hindi ganito yung value, we can consider na meron Double ...
Transthoracic Echocardiography
Sensitive finding for tamponade physiology is inferior vena
cava plethora, with absent inspiratory collapse
Pericardial Constriction/ Constrictive Pericarditis
Right ventricle and atrial collapse on echocardiography is the
most accurate finding for diagnosis Definition
ECHOCARDIOGRAPHY- confirms the dx of pericardial
effusion and cardiac tamponade and to the point that An abnormal thickening of the pericardium, resulting in impaired
effusion is called swimming heart ventricular filling and decreased cardiac output
Most cases idiopathic
Right Heart Catheterization May have history of acute or chronic pericarditis
Most typical finding: equalization of mean right atrial, right ventricular
and pulmonary artery diastolic, and mean pulmonary capillary wedge Essentials of Diagnosis
pressures. Markedly elevated JVP with accentuated x and y descent and
Kussmauls sign
Treatment Kussmauls sign- enlargement of neck vein during deep inspiration (
Medical emergency Normal:collapsed neck vein )
Remove the fluid Kussmaul's sign is a paradoxical rise in jugular venous
Immediate hospital admission and prompt pressure (JVP) on inspiration.
pericardial drainage by pericardiocentesis It can be seen in some forms of heart disease and is
If follow-up echocardiography documents fluid re-accumulation usually indicative of limited right ventricular filling due
pericardial window should be considered to right heart failure.
Infection risk associated with a pericardial drain increases after 48 hours Pericardial knock on auscultation
MRI, CT or echocardiographic imaging showing a thickened
Differential Diagnosis pericardium
1. Right-sided heart failure
2. Right ventricular infarction
3. Constrictive pericarditis Pathophysiology
4. Pulmonary embolism
Initiating event causes a chronic inflammatory pericardial process fibrinous
Treatment thickening & calcification of pericardium limitation of intrapericardial
Immediate hospital admission and prompt pericardial drainage by volume impaired ventricular filling decreased cardiac output right and
pericardiocentesis left ventricular failure
If follow-up echocardiography documents fluid re-accumulation
pericardial window should be considered
Infection risk associated with a pericardial drain increases after 48
hours
Shiela and Young
Work hard in silence
let success make the noise Page 7 of 8
Calcification of the pericardium by CT
Physical Examination
Increased ventricular filling pressures cause:
1. Jugular vein distention
2. Kussmauls sign absent inspiratory decline of jugular venous distention
Auscultation: muffled heart sounds and occasionally a
characteristic pericardial knock (60-200 milliseconds after the
second heart sound)
Diagnosis
ECG
Non-specific but low voltage of QRS complex may be seen
Laboratory tests
Brain natriuretic peptide (BNP) serum biomarker; distinguish
constrictive from restrictive pericarditis higher in resetrictive
Echocardiography
Best imaging modality for assessing
hemodynamic parameters non-invasively
Doppler echocardiographic
findings have the highest sensitivity and specificity for detecting
constrictive physiology
MRI & CT
CT is the imaging modality of choice to evaluate the
pericardium
Pericardial calcifications may easily be identified on CT
Finding of thickened pericardium on the CT or MRI is specific
for constriction
Treatment
Medical treatment is difficult and does not affect the natural
progression or prognosis of the disease
Diuretics and a low-sodium diet for patients with mild to moderate
(New York Heart Association [NYHA] Class I or II) symptoms or
contraindications to surgery
For most patients, pericardiectomy is advised, with 80% to 90% of
patients experiencing improvement and 50% complete relief of
symptoms
remove the pericardium
Shiela and Young
Work hard in silence
let success make the noise Page 8 of 8
También podría gustarte
- Cardiovascular MneumonicsDocumento10 páginasCardiovascular MneumonicsKaly RieAún no hay calificaciones
- Cardiac ArrythmiasDocumento63 páginasCardiac ArrythmiasSankara SubramanianAún no hay calificaciones
- EBM - 5. Adrenal DisordersDocumento101 páginasEBM - 5. Adrenal DisordersBRI KUAún no hay calificaciones
- Cardiac MurmursDocumento28 páginasCardiac MurmursAlvin BlackwellAún no hay calificaciones
- Cardiac MurmursDocumento3 páginasCardiac MurmursDanielleAún no hay calificaciones
- Up To Date in Internal MedicineDocumento366 páginasUp To Date in Internal Medicinez13407100% (2)
- DAVIS MedSurg Notes Nurse S Clinical Pocket Guide FA Davis 2007Documento242 páginasDAVIS MedSurg Notes Nurse S Clinical Pocket Guide FA Davis 2007amaliea234100% (1)
- Internal MedicineDocumento161 páginasInternal Medicinemain.genevive.dilig100% (1)
- SURGERY Lecture 5 - Abdominal Wall, Omentum, Mesentery, Retroperitoneum (Dr. Wenceslao)Documento13 páginasSURGERY Lecture 5 - Abdominal Wall, Omentum, Mesentery, Retroperitoneum (Dr. Wenceslao)Medisina101Aún no hay calificaciones
- SURGERY Lecture 3 - Abdominal Hernia (Dr. Mendoza)Documento12 páginasSURGERY Lecture 3 - Abdominal Hernia (Dr. Mendoza)Medisina101100% (1)
- Ishemic Heart Disease-y-II-2011 (Student Version)Documento51 páginasIshemic Heart Disease-y-II-2011 (Student Version)kays30002403Aún no hay calificaciones
- SURGERY Lecture 2 - Liver & Gallbladder (Dr. Wenceslao)Documento19 páginasSURGERY Lecture 2 - Liver & Gallbladder (Dr. Wenceslao)Medisina101100% (1)
- Pedia Cardiology 2Documento5 páginasPedia Cardiology 2Medisina101Aún no hay calificaciones
- Health HistoryDocumento19 páginasHealth HistoryAngelene Caliva100% (1)
- Cvspa05 Valvular Heart DiseaseDocumento8 páginasCvspa05 Valvular Heart DiseaseRobert So JrAún no hay calificaciones
- Panre and Pance Review Cardiovascular IIDocumento26 páginasPanre and Pance Review Cardiovascular IIThe Physician Assistant Life100% (1)
- Mkasap Endocrinology NotesDocumento6 páginasMkasap Endocrinology NotesUm HamoOdAún no hay calificaciones
- Pathophysiology of Heart FailureDocumento2 páginasPathophysiology of Heart FailureJaysellePuguonTabijeAún no hay calificaciones
- Abnomalites of ECGDocumento81 páginasAbnomalites of ECGgrreddy8364320Aún no hay calificaciones
- Cardiology (300) MRCP Part 1 2014Documento927 páginasCardiology (300) MRCP Part 1 2014elite949150% (2)
- 10 CardiomyopathyDocumento71 páginas10 CardiomyopathyAnonymous vUEDx8100% (5)
- H P MedicineDocumento2 páginasH P Medicinerishu2Aún no hay calificaciones
- Cardiomyopathy and Myocarditis HarrisonsDocumento62 páginasCardiomyopathy and Myocarditis HarrisonsGrace CastilloAún no hay calificaciones
- Cardiomyopathy and MyocarditisDocumento8 páginasCardiomyopathy and Myocarditisoddone_out100% (1)
- Presentation Liver CirrhosisDocumento26 páginasPresentation Liver CirrhosisFaye Dominique Roxas PalmaresAún no hay calificaciones
- Acute Coronary Syndrome - AMBOSSDocumento31 páginasAcute Coronary Syndrome - AMBOSSSarah Ronquillo100% (1)
- Treatment of Resistant and Refractory HypertensionDocumento21 páginasTreatment of Resistant and Refractory HypertensionLuis Rodriguez100% (1)
- DIFFERENTIALS and MnemonicsDocumento20 páginasDIFFERENTIALS and MnemonicsqurbanAún no hay calificaciones
- Surgery II - Pancreas 2014Documento20 páginasSurgery II - Pancreas 2014Medisina101Aún no hay calificaciones
- MED1 Samplex Rationale 6 - Endocrine DisordersDocumento6 páginasMED1 Samplex Rationale 6 - Endocrine DisordersMartina GarciaAún no hay calificaciones
- Heart BNHADocumento13 páginasHeart BNHAX OloGyAún no hay calificaciones
- Heart BNHADocumento13 páginasHeart BNHAX OloGyAún no hay calificaciones
- Valvular Heart DiseaseDocumento43 páginasValvular Heart Diseaseurmila prajapatiAún no hay calificaciones
- Rheumatic Heart Disease AustrliaDocumento63 páginasRheumatic Heart Disease AustrliaMuhammad Reza100% (2)
- Alarm Symptoms of Hematoonco in Pediatrics: Dr. Cece Alfalah, M.Biomed, Sp.A (K) Pediatric Hematology and OncologyDocumento22 páginasAlarm Symptoms of Hematoonco in Pediatrics: Dr. Cece Alfalah, M.Biomed, Sp.A (K) Pediatric Hematology and OncologyMuhammad ArifAún no hay calificaciones
- Bates Physical Examination RED NOTESDocumento2 páginasBates Physical Examination RED NOTESAmanda Gomez100% (1)
- SURGERY Lecture 4 - Breast (Dra. Fernandez)Documento15 páginasSURGERY Lecture 4 - Breast (Dra. Fernandez)Medisina101100% (1)
- Head and Neck SurgeryDocumento15 páginasHead and Neck SurgeryMedisina101100% (1)
- SURGERY Lecture 1 - Small Intestine (Dr. Mendoza)Documento16 páginasSURGERY Lecture 1 - Small Intestine (Dr. Mendoza)Medisina101100% (1)
- Third-Year OSCE Manual 2019-2020Documento17 páginasThird-Year OSCE Manual 2019-2020Agleema AhmedAún no hay calificaciones
- Goljan - CardiovascularDocumento22 páginasGoljan - Cardiovascularcollege3Aún no hay calificaciones
- Approach: A. How The Kidney Handle The Proteins?Documento9 páginasApproach: A. How The Kidney Handle The Proteins?Rashed ShatnawiAún no hay calificaciones
- Source NotesDocumento30 páginasSource NotesChris Jardine Li100% (1)
- CardiomyopathyDocumento17 páginasCardiomyopathysarguss1450% (2)
- Pericarditis 65 SlidesDocumento65 páginasPericarditis 65 SlidesAtifBhoreAún no hay calificaciones
- Pericardial DiseaseDocumento59 páginasPericardial DiseaseGunawan Yoga100% (1)
- PericarditisDocumento29 páginasPericarditisPavin KumarAún no hay calificaciones
- Pericardial Diseases 3rd Yr BMTDocumento38 páginasPericardial Diseases 3rd Yr BMT211941103014100% (1)
- Cardiovascular DisordersDocumento9 páginasCardiovascular DisordersChristine Evan HoAún no hay calificaciones
- PEDIA - Cardio (Esguerra) PDFDocumento9 páginasPEDIA - Cardio (Esguerra) PDFMedisina101Aún no hay calificaciones
- Diseases of The Aorta - Dr. Deduyo PDFDocumento11 páginasDiseases of The Aorta - Dr. Deduyo PDFMedisina101Aún no hay calificaciones
- Acquired Heart DiseaseDocumento44 páginasAcquired Heart DiseaseMedisina101Aún no hay calificaciones
- MCQ Internal Medicine PDFDocumento448 páginasMCQ Internal Medicine PDFAyaa Yousef100% (5)
- Congenital Heart Diseases, A Simple Guide to these Medical ConditionsDe EverandCongenital Heart Diseases, A Simple Guide to these Medical ConditionsAún no hay calificaciones
- Congenital Heart DiseaseDocumento106 páginasCongenital Heart DiseaseHarold DiasanaAún no hay calificaciones
- Torsade De Pointes, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsDe EverandTorsade De Pointes, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsAún no hay calificaciones
- Valvular Heart Diseases Part 2 - Dr. BartolomeDocumento9 páginasValvular Heart Diseases Part 2 - Dr. BartolomeMedisina101Aún no hay calificaciones
- Peritoneal Dialysis SeminarDocumento25 páginasPeritoneal Dialysis SeminardrresmiajithAún no hay calificaciones
- GIT Physical Examination 4th YearDocumento60 páginasGIT Physical Examination 4th YearKholoud Kholoud100% (1)
- Hemodialysis Emergencies: Core Curriculum 2021.Documento14 páginasHemodialysis Emergencies: Core Curriculum 2021.Tariq ZayanAún no hay calificaciones
- Fundamentals Nursing Active Learning 1st Edition Yoost Crawford - Test BankDocumento44 páginasFundamentals Nursing Active Learning 1st Edition Yoost Crawford - Test BankRaymondCenteno100% (3)
- Medical Case 1: Language Centre of Malahayati University at 2010Documento16 páginasMedical Case 1: Language Centre of Malahayati University at 2010putri1114Aún no hay calificaciones
- Hanson Infectious Diseases - Anamneza I StatusDocumento33 páginasHanson Infectious Diseases - Anamneza I StatusSilvia KesegAún no hay calificaciones
- Chest Pain Non TraumaDocumento45 páginasChest Pain Non TraumaTita LuthfiaAún no hay calificaciones
- Ventricular Septal Defect, A Simple Guide To The Condition, Treatment And Related ConditionsDe EverandVentricular Septal Defect, A Simple Guide To The Condition, Treatment And Related ConditionsAún no hay calificaciones
- Myocarditis, (Inflamed Heart Muscles) A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsDe EverandMyocarditis, (Inflamed Heart Muscles) A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsAún no hay calificaciones
- (MED1) 3.04 Approach To Hypertension (Dr. Bago-Azares)Documento11 páginas(MED1) 3.04 Approach To Hypertension (Dr. Bago-Azares)NoreenAún no hay calificaciones
- Notes On History Taking in The Cardiovascular SystemDocumento10 páginasNotes On History Taking in The Cardiovascular Systemmdjohar72Aún no hay calificaciones
- Grand Rounds - Pulmonary EmbolismDocumento25 páginasGrand Rounds - Pulmonary EmbolismAdrian CastroAún no hay calificaciones
- Cardiac Murmurs - 1p Cheat Sheet PDFDocumento1 páginaCardiac Murmurs - 1p Cheat Sheet PDFPkernAún no hay calificaciones
- Blood and Drugs Medicine NotesDocumento39 páginasBlood and Drugs Medicine Notesrahuul prasadAún no hay calificaciones
- Thyroid Status Examination OSCE GuideDocumento20 páginasThyroid Status Examination OSCE GuideemmaAún no hay calificaciones
- Bronchial AsthmaDocumento27 páginasBronchial AsthmachandrikaismailAún no hay calificaciones
- Internal Medicine Sample Osce Examination Component Questions eDocumento2 páginasInternal Medicine Sample Osce Examination Component Questions eFajar ChampionAún no hay calificaciones
- HivDocumento36 páginasHivfenendriyaniAún no hay calificaciones
- Aquifer InternalMedicine11 - 45Documento8 páginasAquifer InternalMedicine11 - 45JulieAún no hay calificaciones
- Rheumatic Fever and Rheumatic Heart DiseaseDocumento132 páginasRheumatic Fever and Rheumatic Heart DiseaseDamie FernandezAún no hay calificaciones
- Approximate Equivalents:: 0.100 Gmn. 1.00 GMDocumento8 páginasApproximate Equivalents:: 0.100 Gmn. 1.00 GMakane ryuAún no hay calificaciones
- Glomerulonephritis PresentationDocumento23 páginasGlomerulonephritis Presentationjacksonyu1234Aún no hay calificaciones
- Malassezia Furfur An-An Ap-Ap Naturally Found On The SkinDocumento48 páginasMalassezia Furfur An-An Ap-Ap Naturally Found On The SkinNikki ValerioAún no hay calificaciones
- AntibioticsDocumento30 páginasAntibioticsRoza RahbeniAún no hay calificaciones
- 3 Surgery - Mediastinum and PleuraDocumento6 páginas3 Surgery - Mediastinum and PleuraCassey Koi FarmAún no hay calificaciones
- Pulmonary Path PearlsDocumento33 páginasPulmonary Path PearlsCristi Popescu100% (1)
- Harrison TablesDocumento5 páginasHarrison TablesSANTHILAL ADHIKARLAAún no hay calificaciones
- Rhythms of Death MD1TALKDocumento1 páginaRhythms of Death MD1TALKAmalAún no hay calificaciones
- Peripheral Vascular Medicine - Dr. Deduyo PDFDocumento14 páginasPeripheral Vascular Medicine - Dr. Deduyo PDFMedisina101Aún no hay calificaciones
- Pedia Pulmo 2 10.18.16Documento73 páginasPedia Pulmo 2 10.18.16Medisina101Aún no hay calificaciones
- Appendix Skin Gi ManifestationsDocumento25 páginasAppendix Skin Gi ManifestationsMedisina101Aún no hay calificaciones
- General Surgery SMALL INTESTINES-Dr MendozaDocumento101 páginasGeneral Surgery SMALL INTESTINES-Dr MendozaMedisina101Aún no hay calificaciones
- 312 MR NathanielDocumento2 páginas312 MR NathanielCarl SantosAún no hay calificaciones
- Purulent Inflammations of Serous Cavities: PeritonitisDocumento14 páginasPurulent Inflammations of Serous Cavities: PeritonitisSara Abdul RahmanAún no hay calificaciones
- CH 29 - Management of Patients With Structural, Infectious, and Inflmmatory Cardiac DisordersDocumento15 páginasCH 29 - Management of Patients With Structural, Infectious, and Inflmmatory Cardiac DisordersPye Antwan Delva100% (1)
- Peri, Mio, EndoDocumento21 páginasPeri, Mio, Endosalsabilah arrahmanAún no hay calificaciones
- 2015 ESC Guidelines For The Diagnosis and Management of Pericardial DiseasesDocumento44 páginas2015 ESC Guidelines For The Diagnosis and Management of Pericardial DiseasesRoberto López MataAún no hay calificaciones
- Chest Pain in Pediatrics: Tisha K. Yeh, MD and Jay Yeh, MDDocumento5 páginasChest Pain in Pediatrics: Tisha K. Yeh, MD and Jay Yeh, MDMahmoud AbouelsoudAún no hay calificaciones
- Constrictive PericarditisDocumento54 páginasConstrictive PericarditisRazib AlamAún no hay calificaciones
- UNIT II MedicalDocumento34 páginasUNIT II Medicalangelax1.1Aún no hay calificaciones
- Acute Pericarditis PDFDocumento14 páginasAcute Pericarditis PDFMila CcasaniAún no hay calificaciones
- Pericardial Diseases: Acute PericarditisDocumento26 páginasPericardial Diseases: Acute PericarditisamsirakAún no hay calificaciones
- Curs Engleza Partea 2 Corectat - LariDocumento205 páginasCurs Engleza Partea 2 Corectat - LariVili Robert VoichițoiuAún no hay calificaciones
- Elective II FinalsDocumento15 páginasElective II FinalsAljon Dofeliz LlamasAún no hay calificaciones
- Care of Mother and Child at Risk or With Problems - Acute and Chronic (Lecture)Documento97 páginasCare of Mother and Child at Risk or With Problems - Acute and Chronic (Lecture)Mariah Alexis EncinaAún no hay calificaciones
- ONDOC Format & Guide To Oral PresentationsDocumento10 páginasONDOC Format & Guide To Oral PresentationsZainAún no hay calificaciones
- Cardiac Tumors: Dr. Asif WazirDocumento20 páginasCardiac Tumors: Dr. Asif WazirHillary BushnellAún no hay calificaciones
- Myocardia IschemiaDocumento114 páginasMyocardia Ischemiasara rababahAún no hay calificaciones
- Possible Causes of Chest PainDocumento4 páginasPossible Causes of Chest PainironAún no hay calificaciones