Documentos de Académico
Documentos de Profesional
Documentos de Cultura
Acoustic Stapedius Reflexes
Cargado por
Girish SubashTítulo original
Derechos de autor
Formatos disponibles
Compartir este documento
Compartir o incrustar documentos
¿Le pareció útil este documento?
¿Este contenido es inapropiado?
Denunciar este documentoCopyright:
Formatos disponibles
Acoustic Stapedius Reflexes
Cargado por
Girish SubashCopyright:
Formatos disponibles
OPEN ACCESS GUIDE TO AUDIOLOGY AND HEARING
AIDS FOR OTOLARYNGOLOGISTS
ACOUSTIC (STAPEDIUS) REFLEXES
Jackie L. Clark
The acoustic reflex, also known as the
stapedius reflex refers to an involuntary
muscle contraction of the stapedius muscle
in response to a high-intensity sound stimulus. Due to ease of administration and
information yielded, the acoustic reflex is
considered one of the most powerful
differential diagnostic audiological procedures.
The premise behind the immittance
instrumentation used to measure the
acoustic reflex is the ability to accurately
measure changes in reflected energy
occurring from stiffening of the tympanic
membrane as a result of contraction of the
stapedius muscle (For the premise behind
tympanometry see tympanometry chapter).
The amount of reflected and absorbed
energy varies depending on the admittance/impedance (flow/resistance) of energy within the system and the complex
interaction between the ear structures.
The acoustic reflex and the tympanogram
(see tympanometry chapter) are commonly
used to assess middle ear function and are
considered best practice. Each test yields
invaluable information based on the
delivery of acoustic energy (sound) to the
ear canal. Thanks to microprocessors, the
instruments used are now capable of rapid
middle ear function assessment (typically
<1min/ear).
Acoustic reflexes do not measure hearing
threshold. Rather, they measure reflected
energy which is a function of stapedius
muscle contraction; it allows one to indirectly assess the middle ear, cochlea and
neural innervation of the stapedius muscle.
As the acoustic reflex is involuntary and
bilateral, it is replicable and provides
valuable diagnostic information when
comparing the amount of reflected energy
according to signal intensity, as well as the
presence of ipsilateral and bilateral acoustic reflexes.
Premise behind instrumentation
An acoustic stimulus is presented to the
external auditory canal; energy is transferred from the ear canal through the middle
ear, some of which is reflected and some
absorbed by the tympanic membrane and
external ear structures.
The presence of reflexes within normal
intensity limits is consistent with normal
middle ear and brainstem function and
suggests that auditory sensitivity is not
significantly impaired. An elevated or absent acoustic reflex threshold is consistent
with a middle ear disorder, hearing loss in
the stimulated ear, and/or interruption of
neural innervation of the stapedius muscle.
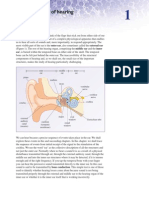
Anatomy & Physiology
Neural mechanisms mediate the acoustic
reflex that results in involuntary stapedius
muscle contraction stiffening the stapes
within the middle ear. It is presumed that
the physiologic reason for the reflex is that
it serves as an inhibitory response to reduce the sound intensities reaching the inner ear by as much as 20 dB evoked when
individuals vocalise (Mller, 2000).
As is illustrated in Figure 1, once a high
intensity auditory stimulus is initiated and
reaches the cochleae, neural impulses from
the auditory nerves (CN VIII) ascend from
both cochleae to each ipsilateral ventral
cochlear nucleus (VCN). From VCN the
reflex has two main neural pathways: one
passes from the VCN directly to the ipsilateral facial motor nucleus (CN VII) that
directly innervates the stapedius muscle
via the facial nerve and its stapedius
branch; the other passes from the VCN to
the superior olivary complex (SOC) before
the impulses cross at the brainstem to
innervate both ipsilateral and contralateral
facial motor nuclei.
is elicited at each frequency for each ear.
Stapedius muscle contraction increases as
the stimulus intensity is increased; it is
therefore possible to determine acoustic
reflex thresholds by incrementally increasing the stimulus by 5 dB steps, beginning
at 80 dB HL, until a contraction occurs
(Figure 2). With a normally functioning
middle ear and cochlea, an acoustic reflex
is elicited contralaterally at four frequencies (500, 1000, 2000, 4000 Hz), and
ipsilaterally at two frequencies (1000, 2000
Hz) when stimulus intensities of 85-90 dB
HL (hearing level) are delivered to the ear
canal.
Figure 1: Schematic of the acoustic reflex neural
pathways. CNVII (facial/seventh cranial nerve);
CNVIII (auditory/eighth cranial nerve); MNVII
(motor nucleus of seventh cranial nerve); SOC
(superior olivary complex); VCN (ventral cochlear
nucleus). Dashed lines represent the contralateral
pathway and solid lines represent ipsilateral pathway of acoustic reflex
Contraction of the stapedius muscle
stiffens the middle ear ossicles and tilts the
stapes in the oval window of the cochlea;
this effectively decreases the vibrational
energy transmitted to the cochlea. Stapedius muscle contraction is clinically apparent by a marked change in the impedance
properties of the middle ear.
It is important to realize that a bilateral
acoustic reflex occurs i.e. stimulating one
ear (ipsilateral ear) elicits an acoustic reflex in both the ipsilateral and contralateral
ears.
Acoustic Threshold
An acoustic reflex threshold is the lowest
intensity level at which an acoustic reflex
Figure 2: Example (right ear) of acoustic reflex
threshold obtained from an immittance instrument.
Results shown would indicate 85 & 90 dB HL
thresholds for 1000 and 2000 Hz respectively,
which would be expected for a normal ear
In a normal ear, after an initial contraction
the strength increases with each sequential
increase of signal intensity until a plateau
is reached. Threshold is defined as the
lowest acoustic stimulus intensity elicited
with a deflection magnitude of at least
0.03ml. As seen in the magnitude of
deflections in Figure 2, thresholds for both
frequencies assessed clearly fall within the
2
criteria of at least 0.03ml deflection. To
identify a threshold it is advisable to
confirm the magnitude of the deflection
with a repeat presentation. Once a threshold has been established at one frequency,
the intensity is recorded, and the other
frequencies are then assessed. During
quick screening it is not unusual to assess
an acoustic reflex threshold at only one
frequency and a single set intensity (~95 or
100 dB HL. An ipsilateral acoustic reflex
threshold tends to be attained at a slightly
lower intensity stimulus than an acoustic
reflex threshold elicited by a contralateral
stimulus.
Factors affecting acoustic reflexes
Ipsilateral conductive hearing loss:
Anything that obstructs transmission of
a sound signal to the cochlea in the
stimulated ear results in reduced or
absent contraction of the stapedius
muscles. Middle ear disorders therefore
easily mask an acoustic reflex. Forty
percent of patients with conductive
hearing loss of >20 dB HL do not have
an acoustic reflex. Once conductive
hearing loss reaches 40 dB HL, about
80% of patients do not have a reflex
(Jerger, Anthony, Jerger and Mauldin,
1974)
Ipsilateral sensorineural hearing loss:
This may obstruct transmission of a
signal beyond the cochlea of the stimulated ear and usually causes reduced or
absent contraction of the stapedius
muscles. However, because of recruitment of loudness in cochlear sensorineural hearing loss, acoustic reflexes
may occur even within the expected
normal or partially elevated intensity
range in the presence of mild or
moderate-to-severe sensorineural hearing loss.
Stapes fixation: The stapes footplate is
more-or-less fixed to the surrounding
bone with otosclerosis (and sometimes
with tympanosclerosis). This may interfere with the acoustic reflex in two
ways: it causes a conductive hearing
loss; and reduced mobility of the stapes
prevents stiffening of the tympanic
membrane when the stapedius muscle
contracts
Ossicular disarticulation: As with
otosclerosis, it causes a conductive
hearing loss, and if located lateral to
the stapes, prevents stiffening of the
ossicles and tympanic membrane when
the stapedius muscle contracts
Middle ear effusion: This causes a
conductive hearing loss, and reduces
compliance of the tympanic membrane
and middle ear structures and may
mask the presence of an acoustic reflex
Tympanic membrane perforation:
This causes a conductive hearing loss.
Furthermore, due to the perforation,
changes in compliance caused by contraction of the stapedius muscle cannot
be measured
Negative/abnormal middle ear pressure: To maximize the likelihood that a
reflex will be detected, the pressure on
either side of the tympanic membrane
has to be equal for the tympanic membrane to be at or near the point of
maximum compliance (see tympanometry chapter for further explanation).
This necessitates one to match the peak
pressure of the tympanogram to the
actual middle ear pressure so that valid
acoustic reflex threshold values may be
obtained
Facial nerve dysfunction: The stapedius muscle is innervated by the facial
nerve. Contraction of the stapedius
muscle has to occur for both ipsi- and
contralateral acoustic reflexes.
Interpretation of acoustic reflexes
Acoustic reflexes may be reported as:
Ipsilateral: Reflex recorded in ear to
which auditory stimulus is presented
Contralateral: Reflex recorded in ear
contralateral to which auditory stimulus is presented
Partially present: Reflex present at
some frequencies and absent at others
Elevated threshold: Reflex thresholds
elicited >100 dB HL
Absent reflex: No reflex elicited
transduction of neural impulses resulting in
an absence or reduction of acoustic reflexes elicited with ipsi- and/or contralateral
stimulation.
Reflex
Pattern
Reflex
Probe
Right
Probe
Left
Absent reflexes have also been observed in
individuals with normal or near-normal
hearing, which may then indicate middle
ear disease or neurological involvement of
the 8th cranial nerve, such as in pontine
angle tumours and auditory neuropathy
(see below), or neurological involvement
of the 7th cranial nerve. With facial nerve
paralysis, the absence of acoustic reflexes
in the presence of normal middle ear
function suggests a lesion in the neural
pathway proximal to the stapedius nerve,
whereas the presence of an acoustic reflex
in patients with facial nerve paralysis suggests that the lesion is distal to the origin
of the nerve. A very small percentage of
people will have normal auditory sensitivity and absent acoustic reflexes across all
frequencies without other identifiable pathology.
Interruption of Neural Transmission
As is illustrated in Figure 1, both ipsi- and
contralateral acoustic reflex pathways pass
through the SOC of the lower brainstem
before proceeding to the facial nerve. Consequently, brainstem lesions can interrupt
Interpretation
Normal
Normal
Contra
Normal
Ipsi
Contra
Vertical
Ipsi
Contra
Partial or elevated reflex thresholds may
indicate the presence of hearing loss at the
frequencies where they are specifically
absent.
Description
Diagonal
Ipsi
Contra
Inverted
L-shape
Ipsi
Horizontal
Contra
Ipsi
Contra
Unibox
Ipsi
Abnormal
whenever
probe in
affected ear
Abnormal
with sound
to the
affected ear
Crossed
stimulation
abnormal in
both ears;
uncrossed
stimulation
abnormal in
affected ear
Abnormal
to crossed
stimulation
on both
ears
Abnormal
with sound
to affected
ear on crossed stimulation only
Mild middle ear
disorder (left ear)
CN VII (facial
nerve) disorder
(left side)
Right nerve
disorder (left side)
Severe cochlear
loss (left ear)
Unilateral middle
ear disorder (left
ear)
Intra-axial
brainstem disorder
eccentric to one
side (left side)
Extra-axial and/or
intra-axial
brainstem disorder
Extra-axial and/or
intra-axial
brainstem disorder
Red box = Absent reflex
Table 1: Six patterns of acoustic reflex
based on presence or absence of each
and contralateral reflexes, based on
Jerger (1977). This example depicts
involvement.
thresholds
ipsilateral
Jerger &
left sided
Table 1 is a system to classify acoustic
reflex thresholds according to the presence
or absence of ipsilateral and contralateral
reflexes; it has great diagnostic value
(Jerger and Jerger, 1977). The system
categorises acoustic reflex thresholds into
six distinct patterns based on presence or
absence of ipsilateral and contralateral
reflexes. Cochlear, CN VII, CN VIII, or
brainstem sites of lesion are represented by
vertical, diagonal, inverted L-shape, horizontal, and unibox patterns.
4
Wideband reflectance technique
This is a newer measuring technique (Feeney, Douglas and Sanford, 2004) to assess
acoustic stapedius reflex thresholds by
using complex wideband (125 - 10,000 Hz
range) reflectance with a stimulus
resembling chirplike sounds instead of a
single probe tone frequency. The wideband
reflectance technique reportedly yields
more reliable results than the single probe
tone technique, and appears to hold
promise as a clinical procedure for
measuring acoustic reflexes for normalhearing subjects who fail to demonstrate
reflexes with the standard clinical procedure.
Acoustic Reflex Decay
This is another powerful differential diagnostic test and has a high degree of sensitivity to identify retrocochlear pathology
due to e.g. tumours of the cerebellopontine
angle. However magnetic resonance
imaging is considered the examination of
choice to identify retrocochlear pathology.
In order to examine acoustic reflex decay,
an extended duration signal (>10 seconds)
is presented, using low-frequency stimuli
(500, 1000 and 2000 Hz) contralateral to
the probe (test) ear. Muscle contraction of
the acoustic reflex is sustained in the
normal ear at maximum or near-maximum
amplitude throughout the entire duration of
the stimulus.
The standard procedure is to present the
stimulus contralaterally at 10 dB SL
(threshold of acoustic reflex of test ear), or
between 90 and 105 dB HL for 10 seconds.
Abnormal reflex decay is evidenced by an
inability of the stapedius muscle to
maintain full contraction (amplitude) for
the duration of the stimulus signal. When
reflex decay occurs within 5 seconds or at
frequencies less than 1000 Hz, it is
suggestive of 8th nerve dysfunction.
A.
B.
Figure 4: (A) Normal and (B) abnormal
findings on acoustic reflex decay test
Concerns have recently been raised about
causing temporary or permanent auditory
threshold shifts as a consequence of
presenting acoustic stimuli for extended
periods of time at exceptionally high
intensities. For this reason, clinicians are
cautioned to administer acoustic reflex
decay tests judiciously and never to exceed
105 dB HL presentation levels at any
frequency.
Caveats with acoustic reflex measures
It is important to recognize that there are
some limitations with acoustic reflex
measures.
Correct probe placement may become
challenging for those patients with
external auditory meatal openings
being larger than the available probe
tips (as seen in the elderly)
Conversely, the very small canal
openings (as seen in infants) may not
be compatible with any of the available
probes
In addition, care must be taken that the
patient is capable of sitting quietly.
Any jaw movements that occur during
5
coughing, crying, talking, swallowing,
or jaw clenching will result in artifact
and provide fallacious results.
Reportedly, collapsed canals due to
placement of supra-aural headphones
on the pinna of the contralateral ear
may also result in fallacious findings
Concluding remarks
Despite the few limitations with acoustic
reflex threshold testing, the advantages far
overshadow those limitations. Although
few new discoveries have been made with
acoustic reflex threshold testing, it is still
considered one of the most powerful
differential diagnostic tools that should be
within the standard battery of tests
attempted with all patients. Within a very
brief time period it allows one to identify
middle ear pathology; cochlear or retrocochlear pathology; evaluate neural transmission efficiency; while providing a
general indicator of magnitude of hearing
loss.
Author
Jackie L. Clark, PhD/CCC-A; F-AAA
Clinical Associate Professor
School of Behavioral & Brain Sciences,
UT Dallas/Callier Center
Research Scholar; Univ Witwatersrand,
Johannesburg, South Africa
Managing Editor International Journal of
Audiology
jclark@utdallas.edu
http://www.utdallas.edu/~jclark
Editors
Claude Laurent, MD, PhD
Professor in ENT
ENT Unit, Department of Clinical Science
University of Ume
Ume, Sweden
claude.laurent@ent.umu.se
De Wet Swanepoel PhD
Associate Professor
Department of Communication Pathology
University of Pretoria
Pretoria, South Africa
dewet.swanepoel@up.ac.za
References
Feeney MP, Douglas HK, & Sanford
CA (2004). Wideband reflectance
measures of the ipsilateral acoustic
stapedium reflex threshold. Ear
Hearing, 25: 421-30
Jerger S & Jerger J (1977). Diagnostic
value of cross vs. uncrossed acoustic
reflexes: Eighth nerve and brain stem
disorders. Arch Otolaryngol, 103: 44553
Jerger J, Anthony L, Jerger S, and
Mauldin L. (1974). Studies in impedance audiometry. III. Middle ear disorders. Arch Otolaryngol, 99: 165-71
Mller A. (2000). Hearing: Its physiology and pathophysiology. Academic
Press.181-90
Johan Fagan MBChB, FCORL, MMed
Professor and Chairman
Division of Otolaryngology
University of Cape Town
Cape Town, South Africa
johannes.fagan@uct.ac.za
OPEN ACCESS GUIDE TO
AUDIOLOGY & HEARING AIDS
FOR OTOLARYNGOLOGISTS
http://www.entdev.uct.ac.za
Open Access Guide to Audiology & Hearing Aids for
Otolaryngologists
by
Johan
Fagan
(Editor)
johannes.fagan@uct.ac.za is licensed under a Creative
Commons Attribution - Non-Commercial 3.0 Unported
License
También podría gustarte
- Acoustic Reflex: Presented by Arief Fakhrizal, DR Supervisor: Dr. Wijana, SP - THTKL (K)Documento48 páginasAcoustic Reflex: Presented by Arief Fakhrizal, DR Supervisor: Dr. Wijana, SP - THTKL (K)Arief FakhrizalAún no hay calificaciones
- Physiologyof Hearing: DR Seema SDocumento36 páginasPhysiologyof Hearing: DR Seema SDewi BoedhiyonoAún no hay calificaciones
- Hearing and BalanceDocumento72 páginasHearing and BalanceMAMAN100% (1)
- Physiology of Hearing: DR BukanuDocumento31 páginasPhysiology of Hearing: DR BukanuJumanne JayAún no hay calificaciones
- Physiology of HearingDocumento45 páginasPhysiology of HearingJP SouaidAún no hay calificaciones
- Audio BaileyDocumento7 páginasAudio BaileyMonisa HiraAún no hay calificaciones
- Rehab - Hi (New)Documento3 páginasRehab - Hi (New)devAún no hay calificaciones
- The Ear and HearingDocumento55 páginasThe Ear and Hearingc3rberussAún no hay calificaciones
- The Mechanics of Hearing: Ear Is Buried Within The Temporal Bone On Either Side of The Skull. The Temporal BoneDocumento14 páginasThe Mechanics of Hearing: Ear Is Buried Within The Temporal Bone On Either Side of The Skull. The Temporal Bonereal_yooriAún no hay calificaciones
- Auditory Pathways. Anatomy and PhysiologyDocumento23 páginasAuditory Pathways. Anatomy and PhysiologySal MonAún no hay calificaciones
- Auditory Tests With Disease Specific SignificanceDocumento60 páginasAuditory Tests With Disease Specific SignificanceSonal SharmaAún no hay calificaciones
- The Mechanics of HearingDocumento13 páginasThe Mechanics of HearingDustin NguyenAún no hay calificaciones
- CP Otitis PathoDETAILSDocumento9 páginasCP Otitis PathoDETAILSdabbleddave03Aún no hay calificaciones
- AuditionDocumento35 páginasAuditionBam SeñeresAún no hay calificaciones
- AD Unit-4Documento38 páginasAD Unit-4Vasanth VasanthAún no hay calificaciones
- Noise Study ReportDocumento4 páginasNoise Study ReportLiew Shu YanAún no hay calificaciones
- Auditory Pathways: Anatomy and Physiology: Handbook of Clinical Neurology March 2015Documento24 páginasAuditory Pathways: Anatomy and Physiology: Handbook of Clinical Neurology March 2015florensiaAún no hay calificaciones
- The Physics of HearingDocumento4 páginasThe Physics of HearingSaadia HumayunAún no hay calificaciones
- Binaural Science PDFDocumento5 páginasBinaural Science PDFRajko VojnovićAún no hay calificaciones
- Audio Production Theory: School of Science and Humanities Department of Visual CommunicationDocumento43 páginasAudio Production Theory: School of Science and Humanities Department of Visual Communicationpiano&musicaAún no hay calificaciones
- Auditory CognitiveDocumento100 páginasAuditory CognitiveEl KetoAún no hay calificaciones
- Anatomi Klinik TelingaDocumento51 páginasAnatomi Klinik TelingaSyahidatul ArifaAún no hay calificaciones
- Auditory Brainstem ResponseDocumento18 páginasAuditory Brainstem ResponseFree dataAún no hay calificaciones
- Human Auditory System: Audio Processing GuideDocumento11 páginasHuman Auditory System: Audio Processing GuideMohammed PublicationsAún no hay calificaciones
- 03 Friggeri 238174Documento11 páginas03 Friggeri 238174ffontanesiAún no hay calificaciones
- Sound Perception Topic: 92-96 Perceiving SoundDocumento18 páginasSound Perception Topic: 92-96 Perceiving SoundMariabutt ButtAún no hay calificaciones
- PsychoPhisics, ExperimentsDocumento9 páginasPsychoPhisics, ExperimentsMaria Isabel BinimelisAún no hay calificaciones
- Ocupational Hearing LossDocumento38 páginasOcupational Hearing LossNIKOLAOS CHATZAKISAún no hay calificaciones
- FlashcardsDocumento140 páginasFlashcardsDoodAún no hay calificaciones
- Pembahasan A. Fisiologi PendengaranDocumento10 páginasPembahasan A. Fisiologi Pendengarandita putriAún no hay calificaciones
- Auditory Function 2004 0211Documento10 páginasAuditory Function 2004 0211agung anugrahAún no hay calificaciones
- AUDIOMETERDocumento55 páginasAUDIOMETERANUSAYA SAHUAún no hay calificaciones
- Foto Acoustic EmitionDocumento83 páginasFoto Acoustic EmitionAlok kumarAún no hay calificaciones
- Anatomy and Physiology of The EarDocumento196 páginasAnatomy and Physiology of The EarChalsey Jene LorestoAún no hay calificaciones
- Ch. 9Documento51 páginasCh. 9Sara MitteerAún no hay calificaciones
- 2nd sound in medici2 جديDocumento70 páginas2nd sound in medici2 جديhanodywahbiAún no hay calificaciones
- The Psycho AcousticsDocumento10 páginasThe Psycho AcousticsTinh Thần Chiến BinhAún no hay calificaciones
- Anatomy and Physiology of The EarDocumento46 páginasAnatomy and Physiology of The EarKjoAún no hay calificaciones
- Noise and Potential Health EffectsDocumento8 páginasNoise and Potential Health EffectsTawfik Mohamed Abu ZaidAún no hay calificaciones
- 8 - Physiology of HearingDocumento38 páginas8 - Physiology of HearingHealthAún no hay calificaciones
- Presbycusis 181116131215 PDFDocumento66 páginasPresbycusis 181116131215 PDFWael ShamyAún no hay calificaciones
- Intro To SoundDocumento16 páginasIntro To SoundsnailbookAún no hay calificaciones
- Fundamentals of Architectural AcousticsDocumento49 páginasFundamentals of Architectural AcousticsRukminiPriyanka33% (3)
- Human HearingDocumento22 páginasHuman Hearingyasahswi91Aún no hay calificaciones
- Anatomy and Physiology of The EarDocumento46 páginasAnatomy and Physiology of The EarRoni Ananda Perwira HarahapAún no hay calificaciones
- Dr. Ashman's ENT Notes PDFDocumento56 páginasDr. Ashman's ENT Notes PDFJulian GordonAún no hay calificaciones
- Adaptation Adaptation Vs Fatigue: Presented By, P P Miza MariyamDocumento45 páginasAdaptation Adaptation Vs Fatigue: Presented By, P P Miza MariyamMiza Mariyam100% (1)
- Tugas DBDocumento2 páginasTugas DBEveline Sabrina RantiAún no hay calificaciones
- Ultrasound EyesDocumento8 páginasUltrasound Eyes-spectatorAún no hay calificaciones
- Report 2 EMM352 - Muhammad Aiman Danial Bin YatimDocumento3 páginasReport 2 EMM352 - Muhammad Aiman Danial Bin YatimAiman D.Aún no hay calificaciones
- Echo Course Manual 2019 Nov1Documento88 páginasEcho Course Manual 2019 Nov1Chris Jardine LiAún no hay calificaciones
- Physio HearingDocumento56 páginasPhysio Hearing65 Nidheesh Kumar PrabakamoorthyAún no hay calificaciones
- 8th NerveDocumento91 páginas8th NerveKinjal SharmaAún no hay calificaciones
- CHAPTER 21 The Auditory SystemDocumento15 páginasCHAPTER 21 The Auditory SystemRoger Fernando Abril DiazAún no hay calificaciones
- 141Documento22 páginas141Eko CahyonoAún no hay calificaciones
- Do You Hear What I Hear?:: A Lecture On The Auditory SenseDocumento39 páginasDo You Hear What I Hear?:: A Lecture On The Auditory Sensecherub23Aún no hay calificaciones
- Point-Of-View: Focalised. Focalisation Is The Camera EyeDocumento21 páginasPoint-Of-View: Focalised. Focalisation Is The Camera EyeVeerath தமிழன்Aún no hay calificaciones
- Physiology of Auditory SystemDocumento32 páginasPhysiology of Auditory SystemDr. T. Balasubramanian75% (4)
- Plasticidad Del Sistema Nervioso Central y Estrategias de Tratamiento para La Reprogramación SensoriomotoraDocumento6 páginasPlasticidad Del Sistema Nervioso Central y Estrategias de Tratamiento para La Reprogramación SensoriomotoralilishineAún no hay calificaciones
- Electronystagmograp HY: Hanna Rafia Naing Arthur Clyd Jerome Nogas Abdelmar Susulan Patricia Mae TusinDocumento18 páginasElectronystagmograp HY: Hanna Rafia Naing Arthur Clyd Jerome Nogas Abdelmar Susulan Patricia Mae TusinAbdelmar SusulanAún no hay calificaciones
- HEADACHEDocumento3 páginasHEADACHERajithaHirangaAún no hay calificaciones
- Review: Eduardo Tolosa, Alicia Garrido, Sonja W Scholz, Werner PoeweDocumento13 páginasReview: Eduardo Tolosa, Alicia Garrido, Sonja W Scholz, Werner PoeweSaraAún no hay calificaciones
- Parte 1Documento32 páginasParte 1Juan LópezAún no hay calificaciones
- Vertigo and DizzinessDocumento161 páginasVertigo and DizzinessSyariah KhilafahAún no hay calificaciones
- Occipital Neuralgia - Symptoms, Causes, and TreatmentsDocumento11 páginasOccipital Neuralgia - Symptoms, Causes, and Treatmentsthe conquerorAún no hay calificaciones
- Discipline & Ideas in The Applied SS Module 1Documento19 páginasDiscipline & Ideas in The Applied SS Module 1IM DatzAún no hay calificaciones
- DAY 2 Febrile Seizure Kuliah MHSDocumento45 páginasDAY 2 Febrile Seizure Kuliah MHSAdhi WiratmaAún no hay calificaciones
- Vestibular Questionnaire: Fill in The Blank SpacesDocumento2 páginasVestibular Questionnaire: Fill in The Blank SpacesyaddAún no hay calificaciones
- CSF Shift Edema PublishedDocumento15 páginasCSF Shift Edema PublishedIype CherianAún no hay calificaciones
- Vestibular Neuritis and LabyrinthitisDocumento18 páginasVestibular Neuritis and LabyrinthitischiquitaputriAún no hay calificaciones
- Types of Cerebral PalsyDocumento6 páginasTypes of Cerebral PalsySahil SahniAún no hay calificaciones
- What Should - Abstract ConceptsDocumento20 páginasWhat Should - Abstract Conceptsampicca100% (1)
- Cerebral Palsy Current Opinions On Definition Epidemiology Risk Factors Classification and Treatment OptionsDocumento15 páginasCerebral Palsy Current Opinions On Definition Epidemiology Risk Factors Classification and Treatment OptionsLaura RugeAún no hay calificaciones
- Cognitive Assessment: Neurological Perspective: Jimmy BarusDocumento54 páginasCognitive Assessment: Neurological Perspective: Jimmy BarusodiliajessicanpviaAún no hay calificaciones
- Seizures and Epilepsy LectureDocumento7 páginasSeizures and Epilepsy LecturekiaraAún no hay calificaciones
- Gait Disorders in Adults and The Elderly: A Clinical GuideDocumento15 páginasGait Disorders in Adults and The Elderly: A Clinical GuideAziznavii AmegoAún no hay calificaciones
- Frankel ScoreDocumento5 páginasFrankel ScoreaaaAún no hay calificaciones
- Timing of Cranioplasty After Decompressive Craniectomy ForDocumento5 páginasTiming of Cranioplasty After Decompressive Craniectomy ForjoerizalAún no hay calificaciones
- BGVVJH D AdDocumento2 páginasBGVVJH D AdUmmu AmirahAún no hay calificaciones
- Phineas GageDocumento1 páginaPhineas GageCharlotte G SarfatiAún no hay calificaciones
- Neurologic Involvement in Scleroderma, A Systematic ReviewDocumento13 páginasNeurologic Involvement in Scleroderma, A Systematic ReviewIsa RahmatikawatiAún no hay calificaciones
- Greenberg Neurosurgery 8th EditionDocumento3 páginasGreenberg Neurosurgery 8th EditionIde Bagoes Insani0% (1)
- Intracranial Berry Aneurysm - Wikipedia, The Free EncyclopediaDocumento3 páginasIntracranial Berry Aneurysm - Wikipedia, The Free EncyclopediaAniket MittalAún no hay calificaciones
- Misdiagnosis of Gastroesophageal Reux Disease As Epileptic Seizures in ChildrenDocumento4 páginasMisdiagnosis of Gastroesophageal Reux Disease As Epileptic Seizures in ChildrenIoana IaruAún no hay calificaciones
- A Rural Area Problem of Large Epidural Hematoma With HerniationDocumento5 páginasA Rural Area Problem of Large Epidural Hematoma With Herniationrian00019Aún no hay calificaciones
- Cerebellar: AtaxiaDocumento9 páginasCerebellar: AtaxiaAlfa RidziAún no hay calificaciones
- Neurofunctional Blueprints Transcripts For Tempe, January 2015 PDFDocumento82 páginasNeurofunctional Blueprints Transcripts For Tempe, January 2015 PDFAnonymous oCjRxyBP100% (3)
- By the Time You Read This: The Space between Cheslie's Smile and Mental Illness—Her Story in Her Own WordsDe EverandBy the Time You Read This: The Space between Cheslie's Smile and Mental Illness—Her Story in Her Own WordsAún no hay calificaciones
- ADHD is Awesome: A Guide to (Mostly) Thriving with ADHDDe EverandADHD is Awesome: A Guide to (Mostly) Thriving with ADHDCalificación: 5 de 5 estrellas5/5 (3)
- LIT: Life Ignition Tools: Use Nature's Playbook to Energize Your Brain, Spark Ideas, and Ignite ActionDe EverandLIT: Life Ignition Tools: Use Nature's Playbook to Energize Your Brain, Spark Ideas, and Ignite ActionCalificación: 4 de 5 estrellas4/5 (404)
- The Age of Magical Overthinking: Notes on Modern IrrationalityDe EverandThe Age of Magical Overthinking: Notes on Modern IrrationalityCalificación: 4 de 5 estrellas4/5 (32)
- Think This, Not That: 12 Mindshifts to Breakthrough Limiting Beliefs and Become Who You Were Born to BeDe EverandThink This, Not That: 12 Mindshifts to Breakthrough Limiting Beliefs and Become Who You Were Born to BeCalificación: 2 de 5 estrellas2/5 (1)
- The Body Keeps the Score by Bessel Van der Kolk, M.D. - Book Summary: Brain, Mind, and Body in the Healing of TraumaDe EverandThe Body Keeps the Score by Bessel Van der Kolk, M.D. - Book Summary: Brain, Mind, and Body in the Healing of TraumaCalificación: 4.5 de 5 estrellas4.5/5 (266)
- Love Life: How to Raise Your Standards, Find Your Person, and Live Happily (No Matter What)De EverandLove Life: How to Raise Your Standards, Find Your Person, and Live Happily (No Matter What)Calificación: 3 de 5 estrellas3/5 (1)
- Summary: The Psychology of Money: Timeless Lessons on Wealth, Greed, and Happiness by Morgan Housel: Key Takeaways, Summary & Analysis IncludedDe EverandSummary: The Psychology of Money: Timeless Lessons on Wealth, Greed, and Happiness by Morgan Housel: Key Takeaways, Summary & Analysis IncludedCalificación: 4.5 de 5 estrellas4.5/5 (82)
- The Ritual Effect: From Habit to Ritual, Harness the Surprising Power of Everyday ActionsDe EverandThe Ritual Effect: From Habit to Ritual, Harness the Surprising Power of Everyday ActionsCalificación: 4 de 5 estrellas4/5 (4)
- Summary: Outlive: The Science and Art of Longevity by Peter Attia MD, With Bill Gifford: Key Takeaways, Summary & AnalysisDe EverandSummary: Outlive: The Science and Art of Longevity by Peter Attia MD, With Bill Gifford: Key Takeaways, Summary & AnalysisCalificación: 4.5 de 5 estrellas4.5/5 (42)
- Raising Mentally Strong Kids: How to Combine the Power of Neuroscience with Love and Logic to Grow Confident, Kind, Responsible, and Resilient Children and Young AdultsDe EverandRaising Mentally Strong Kids: How to Combine the Power of Neuroscience with Love and Logic to Grow Confident, Kind, Responsible, and Resilient Children and Young AdultsCalificación: 5 de 5 estrellas5/5 (1)
- The Obesity Code: Unlocking the Secrets of Weight LossDe EverandThe Obesity Code: Unlocking the Secrets of Weight LossCalificación: 4 de 5 estrellas4/5 (6)
- Manipulation: The Ultimate Guide To Influence People with Persuasion, Mind Control and NLP With Highly Effective Manipulation TechniquesDe EverandManipulation: The Ultimate Guide To Influence People with Persuasion, Mind Control and NLP With Highly Effective Manipulation TechniquesCalificación: 4.5 de 5 estrellas4.5/5 (1412)
- The Courage Habit: How to Accept Your Fears, Release the Past, and Live Your Courageous LifeDe EverandThe Courage Habit: How to Accept Your Fears, Release the Past, and Live Your Courageous LifeCalificación: 4.5 de 5 estrellas4.5/5 (254)
- The Comfort of Crows: A Backyard YearDe EverandThe Comfort of Crows: A Backyard YearCalificación: 4.5 de 5 estrellas4.5/5 (23)
- The Marshmallow Test: Mastering Self-ControlDe EverandThe Marshmallow Test: Mastering Self-ControlCalificación: 4.5 de 5 estrellas4.5/5 (60)
- Summary: Limitless: Upgrade Your Brain, Learn Anything Faster, and Unlock Your Exceptional Life By Jim Kwik: Key Takeaways, Summary and AnalysisDe EverandSummary: Limitless: Upgrade Your Brain, Learn Anything Faster, and Unlock Your Exceptional Life By Jim Kwik: Key Takeaways, Summary and AnalysisCalificación: 5 de 5 estrellas5/5 (8)
- Dark Psychology & Manipulation: Discover How To Analyze People and Master Human Behaviour Using Emotional Influence Techniques, Body Language Secrets, Covert NLP, Speed Reading, and Hypnosis.De EverandDark Psychology & Manipulation: Discover How To Analyze People and Master Human Behaviour Using Emotional Influence Techniques, Body Language Secrets, Covert NLP, Speed Reading, and Hypnosis.Calificación: 4.5 de 5 estrellas4.5/5 (110)
- Why We Die: The New Science of Aging and the Quest for ImmortalityDe EverandWhy We Die: The New Science of Aging and the Quest for ImmortalityCalificación: 4 de 5 estrellas4/5 (5)
- To Explain the World: The Discovery of Modern ScienceDe EverandTo Explain the World: The Discovery of Modern ScienceCalificación: 3.5 de 5 estrellas3.5/5 (51)
- Summary: Thinking, Fast and Slow: by Daniel Kahneman: Key Takeaways, Summary & Analysis IncludedDe EverandSummary: Thinking, Fast and Slow: by Daniel Kahneman: Key Takeaways, Summary & Analysis IncludedCalificación: 4 de 5 estrellas4/5 (61)
- When the Body Says No by Gabor Maté: Key Takeaways, Summary & AnalysisDe EverandWhen the Body Says No by Gabor Maté: Key Takeaways, Summary & AnalysisCalificación: 3.5 de 5 estrellas3.5/5 (2)
- Cult, A Love Story: Ten Years Inside a Canadian Cult and the Subsequent Long Road of RecoveryDe EverandCult, A Love Story: Ten Years Inside a Canadian Cult and the Subsequent Long Road of RecoveryCalificación: 4 de 5 estrellas4/5 (46)