Documentos de Académico
Documentos de Profesional
Documentos de Cultura
Hypo Thyroid Is Mped in Review
Cargado por
Brenda CaraveoDescripción original:
Título original
Derechos de autor
Formatos disponibles
Compartir este documento
Compartir o incrustar documentos
¿Le pareció útil este documento?
¿Este contenido es inapropiado?
Denunciar este documentoCopyright:
Formatos disponibles
Hypo Thyroid Is Mped in Review
Cargado por
Brenda CaraveoCopyright:
Formatos disponibles
Hypothyroidism in Children Debra Counts and Surendra K. Varma Pediatr. Rev. 2009;30;251-258 DOI: 10.1542/pir.
30-7-251
The online version of this article, along with updated information and services, is located on the World Wide Web at: http://pedsinreview.aappublications.org/cgi/content/full/30/7/251
Pediatrics in Review is the official journal of the American Academy of Pediatrics. A monthly publication, it has been published continuously since 1979. Pediatrics in Review is owned, published, and trademarked by the American Academy of Pediatrics, 141 Northwest Point Boulevard, Elk Grove Village, Illinois, 60007. Copyright 2009 by the American Academy of Pediatrics. All rights reserved. Print ISSN: 0191-9601. Online ISSN: 1526-3347.
Article
endocrinology
Hypothyroidism in Children
Debra Counts, MD,* Surendra K. Varma, MD
Objectives
After completing this article, readers should be able to:
Author Disclosure Drs Counts and Varma have disclosed no nancial relationships relevant to this article. This commentary does not contain a discussion of an unapproved/ investigative use of a commercial product/device.
1. Describe the causes of hypothyroidism in infants and children. 2. Discuss the clinical presentation of and diagnostic approach to hypothyroidism. 3. Differentiate nonthyroidal illness low triiodothyronine (T3) syndrome from hypothyroidism. 4. Identify thyroid-binding globulin deciency as a euthyroid state. 5. Recognize the importance of treatment and implications of inadequate treatment of hypothyroidism in the neonate and young child.
Introduction
Thyroid hormone is essential to growth and neurologic development in childhood. The thyroid begins to take shape at 7 weeks gestation, and thyroid hormone (T4, thyroxine) is produced starting at 12 weeks gestation. Thyroid dysfunction in the neonate, infant, or child has a signicant impact on development. The goal of treatment is to assure normal growth and avoid developmental delay.
Hypothyroidism in the Neonate
Denition
Neonatal hypothyroidism results from decreased T4 production in a newborn. It is the most preventable cause of potential intellectual disability. T4 is critical to the myelinization of the central nervous system (CNS) during the rst 3 years after birth. In the healthy term baby, serum thyroid-stimulating hormone (TSH) concentrations normally rise abruptly to 60 to 80 mU/L within 30 to 60 minutes after delivery. The serum TSH concentration then decreases rapidly to about 20 mU/L by 1 day of age and subsequently more slowly to 6 to 10 mU/L by 1 week of age. This surge in TSH stimulates T4 secretion, with serum T4 concentrations peaking at 24 to 36 hours of age at 10 to 22 mcg/dL (128.7 to 283.2 nmol/L). Serum T3 concentrations also rise simultaneously to about 250 ng/dL (3.9 nmol/L), due to increased conversion of T4 to T3 in peripheral tissues and thyroidal secretion. T4, free T4, and T3 concentrations gradually fall in the rst 4 weeks after birth to total T4 concentrations of 7 to 16 mcg/dL (90.1 to 205.9 nmol/L), free T4 concentrations of 0.8 to 2.0 ng/dL (10.3 to 25.7 pmol/L), and TSH concentrations of 0.9 to 7.7 mU/L, which are higher than adult values. Abbreviations Preterm infants (especially those born at 24 to 27 weeks gestation) have smaller increases in serum TSH and free T4 AAP: American Academy of Pediatrics than do term infants, due to immaturity of the hypothalamicCNS: central nervous system pituitary-thyroid axis. Preterm infants have lower cord T4 IQ: intellectual quotient concentrations at birth, and due to their immaturity and T3: triiodothyronine concurrent nonthyroidal illness, the normal postnatal rise of T4: thyroxine T4 is delayed. Therefore, the number of abnormal newborn TBG: thyroid-binding globulin thyroid screening test results is disproportionately high in TRH: thyrotropin-releasing hormone preterm infants, especially when measuring T4 in heel stick TSH: thyroid-stimulating hormone blood specimens.
*Associate Professor of Pediatrics; Chief, Division of Pediatric Endocrinology, Department of Pediatrics, University of Maryland School of Medicine, Baltimore, Md. Editorial Board. Pediatrics in Review Vol.30 No.7 July 2009 251
endocrinology
hypothyroidism
Epidemiology
Sporadic cases of congenital hypothyroidism account for approximately 85% of cases; 15% are hereditary (autosomal recessive). More than 4 million infants are screened yearly in the United States, and 1,000 infants receive the diagnosis of congenital hypothyroidism each year, an incidence of approximately 1 in 4,000 newborns. In one study, the incidence was 1 in 4,000 in white infants, 1 in 2,000 in Hispanic infants, and 1 in 32,000 in African American infants. The incidence is twice as high in females, and congenital hypothyroidism is more common in twins. The longer the diagnosis and treatment of congenital hypothyroidism are delayed, the lower the intelligence quotient (IQ) versus the expected IQ.
Pathogenesis and Pathophysiology
Thyroid dysgenesis, a group of disorders occurring during thyroid development that includes ectopic thyroid, thyroid aplasia, and thyroid hypoplasia, occurs in 1 in 4,500 babies. Thyroid dysgenesis occasionally is associated (5% of cases) with other congenital anomalies. Inborn errors of thyroxine synthesis (dyshormonogenesis) are the most common genetic causes of congenital hypothyroidism, seen in 1 in 30,000 babies or 10% of diagnosed cases. These defects include a defect in thyroid peroxidase activity (impaired iodide oxidation and organication), abnormalities in iodide transport, production of abnormal thyroglobulin molecules, and iodotyrosine deiodinase deciency. Less frequent causes of congenital hypothyroidism include maternal antibody-mediated hypothyroidism (1 in 25,000 to 1 in 100,000), central hypothyroidism (1in 25,000 to 1 in 100,000), transient hypothyroidism, iodine deciency (seen in parts of Europe, 1 in 100), autoimmune thyroiditis (1 in 50,000), and iodide excess (1 in 50,000). In all these forms of congenital hypothyroidism except central hypothyroidism, serum T4 is low and serum TSH is elevated. In central hypothyroidism, both T4 and TSH are low. Central hypothyroidism may be associated with other pituitary deciencies, other congenital syndromes (especially midline defects such as septo-optic dysplasia or midline cleft lip and palate), birth trauma or asphyxia, and undertreatment of maternal hyperthyroidism (gestational hyperthyroidism). Neonatal screening programs that are based on TSH screening only do not identify babies who have these forms of congenital hypothyroidism. Central hypothyroidism should not be confused with thyroxine-binding globulin (TBG) deciency (1 in 4,300), which causes low serum T4 concentrations without TSH elevation but does not cause hypothyroidism.
252 Pediatrics in Review Vol.30 No.7 July 2009
Infants who are critically ill may have abnormal results on thyroid function studies due to nonthyroidal illness (previously called euthyroid-sick syndrome). In these babies, serum T3 is low due to poor peripheral conversion of T4 to T3, which is due to inhibition of 5monodeiodination by medications (glucocorticoids, amiodarone, propranolol, dopamine, dobutamine, furosemide), cytokines, and other circulating factors induced by the illness. Serum total T4 is low due to decreased binding to thyroid-binding proteins, but free T4 is normal (or even slightly elevated) and is measured best by assaying free T4 by equilibrium dialysis. TSH is low during the illness and typically rises during recovery. To distinguish between nonthyroidal illness and other causes of hypothyroidism, particularly central hypothyroidism, measurement of T3, free T4 by equilibrium dialysis, and TSH is needed. In nonthyroidal illness, the normal free T4 concentration, as measured by equilibrium dialysis, helps clarify the diagnosis. Thyroid replacement therapy is not indicated for treatment of nonthyroidal illness. Preterm infants who have respiratory distress syndrome, intrauterine growth restriction, and other medical problems tend not to have the expected postnatal rise in serum T4, T3, and TSH. T4 and T3 concentrations in these babies may fall after birth and remain low until they rise slowly as the infant improves and gains weight. Some of the fall in serum total T4 is due to decreased serum protein binding (hormonal reservoir), but serum free T4 concentrations are more normal in preterm infants. Serum T3 concentrations are low because peripheral conversion of T4 to T3 is decreased. TSH concentrations also are suppressed in sick infants and infants treated with glucocorticoids or dopamine, which adds to the decline in serum T4 and T3 concentrations.
Symptoms and Signs
More than 95% of newborns who have congenital hypothyroidism have little in the way of clinical manifestations at birth. Some maternal T4 crosses the placenta, so infants who cannot make any thyroid hormone still have serum T4 concentrations that are 25% to 50% of normal. Birth length and weight are within the normal range, but head circumference may be increased. An open posterior fontanelle in a term baby may signal congenital hypothyroidism. Symptoms and signs that may be present include lethargy, hypotonia, hoarse cry, feeding problems, constipation, macroglossia, umbilical hernia, dry skin, hypothermia, and prolonged jaundice. Goiter is uncommon. Newborns who have congenital thyroid dyshormonogenesis may have a palpable goiter, but the goiter typically develops later in untreated patients.
endocrinology
hypothyroidism
Laboratory Tests
For newborn screening, most states in the United States use initial T4 testing with follow-up TSH testing, although some are switching to TSH testing. Between 1 and 4 days of age, the normal range for serum total T4 concentrations is 10 to 22 mcg/dL (128.7 to 283.2 nmol/L). Between 1 and 4 weeks of age, the normal range for serum total T4 concentrations is 7 to 16 mcg/dL (90.1 to 205.9 nmol/L). Subclinical hypothyroidism is dened as a normal serum total or free T4 concentration and a high serum TSH concentration. Although agreement is not clear about whether to treat subclinical hypothyroidism, we recommend that infants who have subclinical hypothyroidism be treated during the rst 3 years after birth due to the critical dependence of the myelinizing CNS on thyroid hormone. Radioiodine scans of the thyroid are recommended by some experts as part of the initial evaluation, but these studies are considered optional in American Academy of Pediatrics (AAP) guidelines.
suspensions prepared by individual pharmacists may result in unreliable dosing. Parents should be instructed to crush the T4 tablet and mix it with a small volume of human milk, formula, or water. Soy formulas or any preparation containing concentrated iron or calcium should not be used because they reduce the absorption of T4. The more rapidly T4 concentrations are corrected, the better the neurologic outcome. In one study, patients who normalized their T4 concentrations in fewer than 2 weeks had better cognitive, attention, and achievement scores than those who took longer to normalize thyroid function. It also is clear that for more severely affected babies, a higher initial dose of thyroid replacement and normalization of thyroid function are associated with better neurologic outcomes. (1) The AAP recommends measurement of serum T4 or free T4 and TSH concentrations as follows:
Management
The overall goals of treatment are normal growth and good cognitive outcome. Serum T4 concentrations should be restored rapidly to the normal range, followed by continued maintenance of euthyroidism. The aim of treatment is to keep the serum T4 or free T4 concentration in the upper half of the normal range adjusted for age. Of note, many commercial laboratories do not provide age-adjusted normal ranges in their reports. In the rst postnatal year, serum T4 should be 10 to 16 mcg/dL (128.7 to 205.9 nmol/L) and serum free T4 should be 1.4 to 2.3 ng/dL (18.0 to 29.6 pmol/ L). The serum TSH concentration should be less than 5 mU/L. Oral T4 (levothyroxine) is the treatment of choice. The AAP recommends an initial dose of 10 to 15 mcg/kg per day, usually 37.5 or 50 mcg/day. Because term babies who were started on 50 mcg/day versus 37.5 mcg/day had IQ scores that were 11 points higher, 50 mcg/day is recommended for all term and full-size infants. In preterm and other low-birthweight infants, the thyroid replacement dose should be calculated by using 10 to 15 mcg/kg per day, with the higher end administered to babies who have low T4 concentrations. Only T4 tablets should be used because thyroid
At 2 and 4 weeks after the initiation of T4 treatment Every 1 to 2 months during the rst 6 postnatal months Every 3 to 4 months between 6 months and 3 years of age Every 6 to 12 months thereafter until growth is complete 2 weeks after any change in dose At more frequent intervals when compliance is questioned or abnormal results are obtained
Babies born with congenital hypothyroidism who are treated adequately
and promptly (in the rst 2 to 6 postnatal weeks) grow and develop normally.
About 10% to 20% of babies diagnosed as having congenital hypothyroidism have transient hypothyroidism. If the diagnosis of permanent hypothyroidism is not clear, T4 therapy can be stopped for 1 month when the child reaches 3 years of age and thyroid function retested off therapy. Permanent hypothyroidism is conrmed if the serum T4 value is low and the TSH value is elevated, and thyroid replacement should be restarted. If the T4 and TSH values remain normal, hypothyroidism has been present and now is resolved.
Prognosis
Babies born with congenital hypothyroidism who are treated adequately and promptly (in the rst 2 to 6 postnatal weeks) grow and develop normally. When these children
Pediatrics in Review Vol.30 No.7 July 2009 253
endocrinology
hypothyroidism
are compared with children born before newborn screening was instituted, the psychometric outcome is improved signicantly. However, children who are treated inadequately in the rst 2 to 3 years after birth have IQs below those of unaffected children. A literature review of 10 studies comparing children aficted with more severe versus moderate or mild congenital hypothyroidism showed six studies that reported no difference in IQ and four studies that reported a 6- to 15-point lower IQ in the more severely affected children. (2) A group of 18 infants who were inadequately treated in the rst 3 years after birth (T4 dose 5 mcg/kg per day) due to poor compliance had mean serum T4 concentrations of 8.6 mcg/dL (110.7 nmol/L) and a mean IQ score of 87 compared with a well-treated group who had mean serum T4 concentrations of 11.2 mcg/dL (114.2 nmol/L) and a mean IQ score of 105. (3) Other studies have found that even when there are no differences in global IQ scores, subtest components related to hypothyroidism may have some deciencies. Some infants who have congenital hypothyroidism, including those whose IQ scores are normal, can have other neurologic problems, including difculties with gross and ne motor coordination, ataxia, altered muscle tone, strabismus, decreased attention span, and speech. A Toronto screening program found language decits at age 3 years, which diminished with age, and poor visualspatial and verbal skills at age 5 years. (4)
age. The hypothyroidism is caused by failure of the hypothalamic-pituitary-thyroid axis, which results in decreased production of thyroid hormones. The hypothyroidism may be primary (at the level of thyroid gland), secondary (at the level of pituitary gland), or tertiary (at the level of hypothalamus).
Epidemiology
Most acquired childhood hypothyroidism is sporadic. Only 10% to 15% of cases are caused by inherited defects in thyroid gland synthesis or inborn errors of thyroid metabolism. Hashimoto thyroiditis (autoimmune), the most common cause of acquired childhood hypothyroidism, is more common in females and usually occurs in early to mid-puberty. The female-to-male ratio is 2:1. The incidence of Hashimoto thyroiditis during adolescence is approximately 1% to 2%. Hashimoto thyroiditis may occur by itself or in association with other autoimmune diseases such as type 1 diabetes mellitus, Addison disease, juvenile idiopathic arthritis, and systemic lupus erythematosus. Hashimoto thyroiditis occurs commonly in individuals who have Down syndrome or Turner syndrome. Both genetic and environmental factors contribute to the pathogenesis of Hashimoto thyroiditis. The autoimmune process is believed to start with activation of CD4 (helper) T lymphocytes specic for thyroid antigens. The other causes of acquired childhood hypothyroidism are listed in Table 1.
Thyroid-binding Globulin Deciency
TBG deciency manifests as the combination of a low serum total T4, low or normal serum free T4, and normal TSH concentrations. This entity should be distinguished from secondary or tertiary hypothyroidism (low T4 and normal TSH due to pituitary or hypothalamic hypofunction) by assessing free T4 by equilibrium dialysis. This assay corrects for inaccurate measurement of T4 and free T4 in a standard radioimmunoassay due to low concentrations of binding protein. Free T4 by dialysis is available in the United States through two commercial laboratories: Esoterix (Labcorps reference laboratory) or Nichols (Quests reference laboratory). TBG also can be measured in serum and is low in most cases. TBG deciency is an X-linked recessive disorder that occurs in approximately 1 in 4,300 newborns, predominantly males. Infants born with TBG deciency are euthyroid and do not require treatment.
Clinical Aspects
Clinical manifestations include a decline in linear growth, fatigue, constipation, cold intolerance, poor school performance, weight gain, irregular menstrual periods, and somnolence (Table 2). Children aficted with Hashimoto thyroiditis also may have other autoimmune disorders and a family history of thyroid and other autoimmune disorders to support the diagnosis. Other clinical features of acquired hypothyroidism include bradycardia, short stature, increased weight for height, dry skin, increased body hair, pallor, myxedema of the face, an enlarged thyroid gland, proximal muscle weakness, delayed relaxation phase of the ankle reex, and delayed puberty. Occasionally, acquired childhood hypothyroidism presents with precocious puberty. The enlarged thyroid gland usually is diffuse and nontender; sometimes the gland may be rm. The onset of acquired childhood hypothyroidism often is very subtle; in retrospect, it may be evident that signs and symptoms were present for a longer time, sometimes for 2 to 3 or more years. If previous height
Childhood (Acquired) Hypothyroidism
Denition
Childhood hypothyroidism also is known as acquired hypothyroidism. The onset usually is after 6 months of
254 Pediatrics in Review Vol.30 No.7 July 2009
endocrinology
hypothyroidism
Table 1.
Acquired Hypothyroidism
Primary (Thyroid Gland)
Hashimoto (autoimmune) thyroiditis Increased in some chromosome disorders Down syndrome Turner syndrome Postablation Surgical Radioiodine therapy Irradiation to neck Medication effects Thionamides (propylthiouracil, methimazole, carbimazole) Lithium Anticonvulsants Amiodarone Iodine deciency Late-onset congenital hypothyroidism Thyroid dysgenesis Inborn errors of thyroid metabolism Central hypothyroidism caused by: Craniopharyngioma and other tumors pressing on hypothalamus/pituitary Neurosurgery Cranial irradiation Head trauma Thyroid hormone resistance
treat bipolar disorder, interferes with thyroid hormone synthesis and secretion, leading to hypothyroidism. About one of three patients taking lithium develops subclinical hypothyroidism and one of six develops overt hypothyroidism. Most anticonvulsant drugs enhance hepatic metabolism and excretion of thyroxine, which could result in hypothyroidism, although patients receiving such drugs should not be treated unless the TSH concentration increases.
Chromosomal Disorders
Children who have Down syndrome or Turner syndrome have a higher incidence of hypothyroidism due to Hashimoto thyroiditis. Such patients should receive ongoing monitoring for evidence of hypothyroidism.
Iodine Deciency
Iodine deciency is uncommon in North America. However, iodine deciency associated with goiter is the most common cause of hypothyroidism globally.
Late Onset of Congenital Hypothyroidism
Late onset of mild forms of congenital hypothyroidism appear after 6 months of age. The most common causes are ectopic gland or one of the inborn errors of thyroid hormone syntheses.
Secondary (Pituitary) and Tertiary (Hypothalamus)
Secondary/Tertiary Hypothyroidism
Central hypothyroidism due to hypopituitarism or hypothalamic lesion leads to hypothyroidism that has subtle clinical features. Hypothyroidism can result from craniopharyngioma or other tumors pressing on the hypothalamic-pituitary axis. Hypothyroidism also can result from the surgery needed to remove the tumor or it can be caused by cranial irradiation.
Miscellaneous
measurements are available, a decline in linear growth from the onset of hypothyroidism will be evident.
Postablative Hypothyroidism
Postablative hypothyroidism may result from surgery, therapy with radioactive iodine, or irradiation. After a subtotal or total thyroidectomy, hypothyroidism eventually manifests. Such surgery may be indicated for removal of a thyroid neoplasm or for the treatment of Graves disease. Most children who have hyperthyroidism and are treated with radioactive iodine develop hypothyroidism, including 10% to 20% in the rst year after treatment. Any irradiation to the neck increases the risk of developing hypothyroidism dose-dependently.
Symptoms and Signs of Acquired Hypothyroidism
Table 2.
Hypothyroidism Due to Medications
Antithyroid medications such as thionamides, which include propylthiouracil, methimazole, and carbimazole, suppress thyroid function and lead to hypothyroidism if a high dose is used or the medication is continued when the childs hyperthyroidism is in remission. Lithium, used to
Fatigue Cold intolerance Somnolence Proximal muscle weakness Delayed relaxation phase of ankle reex Constipation Delayed growth Overweight for height Pallor Coarse and thick skin Increased body hair Enlargement of thyroid gland Bradycardia Irregular menstrual cycles Delayed puberty (occasionally precocious puberty)
Pediatrics in Review Vol.30 No.7 July 2009 255
endocrinology
hypothyroidism
based on the normal range for age. In cases of Hashimoto thyroiditis, thyroid antibody (thyroid peroxidase antibody, antimicrosomal antibodies, thyroglobulin antibody) titers are increased and are diagnostic of Hashimoto thyroiditis. The use of ultrasonography and thyroid scan in the diagnosis of hypothyroidism usually is not warranted, but if a nodule is present, ultrasonography and thyroid scan may be indicated. Determination of bone age to evaluate for short stature may add conrmatory information. The Figure presents a diagnostic scheme for evaluating the child suspected of having acquired hypothyroidism.
Management
Childhood hypothyroidism is treated with levothyroxine. The doses for those ages 6 to 12 months, 1 to 3 years, 3 to 10 years, and 10 to 18 years are 5 to 8, 4 to 6, 3 to 5, and 2 to 4 mcg/kg of body weight, respectively. Treatment should be individualized because the absorption of Figure. Clinical aspects of acquired hypothyroidism. T4thyroxine, TSHthyroid-stimulating T4 and metabolism vary among indihormone, TBGthyroid-binding globulin, TRHthyrotropin-releasing hormone viduals. Serum free T4 and TSH concentrations should be monitored peThyroid Hormone Resistance riodically, preferably at 3- to 6-month intervals. The goal is Thyroid hormone resistance is an autosomal dominant to keep the serum free T4 concentration at the mid-normal defect due to a mutation in the thyroid hormone receprange and the TSH concentration in the normal range. tor beta gene. Clinical features of hypothyroidism are Once the patient is euthyroid, many of the symptoms present but are due to the failure of thyroid hormone disappear. concentrations to overcome the receptor binding defect.
Prognosis
Laboratory Tests
The common thyroid function test results diagnostic of primary hypothyroidism are low serum T4 or low serum free T4 concentrations and elevated serum TSH concentrations. If the serum T4 or free T4 value is low and the serum TSH value is normal or low, secondary or tertiary hypothyroidism may be present but must be distinguished from TBG deciency. In these cases, the difference between secondary and tertiary hypothyroidism can be made on the basis of a thyrotropin-releasing hormone (TRH) stimulation test. In the case of secondary hypothyroidism, no signicant change in TSH values occurs after administration of TRH; in hypothalamic (tertiary) hypothyroidism, TSH values increase. It is important to interpret results
256 Pediatrics in Review Vol.30 No.7 July 2009
The prognosis for recovering lost linear growth depends on the duration of the hypothyroidism as well as the age at which treatment is started. If the diagnosis is made around puberty, growth may not recover fully. Similarly, if hypothyroidism is longstanding, thyroid replacement will not recover all lost stature. If the onset of childhood hypothyroidism occurs after age 2 to 3 years, no permanent intellectual damage or neurologic decit is likely. Children who have type 1 diabetes also should undergo annual thyroid function tests to ensure that hypothyroidism has not become part of the autoimmune glandular process. Overall, the prognosis of acquired childhood hypothyroidism is good if diagnosed in time and hypothyroidism is not of longstanding duration.
endocrinology
hypothyroidism
Summary
Based on strong clinical evidence, congenital hypothyroidism is the most treatable preventable cause of potential intellectual disability. (5) Normal values for thyroid function studies are age-specic, and T4 values in neonates and infants are much higher than in children and adults, based on multiple clinical studies. (6) The overall goals of treatment are normal growth and cognitive outcome. (7) The current standard of practice and clinical evidence show that normalization of the TSH concentration is the best measure of adequate treatment with levothyroxine for patients who have primary hypothyroidism. (8) Studies have shown that thyroid dysgenesis is the most common cause of congenital hypothyroidism, and autoimmune thyroiditis is the most common cause of acquired hypothyroidism in children. (8) TBG deciency is characterized by low T4, normal TSH, low TBG, and normal free T4 values (by dialysis). (6)
References
1. Selva KA, Harper A, Downs A, Blasco PA, Lafranchi SH. Neurodevelopmental outcomes in congenital hypothyroidism: comparison of initial T4 dose and time to reach target T4 and TSH. J Pediatr. 2005;147:775780 2. Grant DB, Fuggle P, Tokar S, Smith I. Psychomotor development in infants with congenital hypothyroidism diagnosed by neonatal screening. Acta Med Austriaca. 1992;19 (suppl 1):54 3. Neonatal hypothyroidism screening: status of patients at 6 years of age. New England Congenital Hypothyroidism Collaborative. J Pediatr. 1985;107:915 4. Rovet JF, Ehrlich RM, Sorbara DL. Neurodevelopment in infants and preschool children with congenital hypothyroidism: etiological and treatment factors affecting outcome. J Pediatr Psychol. 1992;17:187213 5. Foley TP.Hypothyroidism. Pediatr Rev. 2004;25:94 100 6. DeBoer MD, LaFranchi SH. Pediatric thyroid testing issues. Pediatr Endocrinol Rev. 2007;5:570 577 7. Raine JE, Donaldson MDC, Gregory JW, Savage MO, Hintz R. Thyroid disorders. In: Practical Endocrinology and Diabetes in Children. London, United Kingdom: Blackwell; 2006:91108 8. LaFranchi SH, Hanna CE. The thyroid gland and its disorders. In: Kappy MS, Allen DB, Geffner ME, ed. Principles and Practice of Pediatric Endocrinology. Boston, Mass: Charles C Thomas. 2005; 279 356
Pediatrics in Review Vol.30 No.7 July 2009 257
endocrinology
hypothyroidism
PIR Quiz
Quiz also available online at pedsinreview.aappublications.org. 5. Which of the following statements regarding congenital hypothyroidism is true? A. B. C. D. E. Goiter is a common feature seen in infants who have hypothyroidism. Males are affected more commonly than females. Most neonates show clinical features of hypothyroidism at birth. Preterm infants often have abnormal screening results due to delayed rise in T4 values. The most common cause is maternal antibody-mediated hypothyroidism.
6. A 2-week-old neonate born at 36 weeks gestation is receiving antibiotic therapy and ventilator support for presumed pneumonia and sepsis. Thyroid studies are performed because the neonatal screening result was abnormal. These studies reveal low total T4, low T3, low TSH, and normal free T4 values. Of the following, the most likely cause of these ndings is: A. B. C. D. E. Autoimmune thyroiditis. Central hypothyroidism. Nonthyroidal illness (euthyroid sick syndrome). Thyroid aplasia. Thyroxine dyshormonogenesis.
7. Which of the following clinical features is most likely to be present at birth in a neonate who has congenital hypothyroidism? A. B. C. D. E. Bradycardia. Increased muscle tone. Jitteriness. Microcephaly. Normal for gestational age weight and length.
8. You are evaluating a 10-year-old girl who has constipation and a recent decline in school performance. Thyroid studies ordered as part of your evaluation reveal the following: low total T4, low free T4, low TSH, and low T3 values. A TRH stimulation test results in elevation of the TSH to normal values. Which of the following is the most likely cause of her symptoms? A. B. C. D. E. Ectopic thyroid gland. Hashimoto thyroiditis. Hypothalamic tumor. Inborn error of thyroid metabolism. Thyroid-binding globulin deciency.
258 Pediatrics in Review Vol.30 No.7 July 2009
Hypothyroidism in Children Debra Counts and Surendra K. Varma Pediatr. Rev. 2009;30;251-258 DOI: 10.1542/pir.30-7-251
Updated Information & Services Subspecialty Collections
including high-resolution figures, can be found at: http://pedsinreview.aappublications.org/cgi/content/full/30/7/251 This article, along with others on similar topics, appears in the following collection(s): Fetus and Newborn Infant http://pedsinreview.aappublications.org/cgi/collection/fetus_new born_infant Endocrine Disorders http://pedsinreview.aappublications.org/cgi/collection/endocrine _disorders Information about reproducing this article in parts (figures, tables) or in its entirety can be found online at: http://pedsinreview.aappublications.org/misc/Permissions.shtml Information about ordering reprints can be found online: http://pedsinreview.aappublications.org/misc/reprints.shtml
Permissions & Licensing
Reprints
También podría gustarte
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)De EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Calificación: 4.5 de 5 estrellas4.5/5 (119)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaDe EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaCalificación: 4.5 de 5 estrellas4.5/5 (265)
- The Little Book of Hygge: Danish Secrets to Happy LivingDe EverandThe Little Book of Hygge: Danish Secrets to Happy LivingCalificación: 3.5 de 5 estrellas3.5/5 (399)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryDe EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryCalificación: 3.5 de 5 estrellas3.5/5 (231)
- Grit: The Power of Passion and PerseveranceDe EverandGrit: The Power of Passion and PerseveranceCalificación: 4 de 5 estrellas4/5 (587)
- Never Split the Difference: Negotiating As If Your Life Depended On ItDe EverandNever Split the Difference: Negotiating As If Your Life Depended On ItCalificación: 4.5 de 5 estrellas4.5/5 (838)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeDe EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeCalificación: 4 de 5 estrellas4/5 (5794)
- Rise of ISIS: A Threat We Can't IgnoreDe EverandRise of ISIS: A Threat We Can't IgnoreCalificación: 3.5 de 5 estrellas3.5/5 (137)
- Team of Rivals: The Political Genius of Abraham LincolnDe EverandTeam of Rivals: The Political Genius of Abraham LincolnCalificación: 4.5 de 5 estrellas4.5/5 (234)
- Shoe Dog: A Memoir by the Creator of NikeDe EverandShoe Dog: A Memoir by the Creator of NikeCalificación: 4.5 de 5 estrellas4.5/5 (537)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyDe EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyCalificación: 3.5 de 5 estrellas3.5/5 (2219)
- The Emperor of All Maladies: A Biography of CancerDe EverandThe Emperor of All Maladies: A Biography of CancerCalificación: 4.5 de 5 estrellas4.5/5 (271)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreDe EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreCalificación: 4 de 5 estrellas4/5 (1090)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersDe EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersCalificación: 4.5 de 5 estrellas4.5/5 (344)
- Her Body and Other Parties: StoriesDe EverandHer Body and Other Parties: StoriesCalificación: 4 de 5 estrellas4/5 (821)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceDe EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceCalificación: 4 de 5 estrellas4/5 (894)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureDe EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureCalificación: 4.5 de 5 estrellas4.5/5 (474)
- The Unwinding: An Inner History of the New AmericaDe EverandThe Unwinding: An Inner History of the New AmericaCalificación: 4 de 5 estrellas4/5 (45)
- The Yellow House: A Memoir (2019 National Book Award Winner)De EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Calificación: 4 de 5 estrellas4/5 (98)
- The Perks of Being a WallflowerDe EverandThe Perks of Being a WallflowerCalificación: 4.5 de 5 estrellas4.5/5 (2099)
- Examination of Thyroid GlandDocumento1 páginaExamination of Thyroid GlandGerardLumAún no hay calificaciones
- Facial Arterial Depth and Relationship With The Facial Musculature Layer - Lee, 2014Documento8 páginasFacial Arterial Depth and Relationship With The Facial Musculature Layer - Lee, 2014Rafael Autran Cavalcante AraújoAún no hay calificaciones
- On Fire: The (Burning) Case for a Green New DealDe EverandOn Fire: The (Burning) Case for a Green New DealCalificación: 4 de 5 estrellas4/5 (73)
- Immediate Dental Implant 1Documento13 páginasImmediate Dental Implant 1alkhalijia dentalAún no hay calificaciones
- English vocabulary organiser covers parts of the human bodyDocumento4 páginasEnglish vocabulary organiser covers parts of the human bodyIoanaAruncuteanAún no hay calificaciones
- Facial Danger Zones - Avoiding Nerve Injury in Facial Plastic SurgeryDocumento63 páginasFacial Danger Zones - Avoiding Nerve Injury in Facial Plastic Surgeryramarchiori100% (1)
- Abdominal Surgical Emergencies in Infants and Young ChildrenDocumento27 páginasAbdominal Surgical Emergencies in Infants and Young ChildrenBrenda CaraveoAún no hay calificaciones
- Cleft and PalateDocumento77 páginasCleft and PalateNini BendelianiAún no hay calificaciones
- Thyroid in PregnancyDocumento40 páginasThyroid in PregnancyGPFanAún no hay calificaciones
- EYE FOCUS MECHANISM: ACCOMMODATIONDocumento11 páginasEYE FOCUS MECHANISM: ACCOMMODATIONThadei Mruma100% (1)
- Hypercholesterolemia Among Children: When Is It High, and When Is It Really High?Documento4 páginasHypercholesterolemia Among Children: When Is It High, and When Is It Really High?Brenda CaraveoAún no hay calificaciones
- Probioticos en DiarreaDocumento126 páginasProbioticos en DiarreaBrenda CaraveoAún no hay calificaciones
- Ascitis en NiñosDocumento7 páginasAscitis en NiñosBrenda CaraveoAún no hay calificaciones
- c1q NefropatiaDocumento6 páginasc1q NefropatiaBrenda CaraveoAún no hay calificaciones
- BackpainDocumento10 páginasBackpainBrenda CaraveoAún no hay calificaciones
- Cerebral EdemaDocumento6 páginasCerebral EdemaantonopoulosalAún no hay calificaciones
- Mucositis PatobiologiaDocumento9 páginasMucositis PatobiologiaBrenda CaraveoAún no hay calificaciones
- Isolation 2007Documento225 páginasIsolation 2007Kiageng NicoAún no hay calificaciones
- ARIAReport 2010Documento153 páginasARIAReport 2010Syairah Banu DjufriAún no hay calificaciones
- Anemia MicrociticaDocumento15 páginasAnemia MicrociticaBrenda CaraveoAún no hay calificaciones
- Antibiticoterapia en Sepsis Tardia NeoreviewsDocumento11 páginasAntibiticoterapia en Sepsis Tardia NeoreviewsBrenda CaraveoAún no hay calificaciones
- Plaquetas en NeonatosDocumento6 páginasPlaquetas en NeonatosBrenda CaraveoAún no hay calificaciones
- KawasakiDocumento11 páginasKawasakiBrenda CaraveoAún no hay calificaciones
- Treatment of Allergic Rhinitis PDFDocumento23 páginasTreatment of Allergic Rhinitis PDFLydia MamurAún no hay calificaciones
- Alimentacionen Circunstancias EspecialesDocumento9 páginasAlimentacionen Circunstancias EspecialesBrenda CaraveoAún no hay calificaciones
- Diagnosis and Treatment of Atopic DermatitisDocumento19 páginasDiagnosis and Treatment of Atopic DermatitisBrenda CaraveoAún no hay calificaciones
- Cerebral Palsy - RomantsevaDocumento13 páginasCerebral Palsy - RomantsevaBrenda CaraveoAún no hay calificaciones
- Cerebral Palsy - RomantsevaDocumento13 páginasCerebral Palsy - RomantsevaBrenda CaraveoAún no hay calificaciones
- 22Q11.2 Distal Deletion: A Recurrent Genomic Disorder Distinct From Digeorge Syndrome and Velocardiofacial SyndromeDocumento8 páginas22Q11.2 Distal Deletion: A Recurrent Genomic Disorder Distinct From Digeorge Syndrome and Velocardiofacial SyndromeBrenda CaraveoAún no hay calificaciones
- Diagnostic Approach and Management of Cow S Milk.28Documento9 páginasDiagnostic Approach and Management of Cow S Milk.28minerva_stanciuAún no hay calificaciones
- Trombocitopenia Inmune PrimariaDocumento13 páginasTrombocitopenia Inmune PrimariaBrenda CaraveoAún no hay calificaciones
- AnafilaxisDocumento11 páginasAnafilaxisJoãoBrasilAún no hay calificaciones
- Adenomegalias 08Documento10 páginasAdenomegalias 08Brenda CaraveoAún no hay calificaciones
- Absceso Cerebral 99Documento7 páginasAbsceso Cerebral 99shen_siiAún no hay calificaciones
- Acidosis y AlcalosisDocumento10 páginasAcidosis y AlcalosisBrenda CaraveoAún no hay calificaciones
- Alt Coagulacion 08Documento12 páginasAlt Coagulacion 08Brenda CaraveoAún no hay calificaciones
- Update On Food AllergyDocumento15 páginasUpdate On Food AllergyBrenda CaraveoAún no hay calificaciones
- Respiratory Manifestations of Food AllergyDocumento8 páginasRespiratory Manifestations of Food AllergyBrenda CaraveoAún no hay calificaciones
- Sample ROS, PE PDFDocumento4 páginasSample ROS, PE PDFKASIA SyAún no hay calificaciones
- Traditional Malaysian Hairpin Used to Secure HairstylesDocumento6 páginasTraditional Malaysian Hairpin Used to Secure HairstylesarifinAún no hay calificaciones
- Boards - OmaeDocumento4 páginasBoards - OmaeJoyce EbolAún no hay calificaciones
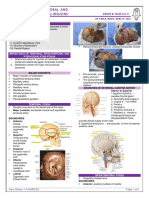
- Gross B Parotid Temporal and Infratemporal Regions Dr. JavierDocumento6 páginasGross B Parotid Temporal and Infratemporal Regions Dr. JavierAngelo HuligangaAún no hay calificaciones
- Serous Otitis MediaDocumento22 páginasSerous Otitis MediaChandra BhanAún no hay calificaciones
- Thyroid CrisisDocumento11 páginasThyroid CrisisKoka KolaAún no hay calificaciones
- Human Eye PDFDocumento13 páginasHuman Eye PDFHaidir MuhammadAún no hay calificaciones
- Cephalometric Study of Alterations Induced by Maxillary Slow Expansion in Adults PDFDocumento7 páginasCephalometric Study of Alterations Induced by Maxillary Slow Expansion in Adults PDFDonald Stephen Florez GuerreroAún no hay calificaciones
- Cleft Lip and Palate - ManagementDocumento35 páginasCleft Lip and Palate - ManagementSrikanth IkkAún no hay calificaciones
- Ear Anatomy: OtolaryngologyDocumento18 páginasEar Anatomy: OtolaryngologysafitriAún no hay calificaciones
- Teeth Crowding Case SolutionDocumento19 páginasTeeth Crowding Case SolutionSri Dewii SafitriAún no hay calificaciones
- Parotid Gland: LocationDocumento111 páginasParotid Gland: LocationFarah FarahAún no hay calificaciones
- Anatomy of Eyelid: Free Powerpoint Templates Free Powerpoint TemplatesDocumento24 páginasAnatomy of Eyelid: Free Powerpoint Templates Free Powerpoint TemplatesUdaif BabuAún no hay calificaciones
- DA Vol 19 3Documento36 páginasDA Vol 19 3Silvana Flores CastilloAún no hay calificaciones
- Subannular Ventilation Tubes Retrospective StudyDocumento6 páginasSubannular Ventilation Tubes Retrospective StudyAyuAnatrieraAún no hay calificaciones
- CT Neck Anatomy DemystifiedDocumento26 páginasCT Neck Anatomy DemystifiedTapi imaging centre Vyara dist TapiAún no hay calificaciones
- Latihan Soal Part of BodyDocumento3 páginasLatihan Soal Part of BodyAulia RomadhoniAún no hay calificaciones
- NoveltyNecktie#Gallery PDFDocumento51 páginasNoveltyNecktie#Gallery PDFAnonymous vH4yPPAún no hay calificaciones
- Thyroid Gland ExaminationDocumento4 páginasThyroid Gland ExaminationMariana Ungur100% (1)
- Five Sense Organs of Human Body and Their FunctionsDocumento36 páginasFive Sense Organs of Human Body and Their FunctionsEmraanAún no hay calificaciones
- tbcppt3 160629130547Documento37 páginastbcppt3 160629130547Evan AninditoAún no hay calificaciones
- Eye anatomy guide - cornea, iris, retinaDocumento2 páginasEye anatomy guide - cornea, iris, retinaminaAún no hay calificaciones