Documentos de Académico
Documentos de Profesional
Documentos de Cultura
Acute Upper Abdominal Pain: Step-By-Step Assessment
Cargado por
zafar_183250 calificaciones0% encontró este documento útil (0 votos)
10 vistas1 página1. The document provides steps for assessing acute upper abdominal pain, beginning with checking for free air on chest X-ray indicating perforated hollow viscus and referring for surgery if present.
2. It recommends checking an ECG for signs of ischemia, as abdominal pain can be an atypical presentation of myocardial infarction, and referring to cardiology if ST elevation is present.
3. It advises measuring serum amylase, with levels over 500 U/L indicating pancreatitis 95% of the time and over 1000 U/L being diagnostic, then considering CT scan if amylase is normal or equivocal but history suggests pancreatitis.
Descripción original:
usmle
Título original
mcleaod 48
Derechos de autor
© © All Rights Reserved
Formatos disponibles
PDF, TXT o lea en línea desde Scribd
Compartir este documento
Compartir o incrustar documentos
¿Le pareció útil este documento?
¿Este contenido es inapropiado?
Denunciar este documento1. The document provides steps for assessing acute upper abdominal pain, beginning with checking for free air on chest X-ray indicating perforated hollow viscus and referring for surgery if present.
2. It recommends checking an ECG for signs of ischemia, as abdominal pain can be an atypical presentation of myocardial infarction, and referring to cardiology if ST elevation is present.
3. It advises measuring serum amylase, with levels over 500 U/L indicating pancreatitis 95% of the time and over 1000 U/L being diagnostic, then considering CT scan if amylase is normal or equivocal but history suggests pancreatitis.
Copyright:
© All Rights Reserved
Formatos disponibles
Descargue como PDF, TXT o lea en línea desde Scribd
0 calificaciones0% encontró este documento útil (0 votos)
10 vistas1 páginaAcute Upper Abdominal Pain: Step-By-Step Assessment
Cargado por
zafar_183251. The document provides steps for assessing acute upper abdominal pain, beginning with checking for free air on chest X-ray indicating perforated hollow viscus and referring for surgery if present.
2. It recommends checking an ECG for signs of ischemia, as abdominal pain can be an atypical presentation of myocardial infarction, and referring to cardiology if ST elevation is present.
3. It advises measuring serum amylase, with levels over 500 U/L indicating pancreatitis 95% of the time and over 1000 U/L being diagnostic, then considering CT scan if amylase is normal or equivocal but history suggests pancreatitis.
Copyright:
© All Rights Reserved
Formatos disponibles
Descargue como PDF, TXT o lea en línea desde Scribd
Está en la página 1de 1
Abdominal pain
Acute upper abdominal pain: step-by-step assessment
1
Free air on CXR?
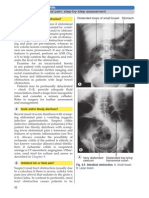
Perform an erect CXR in all unwell patients
with acute upper abdominal pain; the presence of free air under the diaphragm(s) (see
Fig. 4.4) indicates perforation of a hollow
viscus. Secure IV access, cross-match for
blood, resuscitate with IV fluids and refer
immediately to surgery.
If the CXR fails to demonstrate free air or
is equivocal but clinical suspicion is high
e.g. sudden-onset severe pain with epigastric tenderness and guarding, consider an
abdominal CT, but first check amylase and
ECG as described in steps 2 and 3.
2
ECG evidence of ischaemia?
Acute coronary syndromes, particularly
inferior myocardial infarction (MI), may
present atypically with epigastric pain.
However, hypotension or severe bleeding
in patients with acute abdominal pathology
may provoke or exacerbate ischaemia in
patients with stable coronary artery disease;
in these circumstances, administration of
powerful antithrombotic agents may have
catastrophic consequences.
Perform an ECG in all patients.
Refer immediately to cardiology if there
are features of an ST elevation MI (see
Box 6.1, p. 49).
In patients with ST depression, evaluate
carefully for hypotension, sepsis,
hypoxia and bleeding before
attributing changes to an acute
coronary event.
In patients with non-specific T wave
changes (see Box 6.1, p. 49), measure
cardiac biomarkers to assist diagnosis
and continue to search for alternative
causes.
Seek cardiology input if there is any
diagnostic doubt.
3
Amylase >500U/L?
Measure serum amylase in any patient with
acute severe epigastric pain. Patients with
an amylase >3 the reference range are 95%
likely to have pancreatitis; levels >1000U/L
are considered diagnostic.
If amylase levels are normal or equivocal,
continue to suspect the diagnosis if the
history is characteristic and:
there has been a delay in presentation
OR
there is a history of alcoholism
especially if the patient has had
previous episodes of pancreatitis.
In these patients, consider contrast
CT to look for evidence of pancreatic
inflammation.
Once the diagnosis has been made, evaluate repeatedly for evidence of complications, e.g. shock, hypoxia (acute respiratory
distress syndrome, ARDS), disseminated
intravascular coagulation (DIC); calculate
the Glasgow prognostic criteria score (Box
4.2) or other validated prognostic score;
and monitor CRP. Manage all patients
with severe or high-risk acute pancreatitis
(shock, organ failure, Glasgow score 3 or
peak CRP >210mg/L) in a critical care unit.
Perform an abdominal USS to look for
gallstones; those with severe pancreatitis
may require urgent ERCP and stone extraction, especially if there is jaundice or a
dilated common bile duct (CBD). Consider
CT to assess the extent of pancreatic injury
Box 4.2 Modified Glasgow criteria* for
assessing prognosis in acute pancreatitis
Age >55 years
PaO2 <8 kPa (60mmHg)
WBC >15 109/L
Albumin <32g/L
Serum calcium <2.00mmol/L (8mg/dL)
(corrected)
Glucose >10mmol/L (180mg/dL)
Urea >16mmol/L (45mg/dL) (after
rehydration)
ALT >200U/L
LDH >600U/L
*Severity and prognosis worsen as the number of these factors
increases. More than three implies severe disease.
35
También podría gustarte
- Institutional Pharmacy PracticeDocumento17 páginasInstitutional Pharmacy PracticeRichmond AmuraoAún no hay calificaciones
- Huntsville Businesses That Received More Than $150,000 From The Paycheck Protection ProgramDocumento14 páginasHuntsville Businesses That Received More Than $150,000 From The Paycheck Protection ProgramJonathan GrassAún no hay calificaciones
- Cardiac ReflexesDocumento2 páginasCardiac ReflexesfeliciaAún no hay calificaciones
- Anatomy MCQDocumento23 páginasAnatomy MCQPirabakar Mahendran100% (3)
- Charge Nurse ResponsibilitiesDocumento4 páginasCharge Nurse ResponsibilitiesdocpanchuAún no hay calificaciones
- Liver Trauma: DR Tarik El Batrawy Specialist General SurgeryDocumento50 páginasLiver Trauma: DR Tarik El Batrawy Specialist General Surgerykata61Aún no hay calificaciones
- PANCREASDocumento74 páginasPANCREASzaiba0786Aún no hay calificaciones
- Intermittent ExotropiaDocumento15 páginasIntermittent ExotropiakarenafiafiAún no hay calificaciones
- NCM 118 ReviewerDocumento315 páginasNCM 118 ReviewerKarlo BallonAún no hay calificaciones
- Sutures and Suturing PDFDocumento56 páginasSutures and Suturing PDFFrederick Alexander Trisna0% (1)
- Abdominal Compartment SyndromeDocumento7 páginasAbdominal Compartment Syndromemezgebu alemnehAún no hay calificaciones
- Post Test PEDIA FDocumento51 páginasPost Test PEDIA FGerry Aseo BritalAún no hay calificaciones
- Cholangitis: Reported By: R. DongaranDocumento18 páginasCholangitis: Reported By: R. DongaranVishnu Karunakaran100% (1)
- Watson and Raynor 1920Documento9 páginasWatson and Raynor 1920ShaneLee10267% (3)
- Acute Abdominal Pain: Step-By-Step AssessmentDocumento1 páginaAcute Abdominal Pain: Step-By-Step Assessmentzafar_18325Aún no hay calificaciones
- Acute PancreatitisDocumento40 páginasAcute PancreatitisAbdulsalam DostAún no hay calificaciones
- 26 2 KatzDocumento2 páginas26 2 KatznoemaraleAún no hay calificaciones
- Upper GI Bleed - SymposiumDocumento38 páginasUpper GI Bleed - SymposiumSopna ZenithAún no hay calificaciones
- Clinical Clerk Seminar Series: Approach To Gi BleedsDocumento11 páginasClinical Clerk Seminar Series: Approach To Gi BleedsAngel_Liboon_388Aún no hay calificaciones
- Acute Abdominal Pain: Step-By-Step AssessmentDocumento1 páginaAcute Abdominal Pain: Step-By-Step Assessmentzafar_18325Aún no hay calificaciones
- Bowels Open 6 Times Per 24 Hours: Document ControlDocumento7 páginasBowels Open 6 Times Per 24 Hours: Document ControlKeith PohlAún no hay calificaciones
- Acute Pancreatitis by DR DilmoDocumento50 páginasAcute Pancreatitis by DR Dilmosinan kAún no hay calificaciones
- Acute Pancreatitis: Presented By: DAHAL SHIRISHADocumento25 páginasAcute Pancreatitis: Presented By: DAHAL SHIRISHASiruAún no hay calificaciones
- Dr. S.P. Hewawasam (MD) Consultant Gastroenterologist/Senior Lecturer in PhysiologyDocumento33 páginasDr. S.P. Hewawasam (MD) Consultant Gastroenterologist/Senior Lecturer in PhysiologyAjung SatriadiAún no hay calificaciones
- Compartment SyndromeDocumento10 páginasCompartment SyndromeFebriyan EdmiAún no hay calificaciones
- Upper GIB Lecture and Presentation.Documento75 páginasUpper GIB Lecture and Presentation.Williams Emmanuel AdeyeyeAún no hay calificaciones
- Disease of The Biliary TreeDocumento7 páginasDisease of The Biliary TreeAbedinego MalukaAún no hay calificaciones
- Acute Lower Gastrointestinal BleedingDocumento18 páginasAcute Lower Gastrointestinal BleedingTrii Asih FatubunAún no hay calificaciones
- Abdominal Compartment SyndromeDocumento23 páginasAbdominal Compartment SyndromeUmar Farooq GondalAún no hay calificaciones
- Pancreatitis, Acute: Clinical PresentationDocumento26 páginasPancreatitis, Acute: Clinical Presentationapi-19641337Aún no hay calificaciones
- Review Small Bowel Colon: of The ANDDocumento43 páginasReview Small Bowel Colon: of The ANDgrahamabraAún no hay calificaciones
- Acute Pancreatitis: ManagementDocumento11 páginasAcute Pancreatitis: ManagementKakhaAún no hay calificaciones
- GIS-K-25 Acute Appendicitis Appendiceal Mass / AbscessDocumento24 páginasGIS-K-25 Acute Appendicitis Appendiceal Mass / AbscessYasmine Fitrina SiregarAún no hay calificaciones
- Welcome To The Morning Session: Dr. Sadia AfrinDocumento37 páginasWelcome To The Morning Session: Dr. Sadia AfrinGENERAL sharpAún no hay calificaciones
- Acute Abdominal-Wps OfficeDocumento26 páginasAcute Abdominal-Wps OfficeAbhash MishraAún no hay calificaciones
- Pancreatitis Ercp Pain Amylase Lipase ErcpDocumento24 páginasPancreatitis Ercp Pain Amylase Lipase ErcpPerplexed CeleryAún no hay calificaciones
- Surgery CBL Module 4Documento22 páginasSurgery CBL Module 4A SAún no hay calificaciones
- Abdominal Compartment Syndrome - UpdatedDocumento37 páginasAbdominal Compartment Syndrome - UpdatedErasto MwanganikaniAún no hay calificaciones
- Lectura 8Documento8 páginasLectura 8Daniela Andrea Tello GuaguaAún no hay calificaciones
- Biliary System and Pancreatic DisorderDocumento59 páginasBiliary System and Pancreatic DisorderAlda AdeliaAún no hay calificaciones
- Acute PancreatitisDocumento79 páginasAcute Pancreatitiszaiba0786Aún no hay calificaciones
- Surgical AbdomenDocumento3 páginasSurgical Abdomendude dAún no hay calificaciones
- Acute Abdomen Utk SekarwangiDocumento33 páginasAcute Abdomen Utk SekarwangiIca Trianjani SetyaningrumAún no hay calificaciones
- Upper GI BleedingDocumento30 páginasUpper GI BleedingBibek GhimireAún no hay calificaciones
- Abdominal Compartment Syndrome: Erik J. Teicher, MD, Michael D. Pasquale, MD, Facs, and Mark D. Cipolle, MD, PHD, FacsDocumento21 páginasAbdominal Compartment Syndrome: Erik J. Teicher, MD, Michael D. Pasquale, MD, Facs, and Mark D. Cipolle, MD, PHD, FacsholerikAún no hay calificaciones
- A Case of Rectus Sheath HematomaDocumento4 páginasA Case of Rectus Sheath HematomadrthirAún no hay calificaciones
- Acute AbdomenDocumento7 páginasAcute AbdomenStanley MwendaAún no hay calificaciones
- What Is An Acute AbdomenDocumento112 páginasWhat Is An Acute AbdomenLavasa SharmaAún no hay calificaciones
- Acute Upper Abdominal Pain: Step-By-Step AssessmentDocumento1 páginaAcute Upper Abdominal Pain: Step-By-Step Assessmentzafar_18325Aún no hay calificaciones
- Acute Cholecystitis:: Etiological TypesDocumento5 páginasAcute Cholecystitis:: Etiological Typesvivek yadavAún no hay calificaciones
- Acute PancreatitisDocumento76 páginasAcute Pancreatitissembakarani thevagumaranAún no hay calificaciones
- Chauke NJ 201908564 NUTRITIONAL SCREENINGDocumento7 páginasChauke NJ 201908564 NUTRITIONAL SCREENINGRulani PrinceAún no hay calificaciones
- Acute and Chronic Gastrointestinal BleedingDocumento7 páginasAcute and Chronic Gastrointestinal BleedingMarwan M.100% (1)
- ACGGuideline Acute Lower GI Bleeding 03012016 PDFDocumento16 páginasACGGuideline Acute Lower GI Bleeding 03012016 PDFGrahamOliverAceroVieraAún no hay calificaciones
- CholangitisDocumento4 páginasCholangitisNarianne Mae Solis Bedoy100% (1)
- Upper Gastrointestinal BleedingDocumento46 páginasUpper Gastrointestinal BleedingRashed ShatnawiAún no hay calificaciones
- Escalera, EverDocumento2 páginasEscalera, EverEver Seneca EscaLeraAún no hay calificaciones
- 5 Mesenteric IschemiaDocumento39 páginas5 Mesenteric IschemiaFahd Abdullah Al-refaiAún no hay calificaciones
- Pelvic MassesDocumento15 páginasPelvic MassesJulia kwapeAún no hay calificaciones
- Abdminal Compartment SyndromeDocumento9 páginasAbdminal Compartment SyndromeRafael BagusAún no hay calificaciones
- Ischemic Colitis: A Clinical Case and Concise ReviewDocumento15 páginasIschemic Colitis: A Clinical Case and Concise ReviewDevi AmaraAún no hay calificaciones
- Acute ColitisDocumento8 páginasAcute ColitisKhurram NadeemAún no hay calificaciones
- Rheumatology Journal Club Gut Vasculitis: by DR Nur Hidayati Mohd SharifDocumento36 páginasRheumatology Journal Club Gut Vasculitis: by DR Nur Hidayati Mohd SharifEida MohdAún no hay calificaciones
- 81Documento3 páginas81TSHEGOAún no hay calificaciones
- 105 116 Acute Gastrointestinal BleedingDocumento12 páginas105 116 Acute Gastrointestinal Bleedingmonia agni wiyatamiAún no hay calificaciones
- Sangrado Gastrointestinal OscuroDocumento20 páginasSangrado Gastrointestinal OscuroCristian Sandoval RojasAún no hay calificaciones
- AscitesDocumento71 páginasAscitessohilaw210Aún no hay calificaciones
- Colon Surgical Pathology - Clinical CaseDocumento2 páginasColon Surgical Pathology - Clinical CaseMariana UngurAún no hay calificaciones
- The Diagnostic Process: See Further Assessment of Chronic Liver Disease (P. 181) YesDocumento1 páginaThe Diagnostic Process: See Further Assessment of Chronic Liver Disease (P. 181) Yeszafar_18325Aún no hay calificaciones
- The Diagnostic ProcessDocumento1 páginaThe Diagnostic Processzafar_18325Aún no hay calificaciones
- Assessing Patients: A Practical Guide: The Clinical ExaminationDocumento1 páginaAssessing Patients: A Practical Guide: The Clinical Examinationzafar_18325Aún no hay calificaciones
- Assessment of Common Presenting ProblemsDocumento1 páginaAssessment of Common Presenting Problemszafar_18325Aún no hay calificaciones
- Box 4.1 Indicators of Systemic Inflammation: Differential DiagnosisDocumento1 páginaBox 4.1 Indicators of Systemic Inflammation: Differential Diagnosiszafar_18325Aún no hay calificaciones
- Acute Abdominal Pain: OverviewDocumento1 páginaAcute Abdominal Pain: Overviewzafar_18325Aún no hay calificaciones
- Differential Diagnosis: Abdominal PainDocumento1 páginaDifferential Diagnosis: Abdominal Painzafar_18325Aún no hay calificaciones
- Acute Upper Abdominal Pain: OverviewDocumento1 páginaAcute Upper Abdominal Pain: Overviewzafar_18325Aún no hay calificaciones
- Mesenteric Ischaemia Renal Tract Disorders: Non-Ulcer DyspepsiaDocumento1 páginaMesenteric Ischaemia Renal Tract Disorders: Non-Ulcer Dyspepsiazafar_18325Aún no hay calificaciones
- Acute Abdominal Pain: Step-By-Step AssessmentDocumento1 páginaAcute Abdominal Pain: Step-By-Step Assessmentzafar_18325Aún no hay calificaciones
- Acute Abdominal Pain: Step-By-Step AssessmentDocumento1 páginaAcute Abdominal Pain: Step-By-Step Assessmentzafar_18325Aún no hay calificaciones
- Acute Upper Abdominal Pain: Step-By-Step AssessmentDocumento1 páginaAcute Upper Abdominal Pain: Step-By-Step Assessmentzafar_18325Aún no hay calificaciones
- Laurence Hunter Helen Leng Caroline Jones Miles Hitchen Jennifer Rose AntbitsDocumento1 páginaLaurence Hunter Helen Leng Caroline Jones Miles Hitchen Jennifer Rose Antbitszafar_18325Aún no hay calificaciones
- Screening Tests: Click To Edit Master Subtitle StyleDocumento15 páginasScreening Tests: Click To Edit Master Subtitle Stylezafar_18325Aún no hay calificaciones
- TSCUH Trachy Bed Head PDFDocumento4 páginasTSCUH Trachy Bed Head PDFTudistef Analize SanatateAún no hay calificaciones
- NP ResumeDocumento3 páginasNP Resumeapi-554096544Aún no hay calificaciones
- En Brochure Inserts 2Documento44 páginasEn Brochure Inserts 2cr89omfAún no hay calificaciones
- All About Physiotherapy Student PresentationDocumento17 páginasAll About Physiotherapy Student Presentationvida konadu AgyemanAún no hay calificaciones
- Board Quality Committees Best PracticesDocumento5 páginasBoard Quality Committees Best PracticessanybyrAún no hay calificaciones
- Treatment of Childhood Oppositional Defiant Disorder: Bradley S. Hood, MD Marilisa G. Elrod, MD, PHD David B. Dewine, PHDDocumento13 páginasTreatment of Childhood Oppositional Defiant Disorder: Bradley S. Hood, MD Marilisa G. Elrod, MD, PHD David B. Dewine, PHDCristinaAún no hay calificaciones
- JAAOS - Volume 11 - Issue 05 September & October 2003Documento83 páginasJAAOS - Volume 11 - Issue 05 September & October 2003kenthepaAún no hay calificaciones
- Alicia Gardner ResumeDocumento1 páginaAlicia Gardner Resumeapi-454614211Aún no hay calificaciones
- Anaesthesia Syllabus BfuhsDocumento22 páginasAnaesthesia Syllabus BfuhsHarshit ChempallilAún no hay calificaciones
- Bacterial Sepsis in PregnancyDocumento14 páginasBacterial Sepsis in PregnancydraasfourAún no hay calificaciones
- Super Baby Food Starting SolidsDocumento5 páginasSuper Baby Food Starting SolidsJeffrey PeekoAún no hay calificaciones
- Ficha Tecnica Test de StereopsisDocumento2 páginasFicha Tecnica Test de StereopsisJennifer Andrea PardoAún no hay calificaciones
- The Correlation Between Osteophorosis and Tooth LossDocumento10 páginasThe Correlation Between Osteophorosis and Tooth LossAgeng BudianantiAún no hay calificaciones
- Network ListDocumento880 páginasNetwork ListRobbin BajpaiAún no hay calificaciones
- Case Study AppendicitisDocumento3 páginasCase Study Appendicitis2literAún no hay calificaciones
- Resume 2Documento1 páginaResume 2api-436090845Aún no hay calificaciones
- Ladies Doctor in MadhubaniDocumento5 páginasLadies Doctor in MadhubaniShubh ParmarAún no hay calificaciones
- Annotated Bibliography 3Documento2 páginasAnnotated Bibliography 3api-486757147Aún no hay calificaciones
- Hair-Grooming Syncope SeizuresDocumento5 páginasHair-Grooming Syncope Seizurestototm4480Aún no hay calificaciones
- Jurnal AppDocumento19 páginasJurnal AppDira RiskaAún no hay calificaciones
- Clinical Orthotic Services Guide: ProstekDocumento20 páginasClinical Orthotic Services Guide: ProstekJerry NgAún no hay calificaciones