Documentos de Académico
Documentos de Profesional
Documentos de Cultura
tmp847B TMP
Cargado por
FrontiersDescripción original:
Título original
Derechos de autor
Formatos disponibles
Compartir este documento
Compartir o incrustar documentos
¿Le pareció útil este documento?
¿Este contenido es inapropiado?
Denunciar este documentoCopyright:
Formatos disponibles
tmp847B TMP
Cargado por
FrontiersCopyright:
Formatos disponibles
[Downloaded free from http://www.najms.org on Thursday, February 25, 2016, IP: 77.42.170.
220]
Review Article
Stress, Burnout and Coping Strategies
in Preclinical Medical Students
Jawad Fares1,2, Hayat Al Tabosh1, Zein Saadeddin1, Christopher El Mouhayyar1, Hussam Aridi1
1
Faculty of Medicine, American University of Beirut, 2Neuroscience Research Center, Faculty of Medical Sciences,
Lebanese University, Beirut, Lebanon
Abstract
It is acknowledged that physicians do not seek the same expert aid for themselves as they would offer their patients. In their preclinical years, medical
students appear to espouse comparable behavior. To many, medicine is described as a never-ending path that places the student under heavy stress
and burnout from the beginning, leaving him/her vulnerable and with insufficient coping methods. Hence, the objective of this study is to 1) explore
the prevalence of stress and burnout among preclinical medical students, and 2) propose solutions to decrease stress and burnout and improve
medical education in the preclinical years. A detailed scholarly research strategy using Google Scholar, Scopus, Embase, MEDLINE and PubMed
was implemented to highlight key themes that are relevant to preclinical medical students stress and burnout. Stress varied among different samples
of medical students and ranged between 20.9% and 90%. Conversely, burnout ranged between 27% and 75%. Methods that help in reducing the
incidence of stress and burnout by promoting strategies that focus on personal engagement, extracurricular activities, positive reinterpretation and
expression of emotion, student-led mentorship programs, evaluation systems, career counseling and life coaching should be adopted.
Keywords: Burnout, medical education, medical school, medical student, preclinical years, stress
Address for correspondence: Mr. Jawad Fares, Faculty of Medicine, American University of Beirut, Beirut, Lebanon. E-mail: jyf04@mail.aub.edu
Introduction
Medicine is a never-ending path and a highly
demanding career that appears to leave many
medical students at the risk of stress and burnout. A
gap in the literature exists regarding the assessment
of stress and burnout among preclinical medical
students. Although medical schools strive to support
students during the training process and aim to
graduate knowledgeable, skillful and professional
doctors, studies suggest that medical students
experience high rates of personal distress,[1-15] with
latent unfavorable consequences on academic
performance, [16-18] aptitude, [19] professionalism [20-27]
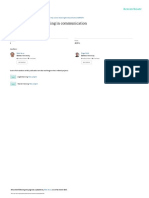
and health[12,28-32] [Figure 1]. There is proof that stress
Access this article online
Quick Response Code:
Website:
www.najms.org
and anxiety during medical school foresee future
predicaments in physicians, [13] which, in addition
to individual torment, may unconstructively affect
patient care.[13] Therefore, the objective of this article
is to:
1. Present the epidemiology and manifestations of stress
and burnout among preclinical medical students, and
2. Propose solutions to decrease stress and burnout and
improve medical education in the preclinical years.
To explore the central themes and epidemiology
of preclinical medical students stress and burnout
reported in the literature, sources were identified by
searching Google Scholar, Scopus, Embase, MEDLINE
This is an open access article distributed under the terms of the
Creative Commons Attribution-NonCommercial-ShareAlike 3.0
License, which allows others to remix, tweak, and build upon the
work non-commercially, as long as the author is credited and the
new creations are licensed under the identical terms.
For reprints contact: reprints@medknow.com
DOI:
10.4103/1947-2714.177299
How to cite this article: Fares J, Al Tabosh H, Saadeddin Z,
El Mouhayyar C, Aridi H. Stress, burnout and coping strategies in
preclinical medical students. North Am J Med Sci 2016;8:75-81.
2016 North American Journal of Medical Sciences | Published by Wolters Kluwer - Medknow
75
[Downloaded free from http://www.najms.org on Thursday, February 25, 2016, IP: 77.42.170.220]
Fares, et al.: Stress, burnout and coping strategies in medical students
Figure 1: A model illustrating the relations between contributing factors and health outcomes of burnout among medical students
and PubMed for English language articles published
between 1953 and 2015. We used the following search
terms: Medical student AND stress, burnout, distress,
ethics, medical education, professionalism, emotional
exhaustion, cynicism or academic performance.
Additional studies were identified from the reference
lists of these articles. Articles were reviewed critically
by authors and included as appropriate to provide
readers with a current overview of the research on
medical student stress and burnout in the preclinical
years.
Stress
Stress is a psychological and physical reaction to the
ever-increasing demands of life. To a degree, it is a
normal part of medical education and can be a motivator
for certain individuals; however, not all students find
stress constructive.[13] For many students, stress arouses
feelings of fear, incompetence, uselessness, anger and
guilt, and can be associated with both psychological
and physical morbidities.[33-35] Among medical students,
stress has been reported to be due to academic
demands, exams, an inability to cope, helplessness,
increased psychological pressure, mental tension,
excessive workload,[36] curricular factors, personal life
events and the learning environment.[37-39] These factors
can result in decreased life satisfaction,[40] which in
turn leads to unprofessional conduct, increased risk
of suicidal ideation and serious thoughts of dropping
out.[41,42] The literature reports varying rates of stress
among samples of preclinical medical students. Fares
et al.[43] rated stress among preclinical students from
Lebanon at 62%. Sidik et al.,[44] Zaid et al.[45] and Fuad
et al.[46] reported stress prevalence that ranges between
41.9% and 46.9% in Malaysian medical students.
Moreover, Mosley et al.[8] and Ko et al.[47] reported a
stress prevalence of 57% among preclinical medical
students in the US and Singapore, respectively. In the
UK, Guthrie revealed a 35.4% stress prevalence among
preclinical medical students. [48] Similarly in India,
Konjengbam et al.[49] reported a 37% stress prevalence
among undergraduate medical students. Other studies
report lower medical student stress ranging between
20.9% and 29.6%.[50-52]
76
Burnout
Burnout is another measure of physical exhaustion
and mental distress, which is catalyzed primarily
by occupational and professional demands. This
syndrome of emotional exhaustion, depersonalization
and low personal accomplishment culminates in
decreased effectiveness at work.[42] A broad range of
professions that heavily involve human interactions,
such as physicians,[53,54] nurses[55,56] and educators,[57]
experience burnout. Burnout is associated with
decreased job performance [58] and reduced job
commitment [56] and predicts stress-related health
problems[59] and low career satisfaction.[60-62] It is well
established in the literature that workload, lack of
support and loss of control at times contribute to a sense
of emotional exhaustion in those who endure medical
education.[42,43] In addition, feelings of reduced personal
accomplishment, overwork and emotional commitment
to medicine can lead to depersonalization.[8] Hence, the
development of burnout begins during the preclinical
years, in which the setting is that of overwhelming
work and facts to be learned with limited resources
of time and memory, and continues throughout the
clinical years.[33,43,52]
Burnout and stress are symptomatically similar, with
burnout attributed specifically to occupational or
academic stressors.[63] McManus et al.[64] proposed that
there is a cyclic relation between stress and emotional
exhaustion, which suggests that heightened levels of
stress and poor coping strategies may be key contributors
in the development of burnout.
A study in Lebanon that measures burnout risk in
preclinical medical students showed that 75% suffered
from burnout.[43] Another study from Spain revealed
that 14.8% experienced burnout.[65] The varying levels
of stress and burnout in different countries can be
attributed to the life stressors that vary from one region
to another. In addition to academic and medical school
stressors, socioeconomic, political, conflict-related and
health-related factors contribute to the increased levels
of stress and burnout. In Lebanon, a Middle Eastern
country amid conflicts and regional instability,[66-70] stress
North American Journal of Medical Sciences | Feb 2016 | Volume 8 | Issue 2 |
[Downloaded free from http://www.najms.org on Thursday, February 25, 2016, IP: 77.42.170.220]
Fares, et al.: Stress, burnout and coping strategies in medical students
Table 1: Stress and burnout levels in studies involving preclinical medical students between 1988 and 2015
Authors
Year
Number of medical
students
Number of preclinical
medical students
Stress
(%)
Burnout
(%)
Country
Fares et al.[43]
Konjengbam et al.[49]
Fuad et al.[46]
Galan et al.[65]
Dyrbye et al.[80]
Yusoff et al.[51]
Dyrbye et al.[41]
Santen et al.[39]
Drybye et al.[42]
Dahlin et al.[81]
Sreeramareddy et al.[52]
Zaid et al.[45]
Dyrbye et al.[79]
Dyrbye et al.[78]
Aktekin et al.[3]
Moffat et al.[2]
Shaikh et al.[36]
Sidik et al.[44]
Ko et al.[47]
Guthrie et al.[48]
Guthrie et al.[1]
Mosley et al.[8]
Vitaliano et al.[10]
2015
2015
2015
2011
2011
2010
2010
2010
2008
2007
2007
2007
2007
2006
2005
2004
2004
2003
1999
1997
1995
1994
1988
165
299
762
270
1846
761
2682
194
2248
98
407
253
1694
1098
119
275
264
166
135
254
172
162
312
165
40
450
176
476
1373
194
1201
98
239
149
892
119
275
211
105
135
254
172
312
62
37
46.9
58
29.6
20.9
46.2
49
47.9
52.4
>90
41.9
57
35.4
36
57
25
75
Lebanon
India
Malaysia
Spain
US
Malaysia
US
US
US
Sweden
Nepal
Malaysia
US
US
Turkey
UK
Pakistan
Malaysia
Singapore
UK
UK
US
US
37.5
52.8
33.3
49.6
27
47
45
and burnout levels are expected to be higher than in
Spain, for example, where similar stressors are relatively
non-existent.
Numerous studies note rates of burnout between
25% and 60% in a wide spectrum of health-related
specialties.[71-76] Nine US-based studies on burnout in
medical students reported a prevalence ranging between
45% and 71%.[4,38,40,42,77-81] Table 1 shows the prevalence
of stress and burnout in studies that include preclinical
medical students from 1988 until 2015.
Coping Mechanisms and Proposed
Solutions
Students use various coping mechanisms to process stress
[Figure 2]. Strategies that involve engagement such as
problem solving, positive reinterpretation and expression
of emotion, facilitate student adaptation, [2,8,33,43,82]
which reduces anxiety and depression and their
effects on mental wellbeing[59] and physical health.[82]
Extracurricular activities involving music and physical
exercise have been associated with decreased stress
and burnout levels in preclinical medical students.[43]
Unfortunately, few students seek help,[83] and distress
often continues into residency and beyond[13] where
it may have adverse effects on the quality of patient
care delivered.[84,85] Therefore, it is critical for medical
Figure 2: Methods and strategies that help in reducing stress and
burnout in preclinical medical students
educators to understand the prevalence and severity
of student stress and burnout, the potential adverse
personal and professional consequences and the
institutional factors that can affect student health from
an early time.
North American Journal of Medical Sciences | Feb 2016 | Volume 8 | Issue 2 |
77
[Downloaded free from http://www.najms.org on Thursday, February 25, 2016, IP: 77.42.170.220]
Fares, et al.: Stress, burnout and coping strategies in medical students
Student-led support programs that are designed to
promote the mentorship of junior students by senior
students are recommended because they appear to
lower student stress and ultimately burnout. Although
the Association of American Medical Colleges urges
medical schools to foster relationships between faculty
members and students to promote a positive learning
environment,[86] we agree with Wolf et al.[87] that studentguided programs may present a stronger source of
support and promote positive strategies for coping with
stress. Mouret[88] proposed that senior medical students
can more easily relate to challenges encountered by
junior students. Many studies have shown that such
events help in easing anxiety and stress and preventing
burnout.[14,89-92]
Linzer et al.[93] and Freedborn et al.[94] discussed the
importance of autonomy as a central component of
physician job satisfaction. Dyrbye et al.[95] believed
that autonomy was likely to be important for medical
students as well. Students bring unique perspectives
to curriculum committees and provide them a sense of
ownership in their educational experience.[95]
The evaluation system used to assess student
performance can also have a massive effect on the
learning environment. Robins et al.[96] evaluated the effect
of changing from numerical and letter grading schemes
to a pass-fail grading system on student performance
and satisfaction; they reported that students satisfaction
with the evaluation system and learning environment
improved with the pass-fail approach. Although certain
medical schools foster a pass-fail evaluation system for
the preclinical years, we believe that the competitive
mentality of the students that has developed during the
premedical years continues throughout the preclinical
years and can lead to anxiety and distress.
We agree with Stewart et al.[33] and Park and Adler[82]
that early poor academic performance in medical
school, mental health problems and avoidant coping
mechanisms may place students at risk of distress both
during and after medical school. We suggest that medical
schools offer career counseling, life-coaching and
confidential resources covered by the universitys health
insurance plan to help these students. We also believe
that student-led support groups, discussed earlier,
can help students in processing conflict, raising selfawareness and nurturing empathy. Maslach[97] added
that peer discussion groups also provide opportunities
for students to express, analyze and share feelings, which
decreases the likelihood of burnout. Pololi and Frankel[98]
asserted that shared reflections helped students in
realizing that their struggles were common and provided
an insight into how colleagues solved similar problems.
78
More work can also be done to improve the stress and
burnout conditions of preclinical medical students.
Parkerson et al. [14] emphasized the importance of
encouraging students to promote personal health with
regular physical activity and adequate sleep. In addition,
Wolf[99] and Gaber and Martin[100] believed that students
should be provided with appropriate periods of rest
during holidays and between modules to allow them to
dissociate from the rigors of education and training. The
transformation of medical students into medical doctors
who are care-giving, compassionate, knowledgeable,
well-appearing, and healthy requires improving the
living and learning conditions during their medical
education.[62]
Conclusion
This article implemented a detailed scholarly research
strategy to highlight key themes that are relevant
to preclinical medical students stress and burnout
by introducing their definitions and exploring their
prevalence and causes. In addition, this article proposed
expert strategies and theories to help in reducing the
incidence of stress and burnout and in promoting wellbeing among medical schools. Stress varied among the
different samples of preclinical medical students and
ranged between 20.9% and >90%, whereas the burnout
prevalence rates ranged between 27% and 75%. As a result
of work overload, overwhelming academic pressures to
learn much within a limited time span and a sense of
emotional commitment to medicine as a future career,
burnout was found to manifest early among preclinical
medical students; it then continues through the clinical
years. High stress and burnout levels are associated with
decreased life satisfaction, serious thoughts of dropping
out and suicidal ideations; these cyclically lead to poorer
performance, reduced commitment and higher levels
of stress. It is particularly important to propose and
implement strategies to reduce the incidence of stress
and burnout among preclinical medical students to
strengthen their commitment to medicine as a profession
and allow for better future patient care. Strategies that
focus on personal engagement, positive reinterpretation
and expression of emotion, support programs delivered
by senior students and extracurricular activities (mainly
musical and physical activities) are among the coping
mechanisms that are needed to reduce anxiety and thus,
stress and burnout. It is the duty of medical educators
to facilitate the utilization of such coping mechanisms
to allow for smoother preclinical years and eventually
more fruitful clinical years with physicians dedicated
to providing the best care and commitment to patients.
Financial support and sponsorship
Nil.
North American Journal of Medical Sciences | Feb 2016 | Volume 8 | Issue 2 |
[Downloaded free from http://www.najms.org on Thursday, February 25, 2016, IP: 77.42.170.220]
Fares, et al.: Stress, burnout and coping strategies in medical students
Conflicts of interest
There are no conflicts of interest.
19.
References
1.
2.
3.
4.
5.
6.
7.
8.
9.
10.
11.
12.
13.
14.
15.
16.
17.
18.
Guthrie EA, Black D, Shaw CM. Hamilton J, Creed FH, Tomenson
B. Embarking upon a medical career: Psychological morbidity in
first year medical students. Med Educ 1995;29:337-41.
Moffat KJ, McConnachie A, Ross S, Morrison JM. First year
medical student stress and coping in a problem-based learning
medical curriculum. Med Educ 2004;38:482-91.
Aktekin M, Karaman T, Senol YY, Erdem S, Erengin H,
Akaydin M. Anxiety, depression and stressful life events
among medical students: A prospective study in Antalya,
Turkey. Med Educ 2005;35:12-7.
Guthrie E, Black D, Bagalkote H, Shaw C, Campbell M,
Creed F. Psychological stress and burnout in medical students:
A five-year prospective longitudinal study. J R Soc Med
1998;91:237-43.
Givers JL, Tjia J. Depressed medical students use of mental
health services and barriers to use. Acad Med 2002;77:918-21.
Clark DC, Zeldow PB. Vicissitudes of depressed mood during
four years of medical school. JAMA 1988;260:2521-8.
Rosal MC, Ockene IS, Ockene JK, Barren SV, Ma Y, Hebert JR.
A longitudinal study of students depression at one medical
school. Acad Med 1997;72:542-6.
Mosley TH Jr, Perrin SG, Neral SM, Dubbert PM, Grothues CA,
Pinto BM. Stress, coping, and well-being among third-year
medical students. Acad Med 1994;69:765-7.
Roberts LW, Warner TD, Lyketsos C, Frank E, Ganzini L,
Carter D.; Collaborative Research Group on Medical Student
Health. Perceptions of academic vulnerability associated with
personal illness: A study of 1,027 students at nine medical
schools. Compr Psychiatry 2004;42:1-15.
Vitaliano PP, Maiuro RD, Russo J, Mitchell ES, Carr JE, Van
Citters RL. A biopsychosocial model of medical student
distress. J Behav Med 1988;11:311-31.
Raj SR, Simpson CS, Hopman WM, Singer MA. Health-related
quality of life among final-year medical students. CMAJ
2000;162:509-10.
Ball S, Bax A. Self-care in medical education: Effectiveness of
health-habits interventions for first-year medical students.
Acad Med 2002;77:911-7.
Tyssen R, Vaglum P, Gronvold NT, Ekeberg O. Suicidal
ideation among medical students and young physicians:
A nationwide and prospective study of prevalence and
predictors. J Affect Disord 2001;64:69-79.
Parkerson GR Jr, Broadhead WE, Tse CK. The health status
and life satisfaction of first-year medical students. Acad Med
1990;65:586-8.
Carson AJ, Dias S, Johnston A, McLoughlin MA, OConnor M,
Robinson BL, et al. Mental health in medical students: A case
control study using the 60 item General Health Questionnaire.
Scott Med J 2000;45:115-6.
Spiegel DA, Smolen RC, Jonas CK. An examination of
the relationships among interpersonal stress, morale and
academic performance in male and female medical students.
Soc Sci Med 1986;23:1157-61.
Spiegel DA, Smolen RC, Hopfensperger KA. Medical student
stress and clerkship performance. J Med Educ 1986;61:929-31.
Hojat M, Robeson M, Damjanov I, Veloski JJ, Glaser K, Gonnella JS.
20.
21.
22.
23.
24.
25.
26.
27.
28.
29.
30.
31.
32.
33.
34.
35.
36.
37.
38.
39.
Students psychosocial characteristics as predictors of academic
performance in medical school. Acad Med 1993;68:635-7.
Hojat M, Gonnella JS, Mangione S, Nasca TJ, Veloski JJ,
Erdmann JB, et al. Empathy in medical students as related to
academic performance, clinical competence and gender. Med
Educ 2002;36:522-7.
Woloschuk W, Harasym PH, Temple W. Attitude change during
medical school: A cohort study. Med Educ 2004;38: 522-34.
Hojat M, Mangione S, Nasca T, Rattner S, Erdmann JB,
Gonnella JS, et al. An empirical study of decline in empathy
in medical school. Med Educ 2004;38:934-41.
Crandall SJ, VoIk RJ, Loemker V. Medical students attitudes
toward providing care for the underserved: Are we training
socially responsible physicians? JAMA 1993;269:2519-23.
Rezler AG, Ten Haken JT. Affect and research in medical
education. Med Educ 1984;18:331-8.
Eron LD. D. The effect of medical education on attitudes:
A follow-up study. J Med Educ 1958;33:25-33.
Wolf TM, Balson PM, Faucett JM, Randall HM. A retrospective
study of attitude change during medical education. Med Educ
1989;23:19-23.
Eron LD. Effect of medical education on medical students
attitudes. J Med Educ 1955;30:559-66.
Rezler AG, Flaherty JA. The Interpersonal Dimension in
Medical Education. New York, NY: Springer; 1985.
Gutgesell M, Reeve R, Parsons B, Morse RM. Exercise and
alcohol consumption among medical students. Acad Med
1999;74:750-1.
Croen LG, Woesner M, Herman M, Reichgott M. A
longitudinal study of substance use and abuse in a single
class of medical students. Acad Med 1997;72:376-81.
Clark D, Eckenfels EJ, Daugherty SR, Fawcett J. Alcohol-use
patterns through medical school: A longitudinal study of one
class. JAMA 1987;257:2921-6.
Mangus RS, Hawkins CE, Miller MJ. Tobacco and alcohol use
among 1996 medical school graduates. JAMA 1998;280:1192-3,
1195.
Newbury-Birch D, Walshaw D, Kamali F. Drink and drugs:
From medical students to doctors. Drug Alcohol Depend
2001;64:265-70.
Stewart SM, Betson C, Lam TH, Marshall IB, Lee PW,
Wong CM. Predicting stress in first year medical students: A
longitudinal study. Med Educ 1997;31:163-8.
Bramness JG, Fixdal TC, Vaglum P. Effect of medical school
stress on the mental health of medical students in early and
late clinical curriculum. Acta Psychiatr Scand 1991;84:340-5.
Tyssen R, Vaglum P, Grnvold NT, Ekeberg O. Factors in
medical school that predict postgraduate mental health
problems in need of treatment: A nationwide and longitudinal
study. Med Educ 2001;35:110-20.
Shaikh BT, Kahloon A, Kazmi M, Khalid H, Nawaz K, Khan N,
et al. Students, stress and coping strategies: A case of Pakistani
medical school. Educ Health (Abingdon) 2001;17:346-53.
Dyrbye LN, Thomas MR, Huntington JL, Lawson KL, Novotny
PJ, Sloan JA, et al. Personal life events and medical student
burnout: A multicenter study. Acad Med 2006;81:374-84.
Dyrbye LN, Thomas MR, Harper W, Massie FS Jr, Power DV,
Eacker A, et al. The learning environment and medical student
burnout: A multicentre study. Med Educ 2009;43:274-82.
Santen SA, Holt DB, Kemp JD, Hemphill RR. Burnout in
medical students: Examining the prevalence and associated
factors. South Med J 2010;103:758-63.
North American Journal of Medical Sciences | Feb 2016 | Volume 8 | Issue 2 |
79
[Downloaded free from http://www.najms.org on Thursday, February 25, 2016, IP: 77.42.170.220]
Fares, et al.: Stress, burnout and coping strategies in medical students
40. Kjeldstadli K, Tyssen R, Finset A, Hem E, Gude T,
Gronvold NT, et al. Life satisfaction and resilience in
medical school A six-year longitudinal, nationwide and
comparative study. BMC Med Educ 2006;6:48.
41. Dyrbye LN, Massie FS Jr, Eacker A, Harper W, Power D,
Durning SJ, et al. Relationship between burnout and
professional conduct and attitudes among US medical
students. JAMA 2010;304:1173-80.
42. Dyrbye LN, Thomas MR, Massie FS, Power DV, Eacker A,
Harper W, et al. Burnout and suicidal ideation among U.S.
medical students. Ann Intern Med 2008;149:334-41.
43. F a r e s J , S a a d e d d i n Z , A l T a b o s h H , A r i d i H ,
El-Mouhayyar C, Koleilat MK, et al. Extracurricular
activities associated with stress and burnout in preclinical
medical students. J Epidemiol Glob Health 2015. [Epub
ahead of print].
44. Sidik SM, Rampal L, Kaneson N. Prevalence of emotional
disorders among medical students in a Malaysian university.
Asia Pac Fam Med 2003;2:213-7.
45. Zaid ZA, Chan SC, Ho JJ. Emotional disorders among medical
students in a Malaysian private medical school. Singapore
Med J 2007;48:895-9.
46. Fuad MD, Al-Zurfi BM, Qader MA, Abu Bakar MF, Elnajeh M,
Abdullah MR. Prevalence and risk factors of stress, anxiety
and depression among medical students of a private medical
university in Malaysia. Education in Medicine Journal
2015;7:e52-9.
47. Ko SM, Kua EH, Fones CS. Stress and the undergraduates.
Singapore Med J 1999;40:627-30.
48. Guthrie EA, Black D, Shaw CM, Hamilton J, Creed FH,
Tomenson B. Psychological stress in medical students: A
comparison of two very different university courses. Stress
Med 1997;13:179-84.
49. Konjengbam S, Laishram J, Singh BA, Elangbam V.
Psychological morbidity among undergraduate medical
students. Indian J Public Health 2015;59:65-6.
50. Sarikaya O, Civaner M, Kalaca S. The anxieties of medical
students related to clinical training. Int J Clin Pract 2006;
60:1414-8.
51. Yusoff MS, Abdul Rahim AF, Yaacob MJ. Prevalence and
sources of stress among Universiti Sains Malaysia medical
students. Malays J Med Sci 2010;17:30-7.
52. Sreeramareddy CT, Shankar PR, Binu VS, Mukhopadhyay C,
Ray B, Menezes RG. Psychological morbidity, sources of stress
and coping strategies among undergraduate medical students
of Nepal. BMC Med Educ 2007;7:26.
53. Gundersen L. Physician burnout. Ann Intern Med 2001;135:
145-8.
54. Ramirez AJ, Graham J, Richards MA, Cull A, Gregory WM,
Leaning MS, et al. Burnout and psychiatric disorder among
cancer clinicians. Br J Cancer 1995;71:1263-9.
55. Kilfedder CJ, Power KG, Wells TJ. Burnout in psychiatric
nursing. J Adv Nurs 2001;34:383-96.
56. Leiter MP, Harvie P, Frizzell C. The correspondence of
patient satisfaction and nurse burnout. Soc Sci Med 1998;
47:1611-7.
57. Cherniss C. Beyond Burnout: Helping Teachers, Nurses,
Therapists, and Lawyers Recover from Stress and
Disillusionment. New York, NY: Psychology Press; 1995.
58. Parker PA, Kulik JA. Burnout, self-and supervisor-rated job
performance, and absenteeism among nurses. J Behav Med
1995;18:581-99.
80
59. Maslach C, Schaufeli WB, Leiter MP. Job burnout. Annu Rev
Psychol 2001;52:397-422.
60. Goldberg R, Boss RW, Chan L, Goldberg J, Mallon WK,
Moradzadeh D, et al. Burnout and its correlates in emergency
physicians: Four years experience with a wellness booth. Acad
Emerg Med 1996;3:1156-64.
61. Lemkau JP, Rafferty JP, Gordon R Jr. Burnout and
career-choice regret among family practice physicians in early
practice. Fam Pract Res J 1994;14:213-22.
62. Ayoub F, Fares Y, Fares J. The psychological attitude of
patients toward health practitioners in Lebanon. N Am J Med
Sci 2015;7:452-8.
63. Maslach C, Jackson SE, Leiter MP. The Maslach Burnout
Inventory. 3rd ed. Palo Alto, CA: Consulting Psychologists
Press; 1996.
64. McManus IC, Keeling A, Paice E. Stress, burnout and doctors
attitudes to work are determined by personality and learning
style: A twelve year longitudinal study of UK medical
graduates. BMC Med 2004;2:29.
65. Galn F, Sanmartn A, Polo J, Giner L. Burnout risk in
medical students in Spain using the Maslach Burnout
Inventory-Student Survey. Int Arch Occup Environ Health
2011;84:453-9.
66. Fares Y, Fares J. Anatomical and neuropsychological effects
of cluster munitions. Neurol Sci 2013; 34: 2095-100.
67. Fares Y, El-Zaatari M, Fares J, Bedrosian N, Yared N. Traumarelated infections due to cluster munitions. J Infect Public
Health 2013;6:482-6.
68. Fares Y, Ayoub F, Fares J, Khazim R, Khazim M, Gebeily S. Pain
and neurological sequelae of cluster munitions on children and
adolescents in South Lebanon. Neurol Sci 2013; 34:1971-6.
69. Fares Y, Fares J, Gebeily S. Head and facial injuries due to
cluster munitions. Neurol Sci 2014; 35: 905-10.
70. Hoteit A, Fares J. Psycho-environmental tribulations arising
from cluster munitions in South Lebanon. Sci-Afric Journal
of Scientific Issues, Research and Essays 2014;2:469-73.
71. Robinson GE. Stresses on women physicians: Consequences
and coping techniques. Depress Anxiety 2003;17:180-9.
72. Doyle C, Hind P. Occupational stress, burnout and job status
in female academics. Gend Work Organ 1998;5:67-82.
73. Firth-Cozens J. Source of stress in women junior house officers.
BMJ 1990;301:89-91.
74. McMurray JE, Linzer M, Konrad TR, Douglas J, Shugerman R,
Nelson K. The work lives of women physicians results from
the physician work life study. The SGIM Career Satisfaction
Study Group. J Gen Intern Med 2000;15:372-80.
75. Gadzella BM, Ginther DW, Tomcala M, Bryant GW. Stress as
perceived by professionals. Psychol Rep 1990;67:979-83.
76. Whitley TW, Allison EJ Jr, Gallery ME, Cockington RA,
Gaudry P, Heyworth J, et al. Work-related stress and
depression among practicing emergency physicians: An
international study. Ann Emerg Med 1994;23:1068-71.
77. Peisah C, Latif E, Wilhelm K, Williams B. Secrets to
psychological success: Why older doctors might have lower
psychological distress and burnout than younger doctors.
Aging Ment Health 2009;13:300-7.
78. Dyrbye LN, Thomas MR, Huschka MM, Lawson KL,
Novotny PJ, Sloan JA, et al. A multicenter study of burnout,
depression, and quality of life in minority and nonminority
US medical students. Mayo Clin Proc 2006;81:1435-42.
79. Dyrbye LN, Thomas MR, Eaker A, Harper W, Massie FS Jr, Power
DV, et al. Race, ethnicity, and medical student well-being in the
North American Journal of Medical Sciences | Feb 2016 | Volume 8 | Issue 2 |
[Downloaded free from http://www.najms.org on Thursday, February 25, 2016, IP: 77.42.170.220]
Fares, et al.: Stress, burnout and coping strategies in medical students
United States. Arch Intern Med 2007;167: 2103-9.
80. Dyrbye LN, Harper W, Durning SJ, Moutier C, Thomas MR,
Massie FS Jr, et al. Patterns of Distress in US Medical Students.
Med Teach 2011;33:834-9.
81. Dahlin ME, Runeson B. Burnout and psychiatric morbidity
among medical students entering clinical training: A three
year prospective questionnaire and interview-based study.
BMC Med Educ 2007;7:6.
82. Park CL, Adler NE. Coping style as a predictor of health and
well-being across the first year of medical school. Health
Psychol 2003;22:627-31.
83. Tjia J, Givens JL, Shea JA. Factors associated with
undertreatment of medical student depression. J Am Coll
Health 2005;53:219-24.
84. Shanafelt TD, Balch CM, Bechamps G, Russell T, Dyrbye L,
Satele D, et al. Burnout and medical errors among American
surgeons. Ann Surg 2010;251:995-1000.
85. West CP, Huschka MM, Novotny PJ, Sloan JA, Kolars JC,
Habermann TM, et al. Association of perceived medical
errors with resident distress and empathy: A prospective
longitudinal study. JAMA 2006;296:1071-8.
86. Association of American Medical Colleges. Physicians for
the Twenty-First Century: The GPEP Report: Report of the
Panel on the General Professional Education of the Physician
and College Preparation for Medicine. Washington, DC:
Association of American Medical Colleges; 1984.
87. Wolf TM, Randall HM, Faucett JM. A survey of health
promotion programs in U.S. and Canadian medical schools.
Am J Health Promot 1988;3:33-6.
88. Mouret GM. Stress in a graduate medical degree. Med J Aust
2002;177(Suppl):S10-1.
89. Lemkau JP, Purdy RR, Rafferty JP, Rudisill JR. Correlates
90.
91.
92.
93.
94.
95.
96.
97.
98.
99.
100.
of burnout among family practice residents. J Med Educ
1988;63:682-91.
Myers DG. The funds, friends, and faith of happy people. Am
Psychol 2000;55:56-67.
Lee J, Graham AV. Students perception of medical school
stress and their evaluation of a wellness elective. Med Educ
2001;35:652-9.
Rathbun J. Helping medical students develop lifelong
strategies to cope with stress. Acad Med 1995;70:955-6.
Linzer M, Visser MR, Oort FJ, Smets EM, McMurray JE, de
Haes HC; Society of General Internal Medicine (SGIM) Career
Satisfaction Study Group (CSSG). Predicting and preventing
physician burnout: Results from the United States and the
Netherlands. Am J Med 2001;111:170-5.
Freedborn DK. Satisfaction, commitment, and psychological
well-being among HMO physicians. Permanente J 2000;2:22-30.
Dyrbye LN, Thomas MR, Shanafelt TD. Medical student
distress: Causes, consequences, and proposed solutions. Mayo
Clin Proc 2005;80:1613-22.
Robins LS, Fantone JC, Oh MS, Alexander GL, Shlafer M,
Davis WK. The effect of pass/fail grading and weekly quizzes
on first-year students performances and satisfaction. Acad
Med 1995;70:327-9.
Maslach C. Burned out. Hum Behav 1976;5:16-22.
Pololi L, Frankel RM. Small-group teaching emphasizing
reflection can positively influence medical students values.
Acad Med 2001;76:1172-3.
Wolf TM. Stress, coping and health: Enhancing well-being
during medical school. Med Educ 1994;28:8-17; discussion 55-7.
Gaber RR, Martin DM. Still-Well osteopathic medical
student wellness program. J Am Osteopath Assoc 2002;102:
289-92.
North American Journal of Medical Sciences | Feb 2016 | Volume 8 | Issue 2 |
81
También podría gustarte
- Academic StressDocumento6 páginasAcademic StressagnesnovaraniAún no hay calificaciones
- Anxiety and Depression Among Students of A Medical College in Saudi ArabiaDocumento6 páginasAnxiety and Depression Among Students of A Medical College in Saudi Arabiahadyan39Aún no hay calificaciones
- Guang 2020Documento6 páginasGuang 2020VANESSA CARIÑOAún no hay calificaciones
- A Cross Sectional Study On Hypochondriasis and Health Anxiety Among Medical Students in A Private Medical College in MalaysiaDocumento9 páginasA Cross Sectional Study On Hypochondriasis and Health Anxiety Among Medical Students in A Private Medical College in Malaysiasalsabela fithriAún no hay calificaciones
- College Students Mental Health Problems and Treatment ConsiderationsDocumento6 páginasCollege Students Mental Health Problems and Treatment ConsiderationsIsuAún no hay calificaciones
- UA OMSE Med/Ed Enews v3 No. 01 (AUG 2014)Documento10 páginasUA OMSE Med/Ed Enews v3 No. 01 (AUG 2014)KC Spear Ellinwood, former Director Instructional DevelopmentAún no hay calificaciones
- Critical Review of Simulation-Based Medical Education Research, 2003-2009Documento14 páginasCritical Review of Simulation-Based Medical Education Research, 2003-2009cegarcia100% (1)
- 2011 Nosocomial Infections - Knowledge and Source of Information Among Clinical Health Care Students in GhanaDocumento4 páginas2011 Nosocomial Infections - Knowledge and Source of Information Among Clinical Health Care Students in GhanaMostafa AbdelrahmanAún no hay calificaciones
- Extended Essay 4Documento20 páginasExtended Essay 4thatoAún no hay calificaciones
- Couden - Final Chikungunya Health Impact Framework PaperDocumento15 páginasCouden - Final Chikungunya Health Impact Framework Paperapi-449016836100% (1)
- An Integrative Literature Review On Post Organ Transplant Mortality Due To Renal Failure: Causes and Nursing CareDocumento18 páginasAn Integrative Literature Review On Post Organ Transplant Mortality Due To Renal Failure: Causes and Nursing CarePATRICK OTIATOAún no hay calificaciones
- How To Prepare A Research Proposal - Asya Al-RiyamiDocumento4 páginasHow To Prepare A Research Proposal - Asya Al-RiyamishemjazAún no hay calificaciones
- Final Research 2019 G9Documento30 páginasFinal Research 2019 G9Hana ZaneAún no hay calificaciones
- Burcu - Baba - MA ThesisDocumento181 páginasBurcu - Baba - MA ThesisBurcu BabaAún no hay calificaciones
- New Mbbs 16-05-2018 PDFDocumento234 páginasNew Mbbs 16-05-2018 PDFAmoAún no hay calificaciones
- Assessing Critical Care Nurses' Caring BehaviorsDocumento10 páginasAssessing Critical Care Nurses' Caring BehaviorsMarc Andreo MalalaAún no hay calificaciones
- PICOT Question Research Critiques: Student's NameDocumento8 páginasPICOT Question Research Critiques: Student's Namecatherine SitatiAún no hay calificaciones
- Recovery High Schools in Massachusetts: A Promising, Comprehensive Model For Adolescent Substance Abuse and DependenceDocumento44 páginasRecovery High Schools in Massachusetts: A Promising, Comprehensive Model For Adolescent Substance Abuse and DependenceThe Stacie Mathewson FoundationAún no hay calificaciones
- Annotated BibliographyDocumento4 páginasAnnotated Bibliographyapi-279741433Aún no hay calificaciones
- Bachelor of Nursing Science With HonourDocumento10 páginasBachelor of Nursing Science With HonourNURUL FARADILA BINTI OTHMAN STUDENTAún no hay calificaciones
- Literature Review of Post-Traumatic Stress Disorder in The Critical Care PDFDocumento14 páginasLiterature Review of Post-Traumatic Stress Disorder in The Critical Care PDFOriza Zara SativaAún no hay calificaciones
- Quality and Safety Education For Nurses CompetenciesDocumento5 páginasQuality and Safety Education For Nurses CompetenciesSammy ChegeAún no hay calificaciones
- Bekele ChakaDocumento74 páginasBekele ChakaDoods QuemadaAún no hay calificaciones
- Multifaceted Role of IL-1 in Cancer and InflammationDe EverandMultifaceted Role of IL-1 in Cancer and InflammationManisha SinghCalificación: 5 de 5 estrellas5/5 (1)
- Consensus Document Surgical Wound Dehiscence Improving Prevention and OutcomesDocumento48 páginasConsensus Document Surgical Wound Dehiscence Improving Prevention and OutcomesJeffri syaputraAún no hay calificaciones
- EditedDocumento108 páginasEditedYsvette JayaAún no hay calificaciones
- Qualitative Journal Club TemplateDocumento7 páginasQualitative Journal Club TemplatenanaAún no hay calificaciones
- Annotated Bibliography-1-1Documento4 páginasAnnotated Bibliography-1-1Alfonso MartinezAún no hay calificaciones
- NURS702 Critique 2Documento9 páginasNURS702 Critique 2natalie nodayAún no hay calificaciones
- Professional Role Development PlanDocumento10 páginasProfessional Role Development Planapi-5327002330% (1)
- Career Research PaperDocumento3 páginasCareer Research Paperapi-267168900100% (1)
- Prevalence of Schizophrenia Among Patients Admitted Into Neuro-Psychiatric Hospital, Rumuigbo, Port Harcourt, Rivers State, NigeriaDocumento9 páginasPrevalence of Schizophrenia Among Patients Admitted Into Neuro-Psychiatric Hospital, Rumuigbo, Port Harcourt, Rivers State, NigeriaSteven JonesAún no hay calificaciones
- Bullying: A Major Problem in NursingDocumento5 páginasBullying: A Major Problem in NursingAshlee PowersAún no hay calificaciones
- Nursing Students' Views On The COVID 19 Pandemic and Their Percieved Stress LevelsDocumento7 páginasNursing Students' Views On The COVID 19 Pandemic and Their Percieved Stress LevelsAudy SaviraAún no hay calificaciones
- Running Head: LITERATURE REVIEW 1Documento8 páginasRunning Head: LITERATURE REVIEW 1Maxine FomunungAún no hay calificaciones
- RBSK Dr. Vinay Gupta: How We Can Make R.B.S.K Better. Research Paper in International Journal of Pharmacy Biology and Medical SciencesDocumento9 páginasRBSK Dr. Vinay Gupta: How We Can Make R.B.S.K Better. Research Paper in International Journal of Pharmacy Biology and Medical SciencesLetTheTruthPrevailAún no hay calificaciones
- Enabling Learning in Nursing and Midwifery Practice: A Guide for MentorsDe EverandEnabling Learning in Nursing and Midwifery Practice: A Guide for MentorsSue WestAún no hay calificaciones
- Cómo Analizar Un PaperDocumento6 páginasCómo Analizar Un PaperAna Karina D'AmbrosioAún no hay calificaciones
- Criteria For Good Assessment: Consensus Statement and Recommendations From The Ottawa 2010 ConferenceDocumento9 páginasCriteria For Good Assessment: Consensus Statement and Recommendations From The Ottawa 2010 Conferencenugroho santosoAún no hay calificaciones
- Letter From PhysiciansDocumento6 páginasLetter From PhysiciansABC Action NewsAún no hay calificaciones
- Recent Global Epidemiology in StrokeDocumento73 páginasRecent Global Epidemiology in StrokeratuhamimAún no hay calificaciones
- Survey On Stress and Coping Strategies of Post Graduate StudentsDocumento9 páginasSurvey On Stress and Coping Strategies of Post Graduate StudentsInternational Journal of Innovative Science and Research TechnologyAún no hay calificaciones
- 2011 06 Commed Research TopicDocumento11 páginas2011 06 Commed Research TopicdtimtimanAún no hay calificaciones
- Infection Control in ICU'sDocumento58 páginasInfection Control in ICU'stummalapalli venkateswara rao100% (1)
- Nurs 603 Assignment 4 D StudentDocumento10 páginasNurs 603 Assignment 4 D Studentapi-429205355Aún no hay calificaciones
- Professionalism 2Documento344 páginasProfessionalism 2Jayson GeronaAún no hay calificaciones
- Jadad ScaleDocumento4 páginasJadad ScaleLuis Henrique SalesAún no hay calificaciones
- Ability Lab Institutional Placements Community Placement 1. Knowledge and Its ApplicationDocumento7 páginasAbility Lab Institutional Placements Community Placement 1. Knowledge and Its ApplicationSavanna ChambersAún no hay calificaciones
- EVIDENCE-BASED MEDICINE GUIDEDocumento34 páginasEVIDENCE-BASED MEDICINE GUIDEMuhamad Ghifari Azhar100% (1)
- Synopsis 8TH AAAAaaDocumento19 páginasSynopsis 8TH AAAAaaعثمان علیAún no hay calificaciones
- Index of Sources of StressDocumento8 páginasIndex of Sources of StressعزمباكلجوتوانAún no hay calificaciones
- Concepts of Health, Illness and DiseaseDocumento11 páginasConcepts of Health, Illness and DiseasetgalksjflkjAún no hay calificaciones
- Strategies To Deal With Uncertainty in Medicine 20Documento2 páginasStrategies To Deal With Uncertainty in Medicine 20Emilio AssisAún no hay calificaciones
- The Problem and Its BackgroundDocumento32 páginasThe Problem and Its BackgroundPRINCESS JOY BUSTILLOAún no hay calificaciones
- Long Term Conditions Collaborative: Improving Self Management SupportDocumento34 páginasLong Term Conditions Collaborative: Improving Self Management SupportDefi DestyawenyAún no hay calificaciones
- Dengue LancetDocumento16 páginasDengue LancetJorge Ricardo Uchuya GómezAún no hay calificaciones
- Measuring The Global Burden of DiseaseDocumento10 páginasMeasuring The Global Burden of DiseaseLili CRAún no hay calificaciones
- Final EssayDocumento9 páginasFinal Essayapi-383024083Aún no hay calificaciones
- Stress, Burnout and Coping Strategies in Preclinical Medical StudentsDocumento7 páginasStress, Burnout and Coping Strategies in Preclinical Medical StudentsChristiana TomescuAún no hay calificaciones
- Recognition of Stressors in Postgraduate PDFDocumento8 páginasRecognition of Stressors in Postgraduate PDFAmalul Fadly HasibuanAún no hay calificaciones
- tmp80F6 TMPDocumento24 páginastmp80F6 TMPFrontiersAún no hay calificaciones
- tmp6382 TMPDocumento8 páginastmp6382 TMPFrontiersAún no hay calificaciones
- tmp3CAB TMPDocumento16 páginastmp3CAB TMPFrontiersAún no hay calificaciones
- tmpCE8C TMPDocumento19 páginastmpCE8C TMPFrontiersAún no hay calificaciones
- tmp60EF TMPDocumento20 páginastmp60EF TMPFrontiersAún no hay calificaciones
- tmpF3B5 TMPDocumento15 páginastmpF3B5 TMPFrontiersAún no hay calificaciones
- tmpF178 TMPDocumento15 páginastmpF178 TMPFrontiersAún no hay calificaciones
- tmpEFCC TMPDocumento6 páginastmpEFCC TMPFrontiersAún no hay calificaciones
- tmp6F0E TMPDocumento12 páginastmp6F0E TMPFrontiersAún no hay calificaciones
- tmpE7E9 TMPDocumento14 páginastmpE7E9 TMPFrontiersAún no hay calificaciones
- tmpFFE0 TMPDocumento6 páginastmpFFE0 TMPFrontiersAún no hay calificaciones
- tmpC0A TMPDocumento9 páginastmpC0A TMPFrontiersAún no hay calificaciones
- Tmp1a96 TMPDocumento80 páginasTmp1a96 TMPFrontiersAún no hay calificaciones
- Tmpa077 TMPDocumento15 páginasTmpa077 TMPFrontiersAún no hay calificaciones
- tmpF407 TMPDocumento17 páginastmpF407 TMPFrontiersAún no hay calificaciones
- tmpE3C0 TMPDocumento17 páginastmpE3C0 TMPFrontiersAún no hay calificaciones
- tmp37B8 TMPDocumento9 páginastmp37B8 TMPFrontiersAún no hay calificaciones
- tmp72FE TMPDocumento8 páginastmp72FE TMPFrontiersAún no hay calificaciones
- tmpA0D TMPDocumento9 páginastmpA0D TMPFrontiersAún no hay calificaciones
- tmpD1FE TMPDocumento6 páginastmpD1FE TMPFrontiersAún no hay calificaciones
- tmp998 TMPDocumento9 páginastmp998 TMPFrontiersAún no hay calificaciones
- tmp8B94 TMPDocumento9 páginastmp8B94 TMPFrontiersAún no hay calificaciones
- tmp4B57 TMPDocumento9 páginastmp4B57 TMPFrontiersAún no hay calificaciones
- tmp9D75 TMPDocumento9 páginastmp9D75 TMPFrontiersAún no hay calificaciones
- Tmp75a7 TMPDocumento8 páginasTmp75a7 TMPFrontiersAún no hay calificaciones
- tmpB1BE TMPDocumento9 páginastmpB1BE TMPFrontiersAún no hay calificaciones
- tmpC30A TMPDocumento10 páginastmpC30A TMPFrontiersAún no hay calificaciones
- tmp2F3F TMPDocumento10 páginastmp2F3F TMPFrontiersAún no hay calificaciones
- tmp27C1 TMPDocumento5 páginastmp27C1 TMPFrontiersAún no hay calificaciones
- tmp3656 TMPDocumento14 páginastmp3656 TMPFrontiersAún no hay calificaciones
- Monitor SOPDocumento1 páginaMonitor SOPKhadsaar SinghAún no hay calificaciones
- 12 Angry MenDocumento42 páginas12 Angry MenMaroune FrankcityAún no hay calificaciones
- PB Mental Health Snapshot 4Documento5 páginasPB Mental Health Snapshot 4amanda wuAún no hay calificaciones
- Freud's Revolutionary Theory of PsychoanalysisDocumento13 páginasFreud's Revolutionary Theory of PsychoanalysisNicoleAún no hay calificaciones
- Relative Speed CalculationsDocumento2 páginasRelative Speed CalculationsShaikh Usman AiAún no hay calificaciones
- Secrets of Higher ConsciousnessDocumento186 páginasSecrets of Higher ConsciousnessRpPaAún no hay calificaciones
- THE CURATORIAL COMPLEX: SOCIAL DIMENSIONS OF KNOWLEDGE PRODUCTION Wiebke GronemeyerDocumento314 páginasTHE CURATORIAL COMPLEX: SOCIAL DIMENSIONS OF KNOWLEDGE PRODUCTION Wiebke GronemeyerJulieta ISECAún no hay calificaciones
- Psy10 Lab Experiment Determining The Abstract Reasoning Score of DATDocumento13 páginasPsy10 Lab Experiment Determining The Abstract Reasoning Score of DATTanbir. Nahid.Aún no hay calificaciones
- G. STANLEY HALL'S ADOLESCENCE: Brilliance and NonsenseDocumento12 páginasG. STANLEY HALL'S ADOLESCENCE: Brilliance and NonsenseDavor Jovanovic100% (1)
- Depression Moodjuice Self-Help GuideDocumento2 páginasDepression Moodjuice Self-Help GuideCleofe Lagura Diaz100% (1)
- Childhood Class 10 CbseDocumento3 páginasChildhood Class 10 CbseMuhammed SabeehAún no hay calificaciones
- 4 Reflective Journal FINALDocumento16 páginas4 Reflective Journal FINALKavita IyerAún no hay calificaciones
- Millennials Guide To Management and Leadership Wisdom en 41718Documento6 páginasMillennials Guide To Management and Leadership Wisdom en 41718jaldanaAún no hay calificaciones
- Reading Progress CHART MONDERONDODocumento20 páginasReading Progress CHART MONDERONDODoejejejAún no hay calificaciones
- Book 2Documento478 páginasBook 2api-3831754Aún no hay calificaciones
- PLT College PE 2 Course Self Defense ArnisDocumento2 páginasPLT College PE 2 Course Self Defense ArnisJessabel Alvarez BalictanAún no hay calificaciones
- Brain Imaging Techniques and HemisphereDocumento4 páginasBrain Imaging Techniques and HemisphereYour MaterialsAún no hay calificaciones
- Format For DefenseDocumento4 páginasFormat For DefenseJade SebastianAún no hay calificaciones
- What Is Taught Is Not LearnedDocumento1 páginaWhat Is Taught Is Not LearnedprasadbbnAún no hay calificaciones
- The Potential of Audio and Video For Formative Assessment of Music EducationDocumento15 páginasThe Potential of Audio and Video For Formative Assessment of Music EducationAmber DeckersAún no hay calificaciones
- Fs 6.on Becoming A TeacherDocumento7 páginasFs 6.on Becoming A TeacherGlenn Harold Ballad100% (1)
- Hannah Jenkins ResumeDocumento2 páginasHannah Jenkins Resumeapi-205543501Aún no hay calificaciones
- Running Head: Effects of Social Media 1Documento5 páginasRunning Head: Effects of Social Media 1Roland PennyAún no hay calificaciones
- Interventional Strategies To Decrease Nursing Student Anxiety in The ClinicalDocumento8 páginasInterventional Strategies To Decrease Nursing Student Anxiety in The ClinicalAlfindo Rio de GuntherswarchzhaffenstrassensAún no hay calificaciones
- The Importance of Listening in Communication PDFDocumento5 páginasThe Importance of Listening in Communication PDFrazian yanAún no hay calificaciones
- Most Research Suggests We Are Not Very Good at Detecting Fake EmotionsDocumento2 páginasMost Research Suggests We Are Not Very Good at Detecting Fake EmotionsVikram Kumar100% (1)
- Pledge of CommitmentDocumento4 páginasPledge of CommitmentCherilyn Saagundo100% (2)
- Focusing in Clinical Practice The Essence of Chang... - (Chapter 1 The Essence of Change)Documento19 páginasFocusing in Clinical Practice The Essence of Chang... - (Chapter 1 The Essence of Change)lemvanderburgAún no hay calificaciones
- Alejandro de Acosta How To Live Now or Never Essays and Experiments 20052013 PDFDocumento286 páginasAlejandro de Acosta How To Live Now or Never Essays and Experiments 20052013 PDFallahAún no hay calificaciones
- The Salesman Analysis by Tanmay TandonDocumento2 páginasThe Salesman Analysis by Tanmay TandonTanmay TandonAún no hay calificaciones