Documentos de Académico
Documentos de Profesional
Documentos de Cultura
Chronic Psoas Syndrome Caused by The Inappropriate Use of A Heel Lift PDF
Cargado por
Tito AlhoTítulo original
Derechos de autor
Formatos disponibles
Compartir este documento
Compartir o incrustar documentos
¿Le pareció útil este documento?
¿Este contenido es inapropiado?
Denunciar este documentoCopyright:
Formatos disponibles
Chronic Psoas Syndrome Caused by The Inappropriate Use of A Heel Lift PDF
Cargado por
Tito AlhoCopyright:
Formatos disponibles
CASE REPORT
Chronic Psoas Syndrome Caused by the Inappropriate Use of a Heel Lift
Christopher M. Rancont, DO
Heel lifts are commonly recommended for patients to
manage the pain and discomfort of leg length discrepancies.
However, used inappropriately, orthotics can create additional pain instead of alleviating it. In the case described, a
79-year-old male physician used a recommended heel lift for
a perceived leg length discrepancy after right hip arthroplasty. Six months postsurgery, chronic, intractable pain
developed in his hip and groin. He underwent a battery of
tests to locate the pain, but its source remained elusive.
Osteopathic evaluation and radiographic examination
revealed an absence of leg length discrepancy and the presence of chronic psoas syndrome. Osteopathic manipulative
treatment was prescribed and heel lift therapy discontinued,
and the patient reported complete remission from pain.
J Am Osteopath Assoc. 2007;107:415-418
Be sure the foundation is level and all will be well.
Andrew Taylor Still, MD, DO
eg length discrepancies contribute to myriad conditions
in patients, including low back pain,1,2 knee pain,3 and
abnormal gait.4 Such discrepancies, which can occur naturally5
or postsurgically,3,6 can often be resolved through the use
of heel lifts. However, used inappropriately, these corrective devices can worsenor even causeleg length discrepancies, leading to somatic dysfunction. Although leg
length discrepancies have not been reported previously in the
medical literature as contributing to psoas syndrome, the
current case illustrates the use of inappropriate heel lifts to be
a plausible, underlying factor in the occurrence of this chronic
condition.
Report of Case
A 79-year-old allopathic physician reported chronic pain in his
right hip and groin that had been plaguing him for more than
6 months. The patient first experienced a similar type of pain
Address correspondence to Christopher M. Rancont, DO, Pontiac Osteopathic
Hospital, 50 N Perry St, Pontiac, MI 48342-2217.
E-mail: crancont@yahoo.com
Submitted January 31, 2005; revision received June 14, 2005; accepted June
28, 2005.
Rancont Case Report
after total right hip arthroplasty 1 year earlier, in January 2003.
However, unlike his current pain, the patient could palliate the
postsurgical pain by extending his right leg while sitting.
Although the patient returned to work 11 days postsurgery, he
had to assume a reclined position while sitting for 3 to 4 weeks
after his arthroplasty in order to alleviate the pain.
The patient reported that in the first postsurgical month,
a physical therapist suggested that the arthroplasty lengthened the right leg. This leg length discrepancy was reported to
the orthopedic surgeon, who subsequently prescribed a 3/8in heel lift (the maximum sized in-shoe lift7) for the left leg, in
accordance with the therapists evaluation and recommendation. The patient had no subsequent pain for 6 months.
Seven months postsurgery, the patient experienced pain
following a game of golf. He did not recall any injury or precipitating event, but stated that the pain began gradually, out
of nowhere, in the right inguinal and groin area. Initially,
analgesics and maintaining a flexed position of the right leg
relieved the patients pain. However, the pain returned intermittently, often after the patient had been sitting for prolonged
periods. The pain prevented him from fully extending his
right leg when standing.
The patients orthopedic surgeon examined him and
ordered radiographs and a computed tomographic scan of
the lumbar region to assess the prosthesis and other potential
orthopedic sources for the pain. These tests showed some agerelated degeneration of the spine, possibly with stenosis.
Follow-up electromyography and magnetic resonance angiography tests were conducted to assess possible neuralgia due to
nerve impingement, disk injury, or other soft-tissue sources.
Although arthritic processes and degenerative changes were
present, no etiology for the pain could be elucidated diagnostically.
The patients episodes of pain and flexion deformity in the
right leg continued through the fall of 2003. At one point, the
patients pain was so severe that he visited the emergency
department. After initial evaluation, a flat plate radiograph
of the abdomen was taken, and a referral was made to a general surgeon for a suspected inguinal hernia, which was later
ruled out. The source of pain was not determined.
The patient, suspecting a possible renal or urologic etiology, visited a urologist. A complete urologic work-up was
ordered, which included urinalysis, blood work, intravenous
pyelogram, cystoscopy, and urine sedimentation tests. Again,
nothing unusual was found and no etiology was determined.
JAOA Vol 107 No 9 September 2007 415
CASE REPORT
During a pain episode in which he was unable to stand
unassisted, the patient described his medical history to the
author of the current report. Suspecting iliopsoas spasm as the
most likely source of dysfunction, I assisted the patient using
the counterstrain technique, fully extending the patients right
leg. Because the procedure alleviated the patients pain, he
agreed to undergo a more complete osteopathic evaluation.
Osteopathic Structural Examination
The patient appeared well-nourished, mesomorphic, and in
excellent health. Early in the day, he had a normal-to-anterior posture and walked with a slight shuffle, but with a symmetrical heel-toe gait. Hyperlordotic and kyphotic spinal features were not present. Later in the day, after sitting for a
prolonged period, the patient had trouble standing erect unassisted. In addition, his right leg became flexed and internally
rotated, and his gait became anteriorly deviated with limited
forward step on the left and an internally rotated step on the
right.
During the structural examination, the standing flexion
test8-11 was positive for iliosacral dysfunction on the right, and
the seated flexion test8-11 was positive for sacroiliac dysfunction on the left. Thomas test,8 performed with the patient in a
supine position, was positive for psoas shortening. The patient
was unable to extend his right leg beyond 160 degrees (flexion
deformity). Tissue tenderness and ropiness were palpable
along the right iliopsoas from the point of its insertion on the
femur, and proximally through the belly of the muscle, superior to the inguinal ligament. Right anterior superior iliac spine
(ASIS) was 2 cm inferior to the left ASIS, and the right posterior superior iliac spine (PSIS) was 1 cm superior to the left PSIS.
Superior sacral sulcus was deep on the left, shallow on the
right; inferior sacral sulcus was deep on the left and shallow
on the right. Motion (springing) of the left sacral base and
limited motion of the right sacral base were present. Lumbar
vertabra 5 (L5) was sidebent right and rotated left. The medial
malleoli were compared and found to be equidistant from
the pelvis. The greater trochanteric and iliac crest heights in the
standing position were compared with no appreciable discrepancy noted. After osteopathic evaluation was complete, the
initial differential diagnoses were chronic psoas syndrome,
right anterior innominate rotation, and forward sacral torsion
on a right oblique axis (ie, right-on-right torsion).
Osteopathic Manipulative Treatment
A sequence of indirect osteopathic techniques were initially
attempted to treat the psoas spasm during the acute exacerbation, but were unsuccessful. Counterstrain8-11 reduced the
pain during treatment but did not allow for increased extension of the leg. Facilitated positional release (FPR)8-11 and articulatory technique (also known as springing technique)8-12 allowed
the patient to achieve a slight increase in leg extension (ie,
416 JAOA Vol 107 No 9 September 2007
approximately 10 degrees), but this position remained uncomfortable for the patient. The direct osteopathic technique of
muscle energy8-11 proved painful for the patient and did not
appreciably increase the resting length of his psoas muscle.
Muscle energy to the anterior right innominate rotation with
direct manipulation of the pelvis to minimize tension on the
prosthetic hip resulted in reduction of pelvic dysfunction and
eventual restoration of pelvic symmetry.
Following this restoration, the patients pain from the
psoas spasm was relieved and he was then able to lie supine
with his right leg fully extended. At this point, osteopathic
manipulative treatment (OMT) used for treating the psoas
muscle was repeated (ie, counterstrain, FPR, articulatory techniques, and muscle energy), providing positive relief and an
increase in functional range of motion to greater than 180
degrees.
Radiographic Findings
A standing postural radiograph of the pelvic region and hips
was obtained (Figure 1) with the patient standing barefoot on
a level surface with his feet in line with his shoulders. The
radiologist reported a difference of 2 mm in femoral head
height and concluded that there was no appreciable leg length
discrepancy. The prosthetic hip and degenerative changes
of the spine were observed, but no considerable sacral base
tilting was noted.
The methods described by Kuchera and Kuchera9 for
evaluating leg length discrepancy and resultant sacral base
unleveling (Figure 2) were applied using a high resolution
inverted radiograph (Figure 3). The right femoral head was
3 mm higher than the left, but the greater trochanteric and
iliac crest heights were equal for each leg. Sacral base unleveling
was minimal at 4.4 mm toward the right. In general, the sacral
base unleveling that occurs as a result of leg length discrepancy
is toward the shorter leg,9,11 the opposite of the finding in the
current case. Using the Heilig formula,11 it was determined that
a 2.2 mm lift on the right leg would be appropriatethe opposite leg for which the lift was originally recommended.
The minimal differences in leg lengths (2-3 mm) as measured by the radiologist and by application of subsequent
measurement techniques are not of the magnitude that would
require correction with the use of a heel lift.7,11,13,14 In addition,
as a result of the inability to distinguish the prosthetic femoral
head from the acetabular prosthesis, it was not reliable to compare the two femoral head heights when evaluating leg length
discrepancies. Therefore, more confidence in this case should
be given to comparing sacral base unleveling in combination
with greater trochanteric and iliac crest heights, all of which
showed no appreciable difference.
The structural examination findings, correlating history
and flexion deformity, and resolution of symptoms after OMT
confirm that the principle dysfunction causing the patients pain
Rancont Case Report
CASE REPORT
and deformity was a psoas spasm. Physical examination and
radiographic evidence do not support the presence of a significant leg length discrepancy and therefore do not support
the use of a heel lift. The patients minimal sacral base
unleveling was toward the right, which would be consistent
with compensation for a short right leg9,11 or compensation for
the inappropriate use of a heel lift on the left.
After two sessions of OMT as previously described, the
patient experienced relief from symptoms and a decrease in
their recurrence. He was then instructed on how to perform
self-counterstrain and contract opposing muscles (hamstrings)
to block pain in returning the psoas to its resting length while
standing up. The patient followed up with a physical therapist
who was osteopathically trained and who continued to treat
his pelvis, sacrum, and psoas during the time the patient transitioned from using the heel lift. The physical therapist also gave
him a series of psoas-stretching techniques to perform daily at
home. The patient reported a gradual decrease in the severity
and frequency of the pain over several weeks, with complete
remission of symptoms within 2 months.
Figure 1. A standing postural radiograph of the pelvis and hips in
a 79-year-old man with a total right hip arthroplasty. The findings from
this radiographic image did not reveal an appreciable leg length discrepancy.
Discussion
Psoas syndrome can be defined as a muscular imbalance,
strain, spasm, tendonitis, or flexion contracture of the iliopsoas
muscle (consisting of the iliac and psoas major). This syndrome may result in a number of symptoms,8-12 including:
flexion deformity of the leg on the affected side
increased pain when standing or walking
lordosis when supine
nonneutral somatic dysfunction of the lumbar vertebra 1
or 2 (L1 or L2)
pain in the lower back, pain radiating anteriorly toward the
groin, or both
pelvic shift to the opposite side
point tenderness medial to the ASIS or femoral triangle
psoatic gait
sacral dysfunction on an oblique axis
spasm of the contralateral piriformis muscle
The most common causes of psoas syndrome are direct
muscular dysfunctions arising from iliopsoas spasm or strain.
Spasm of the iliopsoas often occurs after a position with a
shortened psoas (eg, sitting, kneeling, crouching) has been
maintained for an extended period of time.11 Strain of the
iliopsoas can result from forceful contraction of these muscles when the thigh is in a fixed or extended position. For
example, this forceful contraction may occur while running
uphill, performing straight-legged sit-ups, stumbling with one
leg extended, or kicking a ball.15 In iliopsoas strains, the pain
begins as a sharp stab in the groin and increases with active
resisted hip flexion or passive external rotation.15 In adolescents,
Rancont Case Report
8
9
R
1
RL
Figure 2. Image for evaluating leg length discrepancy and resultant sacral base unleveling. At the reference line (RL), the differences between lines 1 and 2 indicate femoral head unleveling; lines
5 and 6, iliac crest height inequality; and lines 8 and 9, sacral base
unleveling. Reprinted with permission from the publisher.9
the injury may produce avulsion of the lesser trochanter; in
adults, the result may be a complete or partial tear at the
muscle-tendon junction.15
Other causes of psoas syndrome include irritation to the
psoas muscle directly or through viscerosomatic reflexes.
JAOA Vol 107 No 9 September 2007 417
CASE REPORT
combined with an osteopathic structural examination and
contemplating the whole person, the practitioner can facilitate proper diagnosis and treatment.
Acknowledgments
I thank Michael L. Kuchera, DO, for his assistance as a consultant
and editor in the final preparation of this manuscript. In addition, I
extend sincere gratitude to Richard J. LaBaere II, DO, MPH, for
his encouragement and support in preparing this case report and
for being a true osteopathic mentor.
References
1. Defrin R, Ben Benyamin S, Aldubi RD, Pick CG. Conservative correction of
leg-length discrepancies of 10 mm or less for the relief of chronic low back
pain. Arch Phys Med Rehabil. 2005;86:2075-2080.
2. ten Brinke A, van der Aa HE, van der Palen J, Oosterveld F. Is leg length
discrepancy associated with the side of radiating pain in patients with a
lumbar herniated disc? Spine. 1999;24:684-686.
Figure 3. Representation of measurements for leg length discrepancy as applied to an inverted radiographic image of the pelvis and
hips of a 79-year-old man.
3. Reina R, Vilella FE, Ramrez N, Valenzuela R, Nieves G, Foy CA. Knee pain
and leg-length discrepancy after retrograde femoral nailing. Am J Orthop.
2007;36:325-328.
4. Lai KA, Lin CJ, Su FC. Gait analysis of adult patients with complete congenital
dislocation of the hip. J Formos Med Assoc. 1997;96:740-744.
Organic causes of psoas syndrome, some of which may be
serious or life-threatening, include abdominal aortic aneurysm,
intra-abdominal abscess, appendicitis, diverticulitis, inguinal
hernia, prostate or sigmoid colon cancer, prostatitis, salpingitis, ureteral calculi, and Crohn disease.8-11,16
In the case described, the right sacral base unleveling and
right anterior innominate rotation most likely resulted from
compensating for the use of an inappropriate heel lift. The
innominate rotation lengthened the resting length of the psoas
muscle, placing it under constant strain. The onset of the psoas
dysfunction probably began during a golf game, when the
patient forcefully contracted the iliopsoas with the thigh in a
fixed or extended position. This strain in the context of a chronically lengthened psoas initiated the chronic psoas syndrome.
As illustrated in the current case, the long-term consequences
of compensating for an inappropriate orthotic lift or of actual
leg length discrepancy can become deleterious and even disabling.
Conclusion
The diagnosis of psoas syndrome may be elusive because the
syndrome can masquerade as many different medical conditions that could distract a practitioner from making an accurate diagnosis. In addition, perceived leg length discrepancies should be carefully interrogated and managed properly.
The long-term consequences of compensating for a leg length
discrepancy or use of an improper lifting device can have
serious, detrimental effects. Further research into leg length discrepancy as a cause of chronic psoas syndrome is recommended. Through conscientious appreciation of symptoms
418 JAOA Vol 107 No 9 September 2007
5. Kotoske DE. Reported prevalence rates of somatic dysfunction raise an ...
heel [letter]? J Am Osteopath Assoc. 2007;107:281. Available at: http://www.
jaoa.org/cgi/content/full/107/7/281. Accessed September 19, 2007.
6. Hossain M, Sinha AK. A technique to avoid leg-length discrepancy in total
hip arthroplasty. Ann R Coll Surg Engl. 2007;89:314-315.
7. Braddom RL. Physical Medicine and Rehabilitation. 2nd ed. Philadelphia,
Pa; WB Saunders Co; 2000.
8. DiGiovanna EL, Schiowitz S, Dowling DJ, eds. An Osteopathic Approach to
Diagnosis and Treatment. 2nd ed. Philadelphia, Pa: Lippincott Williams &
Wilkins; 1997.
9. Kuchera WA, Kuchera ML. Osteopathic Principles in Practice. 2nd rev ed.
Columbus, Ohio: Greyden Press; 1994.
10. Savarese RG, Capobianco JD, Cox JJ. OMT Review. 3rd ed. 2003.
11. Ward RC, ed. Foundations for Osteopathic Medicine. 2nd ed. Philadelphia,
Pa: Lippincott Williams & Wilkins; 2003.
12. Still AT. The Philosophy and Mechanical Principles of Osteopathy. Kansas
City, Mo: Hudson-Kimberly Pub Co; 1902.
13. Frontera WR, Silver JK. Essentials of Physical Medicine and Rehabilitation:
Review and Self-Assessment. Philadelphia, Pa: Hanley & Belfus, Inc; 2002.
14. Grabois M, Garrison SJ, Hart KA, Lehnkuhl LD, eds. Physical Medicine and
Rehabilitation: The Complete Approach. Malden, Mass: Blackwell Science, Inc;
2000.
15. DeLee JC, Drez D, Miller MD. DeLee and Drezs Orthopaedic Sports
Medicine: Principles and Practice. 2nd ed. Philadelphia, Pa: WB Saunders Co;
2003.
16. Delaney CP, Fazio VW. Crohns disease of the small bowel. Surg Clin
North Am. 2001;81:137-158.
Rancont Case Report
También podría gustarte
- Limitless Lover GuidebookDocumento64 páginasLimitless Lover GuidebookTito AlhoAún no hay calificaciones
- Rehabilitation of Muscle Dysfunction in HemophiliaDocumento14 páginasRehabilitation of Muscle Dysfunction in HemophiliadavidcorzoAún no hay calificaciones
- Hip Flexors - The Iliopsoas - Tightness or WeaknessDocumento4 páginasHip Flexors - The Iliopsoas - Tightness or Weaknessatpicker100% (1)
- Síndrome Cruzado Superior e InferiorDocumento2 páginasSíndrome Cruzado Superior e InferiorFernandoAún no hay calificaciones
- Trigger Point MapsDocumento77 páginasTrigger Point Mapsazhar_iqbal2000100% (11)
- Physical Therapy Protocols For The Conditions of Hip RegionDocumento50 páginasPhysical Therapy Protocols For The Conditions of Hip RegionAnita GajariAún no hay calificaciones
- Fibromyalgia: July 5, 2012Documento4 páginasFibromyalgia: July 5, 2012Von HippoAún no hay calificaciones
- The Shoulder PainDocumento14 páginasThe Shoulder PainLev KalikaAún no hay calificaciones
- Fascia Forgotten StructureDocumento12 páginasFascia Forgotten StructureFraan GutierrezAún no hay calificaciones
- Hip StrengtheningDocumento1 páginaHip Strengtheningapi-282526794Aún no hay calificaciones
- Hip Adductor RehabilitationDocumento4 páginasHip Adductor RehabilitationOscar NgAún no hay calificaciones
- The Inverted Orthotic Technique: A Process of Foot Stabilization for Pronated FeetDe EverandThe Inverted Orthotic Technique: A Process of Foot Stabilization for Pronated FeetAún no hay calificaciones
- Application of Fascial Manipulation Technique in Chronic Shoulder PainDocumento9 páginasApplication of Fascial Manipulation Technique in Chronic Shoulder PainIsabelGuijarroMartinez100% (1)
- Achilles TendonDocumento30 páginasAchilles TendonMeldianaAún no hay calificaciones
- Posture PDFDocumento30 páginasPosture PDFSairelle Sordilla Obang100% (1)
- Adductor-Related Groin Pain Rehab & Return To Sport Progressions With Andrew Wallis HandoutDocumento46 páginasAdductor-Related Groin Pain Rehab & Return To Sport Progressions With Andrew Wallis Handoutgemichan26100% (1)
- The Hip: Therapeutic Exercise 2 Lino Linford BangayanDocumento91 páginasThe Hip: Therapeutic Exercise 2 Lino Linford BangayanLino Linford Yu Bangayan100% (1)
- Red Flag: MSK Services Pathway - Hand PathologyDocumento10 páginasRed Flag: MSK Services Pathway - Hand PathologyMuhammed ElgasimAún no hay calificaciones
- Anatomy Lower LimbDocumento4 páginasAnatomy Lower Limbch yaqoobAún no hay calificaciones
- Self Help MyofascialTriggerPointsDocumento18 páginasSelf Help MyofascialTriggerPointssalmazz0% (1)
- Assessing Lateral Stability of The Hip and PelvisDocumento7 páginasAssessing Lateral Stability of The Hip and PelvisCristian Alejandro Flores PinuerAún no hay calificaciones
- Practical Applications of Manual Lymphatic TherapyDocumento103 páginasPractical Applications of Manual Lymphatic TherapyTito Alho100% (2)
- Aaron Driver Doctor of PhysiotherapyDocumento12 páginasAaron Driver Doctor of Physiotherapyaaronjdriver2248Aún no hay calificaciones
- Compton - PsoasDocumento25 páginasCompton - PsoasiruizmolinaAún no hay calificaciones
- Uhp Handout PDFDocumento3 páginasUhp Handout PDFMaiSiaoSiao Joe67% (3)
- Self Myofascial ReleaseDocumento2 páginasSelf Myofascial Releasesonopuntura100% (2)
- Keywords Joint PainDocumento10 páginasKeywords Joint PainMayank JhaAún no hay calificaciones
- Kinesiology Taping Theory and ApplicationDocumento8 páginasKinesiology Taping Theory and Applicationtaxel00% (1)
- Hip and PelvisDocumento59 páginasHip and PelvisIbNu OmErAún no hay calificaciones
- ISMST GuidelinesDocumento112 páginasISMST GuidelinesDhrubo TaraAún no hay calificaciones
- 8 Non Structural Misalignments of Body Posture in The Sagittal PlaneDocumento14 páginas8 Non Structural Misalignments of Body Posture in The Sagittal PlaneHusna LathiifaAún no hay calificaciones
- Copper Fungicides OrganicDocumento2 páginasCopper Fungicides OrganicJuanAún no hay calificaciones
- Angela Hand and Upper ExtremityDocumento59 páginasAngela Hand and Upper ExtremityJenny RajanAún no hay calificaciones
- Anatomy Biomechanics of The Hip PDFDocumento8 páginasAnatomy Biomechanics of The Hip PDFangelluis1980Aún no hay calificaciones
- Hip Muscle Imbalances and Their Effects: Anterior Pelvic Tilt PostureDocumento4 páginasHip Muscle Imbalances and Their Effects: Anterior Pelvic Tilt PostureRizki DianraAún no hay calificaciones
- Treatment of Tendinopathy What Works, What Does Not, and What Is On The Horizon PDFDocumento16 páginasTreatment of Tendinopathy What Works, What Does Not, and What Is On The Horizon PDFFranciscoJavierRoblesAún no hay calificaciones
- Prevelance of Piriformis Syndrome in Chronic Low Back Pain Patients. A Clinical Diagnosis With Modified FAIR Test PainPractice20121 PDFDocumento9 páginasPrevelance of Piriformis Syndrome in Chronic Low Back Pain Patients. A Clinical Diagnosis With Modified FAIR Test PainPractice20121 PDFAuliadi AnsharAún no hay calificaciones
- DIAD PleoScope PDFDocumento9 páginasDIAD PleoScope PDFDanielPunctAún no hay calificaciones
- Groin Pain GuideDocumento32 páginasGroin Pain GuideAugusto ManoelAún no hay calificaciones
- Understanding Arthritis: by Kester MarshallDocumento2 páginasUnderstanding Arthritis: by Kester MarshallSN WijesinheAún no hay calificaciones
- Motor Imagery and MirrorTherapyDocumento5 páginasMotor Imagery and MirrorTherapyLorenaMariaAún no hay calificaciones
- MRI of Knee - Part2Documento62 páginasMRI of Knee - Part2Reza AAún no hay calificaciones
- Chemical Hip Denervation For Inoperable Hip FractureDocumento6 páginasChemical Hip Denervation For Inoperable Hip Fracturemanuel torresAún no hay calificaciones
- Hip and Groin Pain Radiological AssessmentDocumento13 páginasHip and Groin Pain Radiological AssessmentOscar NgAún no hay calificaciones
- Kenneth J Koval, Joseph D Zuckerman PDFDocumento340 páginasKenneth J Koval, Joseph D Zuckerman PDFAnonymous hGBXIKA1Aún no hay calificaciones
- Dental Equilibration and OsteopathyDocumento9 páginasDental Equilibration and OsteopathyshivnairAún no hay calificaciones
- Musculoskeletal Disease Associated With Diabetes MellitusDocumento290 páginasMusculoskeletal Disease Associated With Diabetes Mellituscharanmann9165Aún no hay calificaciones
- A Simple Guide to Extensor Tendonitis, Diagnosis, Treatment and Related ConditionsDe EverandA Simple Guide to Extensor Tendonitis, Diagnosis, Treatment and Related ConditionsAún no hay calificaciones
- Iliopsoas Syndrome - The Hidden Root of PainDocumento13 páginasIliopsoas Syndrome - The Hidden Root of Painpeter1234u0% (1)
- Gluteal Tendinopathy A Review of Mechanisms, Assessmentand ManagementDocumento13 páginasGluteal Tendinopathy A Review of Mechanisms, Assessmentand ManagementDaniela Villablanca100% (1)
- Differential Release of Mast Cell Mediators and The Pathogenesis of InflammationDocumento14 páginasDifferential Release of Mast Cell Mediators and The Pathogenesis of InflammationklaumrdAún no hay calificaciones
- Extraarticular Snapping Hip: American Journal of Roentgenology: Vol. 176, No. 1 (AJR) PDFDocumento13 páginasExtraarticular Snapping Hip: American Journal of Roentgenology: Vol. 176, No. 1 (AJR) PDFKeneyziaAún no hay calificaciones
- Hip PathologiesDocumento35 páginasHip PathologiesJoe KhdeirAún no hay calificaciones
- Transversus Abdominis Plane (Tap) BlockDocumento6 páginasTransversus Abdominis Plane (Tap) BlockSuresh KumarAún no hay calificaciones
- Hip Condition PhysiopediaDocumento96 páginasHip Condition PhysiopediaPrethy PhilipAún no hay calificaciones
- Treatment of Osteitis Pubis Via The Pelvic Muscles PDFDocumento4 páginasTreatment of Osteitis Pubis Via The Pelvic Muscles PDFHapplo82Aún no hay calificaciones
- About PRPDocumento5 páginasAbout PRPAllanSalardaAdemAún no hay calificaciones
- Mulligan Vs ART PDFDocumento4 páginasMulligan Vs ART PDFwernsickleAún no hay calificaciones
- Top 10 Effects of The Forward Head Posture Epidemic - Spider Tech Solution HandoutDocumento1 páginaTop 10 Effects of The Forward Head Posture Epidemic - Spider Tech Solution HandoutthevitalitydepotAún no hay calificaciones
- AAPMR - What Makes The Practice of Physiatry MultidisciplinaryDocumento3 páginasAAPMR - What Makes The Practice of Physiatry MultidisciplinaryJared CoganAún no hay calificaciones
- Lumbar Facet Pain ArticleDocumento24 páginasLumbar Facet Pain ArticlejmccoyAún no hay calificaciones
- Marfan Syndrome With Atypical PresentationDocumento4 páginasMarfan Syndrome With Atypical PresentationaiAún no hay calificaciones
- 1 Theory and Application Therapeutic Taping2012Documento30 páginas1 Theory and Application Therapeutic Taping2012Francisco Vicent PachecoAún no hay calificaciones
- Neurogenic BowlDocumento21 páginasNeurogenic BowlFaridatul IsniyahAún no hay calificaciones
- Gait & Posture Volume Issue 2018 - Gluteal Tendinopathy and Hip Osteoarthritis - Different PatholDocumento23 páginasGait & Posture Volume Issue 2018 - Gluteal Tendinopathy and Hip Osteoarthritis - Different PatholGiancarlo Gardella MartínezAún no hay calificaciones
- Foot DropDocumento30 páginasFoot Dropdr_s_ganesh100% (1)
- FasciaeDocumento54 páginasFasciaeSantiago Orihuela0% (1)
- Pericapsular Nerve Group (PENG) Block For Hip FractureDocumento5 páginasPericapsular Nerve Group (PENG) Block For Hip FractureJhonathan Romero100% (1)
- Handout Lat Elbow Pain PDFDocumento47 páginasHandout Lat Elbow Pain PDFgemichan26Aún no hay calificaciones
- Course: Physioteraphy - Mentor: Dijana Njerš - Class: English II - Student: Ella DaradkehDocumento9 páginasCourse: Physioteraphy - Mentor: Dijana Njerš - Class: English II - Student: Ella DaradkehEllaAún no hay calificaciones
- Shoulder Rehabilitation: - Anatomy Review - Muscle Testing Review - Common Problems - TreatmentDocumento29 páginasShoulder Rehabilitation: - Anatomy Review - Muscle Testing Review - Common Problems - TreatmentStefan VladAún no hay calificaciones
- Evaluation of The Patient With Hip PainDocumento12 páginasEvaluation of The Patient With Hip PainannisaAún no hay calificaciones
- 2016 Influence of Scapular Position On The CORE Musculature Activation in The Prone Plank ExerciseDocumento23 páginas2016 Influence of Scapular Position On The CORE Musculature Activation in The Prone Plank ExerciseFrancisco Antonó Castro WeithAún no hay calificaciones
- Stenosing Tenosynovitis, (Trigger Finger) A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsDe EverandStenosing Tenosynovitis, (Trigger Finger) A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsAún no hay calificaciones
- HHS Public Access: Exercise Rehabilitation For Peripheral Artery Disease: A ReviewDocumento17 páginasHHS Public Access: Exercise Rehabilitation For Peripheral Artery Disease: A ReviewTito AlhoAún no hay calificaciones
- HHS Public Access: Exercise Therapy For Older Heart Failure PatientsDocumento17 páginasHHS Public Access: Exercise Therapy For Older Heart Failure PatientsTito AlhoAún no hay calificaciones
- Bjsports 2019 100886Documento12 páginasBjsports 2019 100886Tito AlhoAún no hay calificaciones
- Review Article: The Effectiveness of Physical Exercise On Bone Density in Osteoporotic PatientsDocumento10 páginasReview Article: The Effectiveness of Physical Exercise On Bone Density in Osteoporotic PatientsTito AlhoAún no hay calificaciones
- Exercise Therapy For Muscle and Lower Motor Neuron Diseases: Aisha Munawar Sheikh, John VissingDocumento18 páginasExercise Therapy For Muscle and Lower Motor Neuron Diseases: Aisha Munawar Sheikh, John VissingTito AlhoAún no hay calificaciones
- Exercise in Neuromuscular Disorders: A Promising InterventionDocumento8 páginasExercise in Neuromuscular Disorders: A Promising InterventionTito AlhoAún no hay calificaciones
- MainDocumento16 páginasMainTito AlhoAún no hay calificaciones
- Physical Exercise and Morbid Obesity: A Systematic ReviewDocumento7 páginasPhysical Exercise and Morbid Obesity: A Systematic ReviewTito AlhoAún no hay calificaciones
- 2015 Article 155Documento16 páginas2015 Article 155Tito AlhoAún no hay calificaciones
- Nihms 1001835Documento12 páginasNihms 1001835Tito AlhoAún no hay calificaciones
- 262 2017 Article 1985Documento5 páginas262 2017 Article 1985Tito AlhoAún no hay calificaciones
- Author's Accepted Manuscript: Journal of Affective DisordersDocumento47 páginasAuthor's Accepted Manuscript: Journal of Affective DisordersTito AlhoAún no hay calificaciones
- Indian Journal of Psychiatry: The Limbic SystemDocumento34 páginasIndian Journal of Psychiatry: The Limbic SystemTito AlhoAún no hay calificaciones
- Guruji Pranayama SadhanaDocumento9 páginasGuruji Pranayama SadhanaTito AlhoAún no hay calificaciones
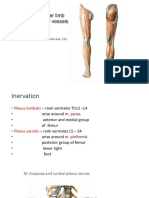
- LOWER LIMB Muscles, Nerves Vessels PDFDocumento92 páginasLOWER LIMB Muscles, Nerves Vessels PDFGeetAún no hay calificaciones
- SMB Thigh Muscles WorksheetDocumento3 páginasSMB Thigh Muscles WorksheetShehryar BaigAún no hay calificaciones
- Anatomy 1Documento17 páginasAnatomy 1Uljana NasonovaAún no hay calificaciones
- Groin Pain in Football Players: A Systematic Diagnostic ApproachDocumento5 páginasGroin Pain in Football Players: A Systematic Diagnostic ApproachCherbiti Mohammed Amine100% (1)
- Comminuted Quadrilateral Plate Fracture Fixation Through The Iliofemoral ApproachDocumento8 páginasComminuted Quadrilateral Plate Fracture Fixation Through The Iliofemoral ApproachdrarunlalAún no hay calificaciones
- Hip Joint AnatomyDocumento14 páginasHip Joint AnatomyIlham Ristananda0% (1)
- Frcem Lower LimbsDocumento69 páginasFrcem Lower LimbsskAún no hay calificaciones
- Lower Limbs PracticalDocumento45 páginasLower Limbs PracticalOleashedAún no hay calificaciones
- Topography of Lower LimbDocumento10 páginasTopography of Lower LimbMarina CretuAún no hay calificaciones
- 2011 - Kim, Kim, Beriwal - Contouring Inguinal and Femoral Nodes How Much Margin Is Needed Around The VesselsDocumento1 página2011 - Kim, Kim, Beriwal - Contouring Inguinal and Femoral Nodes How Much Margin Is Needed Around The VesselsPoljarLijanAún no hay calificaciones
- Tabel KinesiologiDocumento4 páginasTabel KinesiologiMohammad Jofa Rachman PAún no hay calificaciones
- Iliopsoas The Hidden Muscle - Anatomy, Diagnosis, and Treatment (2020)Documento9 páginasIliopsoas The Hidden Muscle - Anatomy, Diagnosis, and Treatment (2020)yuliAún no hay calificaciones
- Kine 3p80 Hip Injury Assignment 1Documento4 páginasKine 3p80 Hip Injury Assignment 1api-437399185Aún no hay calificaciones
- Muscular System Laboratory Guide: Dissection of The Muscles: See Pages 229-230 in The Lab ManualDocumento16 páginasMuscular System Laboratory Guide: Dissection of The Muscles: See Pages 229-230 in The Lab ManualNathaniel CamangonAún no hay calificaciones
- (Gross A) Lower Extremities, Thorax, and Lungs Practicals Reviewer (Gabasan) (Lab)Documento75 páginas(Gross A) Lower Extremities, Thorax, and Lungs Practicals Reviewer (Gabasan) (Lab)Kristine Nicole UbanaAún no hay calificaciones
- Atlas of Nerve Conduction Studies and Electromyography (2 Ed.)Documento21 páginasAtlas of Nerve Conduction Studies and Electromyography (2 Ed.)rodrigocorcino899959Aún no hay calificaciones
- Anatomy TopoDocumento62 páginasAnatomy TopoDoina GoreanuAún no hay calificaciones
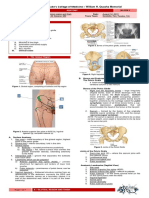
- St. Luke's College of Medicine - William H. Quasha Memorial: AnatomyDocumento7 páginasSt. Luke's College of Medicine - William H. Quasha Memorial: AnatomyMavic VillanuevaAún no hay calificaciones