Documentos de Académico
Documentos de Profesional
Documentos de Cultura
PÇCX M, - LÑJKHGDFSZ PDF
Cargado por
Alejandra SaenzTítulo original
Derechos de autor
Formatos disponibles
Compartir este documento
Compartir o incrustar documentos
¿Le pareció útil este documento?
¿Este contenido es inapropiado?
Denunciar este documentoCopyright:
Formatos disponibles
PÇCX M, - LÑJKHGDFSZ PDF
Cargado por
Alejandra SaenzCopyright:
Formatos disponibles
06_05_JNS.
6/1/05
3:29 PM
Page 987
See the Editorial and the Response in this issue, pp 971973.
J Neurosurg 102:987997, 2005
Diagnosis and management of idiopathic normal-pressure
hydrocephalus: a prospective study in 151 patients
ANTHONY MARMAROU, PH.D., HAROLD F. YOUNG, M.D., GUNES A. AYGOK, M.D.,
SATOSHI SAWAUCHI, M.D., OSAMU TSUJI, M.D., TAKUJI YAMAMOTO, M.D.,
AND JANA DUNBAR, PH.D.
Department of Neurosurgery, Virginia Commonwealth University Medical Center, Richmond, Virginia
Object. The diagnosis and management of idiopathic normal-pressure hydrocephalus (NPH) remains controversial,
particularly in selecting patients for shunt insertion. The use of clinical criteria coupled with imaging studies has limited effectiveness in predicting shunt success. The goal of this prospective study was to assess the usefulness of clinical criteria together with brain imaging studies, resistance testing, and external lumbar drainage (ELD) of cerebrospinal
fluid (CSF) in determining which patients would most likely benefit from shunt surgery.
Methods. One hundred fifty-one patients considered at risk for idiopathic NPH were prospectively studied according to a fixed management protocol. The clinical criterion for idiopathic NPH included ventriculomegaly demonstrated on computerized tomography or magnetic resonance imaging studies combined with gait disturbance, incontinence,
and dementia. Subsequently, all patients with a clinical diagnosis of idiopathic NPH underwent a lumbar tap for the
measurement of CSF resistance. Following this procedure, patients were admitted to the hospital neurosurgical service
for a 3-day ELD of CSF. Video assessment of gait and neuropsychological testing was conducted before and after
drainage. A shunt procedure was then offered to patients who had experienced clinical improvement from ELD. Shunt
outcome was assessed at 1 year postsurgery.
Conclusions. Data in this report affirm that gait improvement immediately following ELD is the best prognostic
indicator of a positive shunt outcome, with an accuracy of prediction greater than 90%. Furthermore, bolus resistance
testing is useful as a prognostic tool, does not require hospitalization, can be performed in an outpatient setting, and
has an overall accuracy of 72% in predicting successful ELD outcome. Equally important is the finding that improvement with shunt surgery is independent of age up to the ninth decade of life in patients who improved on ELD.
KEY WORDS idiopathic normal-pressure hydrocephalus
normal-pressure hydrocephalus hydrocephalus
syndrome of idiopathic NPH was first introduced
by Hakim and Adams12 in 1965, who described a
unique triad of clinical symptoms including gait disturbance, dementia, and incontinence in patients with enlarged ventricles and occurring in the absence of raised ICP.
They introduced the term normal-pressure hydrocephalus
to describe this condition and reported that these symptoms
dramatically improved on shunt placement. Although there
has been significant progress in brain imaging and shunt
technology during the past 40 years, correctly diagnosing
the disease and selecting patients who would benefit from
shunt diversion remain problematic. Moreover, reported
shunt complications vary tremendously (1350%) among
institutions.3,13,16,17,22,25,27,30 As a result, several tests beyond an
assessment of clinical presentation have been proposed to
HE
Abbreviations used in this paper: CI = confidence interval;
CSF = cerebrospinal fluid; CT = computerized tomography; ELD =
external lumbar drainage; FHI = frontal horn index; ICP = intracranial pressure; MMSE = Mini-Mental State Examination; MR = magnetic resonance; NPH = normal-pressure hydrocephalus; PVI =
pressure volume index; SDH = subdural hematoma.
J. Neurosurg. / Volume 102 / June, 2005
identify so-called shunt responders to reduce risk. Such tests
have included cisternograms,29 tap tests,14,18,32,34 resistance
measures,4,5,7,24,28 ELD,11,32,35 and long-term recording of ICP
to identify B wave activity.5,23 Unfortunately, the accuracy
of these methods is difficult to assess because the patient
numbers were small and techniques varied among investigators.
Among these tests, however, resistance measures and
CSF drainage seemed to provide the most useful information; thus, in 1993 we embarked on a prospective study with
the main objective of improving our ability to diagnose
idiopathic NPH and to predict which patients would benefit
from shunt insertion. During the course of this study, we
noted that the number of patients with suspected idiopathic NPH increased yearly in an almost exponential fashion,
perhaps reflecting an aging population and a general trend
to perform surgery in patients in their seventh and eighth
decades of life. With increased numbers of patients supposed to suffer from NPH, it was possible to establish a
standard management protocol and evaluate the sensitivity
and specificity of resistance measures and ELD to identify
those patients who would improve following shunt surgery.
987
06_05_JNS.1
6/1/05
3:29 PM
Page 988
A. Marmarou, et al.
Clinical Material and Methods
One hundred fifty-one patients with a clinical diagnosis
of idiopathic NPH were treated at the Virginia Commonwealth University Medical Center between 1993 and 2003
according to a uniform protocol adopted in 1992 and carefully followed to the present. The clinical criterion for idiopathic NPH was ventriculomegaly demonstrated on CT or
MR imaging studies combined with gait disturbance, incontinence, and dementia. All patients properly consented to all
surgical procedures according to hospital regulations.
Management Protocol Summary
Patients at risk for idiopathic NPH were evaluated in an
outpatient clinic after being referred by a neurologist on service or from the surrounding community. After obtaining
the patients history and completing a physical examination,
CT or MR imaging data were examined and the patient consented to routine lumbar pressure measurement. When possible, spinal MR images were analyzed to exclude spinal
stenosis; in select cases, MR imaging studies were requested in patients with gait disturbance and reported lower-back
pain while walking.
In all cases, the symptoms of gait disturbance, dementia,
and incontinence with associated ventriculomegaly were
without antecedent cause, and idiopathic NPH was diagnosed on the basis of clinical evaluation. Subsequently, all
patients with idiopathic NPH underwent a lumbar tap to
measure CSF resistance. Following this procedure, all patients were admitted to the hospital neurosurgical service
for a 3-day ELD of CSF. A shunt procedure was then
offered to patients who had experienced clinical improvement from the ELD. As time progressed, the predictive
value of ELD was estimated and a shunt procedure was
offered to patients who had not experienced improvement
with drainage, following a careful explanation of risks and
the benefits. In many cases, these patients and their families
requested shunt surgery knowing that the probability of improvement was minimal.
check of the fluid lines to ensure that they were completely
filled, the opening pressure in the patient was recorded using simultaneously the pressure monitor and the computer
software, which provided an electronic stripchart of pressure that could be saved electronically.
Measurement of CSF Resistance
The resistance to CSF outflow was measured using the
bolus technique.20 After establishing a steady lumbar pressure, a 5-ml fluid sample was obtained for analysis. This
fluid was replaced by an equal amount of sterile saline to
return to the initial opening pressure. When the pressure stabilized, the stopcock was turned, opening the syringe to the
patient, and a 4-ml bolus of sterile saline was injected at a
rate of 1 ml/second. The stopcock was immediately closed
at the end of the injection, thereby opening the patients
pressure line to the gauge and the computer. The lumbar
pressure increased sharply and then gradually decreased
over time. The values for initial pressure, peak pressure, and
volume of injected fluid permitted calculation of the PVI
according to the following equation: Dvolume/log (Pp/Po),
where Dvolume is the volume of injected fluid (in millimeters), Pp the peak pressure (in millimeters of mercury), and
Po the initial pressure before injection (in millimeters of
mercury).
Similarly, outflow resistance (Ro) was calculated with
knowledge of the PVI, and a pressure was selected on the
return curve at 1, 1.5, and 2 minutes, according to the equation,12 Ro = t2Po/(PVIinjection) log [(P2/Pp)(Pp/Po)/P2 2 Po], where
PVI is computed as previously described, t2 the time (in seconds) when a pressure P2 is selected on the return curve, Po
the initial pressure before injection, and Pp the peak pressure
immediately after injection. The Ro values from each of
these time points were averaged to yield one Ro value for the
bolus. Subsequently, the bolus injection was repeated at
least three times and the Ro values for all three injections
were averaged to yield the final Ro value for the patient.
In the event of patient movement or disturbance, the ICP
waveform fluctuated and thus these measures were not used
in the calculation.
Lumbar Pressure Measurement and Resistance Testing
Lumbar pressure measurement was performed under
aseptic conditions in the outpatient clinic. Each patient was
asked to lie on his or her side on the examining table, and
following surgical preparation of the site and application of
a local analgesic, a 25-gauge needle was inserted percutaneously into the lumbar intrathecal space. Once we encountered CSF, the small length of tubing contained within the
lumbar puncture set was connected to a three-way stopcock.
On the second portion of the stopcock, a 20-ml syringe
filled with sterile saline was inserted. On the remaining end
of the stopcock, a 1-m length of intravenous extension tubing was connected to a conventional pressure gauge routinely used in our neurointensive care unit. The output of
the gauge was connected to a pressure recorder (Codman,
Raynham, MA), which provided a pressure waveform on
screen along with the averaged digital value of lumbar
pressure. The analog output of the pressure monitor was
connected to an analog/digital converter (Powerlab; ADI
Instruments, Colorado Springs, CO) and a computer for
the measurement of CSF outflow resistance. The pressure
system was then zeroed to atmosphere, and after a careful
988
External Lumbar Drainage
Following measurement of Ro, a patient was admitted to
the hospital for ELD usually within 2 weeks of the outpatient clinic visit. Each patient was asked to stop anticoagulant therapies 5 days prior to hospital admission. Shortly
after admission at the patients bedside, an external lumbar drain was placed under sterile conditions by using a
16-gauge Tuohy needle. A catheter was passed through the
needle, and the flow of CSF out the distal end of the catheter
was verified before connecting it to a sterile collection bag.
The patients bed was moved to the lowest position possible, and the bag was situated 5 or 10 cm below this level. In
a few cases, the bag was lowered below 10 cm to obtain
adequate CSF flow. The attending nurse was asked to open
the collection bag valve each hour, to drain 10 ml, and to
close the valve. No effort was made to maintain the drip at
a fixed rate, and once the bag valve was opened the 10-ml
CSF collection required only 3 to 5 minutes.
Cerebrospinal Fluid Collection
Each patient was asked to lie flat in bed during the 3-day
J. Neurosurg. / Volume 102 / June, 2005
06_05_JNS.1
6/1/05
3:29 PM
Page 989
Diagnosis and management of idiopathic NPH
drainage period and instructed to call the nurse when he or
she wished to get out of bed to use the toilet. In this way, we
could ensure that the valve was closed to drainage when the
patient was upright. The nurse monitored the amount of
fluid collected per hour on a separate form, which was later
placed in the medical record. On the 2nd and 3rd days of
drainage, the patient was permitted to have meals while sitting in a chair for approximately 30 minutes.
Ambulation Before and After ELD
On the day of the clinic visit, each patient was videotaped
while rising from a chair and walking at a normal pace
along a corridor for a distance of 10 m. The patient was then
asked to turn and return to the chair. When approximately
halfway, the patient was asked to tandem walk for approximately five steps. Thereafter, the patient was asked to walk
to the chair, turn, and sit. The video was then analyzed by
an independent observer, who classified the type of walk
(for example, shuffling, or wide based gait), the ability to
tandem walk (easy, difficult, or impossible), and the difficulty involved in rising from the chair (easy, difficult,
or impossible). The steps per minute were calculated from
an offline analysis of the videotape and entered into the
patients record. Additionally, gait was rated as normal;
mildly impaired, unsteady but unassisted walking possible;
moderately impaired, inability to walk without assistance;
or severely impaired, inability to walk even with assistance.
A second video was obtained once the drain was removed
following lumbar drainage.
Mental disturbances were evaluated using the MMSE10
and a series of neuropsychological tests2,26 including the
Galveston Orientation and Amnesia Test, Controlled Oral
Word Association Test,6 and Benton Visual Retention Test
Revised.1 Digit Span Forward and Backward tasks were
used to test attention and concentration.21 The Wechsler
Memory ScaleRevised Logical Memory Test33 was administered to assess auditory memory. The Rey Auditory Verbal Learning Test24 was administered as a measure of verbal
acquisition skills.
Memory impairment was characterized as normal; mildly impaired, testing required to demonstrate deficit; moderately impaired, difficulty noted by physician support staff
or family; or severely impaired, disoriented but delirium excluded.
Bladder function was assessed and described as normal if
there was no urgency, increased frequency, or incontinence.
Impairment in urinary function was categorized as mild if
the patient experienced increased urinary urgency; moderate if the patient had stress, urge, or overflow incontinence;
and severe if the patient experienced any of the severe
forms of incontinence or total incontinence.
Ventriculomegaly was determined based on an Evans
Index9 equal to or greater than 0.30 or an FHI of 0.4. Note
that the FHI is defined as the maximal width of the frontal
horns at their extreme and the brain width along the same
axis. The Evans Index is defined as the maximal width of
the frontal horns measured at their extreme to the maximal
biparietal diameter.
Prior to Discharge
Prior to drain removal, CSF pressure was measured by
connecting the extension tubing to a strain gauge and presJ. Neurosurg. / Volume 102 / June, 2005
sure monitor (Codman). After the pressure was measured,
the drain was removed and a CT scan was obtained to
ensure that drainage had not resulted in a hygroma or SDH.
When the CT scan was cleared by the attending physician,
the patient and caregiver were given instructions to complete 10-day surveys in which they were asked to grade
the patients daily status as improved, same, or worse. The
patient was then scheduled to appear at the next clinic to
discuss clinical recommendations with regard to shunt
placement.
Statistical Analysis
For continuous data, two-sided t-tests were applied. For
categorical data, two-sided chi-square or exact tests were
applied. A level of 0.05 was considered significant. Values
are represented as the means 6 standard deviations.
Results
General Response to ELD Protocol
The patients tolerated the infusion study, which was usually conducted in the outpatient clinic, and the subsequent
in-hospital ELD protocols. The nursing staff had no difficulty in obtaining the required volume of CSF per hour. On
four occasions, the lumbar catheter was removed accidentally by the patient. When removal occurred early in the
drainage cycle, the drain was replaced. When it occurred after a reasonable volume of CSF had been collected (. 300
ml), the drain was removed and the patient discharged once
we had performed a postdrainage CT study, MMSE, and
video.
Patient Age and Sex Distribution
The mean age of men was 74.6 years (range 5989 years)
and that of women was 75.2 years (range 6185 years). The
sex distribution was almost equal: 74 men and 77 women.
In general, the older patients were in reasonably good
health, although there was significant comorbidity.
Opening Pressure and PVI
The lumbar pressure measured using a conventional
strain gauge transducer varied extensively; pressures as low
as 2 mm Hg and as high as 20 mm Hg were observed. The
mean pressure in all patients equaled 9.4 6 4.6 mm Hg.
The distribution of opening pressures is depicted in Fig. 1.
Given that the infusion study required only 20 minutes or
less of recording, B wave activity was observed in relatively few patients during this short interval. Pulsatile pressures
also varied based on the PVI and initial pressure level and
were inconsistent among patients. Both respiratory and cardiac components were present in all recordings. There was
no significant difference in opening pressure between patients who did (9.4 6 4.6 mm Hg) and those who did not
improve (10 6 4 mm Hg) on ELD. Likewise, there was no
significant difference in PVI between patients who experienced improvement and those who did not following ELD.
Patient Symptoms and ELD Outcome
Among the cohort of 151 patients, 100 (66.2%) improved
after ELD. It was interesting to compare the number and
type of symptoms seen on initial presentation with patient
989
06_05_JNS.1
6/1/05
3:29 PM
Page 990
A. Marmarou, et al.
TABLE 2
Types of gait disturbance seen in 120 patients
with idiopathic NPH
No. of Patients (%)
Type of Gait
Disturbance
FIG. 1. Bar graph demonstrating opening pressures measured
electronically in 151 patients with idiopathic NPH during lumbar
infusion studies. Pressure was allowed to stabilize for 30 seconds
before taking a reading. The median pressure was 9 mm Hg. N =
number of patients.
outcome following ELD. Among the 100 patients whose
condition improved postdrainage, the greatest improvement
was associated with patients who had not presented with the
complete triad of impaired gait, incontinence, and dementia.
Of 86 patients with the complete triad, only 59.3% improved compared with improvements of 88.2 and 83.9% in
patients with an impaired gait only and an impaired gait
plus dementia, respectively. Other patient groups were too
small to draw any firm conclusions (Table 1). Based on
these data, however, patients with symptoms of a disturbed
gait alone and those with an impaired gait plus dementia or
incontinence have significantly better outcomes after ELD
compared with patients who present with the complete triad
(chi-square test, p , 0.0006).
As stated previously, patients with an impaired gait
alone or in combination with any other symptomhad a
significantly better outcome after ELD compared with patients who did not have gait disturbance (chi-square test,
p , 0.005). Note that most patients with idiopathic NPH
had more than one type of gait difficulty (Table 2). Most
patients presented with difficulty in tandem walking and
balance, although no specific type of gait disturbance was
predictive of ELD outcome.
In addition to performing a clinical evaluation of gait improvement, we documented the steps per minute before and
after ELD as well as the number of steps used in turning
TABLE 1
Comparison of symptoms on initial presentation and ELD
outcome in 151 patients with idiopathic NPH
shuffling
magnetic gait
wide-based gait
difficulty in rising from chair
difficulty in
turning
imbalance
difficulty in
tandem walking
w/ Gait Deficit*
Improvement
After ELD
No Improvement
After ELD
47 (39)
20 (17)
52 (43)
40 (33)
36 (77)
17 (85)
40 (77)
26 (65)
11 (23)
3 (15)
12 (23)
14 (35)
58 (48)
42 (72)
16 (28)
102 (85)
112 (93)
67 (66)
80 (71)
35 (34)
32 (29)
* Gait assessment was conducted in 120 of 151 patients; 18 patients were
wheelchair bound and the remaining 13 patients did not have gait disturbance. Percentages in this column were based on the assessment of 120
patients.
180. Before ELD, the mean number of steps per minute
was 80 6 12 (55 patients); after ELD, the mean number of
steps per minute was unchanged at 79 6 12. The mean
number of turning steps before ELD was 5.6 6 2.8; after
ELD and prior to discharge, the mean number of turning
steps reduced to 4.4 6 2.3. This reduction in turning steps
was statistically significant (p = 0.004).
Severity of Symptoms and ELD Outcome
Among patients whose symptoms improved following
ELD, the response to drainage correlated with the severity
of symptoms demonstrated on initial clinical presentation
(Fig. 2). For example, patients enduring mild and moderate
gait disturbance experienced significant improvement after
drainage compared with those suffering from severe gait
disturbance (p = 0.0016). Similarly, patients subject to mild
or moderate memory loss experienced significant improvement compared with those subject to severe memory loss
(p = 0.0064). Finally, patients initially demonstrating mild
symptoms of incontinence experienced significant improvement compared with those exhibiting moderate and
severe symptoms (p = 0.016).
Effect of ELD on Neuropsychological Performance
We found no difference between neuropsychometric parameters assessed post-ELD and baseline levels (Fig. 3).
Only one testdelayed auditory memoryshowed significance (p , 0.05). Note, however, that this finding could
have been observed by chance considering the number of
tests administered.
No. of Patients (%)
Symptoms on Admission
No. of
Patients
Improvement
No Improvement
total no. of patients
triad*
impaired gait only
impaired gait & incontinence
impaired gait & dementia
incontinence & dementia
151
86
17
4
31
13
100 (66.2)
51 (59.3)
15 (88.2)
4 (100)
26 (83.9)
4 (30.7)
51 (33.8)
35 (40.7)
2 (11.8)
0 (0)
5 (16.1)
9 (69.3)
* Refers to impaired gait, incontinence, and dementia.
990
Correlation of CSF Resistance and ELD Outcome
The ELD outcome was compared with CSF outflow
resistance (Ro) values less than and greater than or equal to
4 mm Hg/ml/min. Of 44 patients with an Ro less than 4 mm
Hg/ml/min, 20 patients (45.5%) experienced improvement
and 24 (54.5%) did not. This difference was not significant.
Of 78 patients with an Ro greater than 4 mm Hg/ml/min, 64
patients (82%) improved with ELD and 14 (18%) did not.
J. Neurosurg. / Volume 102 / June, 2005
06_05_JNS.1
6/1/05
3:29 PM
Page 991
Diagnosis and management of idiopathic NPH
TABLE 3
Shunt outcome compared with ELD outcome
in patients with idiopathic NPH
No. of Patients (%)
total no. of patients
shunt surgery
improvement w/
shunt surgery
no improvement
w/ shunt surgery
Improvement
From ELD
No Improvement
From ELD
100 (66.2)
84/100 (84.0)
76/84 (90.5)*
51 (33.8)
18/51 (35.0)
4/18 (22.2)
8/84 (9.5)
14/18 (77.7)
* p , 0.0001, compared with patients who did not improve on ELD.
This difference was highly significant (p , 0.0001). Based
on these data, the ability of an Ro value greater than or equal
to 4 mm Hg/ml/min to predict ELD outcome has a sensitivity of 0.75 (95% CI 0.670.84), specificity of 0.63 (95%
CI 0.480.78), positive predictive value of 0.82 (95% CI
0.750.89), and a negative predictive value of 0.53 (95% CI
0.440.62) and is associated with an overall accuracy of
0.72 (95% CI 0.650.79). An example of the ICP course in
a patient with a high Ro ($ 4 mm Hg/ml/min) and another
with a low Ro (, 4 mm Hg/ml/min) is shown in Fig. 4. Because not all patients underwent shunt insertion, it was not
possible to calculate the sensitivity of Ro to predict shunt
outcome.
Correlation of ELD With Shunt Outcome
FIG. 2. Bar graphs demonstrating the percentage of patients
whose condition improved following ELD. Upper: Patients were
classified according to the severity of gait disturbance. Although all
patients shown experienced improvement, proportionally fewer
patients with a severe gait disturbance improved after ELD. *p =
0.016, rank sum test. Center: Patients were classified according to
the severity of dementia. Although all patients shown experienced
improvement with ELD, those with mild or moderate memory loss
had a greater tendency to improve with drainage compared with
those patients with severe memory disturbance. **p = 0.006, rank
sum test. Lower: A greater number of patients who had mild or
moderate (mod) urinary incontinence on presentation demonstrated
improvement following ELD compared with patients with severe
incontinence. *p = 0.033, rank sum test).
J. Neurosurg. / Volume 102 / June, 2005
Of the 100 patients who had experienced improvement
post-ELD, 84 underwent shunt surgery; 76 (90.5%) of these
84 patients improved following shunt insertion. After
explaining to patients whose condition did not improve on
ELD (51 patients) that the probability of benefiting from
shunt placement was low, 18 elected to undergo surgery.
Four of these 18 patients experienced improvement, whereas 14 did not experience improvement 3 and 6 months and
1 year after shunt surgery. Of the four patients whose condition improved, three demonstrated mild improvement in
gait, which was sustained for at least 1 year; the remaining
patient had mild improvement in gait and incontinence,
which was transient and not sustained at the 1-year follow
up. The number of patients who improved on ELD and after
shunt surgery compared with those who did not was statistically significant (p , 0.0001; Table 3). Based on these
data, the use of ELD in predicting shunt outcome has a sensitivity of 0.95 (95% CI 0.840.90), specificity of 0.64
(95% CI 0.440.84), positive predictive value of 0.90 (95%
CI 0.721.00), negative predictive value of 0.78 (95% CI
0.700.80), and accuracy of 0.88 (95% CI 0.830.93).
Influence of Patient Age on ELD Outcome
The mean age in the 151 patients equaled 74.9 years
(range 5989 years. We questioned whether there was an
age beyond which ELD would cease to be an effective
prognostic indicator and/or a percentage of patients with a
positive ELD outcome that would not be reflected in an improved shunt outcome. Several interesting answers were
found. First, patients with an age younger than 75 years had
991
06_05_JNS.1
6/1/05
3:29 PM
Page 992
A. Marmarou, et al.
FIG. 3. Bar graph demonstrating neuropsychological profiles in patients suffering from idiopathic NPH whose condition improved compared with profiles in patients whose condition did not improve on ELD. Neuropsychological testing
was performed before and immediately after removing the drain. Although most patients who improved on ELD seemed
more responsive, more verbal, and more eager to engage in conversation during clinical rounds, this positive effect was
not captured in the neuropsychological tests performed immediately postdrainage.
a higher rate of improvement on ELD (78%) compared with
patients 75 years or older (57%; Table 4). This result was
highly significant (p , 0.007 chi-square), indicating that
proportionally fewer patients older than 75 years would
likely improve on shunt surgery compared with those younger than 75 years. Second, improvement on ELD in patients
younger than 75 years of age who presented with the symptom triad was significantly higher (81%) than that in patients 75 years or older (40%; p , 0.005), indicating that
patients 75 years or older with the symptom triad were less
likely to improve on shunt surgery. Interestingly, in patients
without the triad, ELD outcome was independent of age,
thus indicating that patients were more likely to improve on
TABLE 4
Influence of patient age on outcome
No. of Patients
w/ ELD (%)
Variable
age ,75 yrs
age $75 yrs
age ,75 yrs &
symptom triad
age ,75 yrs &
1 or 2
symptoms
age $75 yrs &
symptom triad
age $75 yrs &
1 or 2
symptoms
No. of Patients
w/ Shunt Placement (%)
Improvement
No Improvement
Improvement
No Improvement
52 (78)*
47 (57)
30 (81)
15 (22)
36 (43)
7 (19)
45 (94)
39 (95)
26 (96)
3 (6)
2 (5)
1 (4)
22 (73)
8 (27)
10 (90)
2 (10)
20 (40)
29 (60)
18 (95)
1 (5)
7 (79)
7 (21)
21 (95)
1 (5)
* p , 0.01, compared with ELD outcomes in patients 75 years or older.
p , 0.005, compared with ELD outcomes in patients 75 years or older
with the complete symptom triad.
992
shunt placement during the intermediate course of NPH and
prior to reaching the stage at which all three symptoms were
present.
Influence of Age on Shunt Outcome
It is conceivable that the elderly patient may improve following short-term drainage (ELD) and yet not improve after
long-term drainage. We explored this idea by comparing
shunt outcome as a function of age (Table 4). The greater
portion of patients who underwent shunt placement had
been evaluated following ELD. Thus, the influence of age
on shunt outcome also referred to patients who improved on
ELD. In those who improved on ELD, there was no difference in shunt outcome in patients younger than or those 75
years of age or older. Improvement on shunt insertion was
90% or greater. Similarly, there was no significant difference in shunt outcome as a function of age in patients with
the complete symptom triad or disturbed gait plus incontinence or dementia. In summary, if the patient improved on
ELD, there was a greater than 90% probability of improving on shunt placement that was independent of age.
Brain Tissue Response to Shunt Placement in the
Elderly Patient
In patients whose condition improved, we occasionally
observed a reduction in ventricle size, which could be easily demonstrated on CT studies or on remarkable recovery of
brain tissue after shunt insertion. Example imaging studies
from a 78-year-old patient with such a remarkable recovery
11 months after shunt placement are shown in Fig. 5. We
analyzed the FHI in patients (27) whose condition had improved after drainage and shunt placement, and who had
follow-up CT studies from within 6 months to 1 year of
surgery. The FHI in this patient group before surgery
equaled 0.46 6 0.04. The FHI measured at the follow up
was 0.40 6 0.05. The reduction in ventricle size among
J. Neurosurg. / Volume 102 / June, 2005
06_05_JNS.1
6/1/05
3:29 PM
Page 993
Diagnosis and management of idiopathic NPH
FIG. 5. Magnetic resonance images (upper) obtained prior to
shunt placement compared with CT scans (lower) obtained 1 year
after shunt surgery in a 78-year-old woman with idiopathic NPH.
The patient, initially wheelchair bound, experienced a remarkable
improvement following ELD and subsequent placement of a ventriculoatrial (V-A) shunt with a programmable valve. In most patients, the improvement following shunt insertion did not always
correlate with a reduction in ventricle size. Nevertheless, this case
demonstrates the potential for tissue reconstitution in the elderly
brain.
ELD gave greater assurance to patients with a positive ELD
outcome that shunt surgery would be worthwhile.
FIG. 4. Graphs demonstrating examples of lumbar pressure response to bolus injections (4 ml) for the measurement of CSF outflow resistance. Upper: Pressure increased rapidly and then gradually returned to baseline values. This rate of recovery was typical
for patients whose Ro was less than 4 mm Hg/ml/min. Lower: Repeated bolus injections (two) did not induce a rapid recovery of
pressure. The Ro in this patient measured 6.7 mm Hg/ml/min and
was typical for patients with Ro values greater than or equal to 4 mm
Hg/ml/min. This Ro analysis performed in an outpatient setting has
a sensitivity of 0.75 for predicting the outcome of an ELD performed in the hospital.
Patient Complications
The complications associated with lumbar pressure measurements and infusion tests were minimal and consisted of
mild to moderate headache (12 [8%] of 151), which usual-
patients who improved was statistically significant (p ,
0.001). The number of patients who did not improve after
ELD and shunt placement together with a follow up between 6 months and 1 year was small (six patients). Among
this group, the FHI prior to surgery equaled 0.45 6 0.04; at
follow up, the FHI equaled 0.45 6 0.05 and there was no
reduction in ventricle size. Of equal importance is the observation of no reduction in FHI before and after 3-day drainage despite the improvement in NPH symptoms.
Response to Survey Following Discharge
Most patients eagerly returned the survey at the follow up
in the clinic to discuss the next step in treatment. Patients
who improved following ELD reported a marked improvement in their symptoms immediately after discharge followed by a gradual return to baseline levels over a 10-day
period (Fig. 6). This patient and caregiver survey was consistent. The self-evaluation by patients who believed that
they did not improve after ELD agreed with the clinical assessment. Allowing the family to document the outcome of
J. Neurosurg. / Volume 102 / June, 2005
FIG. 6. On discharge, patients and caregivers completed surveys
on their daily responses to ELD (rated as better, same, or worse
compared with predrainage symptoms). This graph depicts the assessments in patients who improved on ELD compared with those
who did not improve. Patients who experienced improvement on
ELD (circles) did so markedly immediately after discharge while in
the home setting. This effect gradually decreased toward baseline
levels over a 10-day period. In contrast, patients who did not improve (squares) remained symptomatic despite the mean 500 ml
CSF drained. This survey was invaluable in assessing the risk/benefit ratio for surgical intervention.
993
06_05_JNS.1
6/1/05
3:29 PM
Page 994
A. Marmarou, et al.
TABLE 5
Shunt complications in patients with idiopathic NPH
No. of Cases
Complication (rate)
major (9.8%)
infection
SDH
hygroma
sinus thrombosis
minor (13.7%)
headache
hearing loss
double vision
Total
Complete Recovery
Partial Recovery
3
3
3
1
3
1
1
0
0
2
2
1
5
5
4
4
4
4
1
1
0
ly resolved within 12 hours. The only serious complication
associated with ELD was infection, which occurred in two
(1.3%) of 151 patients. Another four patients (2.6%) suffered headache, which resolved within 1 to 3 days. There
were 9.8% major complications associated with shunts (Table 5), including SDH (three [3%] of 102), hygroma (three
[3%] of 102), infection (three [3%] of 102), and sinus
thrombosis (one [0.98%] of 102). There were 13.7% minor
complications, including headache (five [5%] of 102), hearing problems (five [5%] of 102), and double vision (four
[4%] of 102). The rate of recovery from these complications
is shown in Table 5.
Discussion
Idiopathic NPH is readily diagnosed based on a patients
clinical presentation and brain imaging studies. Nonetheless, determining which patient will benefit from shunt
placement is more problematic. Data in the present study
affirm that improvement in gait immediately following
ELD is the best prognostic indicator of a positive shunt outcome, with a prediction accuracy greater than 90%. We also
found that bolus resistance testing is useful as a prognostic
tool that does not require hospitalization, can be performed
in an outpatient setting, and has an overall accuracy of 72%.
Equally important is the finding that improvement with
shunt insertion is independent of age up to the ninth decade
of life in patients who had improved on ELD.
Classification of NPH
In the first report of NPH in 1965, Hakim and Adams12
discussed the outcome of three patients, only one of whom
was considered to have idiopathic NPH. This patient improved on shunt placement, and as a result a new treatment
was introduced, alleviating symptoms of gait disturbance,
incontinence, and dementia. Note, however, that the treatment of any patient with NPH during the next 40 years became controversial, because the outcome in many with socalled NPH was less than favorable. This result was due in
part to the treatment of both idiopathic and secondary NPH
as a single entity, although it became clear over time that the
two must be separated. The concept of primary (idiopathic) and secondary (all known causes) NPH was introduced
by Black,3 and it was this differentiation that allowed the
specific problems associated with idiopathic NPH to be addressed. First, the disease diagnosis was confounded by
994
the notion that if the patient at risk for NPH improved on
shunt placement, the diagnosis was accurate and indeed
the patient had NPH. In this report, however, we posited
that idiopathic NPH may have progressed to a stage at
which the patient may be refractory to treatment. With this
view, there must be a clear separation between diagnostic
criteria based on clinical presentation and those based on
surgical outcome.
Opening Pressure in Idiopathic NPH
Based on Ekstedts8 study in 100 patients, normal pressure varies over a relatively narrow range of 8.6 to 13.1 mm
Hg, with a mean pressure of 10.4 6 1.43 mm Hg. In contrast, the ICP distribution observed in the present study in
patients with idiopathic NPH extended over a much wider
range of 2 to 20 mm Hg, with a mean pressure of 9.4 6 4.6
mm Hg. Given the relatively large number of patients in this
study, it was reasonable to extend the range of so-called normal pressure in idiopathic NPH to an upper limit of at least
18 mm Hg based on two standard deviations from the mean.
What factors account for the higher pressure level? Considering the equation for steady-state ICP, one would expect
the higher opening pressures to be associated with higher
CSF resistance values, although such was not the case. Using the estimated rate of normal CSF formation of 0.35 ml/
minute, an increase in CSF resistance from 2 to 10 mm Hg/
ml/min, a fivefold increase, would result in an ICP increase
from only 10 to 12.8 mm Hg. Thus, the opening pressure in
patients with idiopathic NPH is an insensitive indicator of
CSF resistance. We posit that the ICP levels associated with
idiopathic NPH are more a function of venous pressure than
CSF resistance. Additional studies are necessary to clarify
this issue, however.
Shunt-Responsive NPH
In the study by Vanneste and colleagues,31 patients predicted to be shunt-responsive based on clinical and CT criteria had an overall improvement of 58% after shunt insertion. Data from other studies have shown that favorable
responses to shunt placement based on clinical criteria alone
ranges from 27 to 53%.8,31 In our view, the accuracy of prediction must be much higher than that achieved using clinical and imaging criteria, especially in the elderly population, which has both NPH symptoms and significant
comorbidity. If all patients in our study had undergone shunt
insertion based on clinical and CT criteria, we would have
achieved an improvement rate of only 66% (100 of 151
cases). This rate is slightly higher than the improvement
rates reported in earlier studies.8,31 The results of using ELD
to predict shunt responsiveness increased our predictive accuracy to 88%. Williams, et al.,35 studied 86 patients with
NPH by using controlled lumbar drainage; however, the
number of patients with idiopathic NPH was not specified.
Nevertheless, among the 47 patients who underwent shunt
surgery, the sensitivity of ELD was 97% and specificity was
60%results very close to those in our study of ELD (95%
sensitivity and 64% specificity).
Value of CSF Resistance Testing
All patients entered into the present study underwent both
CSF testing and ELD, and as a result we had a unique
opportunity to evaluate the sensitivity of CSF resistance
J. Neurosurg. / Volume 102 / June, 2005
06_05_JNS.1
6/1/05
3:29 PM
Page 995
Diagnosis and management of idiopathic NPH
testing in predicting ELD outcome. This opportunity was
important because Ro can be measured in an outpatient setting and could possibly eliminate hospitalization for ELD.
We found that patients with an Ro greater than 4 mm Hg/ml/min are most likely to have a positive ELD response
(p , 0.0001). This value is slightly lower than the 6 mm
Hg/ml/min used in posttraumatic hydrocephalus in an earlier study.19 With regard to predicting ELD outcome, bolus Ro
had a positive predictive value of 82% and a sensitivity of
75%. The overall accuracy of Ro in predicting ELD outcome equaled 72%. We believe that Ro testing is a valuable
supplementary test that increases the predictive accuracy of
potential shunt responders beyond that of clinical criteria
alone. The fact that we tended to place shunts in only those
patients who improved on ELD prevented us from evaluating the accuracy of resistance testing to predict shunt outcome directly.
Several methods can be used to determine CSF resistance,5,7,15,18,20 and the absolute value of Ro varies with the
method used. For this reason, it has been difficult to compare the results of other studies. For example, Malm, et al.,18
prospectively evaluated the predictive value of Ro by using
a modification of the pressure technique. They reported that
the CSF resistance in the group of 35 patients with idiopathic NPH was high, measuring 8.2 mm Hg/ml/min. Nonetheless, these authors concluded that resistance testing could
not predict the outcome of gait or neuropsychological indices. In contrast, Takeuchi, et al.,28 used the bolus method
to predict outcome in 25 patients who had undergone shunt
surgery and reported a sensitivity and specificity of 100 and
92%, respectively. These authors used an epidural monitor,
and the mean Ro value in patients improving after surgery
equaled 35 mm Hg/ml/min. The study published by Boon,
et al.,4 reported results in 101 patients with the objective
of predicting shunt outcome based on CSF resistance. The
study included a mixture of primary and secondary NPH,
although most of the patients had idiopathic NPH. Using
the constant-flow technique for the measurement of Ro, they
found that Ro values correlated with primary outcome measures by using linear regression methods and recommended
18 mm Hg/ml/min as the threshold for shunt insertion. At
18 mm Hg/ml/min, the sensitivity and specificity equaled
46 and 87%, respectively, with a calculated overall prediction accuracy of 67%. The predictive accuracy achieved using the bolus technique in our study (72%) is slightly higher than the value reported by Boon and colleagues.
In summary, CSF resistance testing is a valuable supplementary test that can be performed in an outpatient setting
while measuring opening pressure with a lumbar tap.
The Non-Responder to ELD
The hypothesis underlying ELD is that the response to
short-term drainage is predictive of the response to longterm drainage achieved by shunt placement. In our study, 51
patients did not improve on ELD. Studies by other investigators who used ELD vary in their results. In the retrospective study of 32 patients with idiopathic NPH by Haan, et
al.,11 10 improved after a single lumbar tap and underwent
shunt placement. The remaining 22 patients, who had not
improved with the tap, underwent ELD; all 22 experienced
improvement. These authors concluded that ELD is a safe
and effective means of predicting shunt outcome. In a proJ. Neurosurg. / Volume 102 / June, 2005
spective study of 43 patients with idiopathic NPH, Walchenbach and colleagues,32 who used the drainage method described by Haan, et al.,11 reported a positive predictive
accuracy of 87% with ELD and a negative predictive accuracy of 36%. Walchenbach, et al., concluded that shunt
placement in patients who improve on ELD is justified.
They also concluded that patients who do not improve following drainage should be considered for shunt placement
given the high percentage of patients in the present study
who improved despite a negative ELD outcome.
In the study by Walchenbach and colleagues, of the 51
patients who did experience improvement on ELD, 18 requested shunt surgery despite our prediction of potential
reduced benefits. Of the 18 who received a shunt, four
patients showed some degree of gait improvement. These
numbers are too small at present to draw accurate conclusions, but as our study continues we hope to clarify this issue further. Presently, we explain to our patients that there
is an approximately one-in-five chance that they will experience improvement with shunt placement even though they
received no benefit from ELD.
Comparison of ELD With the Tap Test
There are no direct comparisons between a CSF tap test
and ELD in patients with idiopathic NPH. Nonetheless, in a
study of combined idiopathic and secondary NPH, Wikkelso, et al.,34 who introduced the 50-ml CSF tap, reported a
sensitivity of 68% and specificity of 100% in 24 patients
available to follow up who had received shunts. Malm, et
al.,18 could not confirm the results of Wikkelso and colleagues in their study of 25 patients with idiopathic NPH.
Malm, et al., reported that only 16 of the 25 patients who
improved with gait after shunt insertion showed improvement with the tap test and thus concluded that the tap test
was not predictive of shunt outcome. In general, the positive
predictive value of a CSF tap based on studies by Malm,18
Walchenbach,32 and Haan,11 and their colleagues ranges
from 73 to 100%. In summary, a CSF tap of 45 to 50 ml is
most expedient and has a high positive predictive value for
shunt outcome. Nevertheless, many patients who would potentially benefit from shunt placement would be lost as a result of the tap tests poor sensitivity, which ranges from 26
to 62%.11,18,32 Thus, the highest overall accuracy in terms of
shunt outcome prediction, based on our study data, is provided by ELD.
Patient Response to ELD
Our assessment of ELD outcome occurred at 72 hours
and consisted of both video and neuropsychological documentation and general clinical evaluation of symptoms
following ELD. The improvement described on ELD was
primarily based on clinical assessment of gait and balance
when the 72-hour drainage protocol was completed. The
3-day hospitalization was too short to assess any change
in the frequency of urination. With regard to dementia, in
contrast to some reports following large volume taps,18 we
found no significant improvement on MMSE or neuropsychological parameters, although there was a general
sense of improvement with regard to verbalization, initiation of conversation, and responses to questions during
daily rounds in patients whose gait and balance had improved. We speculate that were neuropsychological testing
995
06_05_JNS.1
6/1/05
3:29 PM
Page 996
A. Marmarou, et al.
performed months after shunt placement, we would probably find a significant difference. Nevertheless, a short practical test of memory and executive function, which can be
administered at the patients bedside or at the clinical follow
up, is still lacking.
Objective Gait Analysis in the Patient With NPH
There is still a need for a simple practical test that would
provide a quantitative index for the improvement of gait
disturbance. We analyzed the steps per minute over a fixed
length of 30 ft on the assumption that doing so would reflect
both the patients increase in stride length as the number of
steps decreased and the resulting increase in walking speed.
With improvement, however, the number of steps decreased
and the time required to traverse the 30-ft length decreased.
Because both the numerator and the denominator decreased, the ratio remained the same. If one uses the number of steps only, the variability among patients does not
lend itself to an analysis of larger patient groups. Among the
scales used in quantitative gait analysis, the only significant
quantitative feature was the number of steps used in turning
180. At baseline, the patient exhibited a multistep turn; the
number of steps used in turning decreased following shunt
placement. More work is needed to derive a gait scale that
reflects improvement following shunt insertion and that is
objective and easily quantified.
Transient Effect of ELD
All patients were discharged following a routine CT
study at the end of the drainage protocol to rule out the
occurrence of SDH or hygroma post-ELD. It is interesting
to note the gradual return to baseline function following discharge in patients who improved. Most improvement occurred immediately following discharge and returned to
near baseline within 10 days. The volume of CSF removed
in the study cohort was a mean of 465 6 135 ml, and the
time required to refill the original CSF volume was much
shorter than 10 days. The gradual return to baseline over a
longer time period was probably due to the fact that patients
continued to drain through the puncture wound until the
CSF leak was healed. The patient and caregiver survey was
invaluable in allowing the family to document the outcome
of ELD and gave greater assurance to patients with positive
ELD outcome that shunt surgery would be worthwhile.
Complications and Comorbidity
Overall, ELD complications are low (1.3%), with the
major complication consisting of the potential for infection.
In the two cases of infection among the 151-patient cohort,
both were successfully treated. No major complication occurred on resistance testing. Shunt complications were reasonably low as major complications, which included both
SDH and hygroma (6%). Nevertheless, other problems with
shunt insertion were not insignificant. Although troublesome, the improvement in response to shunt placement in
these patients had a more significant impact than the transient complications resulting from surgery.
Conclusions
External lumbar drainage is a highly prognostic and safe
996
procedure with a sensitivity of 92% for identifying patients
with NPH most likely to benefit from shunt surgery. Cerebrospinal fluid resistance testing provides a predictive
accuracy of 72% and remains useful because it can be performed in an outpatient setting. Finally, improvement on
shunt placement is independent of patient age up to the
ninth decade of life in those whose condition improved
post-ELD.
References
1. Benton AL: Revised Visual Retention Test: Clinical and Experimental Applications, ed 4. New York: The PsychologicalCorporation, 1974
2. Benton AL, Eslinger PJ, Damasio AR: Normative observations on
neuropsychological test performances in old age. J Clin Neuropsychol 3:3342, 1981
3. Black P: Idiopathic normal-pressure hydrocephalus. Results of
shunting in 62 patients. J Neurosurg 52:371377, 1980
4. Boon AJ, Tans TJ, Delwel EJ, Egeler-Peerdeman SM, Hanlo PW,
wurzer HA, et al: Dutch normal pressure hydrocephalus study:
prediction of outcome after shunting by resistance to outflow of
cerebrospinal fluid. J Neurosurg 87:687693, 1997
5. Brgesen SE, Gjerris F, Srensen SC: Intracranial pressure and
conductance to outflow of cerebrospinal fluid in normal-pressure
hydrocephalus. J Neurosurg 50:489493, 1979
6. Borkowski JG, Benton AL, Spreen O: Word fluency and brain
damage. Neuropsychologica 5:135140, 1967
7. Czosnyka M, Gjerris F, Maksymowicz W, et al: Computerized
lumbar infusion test: multicenter experience in clinical studies in
hydrocephalus, in Nagai H, Kamiya K, Ishii S (eds): Intracranial
Pressure IX. Berlin: Springer, 1994, pp 494495
8. Ekstedt J: CSF hydrodynamic studies in man. 1. Method of constant pressure CSF infusion. J Neurol Neurosurg Psychiatry 40:
105119, 1977
9. Evans WA: An encephalographic ratio for estimating ventricular
enlargement and cerebral atrophy. Arch Neurol Psychiatry 47:
931937,1942
10. Folstein MF, Folstein SE, McHugh PR: Mini-mental state. A
practical method for grading the cognitive state of patients for the
clinician. J Psychiatry Res 12:189198, 1975
11. Haan J, Thomeer RTWM: Predictive value of temporary external
lumbar drainage in normal pressure hydrocephalus. Neurosurgery 22:388391, 1988
12. Hakim S, Adams RD: The special clinical problem of symptomatic hydrocephalus with normal cerebrospinal fluid pressure. Observations on cerebrospinal fluid hydrodynamics. J Neurol Sci 2:
307327, 1965
13. Hughes CP, Siegel BA, Coxe WS, Gado MH, Grubb RL, Coleman RE, et al: Adult idiopathic communicating hydrocephalus
with and without shunting. J Neurol Neurosurg Psychiatry 41:
961971, 1978
14. Kahlon B,Sundberg G, Rehncrona S: Comparison between lumbar infusion and CSF tap test to predict outcome after shunt surgery in suspected normal pressure hydrocephalus. J Neurol Neurosurg Psychiatry 73:721726, 2002
15. Katzman R, Hussey F: A simple constant-infusion manometric
test for measurement of CSF absorption. I. Rationale and method.
Neurology 20:534544, 1970
16. Kosteljanetz M, Nehen AM, Kaalund J: Cerebrospinal fluid outflow resistance measurements in the selection of patients for shunt
surgery in the normal pressure hydrocephalus syndrome. A controlled trial. Acta Neurochir 104:4853, 1990
17. Larsson A, Wikkelso C, Bilting M, Stephensen H: Clinical parameters in 74 consecutive patients shunt operated for normal pressure
hydrocephalus. Acta Neurol Scand 84:475482, 1991
18. Malm J, Kristensen B, Karlsson T, Fagerlund M, Elfverson J,
Ekstedt J: The predictive value of cerebrospinal fluid dynamic
J. Neurosurg. / Volume 102 / June, 2005
06_05_JNS.1
6/1/05
3:29 PM
Page 997
Diagnosis and management of idiopathic NPH
19.
20.
21.
22.
23.
24.
25.
26.
27.
28.
tests in patients with the idiopathic adult hydrocephalus syndrome. Arch Neurol 52:783789, 1995
Marmarou A, Foda MA, Bandoh K, Yoshihara M, Yamamoto T,
Tsusi O, et al: Posttraumatic ventriculomegaly: hydrocephalus or
atrophy? A new approach for diagnosis using CSF dynamics. J
Neurosurg 85:10261035, 1996
Marmarou A, Shulman K, Rosende RM: A nonlinear analysis of
the cerebrospinal fluid system and intracranial pressure dynamics.
J Neurosurg 48:332344, 1978
Mateer CA, Mapou RL: Understanding, evaluating and managing attention disorders following traumatic brain injury. J Head
Trauma Rehabil 11:116, 1996
Petersen RC, Mokri B, Laws ER Jr: Surgical treatment of idiopathic hydrocephalus in elderly patients. Neurology 35: 307311,
1985
Raftopoulos C, Chaskis C, Delecluse F, Cantraine F, Bidaut L,
Brotchi J: Morphological quantitative analysis of intracranial pressure waves in normal pressure hydrocephalus. Neurol Res 14:
389396, 1992
Schmidt M: Rey Auditory and Verbal Learning Tests. Los Angeles: Western Psychological Services, 1996
Spanu G, Sangiovanni G, Locatelli D: Normal-pressure hydrocephalus: twelve years experience. Neurochirurgia 29:1519,
1986
Spreen O, Strauss E: A Compendium of Neuropsychological
Tests: Administration Norms, and Commentary. New York:
Oxford University Press, 1998
Stein SC, Langfitt TW: Normal-pressure hydrocephalus. Predicting the results of cerebrospinal fluid shunting. J Neurosurg
41: 463470, 1974
Takeuchi T, Kasahara E, Iwasaki M, Mima T, Mori K: Indications
for shunting in patients with idiopathic normal pressure hydrocephalus presenting with dementia and brain atrophy (atypical
J. Neurosurg. / Volume 102 / June, 2005
29.
30.
31.
32.
33.
34.
35.
idiopathic normal pressure hydrocephalus). Neurol Med Chir
40:3847, 2000
Vanneste J, Augustijn P, Davies GA, Dirvan C, Tan WF: Normalpressure hydrocephalus: is cisternography still useful in selecting
patients for a shunt? Arch Neurol 49: 366370, 1992
Vanneste J, Augustijn P, Dirven C, Tan WF, Goedhart ZD:
Shunting normal-pressure hydrocephalus: do the benefits outweigh the risks? A multicenter study and literature review. Neurology 42: 5459, 1992
Vanneste J, Augustijn P, Tan WF, Dirven C: Shunting normal
pressure hydrocephalus: the predictive value of combined clinical
and CT data. J Neurol Neurosurg Psychiatry 56:251256, 1993
Walchenbach R, Geiger E, Thomeer RTWM, Vanneste JAL: The
value of temporary external lumbar CSF drainage in predicting
the outcome of shunting on normal pressure hydrocephalus. J
Neurol Neurosurg Psychiatry 72:503506, 2002
Wechsler D: Wechsler Memory Scale Revised. San Antonio:
The Psychological Corporation, 1987
Wikkelso C, Andersson H, Blomstrand C, Lindquist G, Svendsen
P: Normal pressure hydrocephalus. Predictive value of the cerebrospinal fluid tap-test. Acta Neurol Scand 73:566573, 1986
Williams AM, Razomovsky AY, Hanley DF: Comparison of Pcsf
monitoring and controlled CSF drainage diagnose normal pressure hydrocephalus. Acta Neurochir Suppl 71:328330, 1998
Manuscript received March 5, 2004.
Accepted in final form October 7, 2004.
Address reprint requests to: Anthony Marmarou, Ph.D., Department of Neurosurgery, Virginia Commonwealth University Medical Center, 1001 East Broad Street, Suite 235, Richmond, Virginia
232190449. email: marmarou@hsc.vcu.edu.
997
También podría gustarte
- The Yellow House: A Memoir (2019 National Book Award Winner)De EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Calificación: 4 de 5 estrellas4/5 (98)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeDe EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeCalificación: 4 de 5 estrellas4/5 (5795)
- Shoe Dog: A Memoir by the Creator of NikeDe EverandShoe Dog: A Memoir by the Creator of NikeCalificación: 4.5 de 5 estrellas4.5/5 (537)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureDe EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureCalificación: 4.5 de 5 estrellas4.5/5 (474)
- Grit: The Power of Passion and PerseveranceDe EverandGrit: The Power of Passion and PerseveranceCalificación: 4 de 5 estrellas4/5 (588)
- On Fire: The (Burning) Case for a Green New DealDe EverandOn Fire: The (Burning) Case for a Green New DealCalificación: 4 de 5 estrellas4/5 (74)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryDe EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryCalificación: 3.5 de 5 estrellas3.5/5 (231)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceDe EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceCalificación: 4 de 5 estrellas4/5 (895)
- Never Split the Difference: Negotiating As If Your Life Depended On ItDe EverandNever Split the Difference: Negotiating As If Your Life Depended On ItCalificación: 4.5 de 5 estrellas4.5/5 (838)
- The Little Book of Hygge: Danish Secrets to Happy LivingDe EverandThe Little Book of Hygge: Danish Secrets to Happy LivingCalificación: 3.5 de 5 estrellas3.5/5 (400)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersDe EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersCalificación: 4.5 de 5 estrellas4.5/5 (345)
- The Unwinding: An Inner History of the New AmericaDe EverandThe Unwinding: An Inner History of the New AmericaCalificación: 4 de 5 estrellas4/5 (45)
- Team of Rivals: The Political Genius of Abraham LincolnDe EverandTeam of Rivals: The Political Genius of Abraham LincolnCalificación: 4.5 de 5 estrellas4.5/5 (234)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyDe EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyCalificación: 3.5 de 5 estrellas3.5/5 (2259)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaDe EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaCalificación: 4.5 de 5 estrellas4.5/5 (266)
- The Emperor of All Maladies: A Biography of CancerDe EverandThe Emperor of All Maladies: A Biography of CancerCalificación: 4.5 de 5 estrellas4.5/5 (271)
- Rise of ISIS: A Threat We Can't IgnoreDe EverandRise of ISIS: A Threat We Can't IgnoreCalificación: 3.5 de 5 estrellas3.5/5 (137)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreDe EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreCalificación: 4 de 5 estrellas4/5 (1090)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)De EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Calificación: 4.5 de 5 estrellas4.5/5 (121)
- The Perks of Being a WallflowerDe EverandThe Perks of Being a WallflowerCalificación: 4.5 de 5 estrellas4.5/5 (2104)
- Her Body and Other Parties: StoriesDe EverandHer Body and Other Parties: StoriesCalificación: 4 de 5 estrellas4/5 (821)
- Perioperative Management of AdrenalectomyDocumento13 páginasPerioperative Management of AdrenalectomyTJ LapuzAún no hay calificaciones
- The Abington Journal 07-04-2012Documento22 páginasThe Abington Journal 07-04-2012The Times LeaderAún no hay calificaciones
- Nursing Upper Gi BleedingDocumento23 páginasNursing Upper Gi BleedingLord Pozak Miller100% (3)
- E B I W: Safemedicate Rounding Rules GuidelinesDocumento9 páginasE B I W: Safemedicate Rounding Rules Guidelineslesky17Aún no hay calificaciones
- Toefle UjianDocumento19 páginasToefle UjianhistoryAún no hay calificaciones
- Actalyke Mini Op Man D6500091JDocumento29 páginasActalyke Mini Op Man D6500091Jjyoti ranjanAún no hay calificaciones
- Blood Bank Harmening Chapter 10Documento14 páginasBlood Bank Harmening Chapter 10ichummy19100% (3)
- Medical Needs Fatiguing The Descrpit Social CcienceDocumento11 páginasMedical Needs Fatiguing The Descrpit Social Ccienceicicle900Aún no hay calificaciones
- Quiz 5 - PSY1001 Introductory PsychologyDocumento6 páginasQuiz 5 - PSY1001 Introductory Psychologymrsdenison0% (1)
- Bell's Palsy Treatments & Medications - SingleCareDocumento11 páginasBell's Palsy Treatments & Medications - SingleCareRoxan PacsayAún no hay calificaciones
- First Aid TrainingDocumento202 páginasFirst Aid TrainingTheFreeSpiritAún no hay calificaciones
- Drug Study SitagliptinDocumento3 páginasDrug Study SitagliptinEzron Kendrick Duran50% (2)
- Mommy's MedicineDocumento3 páginasMommy's Medicinekcs.crimsonfoxAún no hay calificaciones
- Locomotor SyllabusDocumento5 páginasLocomotor SyllabusAyeshaKhalidAún no hay calificaciones
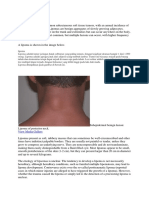
- LipomaDocumento51 páginasLipomaAgnes NiyAún no hay calificaciones
- Case Study: MYXEDEMATOUS COMADocumento5 páginasCase Study: MYXEDEMATOUS COMAjisooAún no hay calificaciones
- Hap-1 Question Paper 2018-19 1st SemesterDocumento1 páginaHap-1 Question Paper 2018-19 1st SemesterLavanya Tanguturi yellaAún no hay calificaciones
- Proposal For Defense Group 3Documento77 páginasProposal For Defense Group 3Kristiene Kyle AquinoAún no hay calificaciones
- A Case Study of Hospital Operations ManagementDocumento10 páginasA Case Study of Hospital Operations ManagementDaniel Goncalves50% (2)
- OHS-TBT-010 - Types of Hazards - 1Documento1 páginaOHS-TBT-010 - Types of Hazards - 1Tony NhabangaAún no hay calificaciones
- Anatomy & Physiology Unit 1Documento29 páginasAnatomy & Physiology Unit 1Priyanjali SainiAún no hay calificaciones
- Ashkenazi Jewish ScreeningDocumento10 páginasAshkenazi Jewish ScreeningJorge SHAún no hay calificaciones
- Acid Base Balance, Acidosis and AlkalosisDocumento28 páginasAcid Base Balance, Acidosis and AlkalosisHussan Ara50% (2)
- Alcoholic Liver DiseaseDocumento70 páginasAlcoholic Liver Diseaseaannaass nAún no hay calificaciones
- All India Futura NexX - Oct'22Documento5 páginasAll India Futura NexX - Oct'22tanwar shivaAún no hay calificaciones
- Trends of Violence Against Healthcare by ShaheerDocumento9 páginasTrends of Violence Against Healthcare by ShaheerShaheer zia100% (1)
- Nurses QuotesDocumento32 páginasNurses QuotesNikka Guban-SoteloAún no hay calificaciones
- Diuretics Antidiabetics AnalgesicsDocumento7 páginasDiuretics Antidiabetics AnalgesicsBillQueAún no hay calificaciones
- Nursing Group Research PaperDocumento16 páginasNursing Group Research Paperapi-368267454Aún no hay calificaciones
- Case Study 25Documento3 páginasCase Study 25Desiree Ladner Scott86% (7)