Documentos de Académico
Documentos de Profesional
Documentos de Cultura
The Importance of Neuroimaging in Abusive Head Trauma: Neuroradiology
Cargado por
Ichiyoki IchsidaTítulo original
Derechos de autor
Formatos disponibles
Compartir este documento
Compartir o incrustar documentos
¿Le pareció útil este documento?
¿Este contenido es inapropiado?
Denunciar este documentoCopyright:
Formatos disponibles
The Importance of Neuroimaging in Abusive Head Trauma: Neuroradiology
Cargado por
Ichiyoki IchsidaCopyright:
Formatos disponibles
Imaging, 23 (2014), 20110067
NEURORADIOLOGY
The importance of neuroimaging in abusive head trauma
1
N STOODLEY, FRCR and 2M WILLIAMS, FRCR
Department of Neuroradiology, Frenchay Hospital, Bristol, UK
Department of Radiology, Craigavon Area Hospital, Portadown, UK
Summary
A shaking event is a common mechanism in abusive head trauma (AHT).
AHT is associated with greater morbidity and mortality than accidental (usually
impact) head trauma.
AHT gives rise to different patterns of subdural haemorrhage (SDH) and
parenchymal brain injury from impact head trauma.
Multifocal SDH is best regarded as a marker of a mechanism of injury but does not
itself cause symptoms and signs.
Associated parenchymal brain injury leads to symptoms and signs and relates to
outcome.
Published standards for the radiological investigation of AHT are available and
should be followed.
doi: 10.1259/img.20110067
2014 The British Institute of
Radiology
Cite this article as: Stoodley N, Williams M. The importance of neuroimaging in abusive head trauma. Imaging 2014;
23:20110067.
Abstract. Abusive head trauma (AHT) is best defined as
a head injury occurring to a child as a result of an act by a carer
that may be negligent, reckless or deliberate. Whilst there are
a number of different potential mechanisms involved in AHT,
one of the most common is generally (although not universally)
accepted to involve shaking; this article will concentrate on this
type of injury and will therefore include AHT that refers to
shaking injuries. Over the past decade, we have gained a much
better understanding of the nature of such injuries from
disciplines such as paediatrics, neuroradiology and neuropathology, and we are now better equipped to recognize such
injuries and to intervene when an injury occurs towards the
lower end of the spectrum of severity to try to prevent a later
potentially more serious injury. This is extremely important as
the mortality and morbidity in terms of neurodevelopmental
outcome of injuries involving shaking are considerably worse
than equivalent accidental injuries (the vast majority of which
are secondary to impact head trauma). Some of the concepts
regarding AHT that were widely held 1015 years ago have
either been shown not to be true or are not sustainable on the
basis of the current evidence base. This article will review
the role of neuroimaging in the diagnosis of AHT in the light of
the current recommendations for imaging in suspected AHT
and will discuss the current state of mainstream opinion in the
context of everyday clinical experience and the published
evidence base.
Address correspondence to: Dr Neil Stoodley. E-mail: neilstoodley@
doctors.org.uk
birpublications.org
Why bother?
A number of studies suggest that the overall incidence
of subdural haemorrhages occurring as a result of abusive
head trauma (AHT) seems fairly consistent at around
24 per 100 0001,2 (a similar incidence to that of all types of
cancer in the infant population). These studies obviously
only relate to infants and children who have presented to
a hospital and where the treating clinicians have requested
neuroimaging studies, which have subsequently shown
appearances consistent with AHT. It is probable that the
overall population incidence of subdural bleeding secondary to a shaking event is greater, as a proportion of
infants who sustain such an injury are likely to develop
transient and non-specific symptoms which resolve spontaneously and these infants are not presented to a hospital.
It is important to remember that the symptoms and signs
seen after an episode of AHT are not due to the subdural
haemorrhages but to the associated brain injury. The
commonest cause of subdural bleeding in infants is being
born, with MRI studies of normal, completely asymptomatic, term infants showing that the incidence of birthrelated subdural bleeding varies from 9% to 46%.3,4 The
lowest reported incidence of birth-related subdural bleeding follows elective Caesarean section and the highest
follows failed instrumental delivery (forceps and/or ventouse). Given the current UK birth rate, this equates to
a considerable number of babies who have birth-related
subdural bleeding that is clinically silent.
If birth-related subdural bleeding can be asymptomatic, it is likely that subdural bleeding from other causes
1 of 9
N Stoodley and M Williams
such as accidental impact head trauma and AHT could
also be clinically silent (in the absence of any associated
brain injury). This is an extremely important consideration in terms of identifying infants who have sustained
subdural bleeding as a result of AHT but in whom there
are no current abnormal neurological symptoms or signs:
identifying this at-risk group may prevent a subsequent
episode where brain injury does occur with associated
morbidity and mortality. This is the rationale behind
using head CT as an extension of the skeletal survey to
identify occult injuries.
Outcome studies have consistently shown that morbidity and mortality are considerably higher in AHT than
following accidental head trauma.1,5 Most episodes of
accidental head trauma in children are neurologically
benign and do not lead to significant long-term problems.6 The difference between these groups seems to be
due to the nature of any associated brain injury: typical
domestic impact head trauma rarely gives rise to parenchymal injury; more severe impact head trauma may give
rise to focal injuries such as contusions or diffuse axonal
injury, whereas the brain injury seen in cases of AHT
involving shaking is hypoxicischaemic in nature.7,8
Outcome studies of infants admitted to hospital following accidental head trauma or AHT with similar degrees
of head injury in terms of assessment of the Glasgow
Coma Score on admission show much higher rates of
death and disability in the AHT group.9,10
Patterns of neuroimaging abnormalities
As radiologists, much of our working lives are spent
looking at images and identifying abnormalities and
assessing the patterns of those abnormalities in light of
the clinical information available to construct a differential diagnosis. This approach is as valid in the assessment
of infant head trauma as for anything else that we do.
Assuming that our clinical colleagues do not find evidence of a naturally occurring medical condition in
a child that would account for subdural bleeding, the
presence of subdural haemorrhage is strongly associated
with head trauma. The types of head trauma that an infant may have sustained are birth related, accidental and
non-accidental head injury and different patterns of
subdural bleeding and of parenchymal brain injury are
seen in these groups.
Subdural bleeding as a result of accidental
head trauma
The vast majority of accidental head trauma occurs as
a result of impact, with other mechanisms such as crush
injury occurring less frequently (certainly in the context of
domestic head trauma). Children are no different from
adults in this respect, and all radiologists will have seen
subdural haematomas as a result of impact head injury.
Most are of relatively small volume (although occasionally we see large space-occupying extradural or subdural
haematomas) but, unless the impact has been very severe,
the subdural haematoma is seen at a single site, usually
related to the site of impact (but occasionally diagonally
opposite).
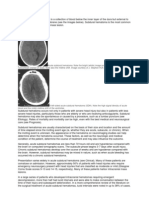
The view is sometimes expressed that a significant
degree of force is required to produce a subdural haematoma. The absolute degree of force required is not
known, and we do not know the true incidence of
subdural haematoma following impact head injury as
not all infants and children who sustain a blow to the
head have a CT or MRI scan. However, as the senior
author (NS) has been involved in a small number of
cases where an independently witnessed toddler fall
from standing height has led to the development of
a small acute subdural haematoma, the degree of force
required is presumably not necessarily that great
(Figure 1).
Subdural bleeding as a result of abusive
head trauma
The typical pattern of acute subdural bleeding in AHT is
of shallow (so-called thin film) subdural haematomas that
are most commonly seen in the posterior interhemispheric
fissure, posterior fossa and, in contradistinction to birthrelated subdural haematomas, over the cerebral convexities. The pattern of subdural bleeding in AHT is in part
similar to that seen in birth-related bleeding, but most
cases can be differentiated from birth-related bleeding by
the appearance of the blood on scans in terms of the
Birth-related subdural bleeding
Although only relatively small numbers of cases have
been reported, the pattern of birth-related subdural
bleeding has been consistent and is reported in the posterior fossa and/or over the posterior aspects of the cerebral hemispheres adjacent to the falx. In the absence of
an obvious history of significant birth trauma, these are
small non-space-occupying collections of blood. Birthrelated subdural bleeding in normal term infants has not
been reported over the frontal regions or related to the
anterior interhemispheric fissure. Even smaller numbers
of babies have been followed up by imaging, but the
published evidence base suggests that birth-related subdural bleeding in this group resolves in terms of scan
appearances by 4 weeks of age.3,4
2 of 9
Figure 1. CT scan showing a single-site acute subdural
haematoma over the right frontal region following an
independently witnessed toddler fall from standing height
onto a carpeted floor.
Imaging 2014, 23, 20110067
The importance of neuroimaging in abusive head trauma
assessment of the age of the blood (discussed further below). By themselves, these thin-film collections are not
space occupying and do not have any primary effect on
the underlying brain. The significance of these collections
of blood is therefore their very presence, not their (lack of)
effect on the underlying brain, and this means that, because they often appear so insignificant, their huge importance as markers of a mechanism of injury is too often
overlooked (Figure 2).
Parenchymal brain injury as a result of accidental
head trauma
Again, the appearances of impact head trauma in
infants and children are similar to those seen in older
children and adults, and, so, everyday radiological experience is as relevant as with the topic of subdural
bleeding. Significant impact head trauma is of course
very unusual in the context of non-ambulant infants in
the absence of an obvious history.
In terms of brain injury, the two main types seen as
a result of impact head trauma are contusions and diffuse
axonal injury (shearing injury). However, even following
significant impact events, such parenchymal injuries are
relatively unusual in the paediatric population (Figure 3).
Some years ago, shearing injuries were considered to be
the primary type of brain injury in AHT, but with
improvements in cross-sectional imaging techniques and
with evidence from neuropathological studies involving
cohorts of fatal cases of AHT, such injuries have been
shown to be unusual in AHT unless significant impact
has been involved in the mechanism of injury.7,8
Pattern of parenchymal brain injury in abusive
head trauma
As discussed above, the primary type of brain injury in
AHT is hypoxicischaemic in nature. The degree of associated brain injury is the primary determinant of outcome
and the difference between the types of parenchymal injury in accidental and non-accidental head trauma is the
likely reason for the different outcomes in groups who
have sustained brain injuries in these different ways. Cases
where the pattern and volume of subdural bleeding are
Figure 3. CT scans of three children following impact head
trauma. (a) Image of a 6-week-old child who sustained
a right-sided parietal skull fracture following a witnessed
fall from his mothers arms onto a pavement (note the
absence of subdural bleeding or parenchymal brain injury).
(b; i, ii) Images of a 4-week-old child who fell approximately
90 cm onto a quarry-tiled floor and sustained a left-sided
diastatic parietal skull fracture with extensive soft-tissue
scalp swelling but no intracranial haemorrhage or parenchymal brain injury. (c; i, ii) Images of an 18-month-old child
who fell from a first floor window and sustained a continuous left-sided frontal and parieto-occipital skull fracture
with a small amount of acute subdural blood seen adjacent
to the left side of the posterior falx but no parenchymal
brain injury.
similar have very different outcomes according to the degree of associated brain injury (Figure 4).
Assessment of the age of subdural bleeding
Figure 2. (a, b) CT scans of two infants admitted with an
encephalopathic illness showing thin-film acute subdural
haematomas in the posterior interhemispheric region.
birpublications.org
As radiologists, we are familiar with the way in which
the appearance of blood on CT and MRI changes with
time: acute blood is brighter than the underlying brain on
CT and becomes progressively darker as it matures such
that a chronic subdural haematoma is darker than the
underlying brain. What is often not appreciated is that
3 of 9
N Stoodley and M Williams
Figure 5. (a, b) CT scans of an 18-month-old child who was
being carried downstairs by a carer. The carer tripped and fell
and landed on the child, who sustained a depressed rightsided skull fracture, acute extra- and subdural haemorrhages
together with an intermediate subdural collection anteriorly;
an acute traumatic effusion.
the underlying brain on CT, thus mimicking chronic (or
subacute) subdural haematomas (Figure 5).
This is extremely important in the context of AHT, as it
means that, in many of the cases where the initial radiology report is of acute and chronic or acute on chronic
subdural bleeds, the subdural abnormalities are actually
due to the presence of both discrete collections of acute
subdural blood and acute traumatic effusions, i.e. all of
the subdural abnormalities are likely to have occurred at
the same time rather than as a result of more than one
event occurring at separate times, weeks apart.
The same applies to appearances on MRI scans. Subdural collections that appear of different signal intensities
(especially on sensitive sequences such as T2 fluid attenuation inversionrecovery) are often reported erroneously as representing blood of different ages. Whilst that
may be true in terms of discrete collections of blood, if the
collection is actually a mixture of blood and other fluid,
then the difference in signal intensity on the same sequence is more likely to represent the different concentration of blood breakdown products within the collection
(Figure 6).
Acute traumatic effusions are now recognized as being
very common in the context of AHT. It is difficult to
differentiate absolutely between acute traumatic effusions
and chronic subdural haematomas, but imaging pointers
are listed in Table 1 and illustrated in Figure 7.
Figure 4. CT scans of three children following an episode of
non-accidental head injury showing similar patterns of acute
subdural haemorrhages but different degrees of hypoxic
ischaemic brain injury. (a) No discernible hypoxic changes and
recovered quickly. (b; i, ii) Diffuse low-attenuation change
with reduced greywhite differentiation and a reversal sign.
The child died a few days later despite full intensive care
measures. (c) Extensive brain infarction (just 3 h after the
child was independently witnessed to be behaving normally).
The child died when intensive care measures were withdrawn
shortly after the scan was performed.
Fractures
this only applies to the appearances of discrete collections
of blood. If blood is mixed with other fluids, such as the
cerebrospinal fluid (CSF), then assessment of the age of
the blood based upon its scan appearances is not valid.
This is important in the context of head injury because if
the arachnoid membrane is damaged at the time of head
injury, CSF can leak into the subdural space and either
collect there or dilute any acute subdural blood that is
present.11,12 These mixtures of acute blood and CSF are
called acute traumatic effusions, and, when they occur,
they appear as subdural collections that are darker than
In general, the presence of a skull fracture is evidence
that there has been an impact injury to the head of
sufficient severity to lead to the fracture. The commonest type of skull fracture seen following an accidental or non-accidental impact head injury is a simple
linear parietal skull fracture. More complex fractures
such as those that are diastatic (widened) or depressed
are seen more commonly in the context of AHT,13 but
it does not follow that simple fractures are due to accidental mechanisms and more complex fractures nonaccidental; the appearance of the fracture is more likely
to depend on the degree of force causing it than whether
it was accidental or non-accidental.
4 of 9
Imaging 2014, 23, 20110067
The importance of neuroimaging in abusive head trauma
Figure 6. (a; iiii) CT scans showing uniformly low-attenuation subdural collections over both cerebral convexities due to acute
traumatic effusions. (b) MRI scan sequences from the same patient showing uniform signal collections on T1 (i) and T2 (ii), fluid
attenuation inversionrecovery (iii) and T2 gradient echo (iv) sequences.
The absolute degree of force required to produce
a skull fracture in infants and children is not known, and,
indeed, we do not know the true incidence of skull
fractures following impact head trauma in children, as
not all children who have sustained such injuries have
skull radiographs or scans. Everyday clinical experience
would, however, suggest that trivial head trauma is unlikely to lead to skull fractures.
It is not possible to assess the age of skull fractures
from their radiological appearances as can be done for rib
and limb fractures; skull bone is different and heals differently. If there is associated soft-tissue scalp swelling,
then it is likely that the causative event will have occurred relatively recently but, as soft-tissue scalp swelling
can take some time to develop (or be noticed) and a variable time to resolve, accurate assessment of the timing of
an injury by the appearance of soft-tissue swelling is inherently unreliable. It is also the case that, when softtissue bruising or marking is visible clinically, there may
not be any scalp swelling visible on scans, and the
converse is also true in that we do see cases where no
soft-tissue swelling is evident clinically but where diffuse
swelling is very obvious on scans. In terms of neuroradiological appearances, most soft-tissue scalp swelling
resolves within a 7- to 10-day period, unless there is
a significant deep component to the swelling.
Fractures are painful, and, so, it is likely that the child
would cry at the time of the causative event, but, in the
absence of any associated brain injury, there may not be
any other symptoms or signs until and unless any
bruising or soft-tissue scalp swelling becomes evident. It
follows that the finding of an unexplained fracture in
a non-mobile child is potentially of greater significance
than in a mobile child who may have sustained an
unwitnessed episode of head trauma.
Just as not all dark subdural fluid seen on CT scans
represents chronic subdural haematomas, not all lucencies seen on skull radiographs represent fractures, and it
is important to be aware of the differential of accessory
sutures or congenital fissures. These tend to be short
Table 1. Factors that may help distinguish acute traumatic effusions and chronic subdural haematomas
Acute traumatic effusions
Chronic subdural haematomas
Common
Uniform attenuation/signal
No differentiating size: may be large or small
Often enlarge on sequential early scans
Fairly uncommon in paediatrics
Areas of different attenuation/signal
No differentiating size
Usually do not change significantly in size unless
significant rebleed
Membrane formation (gives rise to loculation)
May be asymmetrical/symmetrical
No membrane formation/loculation
May be asymmetrical or symmetrical, right vs left
birpublications.org
5 of 9
N Stoodley and M Williams
Figure 8. (a) Frontal and (b) lateral skull radiographs
showing bilateral diastatic parietal skull fractures.
sustained such an injury will, when they have recovered
from their presenting encephalopathic illness, be discharged back into a potentially dangerous environment
and sustain further injury. Ultrasound has been used in the
context of detecting parenchymal shearing injuries16 in
known cases of AHT, but it has no role as a screening
examination.
CT technique
Figure 7. (a) CT and (b) MRI axial T2 and (c) coronal fluid
attenuation inversionrecovery sequences showing loculated
chronic subdural haematomas with loculated areas showing
fluid with different signal intensities.
linear lucencies perpendicular to the main sutures but
differentiation is not always clear.14,15
Imaging modalities
As in the imaging investigation of any other condition,
the various imaging modalities available to us have both
their strengths and limitations.
Plain radiographs
The skeletal survey remains an important investigation
in possible non-accidental injuries and skull radiographs
should form part of the skeletal survey even when a CT
scan of the head has been performed. Fractures that lie
along the plane of the scan sections can be missed on
standard CT (Figure 8).
CT is the initial imaging modality of choice, as it is
widely available and accessible, and once a child has been
stabilized following admission, it is relatively straightforward for them to be scanned. In general, acute subdural haematomas over the cerebral hemispheres are
easily visible on CT and, in the small number of cases
where larger space-occupying haematomas are present,
and require urgent neurosurgical intervention, these are
readily identified on CT. Subdural blood in certain sites
such as the posterior fossa and the subtemporal regions
may not be as well seen on CT, but it is unusual for
subdural blood to be found in such sites in the absence of
obvious subdural blood elsewhere.
CT is generally less sensitive in terms of detecting parenchymal brain injuries, either focal or the more generalized hypoxicischaemic brain injury present in many
AHT cases, but such changes are also often obvious on
early scans with features such as the reversal sign. The
hypoxicischaemic changes seen following episodes of
AHT often develop earlier and progress more rapidly
Cerebral ultrasound
Although a very portable imaging modality, the severe
limitations associated with its use in this context make it
inherently unreliable. As discussed above, the imaging
marker of a shaking injury is of thin-film subdural haemorrhages over the posterior aspect of the cerebral
hemispheres and in the posterior fossa, as well as often
over the lateral aspects of the cerebral hemispheres; all
places are not well visualized on ultrasound (Figure 9).
Because of this, a normal ultrasound may well be falsely
reassuring and, if no other imaging investigations are
performed, this could mean that a child who has
6 of 9
Figure 9. Ultrasound images illustrating the difficulties of
imaging small volume collections in the subdural space over
the lateral aspects of the cerebral hemispheres (a) and in the
posterior fossa (b).
Imaging 2014, 23, 20110067
The importance of neuroimaging in abusive head trauma
than in cases of hypoxicischaemic injury caused by nontraumatic events. It is also important to remember that,
especially in terms of the brain injury, the appearances at
the time of the scan are just that, a snapshot of what is
occurring at the time of the scan in an evolving pathological process. What we are looking at are static images
of a dynamic process and scans only a few hours apart
may look very different.
MRI technique
MRI has a very important role to play in the investigation of these cases both in the acute phase and in
the longer term. Given its multiplanar capability and the
ability to use different imaging sequences, it is well
recognized to be more sensitive than CT in the detection
of parenchymal brain injury of all types, at detecting
small volume subdural bleeds in sites not well seen on
CT and at detecting the small volume subarachnoid
haemorrhages that are very common in AHT (and are
the reason why, when lumbar punctures are performed
in these cases, it is very common to find uniformly
blood-stained CSF). Increasingly, MR investigations of
the spine are being performed at the same time as the
acute imaging of the head and spinal haemorrhage has
been reported in a significant proportion (approximately
5060%) of cases of AHT, most often in the lower thoracic and lumbar regions17,18 (Figure 10).
Given the accepted advantages of MRI over CT, including the fact that MRI does not involve the use of
ionizing radiation, why not just use MRI? There are
a number of reasons. Most units outside tertiary centres
do not have the capability to put sick infants with all the
requisite monitoring equipment into MRI scanners in any
event. Most radiologists in the district general hospital
setting (and many neuroradiologists without paediatric
expertise in teaching centres) would be uncomfortable
interpreting such scans, and it is easier to identify acute
blood on CT than on MRI: the early blood breakdown
products of oxy- and deoxyhaemoglobin can be very
subtle on MRI sequences, and it is not until methaemoglobin develops (which is bright on T1 weighted
scans) that blood becomes more obvious on MRI.
MRI also has a role in the longer term. As many of the
infants who sustain an episode of AHT are very young, it
Figure 10. Sagittal T1 (a) and T2 (b) weighted scans of the
whole spine showing high T1 and intermediate to low T2
signal blood posteriorly in the lumbosacral region.
birpublications.org
can be some time before the likely neurodevelopmental
outcome will become clear on clinical assessment.
Follow-up MRI scanning can give useful prognostic information by identifying areas of permanent structural
brain damage earlier, which may allow appropriate
support to be put in place earlier than would otherwise
have been the case.
A rational approach to the imaging
investigation of possible abusive head trauma
Over the past decade with increased awareness of the
nature of AHT and primarily with the more widespread
use of cross-sectional imaging techniques in head trauma
of various types, it has been possible to use a combination
of experience and published literature to formulate recommendations for the imaging investigation of various
aspects of non-accidental injuries, including AHT. A joint
working party of the Royal College of Radiologists,
London, UK, and the Royal College of Paediatrics and
Child Health, London, UK, published Standards for Radiological Investigations of Suspected Non-Accidental Injury
in 2008.19 The approach to neuroimaging recommended
in these guidelines has been subsequently validated by
the results of a systematic review performed by the
Welsh Child Protection Systematic Review Group,20
and other papers relevant to AHT from this group have
been published.21,22 This multidisciplinary group is
undertaking systematic reviews in many different aspects
of child abuse and summaries of the results are available at
www.core-info.cf.ac.uk.
Imaging
Initial CT scan
A CT scan of the head should be performed as soon as
is reasonably possible following stabilization of the
childs clinical condition if this has been necessary. This
should include the whole head from foramen magnum to
vertex with a slice thickness no greater than 5 mm.
Is there evidence of acute (bright) subdural blood? If
so, where? Look carefully at the posterior falx and in the
posterior fossa. Does the falx appear brighter than it
should and/or irregular or asymmetrical? If so, there is
probably acute blood lying adjacent to it. Is there any
acute blood over the frontal regions?
Look at the CSF in the ventricles and then at the extraaxial spaces over the cerebral convexities. Is there evidence of extra-axial fluid that is darker than the brain but
brighter than the CSF? If so, this is likely to be fluid in the
subdural space (and hence abnormal), but it may not be
possible to tell whether this darker fluid is chronic subdural or acute effusion. If you cannot tell, say that you
cannot and do not assume that all dark subdural fluid is
chronic subdural haematoma (see above).
Look at the brain itself. Are there any focal abnormalities such as parenchymal haematomas or contusions
or areas of focal low attenuation that might be due to
diffuse axonal injury? Look at the overall attenuation of
the brain and the greywhite differentiation. Although
there is less difference between grey matter and unmyelinated white matter in the infant brain than in the
7 of 9
N Stoodley and M Williams
brain of an older child or adult, there should still be clear
differentiation between the grey matter and the white
matter. Reduced attenuation in association with reduced
greywhite differentiation suggests the presence of a degree of hypoxicischaemic brain injury.
Look at the scan on bone windows. Is there evidence of
a fracture and/or of soft-tissue scalp swelling? Compare
the symmetry of the scalp soft tissues on each side and at
the front and back.
Having gone through this process and looked at the CT
images carefully, if the scan appears normal and the child
has no ongoing neurological abnormalities and there are
no other features of possible abusive injury (bruises,
burns, fractures on skeletal survey, blood in the CSF or
retinal haemorrhages), then no further cross-sectional
neuroimaging is required. If, however, the CT scan is
abnormal (or any of the above features are found) then
further imaging is mandatory and should comprise an
MRI scan of the brain and, in the authors view, the whole
spine.
abnormalities. Although MRI is more sensitive for the
detection of hypoxicischaemic injury, the changes can
still be subtle and, depending on when the scan is performed after the causative event, diffusion-weighted imaging is not always as helpful as might be thought.
Although MRI is not very useful in demonstrating bone
injury, any areas of soft-tissue swelling identified on CT
will need to be assessed on the MRI scan to see how they
have (or have not) changed.
The published evidence base on the topic of spinal MRI
in AHT is currently very limited (but is likely to increase
in the near future). On the basis of the published evidence
and current clinical experience, if the spine is imaged then
the whole spine should be scanned as the commonest site
for spinal haemorrhage in the context of AHT is in
the lumbosacral region.17,18 It follows that the whole
spine needs to be reviewed carefully for evidence of spinal
bleeding distant from any intracranial subdural bleeding.
Subsequent MRI scan in the acute phase
A skeletal survey should be performed as soon as is
reasonable. If further neuroimaging is required because
of ongoing clinical concerns about the childs neurological status, then the choice of whether to use CT or MRI
really depends on the clinical questions being asked but,
from a practical point of view, as long as the initial CT
and MRI scans have been performed according to the
guidelines then CT will normally suffice.
This scan should be performed within the first few
(35) days after admission and may require transfer of the
child to a regional centre. An example of a typical imaging protocol is given in Table 2.
Whilst MRI is more sensitive than CT, as discussed
above, the approach to identifying the abnormalities is
not fundamentally different from that set out above in
terms of the approach to the CT scan. In addition to going
through the same analysis, one also needs to consider
other issues for the MRI scan.
If there were areas of unequivocally bright blood on
CT, what do those collections of blood look like on T1 and
T2 weighted scans? This may allow an assessment of the
nature of the predominant blood breakdown products
present [e.g. intracellular methaemoglobin (bright on T1
and dark on T2) vs extracellular methaemoglobin (bright
on T1 and T2)]. If there were dark subdural collections
present on CT, what do those areas look like on MRI in
terms of signal on different sequences and have they
changed in size between the scans? Are they of uniform
signal throughout? Are the collections of different signal
in different areas and/or is there any evidence of membrane formation or loculation? This may help in the assessment of whether the collections are more likely to be
established chronic subdural effusions/haematomas or
acute traumatic effusions.
Look at the brain parenchyma in the same way as for
the CT scan for evidence of both focal and generalized
Table 2. Typical MRI scan protocols in non-accidental head
injury
Initial MRI scan sequences
Follow-up MRI sequences
Sagittal and axial T1
Axial T2
Coronal T2 FLAIR
Axial T2 gradient echo/SWI
Diffusion-weighted imaging
Sagittal T1 and T2 whole spine
Sagittal and axial T1
Axial T2
Coronal FLAIR
Axial T2 gradient echo/SWI
FLAIR, fluid attenuation inversionrecovery; SWI, susceptibilityweighted imaging.
8 of 9
Further imaging in the acute phase
Longer term follow-up
The imaging guidelines recommend that follow-up
MRI should be performed 36 months after the initial
injury primarily to give prognostic information as early
as possible as discussed above. The imaging protocol
does not need to be as extensive as on the initial scan and
a typical protocol is given in Table 2.
Conclusions
Unfortunately, AHT involving a shaking mechanism is
a common clinical problem with a potentially devastating
outcome for all concerned. Despite our inability to perform scientific studies of such events on infants, the more
widespread availability and use of cross-sectional imaging techniques together with observational studies in this
and other types of head trauma has led to a greater understanding of the condition. The population of infants
that we see following AHT is no longer limited to those
who are admitted with obvious external signs of abuse or
in whom skeletal surveys show the presence of occult
bone injury.
Radiologists need to play a full part in the multidisciplinary team dealing with these cases and that means (a)
recognizing the relevant abnormalities as discussed above
and (b) reporting those abnormalities in terms of the possibility of them being due to AHT so that an appropriate
multidisciplinary team investigation can occur. Raising the
possibility of AHT in terms of the differential diagnosis of
the imaging features overall is not the same as getting
embroiled in the forensic process should the case go to
court, but it might make the difference between a child
being discharged back into an abusive environment and
Imaging 2014, 23, 20110067
The importance of neuroimaging in abusive head trauma
a child who does not sustain a further, possibly fatal,
injury.
13.
Further reading
14.
This article has concentrated on the imaging aspects
of AHT. For discussion of some of the wider issues related to this topic, there are a number of good review
articles available.2326
15.
16.
References
1. Jayawant S, Rawlinson A, Gibbon F, Schulte S, Sharples P,
Sibert JR, et al. Subdural haemorrhages in infants: population based study. Br Med J 1998; 317: 155861.
2. Barlow KM, Minns RA. Annual incidence of shaken impact
syndrome in young children. Lancet 2000; 356: 15712. doi:
10.1016/S0140-6736(00)03130-5
3. Whitby EH, Griffiths PD, Rutter S, Smith MF, Sprigg A,
Ohadike P, et al. Frequency and natural history of subdural
haemorrhages in babies and relation to obstetric factors.
Lancet 2004; 363: 84651. doi: 10.1016/S0140-6736(04)15730-9
4. Rooks VJ, Eaton JP, Ruess L, Petermann GW, Keck-Wherley
J, Pedersen R. Prevalence and evolution of intracranial
hemorrhage in asymptomatic term infants. AJNR Am J
Neuroradiol 2008; 29: 10829. doi: 10.3174/ajnr.A1004
5. Barlow KM, Thomson E, Johnson D, Minns RA. Late neurologic and cognitive sequelae of inflicted traumatic brain
injury in infancy. Pediatrics 2005; 116: e17485. doi: 10.1542/
peds.2004-2739
6. Warrington SA, Wright CM. Accidents and resulting injuries in premobile infants: data from the ALSPAC Study.
Arch Dis Child 2001; 85: 1047.
7. Geddes JF, Hackshaw AK, Vowles GH, Nickols CD,
Whitwell HL. Neuropathology of inflicted head injury in
children. I. Patterns of brain damage. Brain 2001; 124: 12908.
8. Geddes JF, Vowles GH, Hackshaw AK, Nickols CD, Scott IS,
Whitwell HL. Neuropathology of inflicted head injury in
children. II. Microscopic brain injury in infants. Brain 2001;
124: 1299306.
9. Haviland J, Russell RI. Outcome after severe non-accidental
head injury. Arch Dis Child 1997; 77: 5047.
10. Ewing-Cobbs L, Kramer L, Prasad M, Canales DN, Louis PT,
Fletcher JM, et al. Neuroimaging, physical and developmental
findings after inflicted and noninflicted traumatic brain injury
in young children. Pediatrics 1998; 102: 3007.
11. Wells RG, Sty JR. Traumatic low attenuation subdural fluid
collections in children younger than 3 years. Arch Pediatr Adolesc Med 2003; 157: 100510. doi: 10.1001/archpedi.157.10.1005
12. Joy HM, Anscombe AM, Gawne-Cain ML. Blood stained,
acute subdural hygroma mimicking a subacute subdural
birpublications.org
17.
18.
19.
20.
21.
22.
23.
24.
25.
26.
haematoma in non-accidental head injury. Clin Radiol 2008;
62: 7036. doi: 10.1016/j.crad.2006.12.010
Hobbs CJ. Skull fracture and the diagnosis of abuse. Arch
Dis Child 1984; 59: 24652.
Sanchez T, Stewart D, Walvick M, Swischuk L. Skull fracture vs. accessory sutures: how can we tell the difference?
Emerg Radiol 2010; 17: 41318. doi: 10.1007/s10140-0100877-8
Weir P, Suttner NJ, Flynn P, McAuley D. Normal skull suture variant mimicking intentional injury. BMJ 2006; 332:
10201. doi: 10.1136/bmj.332.7548.1020
Jaspan T, Narborough G, Punt JA, Lowe J. Cerebral contusional tears as a marker of child abusedetection by cranial
sonography. Pediatr Radiol 1992; 22: 23745.
Koumellis P, McConachie NS, Jaspan T. Spinal subdural
hematomas in children with non accidental head injury.
Arch Dis Child 2009; 94: 21619. doi: 10.1136/adc.2008.
141671
Choudhary AK, Bradford RK, Dias MK, Moore GJ, Boal DK.
Spinal subdural hemorrhage in abusive head trauma: a retrospective study. Radiology 2012; 262: 21623. doi: 10.1148/
radiol.11102390
Royal College of Paediatrics and Child Health. Standards for
radiological investigations of suspected non-accidental injury.
London, UK: The Royal College of Radiologists and Royal
College of Paediatrics and Child Health; 2008.
Kemp AM, Rajaram S, Mann M, Tempest V, Farewell D,
Gawne-Cain ML, et al. What neuroimaging should be performed in children in whom inflicted brain injury (iBI) is
suspected? A systematic review. Clin Radiol 2009; 64: 47383.
doi: 10.1016/j.crad.2008.11.011
Kemp AM, Jaspan T, Griffiths J, Stoodley N, Mann MK,
Tempest V, et al. Neuroimaging: what neuroradiological
features distinguish abusive from non-abusive head
trauma? A systematic review. Arch Dis Child 2011; 96:
110312. doi: 10.1136/archdischild-2011-300630
Maguire S, Pickerd N, Farewell D, Mann M, Tempest V,
Kemp AM. Which clinical features distinguish inflicted from
non-inflicted brain injury? A systematic review. Arch Dis
Child 2009; 94: 8607. doi: 10.1136/adc.2008.150110
Minns RA, Busuttil A. Patterns of presentation of the shaken
baby syndrome: four types of inflicted brain injury predominate. Br Med J 2004; 328: 766. doi: 10.1136/bmj.328.
7442.766
Kemp AM. Investigating subdural haemorrhage in infants.
Arch Dis Child 2002; 86: 98102.
Jaspan T. Current controversies in interpretation of nonaccidental head injury. Pediatr Radiol 2008; 38(Suppl. 3):
S37887. doi: 10.1007/s00247-008-0896-8
Maguire SA, Kemp AM, Lumb RC, Farewell DM. Estimating
the probability of abusive head trauma: a pooled analysis.
Pediatrics 2011; 128: e550564. doi: 10.1542/peds.20102949
9 of 9
También podría gustarte
- Intra-Operative Neuropathology for the Non-Neuropathologist: A Case-Based ApproachDe EverandIntra-Operative Neuropathology for the Non-Neuropathologist: A Case-Based ApproachAún no hay calificaciones
- Help Pedsurgeryafrica30Documento10 páginasHelp Pedsurgeryafrica30Andi Firman MubarakAún no hay calificaciones
- BB Sacudido PDFDocumento62 páginasBB Sacudido PDFEvelynMenesesAún no hay calificaciones
- Stood Ley 2016Documento7 páginasStood Ley 2016Putri Rahmadhani Ngakpaniklage AsdsAún no hay calificaciones
- Diagnosis and Treatment of Traumatic Brain InjuryDocumento22 páginasDiagnosis and Treatment of Traumatic Brain InjuryAmandaAún no hay calificaciones
- Tec 2012Documento16 páginasTec 2012claugg123Aún no hay calificaciones
- Shaken Baby SyndromeDocumento25 páginasShaken Baby SyndromeArdanta Dat Topik TariganAún no hay calificaciones
- RCH DEM Head Injury GuidelinesDocumento4 páginasRCH DEM Head Injury GuidelinesJerry LeeAún no hay calificaciones
- Pediatric Head Injury 2013Documento16 páginasPediatric Head Injury 2013Salim Issa KhamashtaAún no hay calificaciones
- Intracranial Hemorrhage in Term Newborns: Management and OutcomesDocumento12 páginasIntracranial Hemorrhage in Term Newborns: Management and OutcomesNasibah Tuan YaacobAún no hay calificaciones
- Epidural Hematoma: Continuing Education ActivityDocumento16 páginasEpidural Hematoma: Continuing Education ActivityIka AriandanaAún no hay calificaciones
- Craniocerebral TraumaDocumento64 páginasCraniocerebral TraumaBentoys StreetAún no hay calificaciones
- Daniel D Price, MD Director of International Ultrasound, Department ofDocumento3 páginasDaniel D Price, MD Director of International Ultrasound, Department ofPutri Swandayani NofendyAún no hay calificaciones
- Clinical Features, Diagnosis, and Treatment of Neonatal EncephalopathyDocumento15 páginasClinical Features, Diagnosis, and Treatment of Neonatal EncephalopathyAlvaro SagredoAún no hay calificaciones
- Traumatic Brain Injury in KidsDocumento19 páginasTraumatic Brain Injury in KidsАлевтина ЛогиноваAún no hay calificaciones
- Author's Accepted Manuscript: Seminars in Ultrasound, CT, and MRIDocumento29 páginasAuthor's Accepted Manuscript: Seminars in Ultrasound, CT, and MRIasfwegereAún no hay calificaciones
- Clinics 5Documento19 páginasClinics 5Renju KuriakoseAún no hay calificaciones
- Strangulation Injuries - StatPearls - NCBI BookshelfDocumento8 páginasStrangulation Injuries - StatPearls - NCBI BookshelfSteven CraigAún no hay calificaciones
- Imaging Abusive Head Trauma: Why Use Both Computed Tomography and Magnetic Resonance Imaging?Documento15 páginasImaging Abusive Head Trauma: Why Use Both Computed Tomography and Magnetic Resonance Imaging?ariqAún no hay calificaciones
- Understanding Subdural Collections in Pediatric Abusive Head TraumaDocumento8 páginasUnderstanding Subdural Collections in Pediatric Abusive Head Traumapablo gonzalezAún no hay calificaciones
- Research Paper On Shaken Baby SyndromeDocumento8 páginasResearch Paper On Shaken Baby Syndromefys4gjmk100% (1)
- Management of Head TraumaDocumento15 páginasManagement of Head TraumaBetrice KotanAún no hay calificaciones
- Subdural Hematomas in The ElderlyDocumento19 páginasSubdural Hematomas in The ElderlyRegina PhilyriaAún no hay calificaciones
- HeadinjuryDocumento102 páginasHeadinjuryNinaAún no hay calificaciones
- Management Head Injury in ICUDocumento5 páginasManagement Head Injury in ICUIrma KusumaAún no hay calificaciones
- Jurnal SBSDocumento16 páginasJurnal SBSKiki PadeliaAún no hay calificaciones
- Head TraumaDocumento15 páginasHead TraumaDede Yusuf FAún no hay calificaciones
- The Shaken Baby SyndromeDocumento9 páginasThe Shaken Baby SyndromeDiana LoloiuAún no hay calificaciones
- 138975-Article Text-370968-1-10-20160708Documento5 páginas138975-Article Text-370968-1-10-20160708john smithAún no hay calificaciones
- Birth TraumaDocumento8 páginasBirth Traumaسحر احمدAún no hay calificaciones
- Maller2019 Neonatal Head Ultrasound Part 2Documento12 páginasMaller2019 Neonatal Head Ultrasound Part 2Modou NianeAún no hay calificaciones
- Pediatric Chest Trauma: A Unique ChallengeDocumento7 páginasPediatric Chest Trauma: A Unique ChallengeRolando Miranda PeñaAún no hay calificaciones
- Diagnosis and Initial Emergency Department Management of Subarachnoid HemorrhageDocumento13 páginasDiagnosis and Initial Emergency Department Management of Subarachnoid HemorrhageIngrid Paola Serrano MoralesAún no hay calificaciones
- Poster No.: Congress: Type: Authors: Keywords:: Page 1 of 20Documento22 páginasPoster No.: Congress: Type: Authors: Keywords:: Page 1 of 20adityaAún no hay calificaciones
- Biomedical Journal: SciencedirectDocumento11 páginasBiomedical Journal: SciencedirectTahir AlyasAún no hay calificaciones
- Hematoma SubduralDocumento27 páginasHematoma SubduralRoeder Max Pangramuyen100% (4)
- Epidural Hematoma Case ReportDocumento48 páginasEpidural Hematoma Case ReportJansept Bruce Guinto67% (6)
- Management of Mild and Moderate Head Injuries in Adults: Dana Turliuc, A. CucuDocumento11 páginasManagement of Mild and Moderate Head Injuries in Adults: Dana Turliuc, A. CucuSarrah Kusuma DewiAún no hay calificaciones
- A Subdural HematomaDocumento12 páginasA Subdural HematomaGina Irene IshakAún no hay calificaciones
- Management of Facial AsymmetryDocumento28 páginasManagement of Facial AsymmetrykrazeedoctorAún no hay calificaciones
- Overview of The Clinical Features and Diagnosis of Brain Tumors in AdultsDocumento37 páginasOverview of The Clinical Features and Diagnosis of Brain Tumors in AdultsFSHB-A&AAún no hay calificaciones
- Originally Published AsDocumento12 páginasOriginally Published AsEcaterina ChiriacAún no hay calificaciones
- Subdural HematomaDocumento8 páginasSubdural HematomaaaronmanullangAún no hay calificaciones
- Brain Tumor: BackgroundDocumento9 páginasBrain Tumor: Backgroundanak99Aún no hay calificaciones
- Utd 22823 Case - Reports DasDocumento5 páginasUtd 22823 Case - Reports DasVanny RosalinaAún no hay calificaciones
- Non Traumatic SDHDocumento11 páginasNon Traumatic SDHLuxein AkarAún no hay calificaciones
- Approach To HeadacheDocumento61 páginasApproach To Headachesabahat.husainAún no hay calificaciones
- Malak 2021Documento19 páginasMalak 2021Firmansyah FirmansyahAún no hay calificaciones
- CASE STUDY - CVA (Cerebrovascular Accident)Documento28 páginasCASE STUDY - CVA (Cerebrovascular Accident)'jmark FranciaAún no hay calificaciones
- Chesnut 2007Documento38 páginasChesnut 2007ALVARO ARIASAún no hay calificaciones
- Sumber 9Documento18 páginasSumber 9Ali Laksana SuryaAún no hay calificaciones
- Hess 2010Documento19 páginasHess 2010wiwiAún no hay calificaciones
- Stroke and PregnancyDocumento12 páginasStroke and PregnancyISMI NOVITA SARIAún no hay calificaciones
- Head Trauma PDFDocumento16 páginasHead Trauma PDFCharlene FernándezAún no hay calificaciones
- Brain AbscessDocumento13 páginasBrain Abscesskashim123Aún no hay calificaciones
- Readings About Cerebral Venous Sinus Thrombosis (CVST) (ER-RMPH)Documento8 páginasReadings About Cerebral Venous Sinus Thrombosis (CVST) (ER-RMPH)Raquel Beldia FuentesAún no hay calificaciones
- Tema 1. - Neurotrauma Aproximación Genral y Estrategias de ResuscitaciónDocumento17 páginasTema 1. - Neurotrauma Aproximación Genral y Estrategias de ResuscitaciónaniadAún no hay calificaciones
- Pathophysiology and Treatment of SevereDocumento13 páginasPathophysiology and Treatment of SevereIva Pinasti DestaraniAún no hay calificaciones
- A Subdural HematomaDocumento2 páginasA Subdural HematomaMohammadAwitAún no hay calificaciones
- New Microsoft PowerPoint PresentationDocumento1 páginaNew Microsoft PowerPoint PresentationIchiyoki IchsidaAún no hay calificaciones
- NTCM Ekg 1 DasarDocumento66 páginasNTCM Ekg 1 DasarEliharharianja100% (1)
- Test File FGHJKDocumento1 páginaTest File FGHJKIchiyoki IchsidaAún no hay calificaciones
- Test File FGHJKDocumento1 páginaTest File FGHJKIchiyoki IchsidaAún no hay calificaciones
- Test File FGHJKDocumento1 páginaTest File FGHJKIchiyoki IchsidaAún no hay calificaciones
- Test File FGHJKDocumento1 páginaTest File FGHJKIchiyoki IchsidaAún no hay calificaciones
- Test File FGHJKDocumento1 páginaTest File FGHJKIchiyoki IchsidaAún no hay calificaciones
- Oto SclerosisDocumento4 páginasOto SclerosisIchiyoki IchsidaAún no hay calificaciones
- Mual Muntah Pada KehamilanDocumento7 páginasMual Muntah Pada KehamilanIchiyoki IchsidaAún no hay calificaciones
- Template 0730Documento893 páginasTemplate 0730hadiAún no hay calificaciones
- Template 0608 Sky3dsDocumento868 páginasTemplate 0608 Sky3dsIchiyoki IchsidaAún no hay calificaciones
- Template 0730Documento893 páginasTemplate 0730hadiAún no hay calificaciones
- Gui 209 CPG 0807Documento8 páginasGui 209 CPG 0807Cendol_34Aún no hay calificaciones
- Hyperemesis GravidarumDocumento8 páginasHyperemesis GravidarumIchiyoki IchsidaAún no hay calificaciones
- Template 0522Documento858 páginasTemplate 0522Ichiyoki IchsidaAún no hay calificaciones
- Mual Muntah Pada KehamilanDocumento7 páginasMual Muntah Pada KehamilanIchiyoki IchsidaAún no hay calificaciones
- Mual Muntah Pada KehamilanDocumento7 páginasMual Muntah Pada KehamilanIchiyoki IchsidaAún no hay calificaciones
- Arteriovenous Malformation (Avm) Di Instalasi Radiologi Rsup DRDocumento5 páginasArteriovenous Malformation (Avm) Di Instalasi Radiologi Rsup DRyani radiologyAún no hay calificaciones
- Ultrasonix Sonixtouch User ManualDocumento308 páginasUltrasonix Sonixtouch User ManualManuel Vivero Diéguez100% (1)
- Medical Imaging Equipment Theory - Richard AstonDocumento145 páginasMedical Imaging Equipment Theory - Richard Astongennaro0% (1)
- Health Technology Assessment: Hailey DDocumento7 páginasHealth Technology Assessment: Hailey DPrisnmAún no hay calificaciones
- (Medical Radiology) Riccardo Lencioni MD, Marzio Perri MD, Dania Cioni MD (Auth.), Davide Caramella MD, Carlo Bartolozzi MD (Eds.)-3D Image Processing_ Techniques and Clinical Applications-Springer-VeDocumento327 páginas(Medical Radiology) Riccardo Lencioni MD, Marzio Perri MD, Dania Cioni MD (Auth.), Davide Caramella MD, Carlo Bartolozzi MD (Eds.)-3D Image Processing_ Techniques and Clinical Applications-Springer-VeNguyễn HùngAún no hay calificaciones
- GE Healthcare: Confirmation of Authorized DistributorshipDocumento1 páginaGE Healthcare: Confirmation of Authorized DistributorshipAsabila SafilaAún no hay calificaciones
- Report On Brain Tumour Detection ( Major)Documento77 páginasReport On Brain Tumour Detection ( Major)Himani Thakkar100% (1)
- CarcinogensDocumento47 páginasCarcinogensCedric Khalifa EdulianAún no hay calificaciones
- LI-RADS 2014 Comprehensive Imaging Diagnosis System For HCCDocumento7 páginasLI-RADS 2014 Comprehensive Imaging Diagnosis System For HCCRobert G. Gish, MD100% (1)
- MIT Case Performance at Quest DiagnosticsDocumento17 páginasMIT Case Performance at Quest DiagnosticsPrettygoodAún no hay calificaciones
- Basic Principles On NMR by KouridakisDocumento84 páginasBasic Principles On NMR by KouridakisErna WatiAún no hay calificaciones
- Balanced SARGE - Phase Balanced SARGEDocumento10 páginasBalanced SARGE - Phase Balanced SARGEwilton alves da silvaAún no hay calificaciones
- Optima CT520 BrochureDocumento24 páginasOptima CT520 BrochureCristina Catana-Buca0% (1)
- Testing Procedure UltrasoundDocumento6 páginasTesting Procedure UltrasoundMitecCenememAún no hay calificaciones
- Pulmovista 500 For Monitoring Ventilation in Critical Care PDF 2285965389402565Documento12 páginasPulmovista 500 For Monitoring Ventilation in Critical Care PDF 2285965389402565keperawatan rswnAún no hay calificaciones
- Guideline Karsinoma HepatoselulerDocumento11 páginasGuideline Karsinoma HepatoselulerMohammad Ihsan RifasantoAún no hay calificaciones
- Kazmi Pool SEQDocumento73 páginasKazmi Pool SEQAsif JamalAún no hay calificaciones
- HL Paper3Documento20 páginasHL Paper3Fake AccountAún no hay calificaciones
- Radiographs in Prosthodontics / Orthodontic Courses by Indian Dental AcademyDocumento38 páginasRadiographs in Prosthodontics / Orthodontic Courses by Indian Dental Academyindian dental academy100% (4)
- Principles of MLS 2 LECDocumento45 páginasPrinciples of MLS 2 LECSab ParkAún no hay calificaciones
- Clinical Investigation Cervix: y Z X K ( (Yy ZZ XX KK ( ( (Yyy ZZZ XXX XXXDocumento8 páginasClinical Investigation Cervix: y Z X K ( (Yy ZZ XX KK ( ( (Yyy ZZZ XXX XXXctuluAún no hay calificaciones
- Case Study On Software As A Service (SaaS) Based Emergency Healthcare in IndiaDocumento12 páginasCase Study On Software As A Service (SaaS) Based Emergency Healthcare in IndiaIcaro CameloAún no hay calificaciones
- A3 1 2Documento4 páginasA3 1 2meowAún no hay calificaciones
- Brain Tumours in EuropeDocumento11 páginasBrain Tumours in EuropeJosé Jorge Kessels DelgadoAún no hay calificaciones
- CP Key Image Note 2003-V3Documento14 páginasCP Key Image Note 2003-V3Charis LeungAún no hay calificaciones
- ESMO GuidelinesDocumento845 páginasESMO GuidelinesMohamed OsamaAún no hay calificaciones
- Dwnload Full Clinical Imaging With Skeletal Chest and Abdominal Pattern Differentials 3rd Edition Marchiori Test Bank PDFDocumento36 páginasDwnload Full Clinical Imaging With Skeletal Chest and Abdominal Pattern Differentials 3rd Edition Marchiori Test Bank PDFcharlesdrakejth100% (11)
- BHT TA RadiographyDocumento4 páginasBHT TA RadiographyhassaniAún no hay calificaciones
- American Philosophical SocietyDocumento14 páginasAmerican Philosophical SocietyCosmina TanaseAún no hay calificaciones
- Vaginal Foreign Body - Mohamad Radhi Bin Mohd Ariffin C 111 12 810Documento19 páginasVaginal Foreign Body - Mohamad Radhi Bin Mohd Ariffin C 111 12 810aliffikri52Aún no hay calificaciones